Abstract
Purpose
The aim of this study was to investigate the relationship between coping strategies and subjective well-being (SWB) among people living with HIV (PLWH) using the latent profile analysis (LPA) with control for socio-medical covariates.
Methods
The sample comprised five hundred and thirty people (N = 530) with a confirmed diagnosis of HIV+. The study was cross-sectional with SWB operationalized by satisfaction with life (Satisfaction with Life Scale) and positive and negative affect (PANAS-X). Coping with stress was measured by the Brief COPE Inventory, enriched by several items that assessed rumination and enhancement of positive emotional states. Additionally, the relevant socio-medical variables were collected.
Results
The one-step model of LPA revealed the following: (1) a solution with five different coping profiles suited the data best; (2) socio-medical covariates, except for education, were not related to the profiles’ membership. Further analysis with SWB as a distal outcome showed that higher intensity coping profiles have significantly worse SWB when compared with lower intensity coping profiles. However, the lowest SWB was noted for mixed intensity coping profile (high adaptive/low maladaptive).
Conclusions
The person-centered approach adopted in this study informs about the heterogeneity of disease-related coping among PLWH and its possible reactive character, as the highest SWB was observed among participants with the lowest intensity of coping.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
The literature on coping among people living with HIV (PLWH) is large but highly heterogeneous with regard to coping measurements, coping outcomes, and final remarks [1]. The vast majority of studies on this topic have concentrated on the role of active and avoidant coping. While active coping is related to greater level of CD4-cell counts [2], fewer HIV-related symptoms [3], better quality of life [4], lower frequency of alcohol and drug use [5] and better adherence to treatment [6], avoidant coping have been associated with deterioration of psychosocial and health status of PLWH, including worse physical functioning [7], poor quality of life [8], frequent use of alcohol and drugs [5], and non-adherence to treatment [6]. More specifically, Moskowitz et al. [9] found that meaning-focused coping was consistently linked with better affective, behavior, and physical health outcomes among PLWH. McIntosh and Rosselli [10] observed that spiritual coping and positive reframing promoted psychological adaptation among HIV-infected women to a greater degree than social support seeking. Furthermore, Kraaij et al. [11] noted that cognitive coping strategies (e.g., positive reappraisal) and a proper goal adjustment (e.g., disengagement from unrealistic goals, and reengaging in alternative meaningful aims) have the strongest impact on well-being among HIV-infected men.
However, even if there is a generally accepted consensus that coping matters with regard to how people deal with adverse life events, little agreement has been reached on how to conceptualize, measure, and classify different ways of coping [12,13,14]. One of the central problems in coping literature is that many authors neglect that the term “coping” is not a unique, observable behavior, stable trait, or easily reported specific belief. On the contrary, it is a dynamic, multidimensional construct that encompasses various actions, behaviors, emotions, and cognitions often used by the same person simultaneously [15, 16]. Finally, the vast majority of authors define ways of coping according to a variable-oriented approach, in terms of dimensions, whereas the fact that the same person may have different positions on each dimension is disregarded [17, 18].
In that light, the central question is not whether some ways of coping are less or more effective, but rather how a specific person copes with a particular stressor and what his or her effectiveness is in doing so. Therefore, a person-centered approach is likely to bring a new perspective to examine coping complexities [19]. It is particularly important since some studies have already demonstrated that a higher intensity of coping may be related to worse, instead of better adaptation (e.g., [20, 21]) and the idea of the possibly defensive nature of intense coping was introduced by Krohne [22] more than two decades ago. Nevertheless, it is worth mentioning that this conceptualization aligns with the definition of coping as individuals’ efforts to reduce imbalance between demands and resources, provided by Folkman and Lazarus [23]. When those efforts are highly diversified and all of them are performed with a high intensity, regardless of specific situational demands, they may actually be a sign of high distress or, in other terms, an indicator of a strong conflict between demands and available resources. When such intensity of coping is performed without goodness of fit to the situational demands for a longer time, it may lead to significant psychological consequences. First, it shows that the aforementioned imbalance has not been resolved despite the efforts made, so the person is still under stress. Second, keeping up such efforts is not possible without costs, which may additionally influence subjective well-being (SWB).
