Abstract
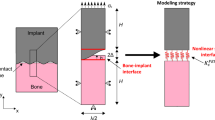
Inserting a titanium implant in the bone tissue may modify its physiological loading and therefore cause bone resorption, via a phenomenon called stress-shielding. The local stress field around the bone-implant interphase (BII) created under shear loading may be influenced by different parameters such as the bone-implant contact (BIC) ratio, the bone Young’s modulus, the implant roughness and the implant material. A 2-D finite element model was developed to model the BII and evaluate the impact of the aforementioned parameters. The implant roughness was described by a sinusoidal function (height 2Δ, wavelength λ), and different values of the BIC ratio were simulated. A heterogeneous distribution of the maximum shear stress was evidenced in the periprosthetic bone tissue, with high interfacial stress for low BIC ratios and low implant roughness and underloaded regions near the roughness valleys. Both phenomena may lead to stress-shielding-related effects, which were concentrated within a distance lower than 0.8λ from the implant surface. Choosing an implant material with mechanical properties matching those of bone tissue leads to a homogenized shear stress field and could help to prevent stress-shielding effects. Finally, the equivalent shear modulus of the BII was derived to replace its complex behavior with a simpler analytical model in future studies.
Graphical abstract
Schematic illustrations of the 2-D finite element model used in the present study and spatial variation of the maximal shear stress in the periprosthetic bone tissue for different implant roughness and bone-implant contact ratios.









Similar content being viewed by others
References
Abuhussein H, Pagni G, Rebaudi A, Wang HL (2010) The effect of thread pattern upon implant osseointegration. Clin Oral Implants Res 21:129–136
Albrektsson T, Brånemark PI, Hansson H-A, Lindström J (1981) Osseointegrated titanium implants: requirements for ensuring a long-lasting, direct bone-to-implant anchorage in man. Acta Orthop Scand 52:155–70
Alla RK, Ginjupalli K, Upadhya N, Mohammed S, Sekar R, Ravi R (2011) Surface roughness of implants: a review. Trends Biomater Artif Org 25:112–118
Arabnejad S, Johnston B, Tanzer M, Pasini D (2017) Fully porous 3D printed titanium femoral stem to reduce stress-shielding following total hip arthroplasty. J Orthop Res 35:1774–1783
Au AG, James Raso V, Liggins AB, Amirfazli A (2007) Contribution of loading conditions and material properties to stress shielding near the tibial component of total knee replacements. J Biomech 40:1410–1416
Bugbee WD, Culpepper WJ 2nd, Engh CA Jr, Engh CA Sr (1997) Long-term clinical consequences of stress-shielding after total hip arthroplasty without cement. J Bone Joint Surg Am 79:1007–1012
Buser D, Ingimarsson S, Dula K, Lussi A, Hirt H, Belser U (2002) Long-term stability of osseointegrated implants in augmented bone: a 5-year prospective study in partially edentulous patients. Int J Periodont Restor Dent 22:109–17
Chong DY, Hansen UN, Amis AA (2010) Analysis of bone-prosthesis interface micromotion for cementless tibial prosthesis fixation and the influence of loading conditions. J Biomech 43:1074–1080
Cole EW, Moulton SG, Gobezie R, Romeo AA, Walker JB, Lederman E et al (2020) Five-year radiographic evaluation of stress shielding with a press-fit standard length humeral stem. JSES Int 4:109–113
Completo A, Fonseca F, Simões JA (2008) Strain shielding in proximal tibia of stemmed knee prosthesis: experimental study. J Biomech 41:560–566
Duyck J, Corpas L, Vermeiren S, Ogawa T, Quirynen M, Vandamme K et al (2010) Histological, histomorphometrical, and radiological evaluation of an experimental implant design with a high insertion torque. Clin Oral Implants Res 21:877–884
