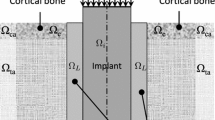
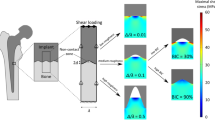
Dental implants are becoming an increasingly important part of modern dental treatment. Developing an optimal implant surface design can improve osseointegration. Promising to increase the rate of osseointegration is the use of extracorporeal shock wave therapy, which has proven itself for the treatment of fractures, bone defects, and bone tissue regeneration during surgery and arthroplasty. This work aims at a numerical investigation of the effects of low-energy shock wave therapy of various intensities on the mechanical behavior of dental implants and surrounding bone tissues, taking into account the physiological characteristics in the area of dental implant placement. Modeling was carried out using the method of movable cellular automata. The results of computer simulation showed that the conditions for the regeneration of bone tissues at the near-contact zone with the implant of the jaw segment are created by a shock wave with intensity greater than 0.1 mJ/mm2.
Similar content being viewed by others
References
J. S. Colombo, S. Satoshi, J. Okazaki, et al., J. Dent., 40 (4), 338–46 (2012); DOI: https://doi.org/10.1016/j.jdent.2012.01.010.
C. P. Hao, N. J. Cao, Y. H. Zhu, and W. Wang, Sci. Rep., 11, 13849 (2021); DOI: https://doi.org/10.1038/s41598-021-93307-4.
W. P. Song, X. H. Ma, Y. X. Sun, et al., Med. Hypotheses, 145, 110294 (2020); DOI: https://doi.org/10.1016/j.mehy.2020.110294.
E. V. Shilko, A. S. Grigoriev, and A. Yu. Smolin, FU Mech. Eng., 19, 7–22 (2021); DOI: https://doi.org/10.22190/FUME201221012S.
S. G. Psakhie, A. V. Dimaki, E. V. Shilko, and S. V. Astafurov, Int. J. Numer. Methods Eng., 106, 623–643 (2016); DOI: https://doi.org/10.1002/nme.5134.
G. M. Eremina and A. Yu. Smolin, Comput. Methods Programs Biomed., 200, 105929 (2021); DOI: https://doi.org/10.1016/j.cmpb.2021.105929.
G. M. Eremina and A. Yu. Smolin, Rus. J. Biomech., 1, 32–45 (2023); DOI: https://doi.org/10.15593/RZhBiomech/2023.1.04.
D. R. Carter and W. C. Hayes, J. Bone Joint Surg., 59(7), 954–962 (1977).
S. C. Cowin and S. B. Doty, Tissue Mechanics, Springer, New York (2007).
K. A. Mann and M. A. Miller, Comput. Methods Biomech. Biomed. Engin., 17(16), 1809–1820 (2014); DOI: https://doi.org/10.1080/10255842.2013.767336.
G. Lewis, J. Biomed. Mater. Res., 38, 155–182 (1977); DOI: https://doi.org/10.1002/(sici)1097-4636(199722)38:2<155::aidjbm10>3.0.co;2-c.
Starbond Ni, https://scheftner.dental/starbond-ni-en.html (accessed on 26 July 2023).
P. Krakhmalev, G. Fredriksson, I. Yadroitsava, et al., Phys. Procedia, 83, 778–788 (2016); DOI: https://doi.org/10.1016/j.phpro.2016.08.080.
J. He, Z. Zeng, H. Li, and S.T. Wang, Mat. Des., 196, 109171 (2020); DOI: https://doi.org/10.1016/j.matdes.2020.109171.
S. Sathishkumar, A. Meka, D. Dawson, et al., J. Dent. Res., 87(7), 687–691 (2008); DOI: https://doi.org/10.1177/154405910808700703.
H. Hazan-Molina, Y. Gabet, I. Aizenbud, et al., Arch. Oral Biol., 134, 105327 (2022); DOI: https://doi.org/10.1016/j.archoralbio.2021.105327.
N. J. Giori, L. Ryd and D. R. Carter, J. Arthroplasty, 10(4), 514–522 (1995); DOI: https://doi.org/10.1016/s0883-5403(05)80154-8.
M. Wang, N. Yang and X. Wang, Med. Biol. Eng. Comput., 55(11), 1895–1914 (2017); DOI: https://doi.org/10.1007/s11517-017-1701-3.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Smolin, A.Y., Eremina, G.M. & Martyshina, I.P. Simulation of the Mechanical Behavior of a Dental Implant in Bone Tissue Under Shock Wave Treatment. Russ Phys J 66, 1310–1315 (2024). https://doi.org/10.1007/s11182-023-03077-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11182-023-03077-x