Numerous studies have been conducted on the concept of well-being not only in psychology, but also in other social sciences (e.g., [24,25,26]). Nevertheless, the question of how well-being should be defined and operationalized still remains largely unresolved [27, 28]. Despite various approaches to well-being, a majority of the authors agree that well-being is a multidimensional construct and there is a necessity to be clear about what is being measured [29, 30]. In this study, we concentrated on SWB defined broadly by the level of satisfaction with life and a combination of positive and negative affect [31,32,33] among people living with HIV (PLWH). The issue of SWB seems to be of special interest among patients dealing with chronic disease, with significant psychological and social burden, such as PLHW. The substantial progress in antiretroviral therapy has changed social attitudes toward HIV/AIDS from a fatal and terminal illness to a chronic medical condition and has given great hope to PLWH for a longer life [34, 35]. However, PLWH still experience major psychological distress stemming from being diagnosed with a potentially life-threatening virus [36, 37], unpredictability of HIV symptoms fluctuation [38, 39], and social isolation and discrimination [40, 41]. Not only can HIV-related distress deteriorate SWB, but poor SWB among this patient group impacts the course of HIV infection by diminishing CD4 cell counts, which influence the pace of HIV progression [42]. Therefore, research on SWB among PLWH has important clinical implications [43, 44]. Nevertheless, the majority of studies on SWB among PLWH concentrated solely on the presence or absence of these negative HIV-related mental health problems (e.g., [45, 46]). Therefore, in this study, we focused on the aforementioned broad definition of SWB among PLWH.
Current study
Despite the same medical diagnosis and controlling for other medical variables, there is a significant interindividual variability in coping with HIV infection [1]. Further, although the results from the variable-centered studies seem reasonably coherent, they do not take into account these individual differences, that is, each person may perform a different combination of so-called adaptive and maladaptive strategies. To address this gap, we implemented a person-centered approach using a latent profile analysis (LPA). Thus, the aim of the study was twofold: First, to investigate heterogeneity of coping with the disease among PLWH, including possible socio-medical covariates; and second, to examine whether different coping profiles are related to SWB in this patient group [47].
On the basis of the aforementioned studies on coping and SWB among PLWH, we generated three specific hypotheses. First, we expected that the sample was heterogeneous in terms of coping, i.e., different coping profiles can be observed among the participants. Second, allocation to a specific coping profile is related to socio-medical status since this status may serve as a proxy of current level of resources available to the person [48]. Finally, we assumed that higher intensity coping profiles are related to worse SWB when compared with lower intensity coping profiles. Additionally, participants belonging to the mixed intensity coping profile (higher intensity on some coping strategies and lower on others) have higher SWB. More specifically, for mixed profiles, a combination of higher intensity of strategies related to more adaptive outcomes (e.g., active and problem-focused coping, including positive reframing and positive emotional enhancement) and lower intensity of so-called maladaptive strategies (e.g., avoidant coping and palliative forms of emotion-focused coping) should be the best in terms of well-being [49].
Method
Participants and procedure
Five hundred and thirty (530) adults with a medical diagnosis of HIV infection were recruited from patients of the out-patient clinic of the state hospital for infectious diseases. The participants completed a paper-and-pencil version of the measures and participated in the study voluntary (there was no remuneration). The eligibility criteria were that participants had to be 18 years of age or older, had to have a medically confirmed diagnosis of HIV+, and had to be a recipient of antiretroviral treatment at the out-patient clinic where the study was conducted. The exclusion criteria included HIV-related cognitive impairment diagnosed by medical doctors. In particular, out of the 750 patients eligible for the study, 530 were approached and agreed to the filed measures (71%), 152 declined (20%), and 68 (9%) had missing data to an extent that precluded them from the analysis [50].
