Abstract
Purpose
The goal of the present study was to examine the safety and efficacy of the vascular disrupting agent (VDA) EPC2407 (Crolibulin™) in experimental glioma models using bioluminescence imaging (BLI) and magnetic resonance imaging (MRI).
Procedures
Experimental imaging studies were performed in subcutaneous human U87 glioma xenografts and orthotopic murine gliomas established by intracranial implantation of luciferase-transfected glioma cells (GL261-luc). Correlative histopathology and long-term survival analysis was also performed.
Results
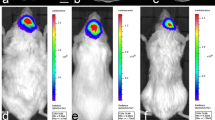
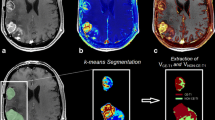
Treatment with EPC2407 decreased tumor perfusion and increased necrosis and tumor doubling times in subcutaneous U87 xenografts. Dynamic BLI and T1-weighted contrast-enhanced MRI showed reduction in blood flow of intracranial GL261-luc gliomas within a few hours of VDA treatment. T2-weighted MRI did not show any evidence of hemorrhaging or edema in uninvolved brain tissue of EPC2407-treated animals. A significant increase in median survival (p < 0.05) was observed in the orthotopic GL261-luc model following VDA treatment compared to untreated controls.
Conclusions
We demonstrate, for the first time, the biological activity of EPC2407 in experimental gliomas. Further investigation into the potential of VDAs in combination with chemoradiation therapy against gliomas is warranted.





Similar content being viewed by others
References
Ostrom QT, Gittleman H, Fulop F et al (2015) CBTRUS statistical report: primary brain and central nervous system tumors diagnosed in the United States in 2008–2012. Neuro Oncol 17(Suppl 4):iv1–iv62
Hottinger AF, Stupp R, Homicsko K (2014) Standards of care and novel approaches in the management of glioblastoma multiforme. Chin J Cancer 33:32–39
Johnson DR, O’Neill BP (2012) Glioblastoma survival in the United States before and during the temozolomide era. J Neurooncol 107:359–364
Thakkar JP, Dolecek TA, Horbinski C et al (2014) Epidemiologic and molecular prognostic review of glioblastoma. Cancer Epidemiol Biomarkers Prev 23:1985–1996
Yong RL, Lonser RR (2012) Surgery for glioblastoma multiforme: striking a balance. World Neurosurg 76:528–530
Young RM, Jamshidi A, Sherman JH (2015) Current trends in the surgical management and treatment of adult glioblastoma. Ann Transl Med 3:121
Deeken JF, Löscher W (2007) The blood–brain barrier and cancer: transporters, treatment, and Trojan horses. Clin Cancer Res 13:1663–1674
Van Tellingen O, Yetkin-Arik B, de Gooijer MC et al (2015) Overcoming the blood–brain tumor barrier for effective glioblastoma treatment. Drug Resist Updat 19:1–12
Ballabh P, Braun A, Nedergaard M (2004) The blood–brain barrier: an overview: structure, regulation, and clinical implications. Neurobiol Dis 16:1–13
Gerstner ER, Fine RL (2007) Increased permeability of the blood–brain barrier to chemotherapy in metastatic brain tumors: establishing a treatment paradigm. J Clin Oncol 25:2306–2312
Pronin IN, Holodny AI, Petraikin AV (1997) MRI of high-grade glial tumors: correlation between the degree of contrast enhancement and the volume of surrounding edema. Neuroradiology 39:348–350
Kemper EM, Boogerd W, Thuis I et al (2004) Modulation of the blood–brain barrier in oncology: therapeutic opportunities for the treatment of brain tumours? Cancer Treat Rev 30:415–423
Wei KC, Chu PC, Wang HY et al (2013) Focused ultrasound-induced blood–brain barrier opening to enhance temozolomide delivery for glioblastoma treatment: a preclinical study. PLoS One 8:e5899
Wang M, Etu J, Joshi S (2007) Enhanced disruption of the blood brain barrier by intracarotid mannitol injection during transient cerebral hypoperfusion in rabbits. J Neurosurg Anesthesiol 19:249–256
Hashizume K, Black KL (2002) Increased endothelial vesicular transport correlates with increased blood‐tumor barrier permeability induced by bradykinin and leukotriene C4. J Neuropathol Exp Neurol 61:725–735
Seshadri M, Ciesielski MJ (2009) MRI-based characterization of vascular disruption by 5,6-dimethylxanthenone-acetic acid in gliomas. J Cereb Blood Flow Metab 29:1373–1382
McKeage MJ, Baguley BC (2010) Disrupting established tumor blood vessels: an emerging therapeutic strategy for cancer. Cancer 116:1859–1871
Kim S, Peshkin L, Mitchison TJ (2012) Vascular disrupting agent drug classes differ in effects on the cytoskeleton. PLoS One 7:e40177
Kanthou C, Tozer GM (2002) The tumor vascular targeting agent combretastatin A-4-phosphate induces reorganization of the actin cytoskeleton and early membrane blebbing in human endothelial cells. Blood 99:2060–2069
Cai SX, Drewe J, Kemnitzer W (2009) Discovery of 4-aryl-4H-chromenes as potent apoptosis inducers using a cell- and caspase-based anti-cancer screening apoptosis program (ASAP): SAR studies and the identification of novel vascular disrupting agents. Anticancer Agents Med Chem 9:437–456
Kasibhatla S, Gourdeau H, Meerovitch K et al (2004) Discovery and mechanism of action of a novel series of apoptosis inducers with potential vascular targeting activity. Mol Cancer Ther 3:1365–1374
