Abstract
Intravenous iron administration has emerged as a crucial intervention for managing patients with cardiorenal syndrome (CRS) and iron deficiency, with or without the presence of anemia. Multiple studies have demonstrated the benefits of intravenous iron supplementation in improving anemia, symptoms, and functional capacity in patients with HF and iron deficiency. Furthermore, iron supplementation has been associated with a reduction in hospitalizations for HF exacerbation and the improvement of patients’ quality of life and clinical outcomes. In addition to its effects on HF management, emerging evidence suggests a potential positive impact on kidney function in patients with CRS. Studies have shown an increase in estimated glomerular filtration rate and improvements in renal function markers in patients receiving intravenous iron therapy, highlighting the potential of this intervention in patients with CRS. This paper reviews the existing literature on the impact of intravenous iron therapy in these patient populations and explores its effects on various clinical outcomes. Future research endeavors are eagerly awaited to further improve our understanding of its clinical implications and optimize patient outcomes.


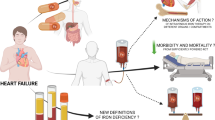
Adapted from Alnuwaysir et al. 2021 [30]
Similar content being viewed by others
References
Ronco C, McCullough P, Anker SD, Anand I, Aspromonte N, Bagshaw SM, Bellomo R, Berl T, Bobek I, Cruz DN, Daliento L, Davenport A, Haapio M, Hillege H, House AA, Katz N, Maisel A, Mankad S, Zanco P, Mebazaa A, Palazzuoli A, Ronco F, Shaw A, Sheinfeld G, Soni S, Vescovo G, Zamperetti N, Ponikowski P, Acute Dialysis Quality Initiative (ADQI) consensus group (2010) Cardio-renal syndromes: report from the consensus conference of the acute dialysis quality initiative. Eur Heart J 31(6):703–711. https://doi.org/10.1093/eurheartj/ehp507
Andrews NC (1999) Disorders of iron metabolism. N Engl J Med 341(26):1986–1995. https://doi.org/10.1056/NEJM199912233412607
Datz C, Felder TK, Niederseer D, Aigner E (2013) Iron homeostasis in the metabolic syndrome. Eur J Clin Invest 43(2):215–224. https://doi.org/10.1111/eci.12032
Ponikowska B, Suchocki T, Paleczny B, Olesinska M, Powierza S, Borodulin-Nadzieja L, Reczuch K, von Haehling S, Doehner W, Anker SD, Cleland JG, Jankowska EA (2013) Iron status and survival in diabetic patients with coronary artery disease. Diabetes Care 36(12):4147–4156. https://doi.org/10.2337/dc13-0528
Baker JF, Ghio AJ (2009) Iron homoeostasis in rheumatic disease. Rheumatology (Oxford) 48(11):1339–1344. https://doi.org/10.1093/rheumatology/kep221
Macdougall IC, Canaud B, de Francisco AL, Filippatos G, Ponikowski P, Silverberg D, van Veldhuisen DJ, Anker SD (2012) Beyond the cardiorenal anaemia syndrome: recognizing the role of iron deficiency. Eur J Heart Fail 14(8):882–886. https://doi.org/10.1093/eurjhf/hfs056
Triposkiadis F, Karayannis G, Giamouzis G, Skoularigis J, Louridas G, Butler J (2009) The sympathetic nervous system in heart failure physiology, pathophysiology, and clinical implications. J Am Coll Cardiol 54(19):1747–1762. https://doi.org/10.1016/j.jacc.2009.05.015
Ganz T, Nemeth E (2016) Iron balance and the role of hepcidin in chronic kidney disease. Semin Nephrol 36(2):87–93. https://doi.org/10.1016/j.semnephrol.2016.02.001
Batchelor EK, Kapitsinou P, Pergola PE, Kovesdy CP, Jalal DI (2020) Iron deficiency in chronic kidney disease: updates on pathophysiology, diagnosis, and treatment. J Am Soc Nephrol 31(3):456–468. https://doi.org/10.1681/ASN.2019020213