Specifically, there were 444 men (84%) and 86 women (16%) between 18 and 76 years of age (M = 39.81; SD = 10.54) of whom 57% of were married. Only 16% of the participants had elementary education, 31% reported secondary and 53% higher education. Majority of the participants, declared full employment (72%), 12% were unemployed, 12% were receiving a pension, and 4% were retired. When it came to the clinical variables, the HIV infection duration ranged from 1 to 32 years (M = 7.71; SD = 6.86). The antiretroviral treatment duration ranged from 1 to 32 years (M = 5.97; SD = 5.53), and the CD4 cell count ranged from 100 to 2,000 (M = 589.46; SD = 222.42). Finally, out of the whole sample, 15% patients were diagnosed with AIDS.
Measures
Subjective well-being indicators
SWB was measured on the Satisfaction with Life Scale (SWLS; [31] along with the Positive and Negative Affect (PANAS-X; Watson and Clark [51]. The SWLS comprises five items, each with a seven-point scale, ranging from 1 (strongly disagree) to 7 (strongly agree). A higher total score means a higher level of satisfaction with life. The Cronbach’s alpha in the current study was satisfactory (.88). The PANAS-X comprises 10 adjectives for positive affect (e.g., proud, excited, etc.) and 10 for negative affect (e.g., frightened, hostile, etc.). The participants were asked to rate their general affective states on a five-point response scale from 1 (not at all) to 5 (extremely). The Cronbach’s alpha coefficients obtained in this study were .85 for the positive affect subscale and .86. for the negative affect subscale.
Coping strategies
To assess strategies for coping with stress, the Brief COPE Inventory was used [52]. This tool consists of 28 items and provides 14 subscales with a different reliability, two items each with a Likert-like response scale ranging from 0 (I haven’t been doing this at all) to 3 (I’ve been doing this a lot). Coping intensity is understood as participants’ self-report on the magnitude with which their use a given strategy to deal with health issues caused by being infected with HIV. The subscales were derived empirically, and they were not theoretically reassessed afterwards to propose a more comprehensive systematization of coping strategies (see [14]). In particular, as this tool does not include items directly referring to rumination, which is one of the most strongly proved maladaptive strategies (see [53]), and items describing coping efforts focused on enhancement of positive emotional states during stress, the relevant two items were added from the Ruminative Response Styles [54]: I think What am I doing to deserve this?; I think Why do I have problems other people don’t have?) and from the Coping with Health Injuries and Problems Scale after modification [55]: I have nice things around; I look for simple pleasures (e.g., having a cup of tea, listening to music, walking, reading a good book)). Therefore, there were 16 coping indicators in the study: self-distraction, active coping, denial, substance use, use of emotional support, use of instrumental support, behavioral disengagement, venting, positive reframing, planning, humor, acceptance, religion, self-blame, rumination, and positive emotion enhancement. The Cronbach’s alpha ranged from .78 to .86. Due to reasons described in the introduction, we did not classify the subscales into the higher order coping indices, as this kind of aggregation may influence segmentation results.
Data analysis
LPA is a statistical method that enables investigation of unobserved heterogeneity within a studied sample, that is, it identifies groups of participants who represent the greatest similarity on the same set of observed continuous variables within a given group and the greatest dissimilarity between other participants’ groups [56]. In our study, this method allows classifying participants into a number of exclusive and exhaustive subgroups, characterized by different coping profiles. A model with an optimal number of such categories (i.e., profiles) is selected on the basis on several indicators. For Akaike’s information criterion (AIC), Bayesian information criterion (BIC), and the sample-size adjusted BIC (SABIC), lower values indicate a model with better fit [57]. Another evaluation of goodness of fit is provided by the results of the bootstrap likelihood ratio test (BLRT [58], which compares neighboring models. An entropy-based criterion indicates a quality of a class separation from 0 to 1, where 1 evidences a perfect classification [19]. Finally, a size of the smallest class is a practical criterion, since classes smaller than 5% of the sample is considered spurious and unreplicable [59].