Engh CA Jr, Young AM, Engh CA Sr, Hopper RH Jr (2003) Clinical consequences of stress shielding after porouscoated total hip arthroplasty. Clin Orthop Relat Res 417:157–63. https://doi.org/10.1097/01.blo.0000096825.67494.e3
Firoozbakhsh K, Aleyaasin M (1989) The effect of stress concentration on bone remodeling: theoretical predictions. J Biomech Eng 111:355–360
Fraulob M, Pang S, Le Cann S, Vayron R, Laurent-Brocq M, Todatry S et al (2020) Multimodal characterization of the bone-implant interface using Raman spectroscopy and nanoindentation. Med Eng Phys 84:60–67
Fraulob M, Vayron R, Le Cann S, Lecuelle B, Hériveaux Y, Albini Lomami H et al (2020) Quantitative ultrasound assessment of the influence of roughness and healing time on osseointegration phenomena. Sci Rep 10:21962
Fritsch A, Hellmich C (2007) ‘Universal’ microstructural patterns in cortical and trabecular, extracellular and extravascular bone materials: micromechanics-based prediction of anisotropic elasticity. J Theor Biol 244:597–620
Frost HM (2004) A 2003 update of bone physiology and Wolff’s Law for clinicians. Angle Orthod 74:3–15
Galloway F, Kahnt M, Ramm H, Worsley P, Zachow S, Nair P et al (2013) A large scale finite element study of a cementless osseointegrated tibial tray. J Biomech 46:1900–1906
Gao X, Fraulob M, Haïat G (2019) Biomechanical behaviours of the bone-implant interface: a review. J R Soc Interface 16:20190259
Gortchacow M, Wettstein M, Pioletti DP, Terrier A (2011) A new technique to measure micromotion distribution around a cementless femoral stem. J Biomech 44:557–560
Gupta S, Patil N, Solanki J, Singh R, Laller S (2015) Oral implant imaging: a review. Malays J Med Sci 22:7–17
Haïat G, Wang H-L, Brunski J (2014) Effects of biomechanical properties of the bone–implant interface on dental implant stability: from in silico approaches to the patient’s mouth. Annu Rev Biomed Eng 16:187–213
Hériveaux Y, Haïat G, Nguyen V-H (2020) Reflection of an ultrasonic wave on the bone-implant interface: comparison of two-dimensional and three-dimensional numerical models. J Acoust Soc Am 147:EL32–EL36. https://doi.org/10.1121/10.0000500
Hériveaux Y, Nguyen VH, Biwa S, Haïat G (2020) Analytical modeling of the interaction of an ultrasonic wave with a rough bone-implant interface. Ultrasonics 108:106223
Heriveaux Y, Nguyen VH, Brailovski V, Gorny C, Haiat G (2019) Reflection of an ultrasonic wave on the bone-implant interface: effect of the roughness parameters. J Acoust Soc Am 145:3370
Heriveaux Y, Nguyen VH, Haiat G (2018) Reflection of an ultrasonic wave on the bone-implant interface: a numerical study of the effect of the multiscale roughness. J Acoust Soc Am 144:488
Huiskes R, Weinans H, van Rietbergen B (1992) The relationship between stress shielding and bone resorption around total hip stems and the effects of flexible materials. Clin Orthop Relat Res 274:124–134
Immel K, Duong TX, Nguyen V-H, Haïat G, Sauer RA (2020) A modified Coulom, s law for the tangential debonding of osseointegrated implants. Biomech Model Mechanobiol 19:1091–1108
Jimenez R (2002) The radiology of orthopaedic implants. An Atlas of Techniques and Assessment. J Bone Joint Surg Am 84:514
Johansson CB, Albrektsson T (1987) Integration of screw implants in the rabbit: a 1-year follow-up of removal torque of titanium implants. Int J Oral Maxillofac Implants 2(2):69–75
Joshi MG, Advani SG, Miller F, Santare MH (2000) Analysis of a femoral hip prosthesis designed to reduce stress shielding. J Biomech 33:1655–1662
Kohli N, Stoddart JC, van Arkel RJ (2021) The limit of tolerable micromotion for implant osseointegration: a systematic review. Sci Rep 11:10797
