Abstract
Purpose
Post-operative pulmonary failure is a major complication of nephrectomy that may lead to severe morbidity and mortality. Hence, we aimed to derive a nephrectomy-specific post-operative respiratory failure index.
Methods
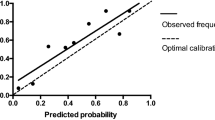
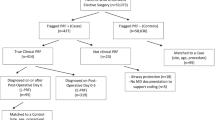
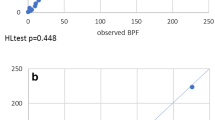
Our cohort was derived from The American College of Surgeons—National Surgical Quality Improvement Program database between 2005 and 2019. The outcome of interest was post-operative respiratory failure (PRF) defined as any incidence of unplanned intubation post-operatively or requiring mechanical ventilation post-operatively for a period > 48 h. A multivariable logistic regression model was constructed, and model calibration and performance were assessed using a ROC analysis and the Hosmer–Lemeshow test. Finally, we derived the nephrectomy-specific respiratory failure (NSRF) index and compared it to Gupta’s index.
Results
Seventy-nine thousand five hundred and twenty-three patients underwent nephrectomy between the years 2005 and 2019 of which nine hundred and sixty-two patients developed PRF. The final NSRF model encompassed ten variables: age, smoking status, American society of anesthesiology class, abnormal creatinine (≥ 1.5 mg/dL), anemia (< 36%), functional health status, chronic obstructive pulmonary disease, surgical approach, emergency case, and obesity (≥ 40 kg/m2). The NSRF ROC analysis provided C-statistic = 0.78, calibration R2 = 0.99, and proper goodness of fit. In comparison, the C-statistics of Gupta’s index was found to be 0.71 (p value < 0.001).
Conclusion
The NSRF is a procedure tailored index for predicting post-operative respiratory failure. It is a valuable tool in the pre-operative evaluation setting that can help identify high-risk patients who will require additional respiratory evaluation and preparation for their surgery.



Similar content being viewed by others
Data availability
The (ACS-NSQIP) data are subject to a data use agreement. To access the dataset, a request to the ACS-NSQIP participant-use form should be placed at the following link (https://www.facs.org/quality-programs/acs-nsqip/participant-use). The American University of Beirut Medical Center is enrolled in ACS-NSQIP as a participating center. As such, the data were made available by the ACS-NSQIP center and the AUBMC Department of Surgery after signing the data use agreement.
References
Kheterpal E, Taneja SS (2012) Partial nephrectomy: contemporary outcomes candidate selection and surgical approach. Urol Clin North Am. https://doi.org/10.1016/j.ucl.2012.02.003
Zelhof B, McIntyre IG, Fowler SM et al (2016) Nephrectomy for benign disease in the UK: results from the British association of urological surgeons nephrectomy database. BJU Int. https://doi.org/10.1111/bju.13141
Asimakopoulos AD, Miano R, Annino F et al (2014) Robotic radical nephrectomy for renal cell carcinoma: a systematic review. BMC Urol 14(1):75
Ashrafi AN, Gill IS (2020) Minimally invasive radical nephrectomy: a contemporary review. Transl Androl Urol. https://doi.org/10.21037/tau-2019-suc-16
Shuford MD, McDougall EM, Chang SS et al (2004) Complications of contemporary radical nephrectomy: comparison of open vs laparoscopic approach. Urol Oncol. https://doi.org/10.1016/s1078-1439(03)00137-600000000o
Tanagho YS, Kaouk JH, Allaf ME et al (2013) Perioperative complications of robot-assisted partial nephrectomy: analysis of 886 patients at 5 United States centers. Urology 81:573–580. https://doi.org/10.1016/j.urology.2012.10.067
Goldwag J, Harris A, Bettis AD (2021) 5-Item modified frailty index as a preoperative predictor of morbidity following minimally invasive partial nephrectomy. Urology. https://doi.org/10.1016/j.urology.2021.05.050