In general, we used LPA with distal outcomes [60]. First, to select a model with an optimal number of coping profiles, we adopted the one-step approach with socio-medical covariates (gender, age, marital status, education, employment, HIV/AIDS status, HIV infection duration in years, antiretroviral treatment duration in years, CD4 count) included in the process of segmentation, thus the obtained coping profiles were adjusted in this regard [61]. Then we regressed a distal outcome, that is, SWB, on latent coping profiles using the bias-adjusted three-step analysis described by Vermunt and Magidson [62, 63]. The calculations were performed using the Latent GOLD 5.1 (containing a submodule called Step3) and IBM SPSS Statistics version 24.
Results
Descriptive statistics
Mean values, standard deviations, and Pearson‘s correlations of the main study variables are presented in Table 1.
All the variables can be regarded as normally distributed. Positive affect and negative affect were uncorrelated (r = −.03) and only up to medium were they related to satisfaction with life. Thus, it indicates that they these domains of SWB are indeed separate to a significant degree. Among coping strategies, the highest correlation was noted for denial and behavioral disengagement (r = .70).
Coping profiles and their socio-medical correlates
Table 2 summarizes the indices of the model selection process for one to six profile solutions. BIC, AIC, and SABIC (see, "Data analysis") indicate on six-profile model. Also, BLRT informs that adding a profile to each consecutive model significantly improves goodness of fit which may also point at the most numerous profile solutions. Entropy values were similar for all the models so each of them provides a good separation in the sample.
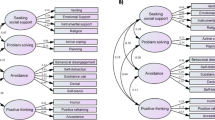
However, the size of the smallest group in the six-profile solution was as low as 3% of the sample. Thus, the second best fitted model, a five-profile solution, was chosen for further analysis. Figure 1 illustrates this model.
As it can be seen, four out of five coping profiles are mostly parallel, whereas the remaining one crosses over from high values to lower ones (profile 3). The most numerous group consists of 159 participants (30%, profile 1) and can be described as high intensity coping profile. The second one, represented by 135 participants (25.5%, profile 2), has a generally lower profile, especially with regards to denial, substance use and turn to religion strategies. As already mentioned, mixed profile was observed for 130 participants (24.5%, profile 3). They have high values on coping strategies frequently named as adaptive coping and lower values on strategies named maladaptive coping. The highest intensity coping profile is represented by 59 participants (11%, profile 4). Finally, the smallest group with the lowest intensity coping profile included 47 participants (9%, profile 5). It is worth noticing, however, that the highest and the lowest profiles have a similar number of members. Also, profiles for intense copers (profile 1 and profile 4) are more flatted whereas profiles for mild copers (profile 2 and 5) have slightly higher values in positive reframing, acceptance and enhancement of positive emotions. The averaged posterior probability ranged from .89 for the mixed profile to.97 for the most intensive coping profile.
Finally, it turned out that profiles differed only in terms of education (Wald = 11.31, p = .02). The pairwise comparisons revealed that the highest proportion of patients with university degree was in profile 2 (2.28) and 5 (1.35), while in other profiles this distribution was statistically equal for all the levels of education. Therefore, the coping profiles’ membership appeared to be relatively independent of socio-medical variables, which was also reflected in standard R squared for a covariate-based classification equaled only .03.
Relations of coping profiles with well-being
Significant differences between coping profiles with regard to SWB were noted. Table 3 presents test values and means for each profile for illustrative purposes.
Additionally, to elaborate on affective well-being, a positive affect to negative affect ratio was added. As can be seen, the highest satisfaction with life and positive affect as well as the lowest negative affect was noted for profile 5 and then for profile 2, thus the lowest profiles have the highest SWB. Interestingly, the lowest SWB was observed among participants with a mixed intensity coping profile.