Korabi R, Shemtov-Yona K, Dorogoy A, Rittel D (2017) The failure envelope concept applied to the bone-dental implant system. Sci Rep 7:2051
Kuiper J, Huiskes R (1997) The predictive value of stress shielding for quantification of adaptive bone resorption around hip replacements. J Biomech Eng 119:228–31
Kurniawan D, Nor FM, Lee HY, Lim JY (2012) Finite element analysis of bone-implant biomechanics: refinement through featuring various osseointegration conditions. Int J Oral Maxillofac Surg 41:1090–1096
Kusano T, Seki T, Higuchi Y, Takegami Y, Osawa Y, Ishiguro N (2018) Preoperative canal bone ratio is related to high-degree stress shielding: a minimum 5-year follow-up study of a proximally hydroxyapatite-coated straight tapered titanium femoral component. J Arthroplasty 33:1764–1769
Le Cann S, Tudisco E, Perdikouri C, Belfrage O, Kaestner A, Hall S, Tägil M, Isaksson H (2017) Characterization of the bone-metal implant interface by Digital Volume Correlation of in-situ loading using neutron tomography. J Mech Behav Biomed Mater 75:271–278. https://doi.org/10.1016/j.jmbbm.2017.07.001
Li M-J, Kung P-C, Chang Y-W, Tsou N-T (2020) Healing pattern analysis for dental implants using the mechano-regulatory tissue differentiation model. Int J Mol Sci 21:9205
Manikyamba YJB, Mc SS, Raju AVR, Rao B, Nair CK (2018) Implant thread designs: an overview
Mathieu V, Vayron R, Richard G, Lambert G, Naili S, Meningaud JP et al (2014) Biomechanical determinants of the stability of dental implants: influence of the bone-implant interface properties. J Biomech 47:3–13
Melnyk AD, Wen TL, Kingwell S, Chak JD, Singh V, Cripton PA et al (2012) Load transfer characteristics between posterior spinal implants and the lumbar spine under anterior shear loading: an in vitro investigation. Spine (Phila Pa 1976) 37:E1126-33
Michel A, Bosc R, Meningaud JP, Hernigou P, Haiat G (2016) Assessing the acetabular cup implant primary stability by impact analyses: a cadaveric study. PLoS ONE 11:e0166778
Mondal S, Ghosh R (2019) Effects of implant orientation and implant material on tibia bone strain, implant-bone micromotion, contact pressure, and wear depth due to total ankle replacement. Proc Inst Mech Eng H 233:318–331
Morgan EF, Unnikrisnan GU, Hussein AI (2018) Bone mechanical properties in healthy and diseased states. Annu Rev Biomed Eng 20:119–143
Natali AN, Pavan PG, Ruggero AL (2006) Analysis of bone-implant interaction phenomena by using a numerical approach. Clin Oral Implants Res 17:67–74
Nicholson JW (2020) Titanium alloys for dental implants: a review. Prosthesis 2:100–116. https://doi.org/10.3390/prosthesis2020011
Niinomi M, Nakai M (2011) Titanium-based biomaterials for preventing stress shielding between implant devices and bone. Int J Biomater 2011:836587
Okulov IV, Volegov AS, Attar H, Bönisch M, Ehtemam-Haghighi S, Calin M et al (2017) Composition optimization of low modulus and high-strength TiNb-based alloys for biomedical applications. J Mech Behav Biomed Mater 65:866–871
Okulov IV, Weissmüller J, Markmann J (2017) Dealloying-based interpenetrating-phase nanocomposites matching the elastic behavior of human bone. Sci Rep 7:20
Orsini G, Assenza B, Scarano A, Piattelli M, Piattelli A (2000) Surface analysis of machined versus sandblasted and acid-etched titanium implants. Int J Oral Maxillofac Implants 15:779–84
Piao C, Wu D, Luo M, Ma H (2014) Stress shielding effects of two prosthetic groups after total hip joint simulation replacement. J Orthop Surg Res 9:71
Raffa ML, Nguyen VH, Haiat G (2019) Micromechanical modeling of the contact stiffness of an osseointegrated bone-implant interface. Biomed Eng Online 18:114
Raffa ML, Nguyen VH, Hernigou P, Flouzat-Lachaniette CH, Haiat G (2021) Stress shielding at the bone-implant interface: influence of surface roughness and of the bone-implant contact ratio. J Orthop Res 39:1174–1183