Opasich C, Cazzola M, Scelsi L, De Feo S, Bosimini E, Lagioia R, Febo O, Ferrari R, Fucili A, Moratti R, Tramarin R, Tavazzi L (2005) Blunted erythropoietin production and defective iron supply for erythropoiesis as major causes of anaemia in patients with chronic heart failure. Eur Heart J 26(21):2232–2237. https://doi.org/10.1093/eurheartj/ehi388
Cunha GJL, Rocha BML, Menezes Falcao L (2018) Iron deficiency in chronic and acute heart failure: a contemporary review on intertwined conditions. Eur J Intern Med 52:1–7. https://doi.org/10.1016/j.ejim.2018.04.013
Ezekowitz JA, McAlister FA, Armstrong PW (2003) Anemia is common in heart failure and is associated with poor outcomes: insights from a cohort of 12065 patients with new-onset heart failure. Circulation 107(2):223–225. https://doi.org/10.1161/01.cir.0000052622.51963.fc
Klip IT, Jankowska EA, Enjuanes C, Voors AA, Banasiak W, Bruguera J, Rozentryt P, Polonski L, van Veldhuisen DJ, Ponikowski P, Comin-Colet J, van der Meer P (2014) The additive burden of iron deficiency in the cardiorenal–anaemia axis: scope of a problem and its consequences. Eur J Heart Fail 16(6):655–662. https://doi.org/10.1002/ejhf.84
Voors AA, Anker SD, Cleland JG, Dickstein K, Filippatos G, van der Harst P, Hillege HL, Lang CC, Ter Maaten JM, Ng L, Ponikowski P, Samani NJ, van Veldhuisen DJ, Zannad F, Zwinderman AH, Metra M (2016) A systems BIOlogy Study to TAilored Treatment in Chronic Heart Failure: rationale, design, and baseline characteristics of BIOSTAT-CHF. Eur J Heart Fail 18(6):716–726. https://doi.org/10.1002/ejhf.531
Alnuwaysir RIS, Grote Beverborg N, Hoes MF, Markousis-Mavrogenis G, Gomez KA, van der Wal HH, Cleland JGF, Dickstein K, Lang CC, Ng LL, Ponikowski P, Anker SD, van Veldhuisen DJ, Voors AA, van der Meer P (2022) Additional burden of iron deficiency in heart failure patients beyond the cardio-renal anaemia syndrome: findings from the BIOSTAT-CHF study. Eur J Heart Fail 24(1):192–204. https://doi.org/10.1002/ejhf.2393
Macdougall IC (2010) Iron supplementation in the non-dialysis chronic kidney disease (ND-CKD) patient: oral or intravenous? Curr Med Res Opin 26(2):473–482. https://doi.org/10.1185/03007990903512461
Pergola PE, Fishbane S, Ganz T (2019) Novel oral iron therapies for iron deficiency anemia in chronic kidney disease. Adv Chronic Kidney Dis 26(4):272–291. https://doi.org/10.1053/j.ackd.2019.05.002
Macdougall IC, Bock AH, Carrera F, Eckardt KU, Gaillard C, Van Wyck D, Roubert B, Nolen JG, Roger SD, Investigators F-CS (2014) FIND-CKD: a randomized trial of intravenous ferric carboxymaltose versus oral iron in patients with chronic kidney disease and iron deficiency anaemia. Nephrol Dial Transplant 29(11):2075–2084. https://doi.org/10.1093/ndt/gfu201
Niehaus ED, Malhotra R, Cocca-Spofford D, Semigran M, Lewis GD (2015) Repletion of iron stores with the use of oral iron supplementation in patients with systolic heart failure. J Card Fail 21(8):694–697. https://doi.org/10.1016/j.cardfail.2015.05.006
Lewis GD, Malhotra R, Hernandez AF, McNulty SE, Smith A, Felker GM, Tang WHW, LaRue SJ, Redfield MM, Semigran MJ, Givertz MM, Van Buren P, Whellan D, Anstrom KJ, Shah MR, Desvigne-Nickens P, Butler J, Braunwald E, Network NHFCR (2017) Effect of oral iron repletion on exercise capacity in patients with heart failure with reduced ejection fraction and iron deficiency: the IRONOUT HF randomized clinical trial. JAMA 317(19):1958–1966. https://doi.org/10.1001/jama.2017.5427