Discussion
The results of our study were consistent with the first hypothesis, that is, we observed the heterogeneity of the sample of PLWH with regard to coping with the disease, as five different coping profiles were observed. Thus, our findings are in line with ideas expressed a long time ago, as well as with contemporary critical observations on the nature of coping that it is a multidimensional construct that operates on the number of different levels [64, 22, 65]. As far as PLWH is concerned, our results may be interesting in and of itself, as till now the vast majority of studies among PLWH were conducted in the variable-oriented model, and were focused on searching for single sociodemographic or medical variables that are independently associated with various coping strategies, neglecting the problem of heterogeneity of coping in this group of patients [45, 43, 1]. The domination of variable-oriented model may also be the reason why ambiguous results on well-being among PLWH exist in the literature. According to Keiser et al. [66], many authors disregard how particular socio-medical and psychosocial variables cluster across different PLWH subgroups distinguished on the basis of various SWB profiles, which can be influenced by a large number of factors simultaneously. Our study addressed these two gaps in the literature by examining both coping profiles and subjective well-being among people living with HIV using latent profile analysis.
Secondly, socio-medical variables, with the exception of education, were not related to the coping profiles among our participants and, as such, were also irrelevant for observed SWB differences between these profiles, which contradicted our second hypothesis. This finding is contrary to several previous studies, which showed that coping among HIV+ individuals is shaped greatly by clinical variables, such as a CD4 cell count [67, 68], HIV infection duration [37], being diagnosed with AIDS in particular [69], being on ART treatment [70, 71] or sociodemographic data [46]. In our sample, however, coping profiles and consequently SWB differences as well were related only to having a university degree. This finding may be discussed in the context of existing HIV-related stigma, and threat of social rejection, including in particular losing social status, which is still a very prevalent experience among PLWH [40, 72]. Perhaps higher education acts here as a personal resource that offers an opportunity for a greater social participation and reduces stress level both directly through a lower number of stressors and indirectly through more effective but less intense coping [73]. Therefore, education may be a better proxy of health-related stress and well-being than clinical variables since the great advancements in HIV/AIDS treatment have improved substantially the life expectancy of PLWH [35]. As a result, an increasing number of PLWH are more concerned with their social status not only with health outcomes. It is also in accordance with other studies, which indicated that subjective well-being among chronically ill patients depends more on psychosocial factors rather than socio-medical variables [74].
Finally, in line with our third hypothesis, higher intensity coping profiles were related to worse well-being when compared with lower intensity coping profiles, but contrary to our expectations, members of the mixed intensity profile (high adaptive/low maladaptive) have the lowest SWB. This result is particularly intriguing, as there is a common assumption in coping literature that more intense adaptive coping provides better effects for individual’s well-being across different stressful situations (e.g., [75,76,77]. Again, perhaps there is a need to come back to basics, as Krohne [22] previously suggested that low- intensity coping and diversity may just mean a low level of distress. There is the theoretical argument that coping is a psychological necessity only when a person is under stress according to his or her cognitive appraisal. However, at least for some, their extensive coping efforts do not bring any relief in this regard. In uncontrollable situations, such as terminal disease, coping may even be purely reactive, that is, the process of coping may be initiated only due to experiencing strong negative emotions, no matter if this specific way of coping is meaningful in this situation or not [78]. One study regarding PLWH provided data in accordance with our findings. Fleishman et al. [79] in a study on coping in response to HIV/AIDS proved that PLWH classified as passive copers had fewer HIV-related symptoms, a better level of physical functioning, and high affective well-being. It is likely that in an uncontrollable situation, and many aspects of being HIV+ can be described as such, intensive coping may elevate more HIV-related distress, but again, there is no consensus on that in the literature [1].