Gourdeau H, Leblond L, Hamelin B et al (2004) Antivascular and antitumor evaluation of 2-amino-4-(3-bromo-4,5-dimethoxyphenyl)-3-cyano-4H-chromenes, a novel series of anticancer agents. Mol Cancer Ther 3:1375–1384
Kalmuk J, Folaron M, Buchinger J et al (2015) Multimodal imaging guided preclinical trials of vascular targeting in prostate cancer. Oncotarget 6:24376–24392
Ciesielski MJ, Apfel L, Barone TA et al (2006) Antitumor effects of a xenogenic survivin bone marrow derived dendritic cell vaccine against murine GL261 gliomas. Cancer Immunol Immunother 55:1491–1503
Rich LJ, Seshadri M (2015) Photoacoustic imaging of vascular hemodynamics: validation with blood oxygenation level-dependent MR imaging. Radiology 275:110–118
Inoue Y, Kiryu S, Izawa K et al (2009) Comparison of subcutaneous and intraperitoneal injection of D-luciferin for in vivo bioluminescence imaging. Eur J Nucl Med Mol Imaging 36:771–779
Louis D, Ohgaki H, Wiestler O et al (2007) The 2007 WHO classification of tumours of the central nervous system. Acta Neuropathol 114:97–109
Fischer I, Gagner JP, Law M et al (2005) Angiogenesis in gliomas: biology and molecular pathophysiology. Brain Pathol 15:297–310
Ramirez YP, Weatherbee JL, Wheelhouse RT, Ross AH (2013) Glioblastoma multiforme therapy and mechanisms of resistance. Pharmaceuticals (Basel) 6:1475–1506
Pardridge WM (1998) CNS drug design based on principles of blood–brain barrier transport. J Neurochem 70:1781–1792
Mason RP, Zhao D, Liu L et al (2011) A perspective on vascular disrupting agents that interact with tubulin preclinical tumor imaging and biological assessment. Integr Biol 3:375–387
Zhao D, Chang CH, Kim JG et al (2011) In vivo near-infrared spectroscopy and magnetic resonance imaging monitoring of tumor response to combretastatin A-4-phosphate correlated with therapeutic outcome. Int J Radiat Oncol Biol Phys 2:574–581
Sun A, Hou L, Prugpichailers T et al (2010) Firefly luciferase-based dynamic bioluminescence imaging: a noninvasive technique to assess tumor angiogenesis. Neurosurgery 66:751–777
Zhao D, Richer E, Antich PP, Mason RP (2008) Antivascular effects of combretastatin A4 phosphate in breast cancer xenograft assessed using dynamic bioluminescence imaging and confirmed by MRI. FASEB 22:2445–2451
Sorensen AG, Batchelor TT, Wen PY et al (2008) Response criteria for glioma. Nat Clin Pract Oncol 5:634–644
Wu CX, Lin GS, Lin ZX et al (2015) Peritumoral edema shown by MRI predicts poor clinical outcome in glioblastoma. World J Surg Oncol 13:97
Wachsberger PR, Burd R, Marero N et al (2005) Effect of the tumor vascular-damaging agent, ZD6126, on the radioresponse of U87 glioblastoma. Clin Cancer Res 11:835–842
Milanović D, Braun F, Weber W et al (2012) The influence of the combined treatment with Vadimezan (ASA404) and taxol on the growth of U251 glioblastoma xenografts. BMC Cancer 12:242
Chamberlain MC, Grimm S, Phuphanich S et al (2014) A phase 2 trial of verubulin for recurrent glioblastoma: a prospective study by the Brain Tumor Investigational Consortium (BTIC). J Neurooncol 118:335–343
Anthony SP, Read W, Rosen PJ et al (2008) Initial results of a first-in-man phase I study of EPC2407, a novel small molecule microtubule inhibitor anticancer agent with tumor vascular endothelial disrupting activity. J Clin Oncol 26:2531
Read WL, Rosen P, Lee P et al (2009) Pharmacokinetic and pharmacodynamics results of a 4-hr IV administration phase I study with EPC2407, a novel vascular disrupting agent [abstract]. J Clin Oncol 27:3569
Jenkins EO, Schiff D, Mackman N, Key NS (2010) Venous thromboembolism in malignant gliomas. J Thromb Haemost 8:221–227
De Vries NA, Beijnen JH, van Tellingen O (2009) High-grade glioma mouse models and their applicability for preclinical testing. Cancer Treat Rev 35:714–723
Syvanen S, Lindhe O, Palner M et al (2009) Species differences in blood–brain barrier transport of three positron emission tomography radioligands with emphasis on P-glycoprotein transport. Drug Metab Dispos 37:635–643
Acknowledgments
The authors would like to thank the technical assistance provided by Marianne Marcotte, Steven Turowski, and the staff of the Laboratory Animal Resource and the Small Animal Bio-Imaging Resource in performing these studies. The authors would also like to thank Dr. Michael Ciesielski for thoughtful discussions and technical assistance in performing these studies. This work was supported by a grant from the American Brain Tumor Association (in honor of Michael Baldasaro) and utilized shared resources supported by the National Cancer Institute P30CA06156 and RPCI Developmental funds.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
ESM 1
(PDF 1087 kb)
Rights and permissions
About this article
Cite this article
Folaron, M., Seshadri, M. Bioluminescence and MR Imaging of the Safety and Efficacy of Vascular Disruption in Gliomas. Mol Imaging Biol 18, 860–869 (2016). https://doi.org/10.1007/s11307-016-0963-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11307-016-0963-8