Okonko DO, Grzeslo A, Witkowski T, Mandal AK, Slater RM, Roughton M, Foldes G, Thum T, Majda J, Banasiak W, Missouris CG, Poole-Wilson PA, Anker SD, Ponikowski P (2008) Effect of intravenous iron sucrose on exercise tolerance in anemic and nonanemic patients with symptomatic chronic heart failure and iron deficiency FERRIC-HF: a randomized, controlled, observer-blinded trial. J Am Coll Cardiol 51(2):103–112. https://doi.org/10.1016/j.jacc.2007.09.036
Anker SD, Comin Colet J, Filippatos G, Willenheimer R, Dickstein K, Drexler H, Luscher TF, Bart B, Banasiak W, Niegowska J, Kirwan BA, Mori C, von Eisenhart RB, Pocock SJ, Poole-Wilson PA, Ponikowski P, Investigators F-HT (2009) Ferric carboxymaltose in patients with heart failure and iron deficiency. N Engl J Med 361(25):2436–2448. https://doi.org/10.1056/NEJMoa0908355
Ponikowski P, van Veldhuisen DJ, Comin-Colet J, Ertl G, Komajda M, Mareev V, McDonagh TA, Parkhomenko A, Tavazzi L, Levesque V, Mori C, Roubert B, Filippatos G, Ruschitzka F, Anker SD (2014) Rationale and design of the CONFIRM-HF study: a double-blind, randomized, placebo-controlled study to assess the effects of intravenous ferric carboxymaltose on functional capacity in patients with chronic heart failure and iron deficiency. ESC Heart Fail 1(1):52–58. https://doi.org/10.1002/ehf2.12006
Ponikowski P, van Veldhuisen DJ, Comin-Colet J, Ertl G, Komajda M, Mareev V, McDonagh T, Parkhomenko A, Tavazzi L, Levesque V, Mori C, Roubert B, Filippatos G, Ruschitzka F, Anker SD, Investigators C-H (2015) Beneficial effects of long-term intravenous iron therapy with ferric carboxymaltose in patients with symptomatic heart failure and iron deficiencydagger. Eur Heart J 36(11):657–668. https://doi.org/10.1093/eurheartj/ehu385
Ponikowski P, Kirwan BA, Anker SD, McDonagh T, Dorobantu M, Drozdz J, Fabien V, Filippatos G, Gohring UM, Keren A, Khintibidze I, Kragten H, Martinez FA, Metra M, Milicic D, Nicolau JC, Ohlsson M, Parkhomenko A, Pascual-Figal DA, Ruschitzka F, Sim D, Skouri H, van der Meer P, Lewis BS, Comin-Colet J, von Haehling S, Cohen-Solal A, Danchin N, Doehner W, Dargie HJ, Motro M, Butler J, Friede T, Jensen KH, Pocock S, Jankowska EA, AFFIRM-AHF Investigators (2020) Ferric carboxymaltose for iron deficiency at discharge after acute heart failure: a multicentre, double-blind, randomised, controlled trial. Lancet 396(10266):1895–1904. https://doi.org/10.1016/S0140-6736(20)32339-4
Graham FJ, Pellicori P, Ford I, Petrie MC, Kalra PR, Cleland JGF (2021) Intravenous iron for heart failure with evidence of iron deficiency: a meta-analysis of randomised trials. Clin Res Cardiol 110(8):1299–1307. https://doi.org/10.1007/s00392-021-01837-8
Kalra PR, Cleland JGF, Petrie MC, Thomson EA, Kalra PA, Squire IB, Ahmed FZ, Al-Mohammad A, Cowburn PJ, Foley PWX, Graham FJ, Japp AG, Lane RE, Lang NN, Ludman AJ, Macdougall IC, Pellicori P, Ray R, Robertson M, Seed A, Ford I, Group IS (2022) Intravenous ferric derisomaltose in patients with heart failure and iron deficiency in the UK (IRONMAN): an investigator-initiated, prospective, randomised, open-label, blinded-endpoint trial. Lancet 400(10369):2199–2209. https://doi.org/10.1016/S0140-6736(22)02083-9
Salah HM, Savarese G, Rosano GMC, Ambrosy AP, Mentz RJ, Fudim M (2023) Intravenous iron infusion in patients with heart failure: a systematic review and study-level meta-analysis. ESC Heart Fail 10(2):1473–1480. https://doi.org/10.1002/ehf2.14310
Dhaliwal S, Kalogeropoulos AP (2023) Markers of iron metabolism and outcomes in patients with heart failure: a systematic review. Int J Mol Sci 24(6). https://doi.org/10.3390/ijms24065645