However, our study is not free of limitations. First of all, the cross-sectional design prevents us from making causal interpretations and future studies should be conducted in a longitudinal design. Even if well-being was an explanatory variable here, the possibility that its low values may be a source of stress itself, thus a cause and not an outcome of coping, cannot be excluded. Secondly, we did not control for the level of stress experienced by the participants. In future research, the intensity of stress should be treated as a covariate, e.g., participants that experienced more level of stress may have higher coping intensity. Thirdly, we assessed, a broad but still selective set of coping strategies, so it would be advisable in the future to check if the obtained effects are present for other coping measurements. Finally, in our sample significant underrepresentation of women is seen, but the gender ratio was typical for PLWH population [80] and this is in line with other studies pointing at a lack of gender differences in coping among PLWH [81, 82].
From a clinical point of view, our findings suggest that when providing psychological help special focused should be put on patients with very intense coping. Furthermore, a modification of coping into so-called favorable profile (high intensity of adaptive strategies accompanied by low intensity of maladaptive strategies) may not necessary is a proper direction. Thus, further research is needed as knowledge about psychological functioning of PLWH is still limited.
Conclusion
The person-centered approach adopted in this study informs about the heterogeneity of disease-related coping among PLWH and its possible reactive character, as the highest SWB, was observed among participants with the lowest intensity of coping. The results of this study illustrate how a person-centered approach may influence clinically relevant knowledge regarding the complexities of dealing with chronic disease as well as elucidate coping research in general. We have to remember that beyond the coping strategies, there is always the person who copes.
References
Moskowitz, J., Hult, J., Bussolari, C., & Acree, M. (2009). What works in coping with HIV? A meta-analysis with implications for coping with serious illness. Psychological Bulletin, 135, 121–141. doi:10.1037/a0014210.
Ironson, G., & Hayward, M. (2008). Do Positive psychosocial factors predict disease progression in HIV-1? A Review of the evidence. Psychosomatic Medicine, 70, 546–554. doi:10.1097/PSY.0b013e318177216c.
Chida, Y., & Vedhara, K. (2009). Adverse psychosocial factors predict poorer prognosis in HIV disease: a meta-analytic review of prospective investigations. Brain, Behavior, and Immunity, 23, 434–445. doi:10.1016/j.bbi.2009.01.013.
Vyavaharkar, M., Moneyham, L., Murdaugh, C., & Tavakoli, A. (2012). Factors associated with quality of life among rural women with HIV disease. AIDS and Behavior, 16, 295–303. doi:10.1007/s10461-011-9917-y.
Pence, B., Thielman, N., Whetten, K., Ostermann, J., Kumar, V., & Mugavero, M. (2008). Coping strategies and patterns of alcohol and drug use among HIV-infected patients in the Unites States southeast. AIDS Patient Care STDs, 22, 777–869. doi:10.1089/apc.2008.0022.
Vervoort, S., Grypdonck, M., de Grauwe, A., Hoepelman, A., & Borleffs, J. (2009). Adherence to HAART: Processes explaining adherence behaviour in acceptors and non-acceptors. AIDS Care, 21, 431–438. doi:10.1080/09540120802290381.
Griswold, G., Evans, S., Spielman, L., & Fishman, B. (2005). Coping strategies of HIV patients with peripheral neuropathy. AIDS Care, 17, 711–720. doi:10.1080/09540120412331336715.
Weaver, K., Antoni, M., Lechner, S., Dura, R., Penendo, F., & Fernandez, M. (2004). Perceived stress mediates the effects of coping on the quality of life in HIV-positive women on highly active antiretroviral therapy. AIDS and Behavior, 8, 175–183. doi:10.1023/B:AIBE.0000030248.52063.11.
Moskowitz, J. (2003). Positive affect predicts lower risk of AIDS mortality. Psychosomatic Medicine, 65, 620–626. doi:10.1097/01.PSY.0000073873.74829.23.
McIntosh, R., & Rosselli, M. (2012). Stress and coping in women living with HIV: A meta-analytic review. AIDS and Behavior, 16, 2144–2159. doi:10.1007/s10461-012-0166-5.
