Abstract
Purpose
To construct a nomogram for evaluation of the recurrence risk of upper urinary tract stones in patients.
Methods
We retrospectively reviewed the clinical data of 657 patients with upper urinary tract stones and divided them into stone recurrence group and non-recurrence group. Blood routine, urine routine, biochemical, and urological CT examinations were searched from the electronic medical record, relevant clinical data were collected, including age, BMI, stones number and location, maximum diameter, hyperglycemia, hypertension, and relevant blood and urine parameters. The Wilcoxon rank-sum test, independent sample t test, and Chi-square test were used to preliminarily analyze the data of the two groups, then LASSO and logistic regression analysis were used to find out the significant difference indicators. Finally, R software was used to draw a nomogram to construct the model, and ROC curve was drawn to evaluate the sensitivity and specificity.
Results
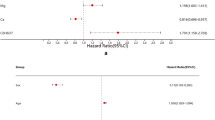
The results showed that multiple stones (OR: 1.832, 95% CI 1.240–2.706), bilateral stones (OR: 1.779, 95% CI 1.226–2.582), kidney stones (OR: 3.268, 95% CI 1.638–6.518), and kidney ureteral stones (OR: 3.375, 95% CI 1.649–6.906) were high risk factors. And the stone recurrence risk was positively correlated with creatinine (OR: 1.012, 95% CI 1.006–1.018), urine pH (OR: 1.967, 95% CI 1.343–2.883), Apo B (OR: 4.189, 95% CI 1.985–8.841) and negatively correlated with serum phosphorus (OR: 0.282, 95% CI 0.109–0.728). In addition, the sensitivity and specificity of the prediction model were 73.08% and 61.25%, diagnosis values were greater than any single variable.
Conclusion
The nomogram model can effectively evaluate the recurrence risk of upper urinary stones, especially suitable for stone postoperative patients, to help reduce the possibility of postoperative stone recurrence.




Similar content being viewed by others
Data availability
Data are available with permission from the corresponding author.
References
Tzelves L, Türk C, Skolarikos A (2021) European association of urology urolithiasis guidelines: where are we going? Eur Urol Focus. https://doi.org/10.1016/j.euf.2020.09.011
Zeng G, Mai Z, Xia S, Wang Z, Zhang K, Wang L, Long Y, Ma J, Li Y, Wan SP, Wu W, Liu Y, Cui Z, Zhao Z, Qin J, Zeng T, Liu Y, Duan X, Mai X, Yang Z, Kong Z, Zhang T, Cai C, Shao Y, Yue Z, Li S, Ding J, Tang S, Ye Z (2017) Prevalence of kidney stones in china: an ultrasonography based cross-sectional study. BJU Int. https://doi.org/10.1111/bju.13828
Sorokin I, Mamoulakis C, Miyazawa K, Rodgers A, Talati J, Lotan Y (2017) Epidemiology of stone disease across the world. World J Urol. https://doi.org/10.1007/s00345-017-2008-6
Milligan M, Berent AC (2019) Medical and interventional management of upper urinary tract uroliths. Vet Clin North Ame. https://doi.org/10.1016/j.cvsm.2018.11.004
Ziemba JB, Matlaga BR (2017) Epidemiology and economics of nephrolithiasis. Investig Clin Urol. https://doi.org/10.4111/icu.2017.58.5.299
Antonelli JA, Maalouf NM, Pearle MS, Lotan Y (2014) Use of the national health and nutrition examination survey to calculate the impact of obesity and diabetes on cost and prevalence of urolithiasis in 2030. Eur Urol 66(4):724–729. https://doi.org/10.1016/j.eururo.2014.06.036
Ingvarsdottir SE, Indridason OS, Palsson R, Edvardsson VO (2020) Stone recurrence among childhood kidney stone formers: results of a nationwide study in iceland. Urolithiasis. https://doi.org/10.1007/s00240-020-01179-6
Wang Z, Zhang Y, Zhang J, Deng Q, Liang H (2021) Recent advances on the mechanisms of kidney stone formation (review). Int J Mol Med. https://doi.org/10.3892/ijmm.2021.4982
Daudon M, Jungers P, Bazin D, Williams JC (2018) Recurrence rates of urinary calculi according to stone composition and morphology. Urolithiasis. https://doi.org/10.1007/s00240-018-1043-0
Daudon M, Dessombz A, Frochot V, Letavernier E, Haymann J, Jungers P, Bazin D (2016) Comprehensive morpho-constitutional analysis of urinary stones improves etiological diagnosis and therapeutic strategy of nephrolithiasis. C R Chim. https://doi.org/10.1016/j.crci.2016.05.008
Baowaidan F, Zugail AS, Lyoubi Y, Culty T, Lebdai S, Brassart E, Bigot P (2022) Incidence and risk factors for urolithiasis recurrence after endourological management of kidney stones: a retrospective single-centre study. Prog Urol. https://doi.org/10.1016/j.purol.2022.02.010