Macdougall IC (2017) Intravenous iron therapy in patients with chronic kidney disease: recent evidence and future directions. Clin Kidney J 10(Suppl 1):i16–i24. https://doi.org/10.1093/ckj/sfx043
Toblli JE, Di Gennaro F, Rivas C (2015) Changes in echocardiographic parameters in iron deficiency patients with heart failure and chronic kidney disease treated with intravenous iron. Heart Lung Circ 24(7):686–695. https://doi.org/10.1016/j.hlc.2014.12.161
Ponikowski P, Filippatos G, Colet JC, Willenheimer R, Dickstein K, Luscher T, Gaudesius G, von Eisenhart RB, Mori C, Greenlaw N, Ford I, Macdougall I, Anker SD, Investigators F-HT (2015) The impact of intravenous ferric carboxymaltose on renal function: an analysis of the FAIR-HF study. Eur J Heart Fail 17(3):329–339. https://doi.org/10.1002/ejhf.229
Alnuwaysir RIS, Hoes MF, van Veldhuisen DJ, van der Meer P, Grote Beverborg N (2021) Iron deficiency in heart failure: mechanisms and pathophysiology. J Clin Med 11(1). https://doi.org/10.3390/jcm11010125
Cairo G, Bernuzzi F, Recalcati S (2006) A precious metal: iron, an essential nutrient for all cells. Genes Nutr 1(1):25–39. https://doi.org/10.1007/BF02829934
Universitätsklinikum H-E, Deutsches Zentrum für H-K-F, Charite University BG (2024) Intravenous iron in patients with systolic heart failure and iron deficiency to improve morbidity & mortality. https://clinicaltrials.gov/show/NCT03036462
Mentz RJ, Ambrosy AP, Ezekowitz JA, Lewis GD, Butler J, Wong YW, De Pasquale CG, Troughton RW, O'Meara E, Rockhold FW, Garg J, Samsky MD, Leloudis D, Dugan M, Mundy LM, Hernandez AF, Investigators H-FT (2021) Randomized placebo-controlled trial of ferric carboxymaltose in heart failure with iron deficiency: rationale and design. Circ Heart Fail 14(5):e008100. https://doi.org/10.1161/CIRCHEARTFAILURE.120.008100
Charite University BG, University of G (2020) Effect of IV iron in patients with heart failure with preserved ejection fraction. https://clinicaltrials.gov/show/NCT03074591
Vinke JS, Eisenga MF, Sanders JF, Berger SP, Spikman JM, Abdulahad WH, Bakker SJ, Gaillard C, van Zuilen AD, van der Meer P, de Borst MH (2023) Effect of intravenous ferric carboxymaltose on exercise capacity after kidney transplantation (EFFECT-KTx): rationale and study protocol for a double-blind, randomised, placebo-controlled trial. BMJ Open 13(3):e065423. https://doi.org/10.1136/bmjopen-2022-065423
Shah AA, Donovan K, Seeley C, Dickson EA, Palmer AJR, Doree C, Brunskill S, Reid J, Acheson AG, Sugavanam A, Litton E, Stanworth SJ (2021) Risk of infection associated with administration of intravenous iron: a systematic review and meta-analysis. JAMA Netw Open 4(11):e2133935. https://doi.org/10.1001/jamanetworkopen.2021.33935
Rund D (2021) Intravenous iron and infection risk-still an unanswered question. JAMA Netw Open 4(11):e2134453. https://doi.org/10.1001/jamanetworkopen.2021.34453
Macdougall IC, White C, Anker SD, Bhandari S, Farrington K, Kalra PA, McMurray JJV, Murray H, Tomson CRV, Wheeler DC, Winearls CG, Ford I, PIVOTAL Investigators and Committees (2019) Intravenous iron in patients undergoing maintenance hemodialysis. N Engl J Med 380(5):447–458. https://doi.org/10.1056/NEJMoa1810742
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no competing interests to declare that are relevant to the content of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Doumani, G., Spanos, G., Theofilis, P. et al. Cardiorenal syndrome and iron supplementation—more benefits than risks: a narrative review. Int Urol Nephrol 56, 597–606 (2024). https://doi.org/10.1007/s11255-023-03741-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-023-03741-8