Abstract
Objective
To establish a prognostic nomogram for PSA-incongruent low-risk prostate cancer (PCa) patients (Gleason score 6 and clinical stage T2a) at diagnosis and treated with radical prostatectomy (RP), based on clinical and pathological metrics.
Methods
In total, 217 patients diagnosed with PCa were included in this study. All patients had a Gleason score of 6 (GS6) in biopsy, had clinical T2a before surgery and were treated with RP. Biochemical progression-free survival (bPFS) was analyzed using the Kaplan–Meier method. Univariate and multivariate analyses were used to determine prognostic factors related to bPFS. A prognostic nomogram was established based on factors that were significant in the multivariate analyses.
Results
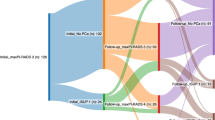
The median bPFS had a significant difference in the subgroup of PSA at diagnosis (‘ < 10 ng/mL’: 71.698 [67.549–75.847] vs ‘10–20 ng/mL’: 71.038 [66.220–75.857] vs ‘ ≥ 20 ng/mL’: 26.746 [12.384–41.108] months [Log Rank P < 0.001]), the subgroup of T stage upgrade (Negative: 70.016 [65.846–74.187] vs ‘T2b/c’: 69.183 [63.544–74.822] vs ‘T3/4’: 32.235 [11.877–52.593] months [Log Rank P < 0.001]) and the subgroup of Gleason score upgrade (Negative: 72.63 [69.096–76.163] vs ‘3 + 4’: 68.393 [62.243–74.543] vs ‘4 + 3’: 41.427 [27.517–55.336] vs ‘ ≥ 8’: 28.291 [7.527–49.055] [Log Rank P < 0.001]). PSA at diagnoses (Hazard Ratio (HR) 1.027, 95% CI 1.015–1.039, P < 0.001), T stage upgrade (HR 2.116, 95% CI 1.083–4.133, P = 0.028), and Gleason score upgrade (HR 2.831, 95% CI 1.892–4.237, P < 0.001) were identified as independent predictors with significance in multivariable Cox regression analysis. A nomogram was established based on these three factors.
Conclusions
Our study indicated that PSA-incongruent low-risk PCa patients (PSA with 10–20 ng/mL) had a similar prognosis to those with real low-risk PCa (PSA < 10 ng/mL) in the D’ Amico criteria. We also established a nomogram based on three significant prognostic factors, including PSA at diagnosis, T stage upgrade, and Gleason score upgrade, which were associated with clinical outcomes in prostate cancer patients with GS6 and T2a after surgery.


Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
D’Amico AV, Whittington R, Malkowicz SB, Schultz D, Blank K, Broderick GA, Tomaszewski JE, Renshaw AA, Kaplan I, Beard CJ et al (1998) Biochemical outcome after radical prostatectomy, external beam radiation therapy, or interstitial radiation therapy for clinically localized prostate cancer. JAMA 280(11):969–974
Mohler JL, Armstrong AJ, Bahnson RR, D’Amico AV, Davis BJ, Eastham JA, Enke CA, Farrington TA, Higano CS, Horwitz EM et al (2016) Prostate cancer, version 1.2016. J Natl Compr Cancer Netw JNCCN 14(1):19–30
Gnanapragasam VJ, Lophatananon A, Wright KA, Muir KR, Gavin A, Greenberg DC (2016) Improving clinical risk stratification at diagnosis in primary prostate cancer: a prognostic modelling study. PLoS Med 13(8):e1002063
Zelic R, Garmo H, Zugna D, Stattin P, Richiardi L, Akre O, Pettersson A (2020) Predicting prostate cancer death with different pretreatment risk stratification tools: a head-to-head comparison in a nationwide cohort study. Eur Urol 77(2):180–188
Walz J, Joniau S, Chun FK, Isbarn H, Jeldres C, Yossepowitch O, Chao-Yu H, Klein EA, Scardino PT, Reuther A et al (2011) Pathological results and rates of treatment failure in high-risk prostate cancer patients after radical prostatectomy. BJU Int 107(5):765–770
D’Amico AV, Cote K, Loffredo M, Renshaw AA, Chen MH (2003) Pretreatment predictors of time to cancer specific death after prostate specific antigen failure. J Urol 169(4):1320–1324