Kraaij, V., van der Veek, S., Garnefski, N., Schroevers, M., Witlox, R., & Maes, S. (2008). Coping, goal adjustment, and psychological well-being in HIV-infected men who have sex with men. AIDS Patient Care STDS, 22, 395–402. doi:10.1089/apc.2007.0145.
Cheng, C., Lau, H., & Chan, M. (2014). Coping flexibility and psychological adjustment to stressful life changes: A meta-analytic review. Psychological Bulletin, 140, 1582–1607. doi:10.1037/a0037913.
Parker, J., & Endler, N. (1992). Coping with coping assessment: A critical review. European Journal of Personality, 6, 321–344. doi:10.1002/per.2410060502.
Skinner, E., Edge, K., Altman, J., & Sherwood, H. (2003). Searching for the structure of coping: A review and critique of category systems for classifying ways of coping. Psychological Bulletin, 129, 216–269. doi:10.1037/0033-2909.129.2.216.
Kato, T. (2013). Frequently used coping scales: A meta-analysis. Stress & Health, 31, 315–323. doi:10.1002/smi.2557.
Sandler, I. N., Wolchik, S. A., MacKinnon, D., Ayers, T. S., & Roosa, M. W. (1997). Developing linkages between theory and intervention in stress and coping processes. In S. A. Wolchik & I. N. Sandler (Eds.), Handbook of children’s coping: Linking theory, research, and intervention (pp. 3–40). New York: Plenum Press.
Anusic, I., Yap, S. C. Y., & Lucas, R. E. (2014). Testing set-point theory in a Swiss national sample: Reaction and adaptation to major life events. Social Indicators Research, 119, 1265–1288. doi:10.1007/s11205-013-0541-2.
Brennan, P. L., Holland, J. M., Schutte, K. K., & Moos, R. H. (2012). Coping trajectories in later life: A 20-year predictive study. Aging & Mental Health, 16, 305–316. doi:10.1080/13607863.2011.628975.
Muthén, B., & Muthén, L. K. (2000). Integrating person-centered and variable-centered analyses: Growth mixture modeling with latent trajectory classes. Alcoholism, Clinical and Experimental Research, 24, 882–891.
Folkman, S. (1997). Positive psychological states and coping with severe stress. Social Science and Medicine, 45, 1207–1221. doi:10.1016/S0277-9536(97)00040-3.
Stanton, A., Revenson, T., & Tennen, H. (2007). Health psychology: Psychological adjustment to chronic disease. Annual Review of Psychology, 58, 565–592. doi:10.1146/annurev.psych.58.110405.085615.
Krohne, H. W. (1993). Vigilance and cognitive avoidance as concepts in coping research. In H. W. Krohne (Ed.), Attention and avoidance: Strategies in coping with aversiveness (pp. 19–50). Seattle, WA: Hogrefe & Huber.
Folkman, S., & Lazarus, R. S. (1980). An analysis of coping in a middle-aged community sample. Journal of Health and Social Behavior, 21, 219–239.
Ryff, C. D. (1989). Happiness is everything, or is it? Explorations on the meaning of psychological well-being. Journal of Personality and Social Psychology, 57, 1069–1081. doi:10.15557/a00144210.
Seligman, M. E. P. (2011). Flourish—a new understanding of happiness and well-being—and how to achieve them. London: Nicholas Brealey Publishing.
Stiglitz, J., Sen, A., & Fitoussi, J. P. (2009). Report by the commission on the measurement of economic performance and social progress.
Dodge, R., Daly, A., Huyton, J., & Sanders, L. (2012). The challenge of defining wellbeing. International Journal of Wellbeing, 2, 222–235. doi:10.1166/20439-3338-72-40.
Steptoe, A., Deaton, A., & Stone, A. (2015). Subjective wellbeing, health, and ageing. Lancet, 14, 640–648.
Diener, E. (2009). Subjective well-being. In E. Diener (Ed.), The science of well-being (pp. 11–58). New York: Springer.
Michaelson, J., Abdallah, S., Steuer, N., Thompson, S., & Marks, N. (2009). National accounts of well-being: Bringing real wealth onto the balance sheet. London: New Economics Foundation.