Nasrallah AA, Dakik HA, Abou Heidar NF et al (2022) Major adverse cardiovascular events following partial nephrectomy: a procedure-specific risk index. Ther Adv Urol. https://doi.org/10.1177/17562872221084847
Wong DH, Weber EC, Schell MJ et al (1995) Factors associated with postoperative pulmonary complications in patients with severe chronic obstructive pulmonary disease. Anesth Analg. https://doi.org/10.1097/00000539-199502000-00013
Hall JC, Tarala RA, Hall JL et al (1991) A multivariate analysis of the risk of pulmonary complications after laparotomy. Chest. https://doi.org/10.1378/chest.99.4.923
Calligaro KD, Azurin DJ, Dougherty MJ et al (1993) Pulmonary( risk factors of elective abdominal aortic surgery. J Vasc Surg 18:914–920
Carey K, Stefos T, Shibei Z et al (2011) Excess costs attributable to postoperative complications. Med Care Res Rev 68:490–503. https://doi.org/10.1177/1077558710396378
Khan NA, Quan H, Bugar JM et al (2006) Association of postoperative complications with hospital costs and length of stay in a tertiary care center. J Gen Intern Med 21:177–180. https://doi.org/10.1111/j.1525-1497.2006.00319.x
Lawrence VA, Hilsenbeck SG, Noveck H et al (2002) Medical complications and outcomes after hip fracture repair. Arch Intern Med 162:2053–2057. https://doi.org/10.1001/archinte.162.18.2053
Rosen AK, Geraci JM, Ash AS et al (1992) Postoperative adverse events of common surgical procedures in the medicare population. Med Care 30:753–765
Escarce JJ, Shea JA, Chen W et al (1995) Outcomes of open cholecystectomy in the elderly: a longitudinal analysis of 21,000 cases in the prelaparoscopic era. Surgery 117:156–164. https://doi.org/10.1016/S0039-6060(05)80079-0
Pedersen T (1994) Complications and death following anaesthesia. a prospective study with special reference to the influence of patient-, anaesthesia-, and surgery-related risk factors. Dan Med Bull 41:319–331
Canet J., Gallart L. (2013) Predicting postoperative pulmonary complications in the general population. Current Opinion in Anesthesiology 26
Nijbroek SG, Schultz MJ and Hemmes SNT. (2019) Prediction of postoperative pulmonary complications. Current Opinion in Anesthesiology 32.
Brooks-Brunn JA (1997) Predictors of postoperative pulmonary complications following abdominal surgery. Chest 111:564–571. https://doi.org/10.1378/chest.111.3.564
Gupta H, Gupta PK, Fang X et al (2011) Development and validation of a risk calculator predicting postoperative respiratory failure. Chest 140:1207–1215. https://doi.org/10.1378/chest.11-0466
ACS NSQIP. User Guide for the 2019 ACS NSQIP Participant Use Data File. 2019
Hua M, Brady JE, Li G (2012) A scoring system to predict unplanned intubation in patients having undergone major surgical procedures. Anesth Analg 115:88–94. https://doi.org/10.1213/ANE.0b013e318257012b
Arozullah AM, Daley J, Henderson WG et al (2000) Multifactorial risk index for predicting postoperative respiratory failure in men after major noncardiac surgery. the national veterans administration surgical quality improvement program. Ann Surg 232:242–253
Johnson AP, Altmark RE, Weinstein MS et al (2017) Predicting the risk of postoperative respiratory failure in elective abdominal and vascular operations using the national surgical quality improvement program (nsqip) participant use data file. Ann Surg 266:968–974
Johnson RG, Arozullah AM, Neumayer L et al (2007) Multivariable predictors of postoperative respiratory failure after general and vascular surgery: results from the patient safety in surgery study. J Am Coll Surg 204:1188–1198. https://doi.org/10.1016/j.jamcollsurg.2007.02.070
Fischer JP, Shang EK, Butler CE et al (2013) Validated model for predicting postoperative respiratory failure: analysis of 1706 abdominal wall reconstructions. Plast Reconstr Surg. https://doi.org/10.1097/PRS.0b013e3182a4c442