Hernandez DJ, Nielsen ME, Han M, Partin AW (2007) Contemporary evaluation of the D’amico risk classification of prostate cancer. Urology 70(5):931–935
Duffy MJ (2020) Biomarkers for prostate cancer: prostate-specific antigen and beyond. Clin Chem Lab Med 58(3):326–339
Zhang L, Yang BX, Zhang HT, Wang JG, Wang HL, Zhao XJ (2011) Prostate cancer: an emerging threat to the health of aging men in Asia. Asian J Androl 13(4):574–578
Olumi AF, Richie JP, Schultz DJ, D’Amico AV (2000) Calculated volume of prostate cancer identifies patients with clinical stage T1C disease at high risk of biochemical recurrence after radical prostatectomy: a preliminary study. Urology 56(2):273–277
Tilki D, Mandel P, Karakiewicz PI, Heinze A, Huland H, Graefen M, Knipper S (2020) The impact of very high initial PSA on oncological outcomes after radical prostatectomy for clinically localized prostate cancer. Urol Oncol 38(5):379–385
Preisser F, Bandini M, Nazzani S, Mazzone E, Marchioni M, Tian Z, Chun FKH, Saad F, Briganti A, Haese A et al (2020) Development and validation of a lookup table for the prediction of metastatic prostate cancer according to prostatic-specific antigen value, clinical tumor stage, and gleason grade groups. Eur Urol Oncol 3(5):631–639
Budäus L, Isbarn H, Eichelberg C, Lughezzani G, Sun M, Perrotte P, Chun FK, Salomon G, Steuber T, Köllermann J et al (2010) Biochemical recurrence after radical prostatectomy: multiplicative interaction between surgical margin status and pathological stage. J Urol 184(4):1341–1346
Han M, Partin AW, Zahurak M, Piantadosi S, Epstein JI, Walsh PC (2003) Biochemical (prostate specific antigen) recurrence probability following radical prostatectomy for clinically localized prostate cancer. J Urol 169(2):517–523
Tollefson MK, Karnes RJ, Rangel LJ, Bergstralh EJ, Boorjian SA (2013) The impact of clinical stage on prostate cancer survival following radical prostatectomy. J Urol 189(5):1707–1712
Chun FK, Briganti A, Lebeau T, Fradet V, Steuber T, Walz J, Schlomm T, Eichelberg C, Haese A, Erbersdobler A et al (2006) The 2002 AJCC pT2 substages confer no prognostic information on the rate of biochemical recurrence after radical prostatectomy. Eur Urol 49(2):273–278 (discussion 278-279)
Fine SW, Epstein JI (2008) A contemporary study correlating prostate needle biopsy and radical prostatectomy Gleason score. J Urol 179(4):1335–1338 (discussion 1338-1339)
Epstein JI, Feng Z, Trock BJ, Pierorazio PM (2012) Upgrading and downgrading of prostate cancer from biopsy to radical prostatectomy: incidence and predictive factors using the modified Gleason grading system and factoring in tertiary grades. Eur Urol 61(5):1019–1024
Epstein JI, Zelefsky MJ, Sjoberg DD, Nelson JB, Egevad L, Magi-Galluzzi C, Vickers AJ, Parwani AV, Reuter VE, Fine SW et al (2016) A contemporary prostate cancer grading system: a validated alternative to the gleason score. Eur Urol 69(3):428–435
Acknowledgements
This study was supported by the Clinical Research Plan of the SHDC (No. SHDC2020CR3014A).
Author information
Authors and Affiliations
Contributions
YW and YZ: contributed to the design and implementation of the research, YW and JP to the analysis of the results and to the writing of the manuscript. WX: conceived the original and supervised the project.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that there are no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, Y., Zhu, Y., Fan, L. et al. The prognostic nomogram for PSA-incongruent low-risk prostate cancer treated by radical prostatectomy. Int Urol Nephrol 55, 1447–1452 (2023). https://doi.org/10.1007/s11255-023-03560-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-023-03560-x