Rojek J, Telega JJ (1999) Numerical simulation of bone-implant systems using a more realistic model of the contact interfaces with adhesion. J Theor Appl Mech 37:659–686
Rønold HJ, Ellingsen JE (2002) Effect of micro-roughness produced by TiO2 blasting–tensile testing of bone attachment by using coin-shaped implants. Biomaterials 23:4211–4219
Rupp F, Liang L, Geis-Gerstorfer J, Scheideler L, Hüttig F (2018) Surface characteristics of dental implants: a review. Dent Mater 34:40–57
Ryu HS, Namgung C, Lee JH, Lim YJ (2014) The influence of thread geometry on implant osseointegration under immediate loading: a literature review. J Adv Prosthodont 6:547–554
Sadegh AM, Luo GM, Cowin SC (1993) Bone ingrowth: an application of the boundary element method to bone remodeling at the implant interface. J Biomech 26:167–182
Shirazi-Adl A, Dammak M, Paiement G (1993) Experimental determination of friction characteristics at the trabecular bone/porous-coated metal interface in cementless implants. J Biomed Mater Res 27:167–175
Sumner DR (2015) Long-term implant fixation and stress-shielding in total hip replacement. J Biomech 48:797–800
Tang T, Ebacher V, Cripton P, Guy P, McKay H, Wang R (2015) Shear deformation and fracture of human cortical bone. Bone 71:25–35
Turner CH, Wang T, Burr DB (2001) Shear strength and fatigue properties of human cortical bone determined from pure shear tests. Calcif Tissue Int 69:373–378
Vayron R, Matsukawa M, Tsubota R, Mathieu V, Barthel E, Haiat G (2014) Evolution of bone biomechanical properties at the micrometer scale around titanium implant as a function of healing time. Phys Med Biol 59:1389–1406
Vayron R, Nguyen V-H, Lecuelle B, Albini Lomami H, Meningaud J-P, Bosc R et al (2018) Comparison of resonance frequency analysis and of quantitative ultrasound to assess dental implant osseointegration. Sensors (Basel, Switzerland) 18:1397
Voigt C, Klöhn C, Bader R, von Salis-Soglio G, Scholz R (2007) Finite element analysis of shear stresses at the implant-bone interface of an acetabular press-fit cup during impingement. Biomed Tech (Berl) 52:208–215
Weinans H, Sumner DR, Igloria R, Natarajan RN (2000) Sensitivity of periprosthetic stress-shielding to load and the bone density-modulus relationship in subject-specific finite element models. J Biomech 33:809–817
Yamako G, Janssen D, Hanada S, Anijs T, Ochiai K, Totoribe K et al (2017) Improving stress shielding following total hip arthroplasty by using a femoral stem made of β type Ti-33.6Nb-4Sn with a Young’s modulus gradation. J Biomech 63:135–143
Zhang QH, Cossey A, Tong J (2016) Stress shielding in periprosthetic bone following a total knee replacement: effects of implant material, design and alignment. Med Eng Phys 38(12):1481–1488. https://doi.org/10.1016/j.medengphy.2016.09.018
Zhou Y, Gong C, Hossaini-Zadeh M, Du J (2019) 3D contact and strain in alveolar bone under tooth/implant loading. In: TMS 2019 148th Annual Meeting & Exhibition Supplemental Proceedings, Cham, pp 793–798
Acknowledgements
This project has received funding from the Paris Ile-de-France Region (DIM “Respore” and F2M Federation), from the CNRS through the MITI interdisciplinary program, and from the European Research Council (ERC) under the European Union’s Horizon 2020 research and innovation program (grant agreement No 682001, project ERC Consolidator Grant 2015 BoneImplant).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hériveaux, Y., Le Cann, S., Fraulob, M. et al. Mechanical micromodeling of stress-shielding at the bone-implant interphase under shear loading. Med Biol Eng Comput 60, 3281–3293 (2022). https://doi.org/10.1007/s11517-022-02657-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11517-022-02657-2