Hassan WM, Al-Dbass A, Al-Ayadhi L et al (2022) Discriminant analysis and binary logistic regression enable more accurate prediction of autism spectrum disorder than principal component analysis. Sci Rep 12:3764. https://doi.org/10.1038/s41598-022-07829-6
Ayoub CH, El-Asmar JM, Abou Heidar NF et al (2022) A novel radical prostatectomy specific index (PSI) for the prediction of major cardiovascular events following surgery. Int Urol Nephrol 54:3069–3078. https://doi.org/10.1007/s11255-022-03293-3
Rassi A Jr, Rassi A, Little WC et al (2006) Development and validation of a risk score for predicting death in chagas’ heart disease. N Engl J Med 355:799–808. https://doi.org/10.1056/NEJMoa053241
Pannucci CJ, Shanks A, Moote MJ et al (2012) Identifying patients at high risk for venous thromboembolism requiring treatment after outpatient surgery. Ann Surg 255:1093–1099. https://doi.org/10.1097/SLA.0b013e3182519ccf
Sameed M, Choi H, Auron M et al (2021) Preoperative pulmonary risk assessment. Respir Care 66:1150–1166. https://doi.org/10.4187/respcare.09154
Canet J, Gallart L (2014) Postoperative respiratory failure: pathogenesis, prediction, and prevention. Curr Opin Crit Care 20:56–62. https://doi.org/10.1097/mcc.0000000000000045
Hughes MJ, Hackney RJ, Lamb PJ et al (2019) Prehabilitation before major abdominal surgery: a systematic review and meta-analysis. World J Surg 43:1661–1668. https://doi.org/10.1007/s00268-019-04950-y
Pierorazio PM, Johnson MH, Ball MW et al (2015) Five-year analysis of a multi-institutional prospective clinical trial of delayed intervention and surveillance for small renal masses: the DISSRM registry. Eur Urol 68:408–415
Jewett MA, Mattar K, Basiuk J et al (2011) Active surveillance of small renal masses: progression patterns of early stage kidney cancer. Eur Urol 60:39–44
Uhlig J, Strauss A, Rücker G et al (2019) Partial nephrectomy versus ablative techniques for small renal masses: a systematic review and network meta-analysis. Eur Radiol. https://doi.org/10.1007/s00330-018-5660-3
Forbes A, Gallagher H (2020) Chronic kidney disease in adults: assessment and management. Clin Med (Lond) 20:128–132. https://doi.org/10.7861/clinmed.cg.20.2
Webster AC, Nagler EV, Morton RL et al (2017) Chronic kidney disease. Lancet 389:1238–1252. https://doi.org/10.1016/s0140-6736(16)32064-5
Upasani A, Barnacle A, Roebuck D et al (2017) Combination of surgical drainage and renal artery embolization: an alternative treatment for Xanthogranulomatous Pyelonephritis. Cardiovasc Intervent Radiol 40:470–473
Funding
No funding was received to assist with the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
CHA: conceptualized the study, retrieved, and analyzed the data, and wrote/edited the manuscript. JMA: conceptualized the study, wrote/edited the manuscript. AEA wrote/edited the manuscript. ADE, AC/L, ElK: wrote/edited the manuscript. HT: helped in retrieval and analyzed the data. A.EHVC: project conception/design, manuscript writing/editing. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors have no competing interests to declare that are relevant to the content of this article.
Ethical approval and consent to participate
The de-identified database (ACS-NSQIP) does not constitute human subject research; therefore, no consent to participate or institutional review board (IRB) approval was required or attained.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ayoub, C.H., El-Asmar, J.M., El-Achkar, A. et al. A novel nephrectomy-specific respiratory failure index using the ACS-NSQIP dataset. Int Urol Nephrol 55, 813–822 (2023). https://doi.org/10.1007/s11255-023-03507-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-023-03507-2