Ding Q, Ouyang J, Fan B, Cao C, Fan Z, Ding L, Li F, Tu W, Jin X, Wang J, Shi Y (2019) Association between dyslipidemia and nephrolithiasis risk in a chinese population. Urol Int. https://doi.org/10.1159/000496208
Otto BJ, Bozorgmehri S, Kuo J, Canales M, Bird VG, Canales B (2017) Age, body mass index, and gender predict 24-hour urine parameters in recurrent idiopathic calcium oxalate stone formers. J Endourol. https://doi.org/10.1089/end.2017.0352
Wang K, Ge J, Han W, Wang D, Zhao Y, Shen Y, Chen J, Chen D, Wu J, Shen N, Zhu S, Xue B, Xu X (2022) Risk factors for kidney stone disease recurrence: a comprehensive meta-analysis. BMC Urol. https://doi.org/10.1186/s12894-022-01017-4
Thongprayoon C, Krambeck AE, Rule AD (2020) Determining the true burden of kidney stone disease. Nat Rev Nephrol. https://doi.org/10.1038/s41581-020-0320-7
Skolarikos A, Straub M, Knoll T, Sarica K, Seitz C, Petřík A, Türk C (2015) Metabolic evaluation and recurrence prevention for urinary stone patients: eau guidelines. Eur Urol. https://doi.org/10.1016/j.eururo.2014.10.029
Tiselius H (2016) Metabolic risk-evaluation and prevention of recurrence in stone disease: does it make sense? Urolithiasis. https://doi.org/10.1007/s00240-015-0840-y
Alhamzawi R, Alhamzawi A, Mohammad Ali HT (2019) New gibbs sampling methods for bayesian regularized quantile regression. Comput Biol Med. https://doi.org/10.1016/j.compbiomed.2019.05.011
Meurer WJ, Tolles J (2017) Logistic regression diagnostics: understanding how well a model predicts outcomes. JAMA. https://doi.org/10.1001/jama.2016.20441
Park SY (2018) Nomogram: an analogue tool to deliver digital knowledge. J Thoracic Cardiovasc Surg. https://doi.org/10.1016/j.jtcvs.2017.12.107
Ang X, Jiang Y, Cai Z, Zhou Q, Li M, Zhang B, Chen W, Chen L, Zhang X (2021) A nomogram for bladder pain syndrome/interstitial cystitis based on netrin-1. Int Urol Nephrol. https://doi.org/10.1007/s11255-021-03084-2
Van Calster B, Wynants L, Verbeek JFM, Verbakel JY, Christodoulou E, Vickers AJ, Roobol MJ, Steyerberg EW (2018) Reporting and interpreting decision curve analysis: a guide for investigators. Eur Urol. https://doi.org/10.1016/j.eururo.2018.08.038
Soghra R, Armin R, Jeffrey IM, Fatemeh M, Yekta R, Manouchehr N, Alireza E (2021) Ldl/apo b ratio predict coronary heart disease in type 2 diabetes independent of ascvd risk score: a case-cohort study. Nutr Metab Cardiovasc Dis. https://doi.org/10.1016/j.numecd.2021.01.013
Acknowledgements
We were supported by the Natural Science Foundation of Anhui Province (1908085MH246), and the National Natural Science Foundation of China (82070724).
Author information
Authors and Affiliations
Contributions
KX and professor Hao were in charge of designing the project, KX and YX were in charge of writing, KX and QQ were in charge of statistical analysis, QH, JZ, and RY were in charge of collecting data. All the authors reviewed the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing financial interests.
Ethical approval
This article was a retrospective study, and supported by the Ethics Committee of the First Affiliated Hospital of Anhui Medical University, the ethical batch number was Quick-PJ2022-14-32. Patient consent were not required in accordance with local or national guidelines.
Consent for publication
All authors supported the publication of manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
11255_2023_3698_MOESM1_ESM.tif
Supplementary file1 Urea, creatinine (Cr), cystatin C, serum phosphorus (P), apo B, and urine pH expression levels in the stone recurrence and non-recurrence groups. A-E. The expression level of urea, creatinine (Cr), cystatin C, apo B, and urine pH were higher in stone recurrence group than stone non-recurrence group; F. Serum phosphorus (P) levels were lower in stone recurrence group than stone non-recurrence group (TIF 1885 KB)
11255_2023_3698_MOESM2_ESM.tif
Supplementary file2 Nomogram of upper urinary tract stones prediction model including serum creatinine and serum phosphate as mg/dl (TIF 17276 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xia, K., Xu, Y., Qi, Q. et al. Establishment of a new predictive model for the recurrence of upper urinary tract stones. Int Urol Nephrol 55, 2411–2420 (2023). https://doi.org/10.1007/s11255-023-03698-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-023-03698-8