Abstract
Introduction
To report the feasibility, efficacy and safety of decellularized dermal strip as a sling material in the pudendal denervated stress urinary incontinence (SUI) in an animal model.
Methods
Thirty female Sprague–Dawley rats were randomly allocated into three equal groups (n = 10). In group 1, rats underwent bilateral pudendal nerve transection (BPNT) with no vaginal sling placement. Group 2 underwent BPNT with homologous decellularized dermal strip placement as vaginal sling 12 weeks later. Group 3 was considered as controls to evaluate baseline leak point pressure (LPP). Leak point pressure was measured 18 weeks after BPNT in group 1 and 6 weeks after sling implantation in group 2. Sling and sphincter samples were prepared for histological and immunohistochemistry (IHC) staining.
Results
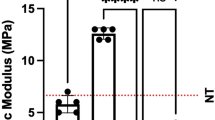
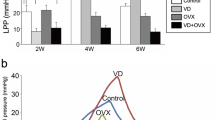
H&E staining of external urethral sphincter showed decrease in striated muscle layer in group 1 (BPNT) compared to control confirmed by desmin staining (45 % decrease in desmin staining). Sling implantation caused significant increase in mean LPP from 11.6 ± 2.8 cm H2O in group 1 (BPNT) to 27.2 ± 5.4 cm H2O in group 2 (BPNT/sling). There was no significant difference between LPP after the sling placement in group 2 and LPP in group 3 (27.2 ± 5.4 cm H2O vs. 27.6 ± 5.9, P = 0.832). IHC staining was positive for α-SMA and CD34.
Conclusions
Based on present results, this dermal strip could be considered as a potential sling material for treatment of SUI in this animal model. This study provides the basis for further investigation of the efficacy of biological decellularized scaffold as suburethral sling material.




Similar content being viewed by others
References
Norton P, Brubaker L (2006) Urinary incontinence in women. Lancet 367(9504):57–67
Austin PF, Bauer SB, Bower W, Chase J, Franco I, Hoebeke P et al (2014) The standardization of terminology of lower urinary tract function in children and adolescents: update report from the Standardization Committee of the International Children’s Continence Society. J Urol 191(6):1863–1865
Kim HL, Gerber GS, Patel RV, Hollowell CM, Bales GT (2001) Practice patterns in the treatment of female urinary incontinence: a postal and internet survey. Urology 57(1):45–48
Bartley JM, Sirls LT, Killinger KA, Boura JA (2015) Secondary surgery after vaginal prolapse repair with mesh is more common for stress incontinence and voiding dysfunction than for mesh problems or prolapse recurrence. Int Urol Nephrol 47(4):609–615. doi:10.1007/s11255-015-0930-3
Falconer C, Soderberg M, Blomgren B, Ulmsten U (2001) Influence of different sling materials on connective tissue metabolism in stress urinary incontinent women. Int Urogynecol J Pelvic Floor Dysfunct 12(Suppl 2):S19–S23
Birch C, Fynes MM (2002) The role of synthetic and biological prostheses in reconstructive pelvic floor surgery. Curr Opin Obstet Gynecol 14(5):527–535
Huebner M, Hsu Y, Fenner DE (2006) The use of graft materials in vaginal pelvic floor surgery. Int J Gynaecol Obstet 92(3):279–288
Birch C (2005) The use of prosthetics in pelvic reconstructive surgery. Best Pract Res Clin Obstet Gynaecol 19(6):979–991
Soergel TM, Shott S, Heit M (2001) Poor surgical outcomes after fascia lata allograft slings. Int Urogynecol J Pelvic Floor Dysfunct 12(4):247–253
Ng CS, Rackley RR, Appell RA (2001) Incidence of concomitant procedures for pelvic organ prolapse and reconstruction in women who undergo surgery for stress urinary incontinence. Urology 57(5):911–913
Onur R, Singla A, Kobashi KC (2008) Comparison of solvent-dehydrated allograft dermis and autograft rectus fascia for pubovaginal sling: questionnaire-based analysis. Int Urol Nephrol 40(1):45–49
Huang YH, Lin AT, Chen KK, Pan CC, Chang LS (2001) High failure rate using allograft fascia lata in pubovaginal sling surgery for female stress urinary incontinence. Urology 58(6):943–946
Cannon TW, Sweeney DD, Conway DA, Kamo I, Yoshimura N, Sacks M et al (2005) A tissue-engineered suburethral sling in an animal model of stress urinary incontinence. BJU Int 96(4):664–669
Kim IG, Piao S, Hong SH, Kim SW, Hwang TK, Oh SH et al (2011) The effect of a bioactive tissue-engineered sling in a rat of stress incontinence model. J Biomed Mater Res A 100(2):286–292
VandeVord PJ, Broadrick KM, Krishnamurthy B, Singla AK (2010) A comparative study evaluating the in vivo incorporation of biological sling materials. Urology 75(5):1228–1233
Kajbafzadeh AM, Mohammadinejad P, Hojjat A, Nezami BG, Talab SS, Emami H et al (2012) The timing of established detrusor hyperreflexia in a rat model of neuropathic bladder. J Surg Res 178(1):346–351
De Spiegelaere W, Cornillie P, Casteleyn C, Burvenich C, Van den Broeck W (2010) Detection of hypoxia inducible factors and angiogenic growth factors during foetal endochondral and intramembranous ossification. Anat Histol Embryol 39(4):376–384
Baessler K (2012) Do we need meshes in pelvic floor reconstruction? World J Urol 30(4):479–486
Woodruff AJ, Cole EE, Dmochowski RR, Scarpero HM, Beckman EN, Winters JC (2008) Histologic comparison of pubovaginal sling graft materials: a comparative study. Urology 72(1):85–89
Brown SL, Govier FE (2000) Cadaveric versus autologous fascia lata for the pubovaginal sling: surgical outcome and patient satisfaction. J Urol 164(5):1633–1637
Crapo PM, Gilbert TW, Badylak SF (2011) An overview of tissue and whole organ decellularization processes. Biomaterials 32(12):3233–3243
Wainwright D, Madden M, Luterman A, Hunt J, Monafo W, Heimbach D et al (1996) Clinical evaluation of an acellular allograft dermal matrix in full-thickness burns. J Burn Care Rehabil 17(2):124–136
Clark JM, Saffold SH, Israel JM (2003) Decellularized dermal grafting in cleft palate repair. Arch Facial Plast Surg 5(1):40–44 (discussion 45)
Turner NJ, Badylak SF (2013) Biologic scaffolds for musculotendinous tissue repair. Eur Cell Mater 25:130–143
Bindingnavele V, Gaon M, Ota KS, Kulber DA, Lee DJ (2007) Use of acellular cadaveric dermis and tissue expansion in postmastectomy breast reconstruction. J Plast Reconstr Aesthet Surg 60(11):1214–1218
Venouziou AI, Kokkalis ZT, Sotereanos DG (2013) Human dermal allograft interposition for the reconstruction of massive irreparable rotator cuff tears. Am J Orthop (Belle Mead NJ) 42(2):63–70
Branch JP (2011) A tendon graft weave using an acellular dermal matrix for repair of the Achilles tendon and other foot and ankle tendons. J Foot Ankle Surg 50(2):257–265
Conway DA, Kamo I, Yoshimura N, Chancellor MB, Cannon TW (2005) Comparison of leak point pressure methods in an animal model of stress urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct 16(5):359–363
Raghavan D, Kropp BP, Lin HK, Zhang Y, Cowan R, Madihally SV (2005) Physical characteristics of small intestinal submucosa scaffolds are location-dependent. J Biomed Mater Res A 73(1):90–96
Kropp BP, Cheng EY, Lin HK, Zhang Y (2004) Reliable and reproducible bladder regeneration using unseeded distal small intestinal submucosa. J Urol 172(4 Pt 2):1710–1713
Kim RJ, Kerns JM, Liu S, Nagel T, Zaszczurynski P, Lin DL et al (2007) Striated muscle and nerve fascicle distribution in the female raturethral sphincter. Anat Rec 290(2):145–154
Hijaz A, Bena J, Daneshgari F (2005) Long-term efficacy of a vaginal sling procedure in a rat model of stress urinary incontinence. J Urol 173(5):1817–1819
Onur R, Singla A (2005) Solvent-dehydrated cadaveric dermis: a new allograft for pubovaginal sling surgery. Int J Urol 12(9):801–805
Conflict of interest
Abdol-Mohammad Kajbafzadeh, Sarah Mozafarpour, Seyedeh Sanam Ladi Seyedian, Reza Khorramirouz and Haleh Nasser Hojjati declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kajbafzadeh, AM., Mozafarpour, S., Ladi Seyedian, S. et al. Decellularized dermal strip as a suburethral sling in a rat model of stress urinary incontinence. Int Urol Nephrol 47, 1303–1310 (2015). https://doi.org/10.1007/s11255-015-1025-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-015-1025-x