Diener, E., Emmons, R. A., Larsen, R., & Griffin, S. (1985). The Satisfaction With Life Scale. Journal of Personality Assesment, 49, 71–75. doi:10.1207/s15327752jpa4901_13.
Fredrickson, B. L. (2013). Updated thinking on positivity ratios. American Psychologist, 68, 814–822. doi:10.1037/a0033584.
Fredrickson, B. L. (2013). Updated thinking on positivity ratios. American Psychologist, 68, 814–822. doi:10.1037/a0033584.
Deeks, S., Lewin, S., & Havlir, D. (2013). The end of AIDS: HIV infection as a chronic disease. Lancet. doi:10.1016/S0140-6736(13)61809-7.
Samji, H., Cescon, A., Hogg, R., Modur, S., & Althoff, K. (2013). Closing the gap: Increases in life expectancy among treated HIV-positive individuals in the United States and Canada. PLoS ONE, 18, 144–156. doi:10.1371/journal.pone.0081355.
Rzeszutek, M., Oniszczenko, W., & Firląg-Burkacka, E. (2012). Temperament traits, coping style and trauma symptoms in HIV+ men and women. AIDS Care, 24, 1150–1154. doi:10.1080/09540121.2012.687819.
Rzeszutek, M., Oniszczenko, W., Żebrowska, M., & Firląg-Burkacka, E. (2015). HIV infection duration, social support and the level of trauma symptoms in a sample of HIV-positive Polish individuals. AIDS Care, 27, 363–369. doi:10.1080/09540121.2014.963018.
Jayarajan, N., & Prabha, S. (2010). HIV and mental health: An overview of research from India. Indian Journal of Psychiatry, 16, 23–39. doi:10.4103/0019-5545.69245.
Theuninck, A., Lake, N., & Gibson, S. (2010). HIV-related posttraumatic stress disorder: Investigating the traumatic events. AIDS Patient Care and STDs, 24, 458–491. doi:10.1089/apc.2009.0231.
Bogart, L., Wagner, G., Galvan, F., Landrine, H., & Klein, D. (2011). Perceived discrimination and mental health symptoms among black men with HIV. Cultural diversity and ethnic minority. Psychology, 17, 295–302. doi:10.1037/a0024056.
Emlet, C. (2006). A comparison of HIV stigma and disclosure patterns between older and younger adults living with HIV/AIDS. AIDS Patient Care and STDs, 20, 350–358. doi:10.1089/apc.2006.20.350.
Pacella, M., Armelie, A., Boarts, J., Wagner, G., Jones, T., Feny, N., et al. (2012). The impact of prolonged exposure on PTSD symptoms and associated psychopathology in people living with HIV: A randomized test of concept. AIDS and Behavior, 16, 1327–1340. doi:10.1007/s10461-011-0076-y.
Mekuria, L., Sprangers, M., Prins, J., Alemayehu, W., & Yalew, P. (2015). Health-related quality of life of HIV-infected adults receiving combination antiretroviral therapy in Addis Ababa. AIDS Care, 27, 934–945. doi:10.1080/09540121.2015.1020748.
Tsevat, J., Leonard, A., Szaflarski, M., Sherman, S., & Cotton, S. (2009). Change in quality of life after being diagnosed with HIV: A multicenter longitudinal study. AIDS Patient Care STDS, 23, 931–937. doi:10.1089/apc.2009.0026.
Degroote, S., Vogelaers, D., & Vandijck, D. (2014). What determines health-related quality of life among people living with HIV: an updated review of the literature. Archives of Public Health, 72, 40. doi:10.1186/2049-3258-72-40.
Logie, C., & Gadalla, T. (2009). Meta-analysis of health and demographic correlates of stigma towards people living with HIV. AIDS Care, 21, 742–753. doi:10.1080/09540120802511877.
Gruszczyńska, E., & Knoll, N. (2015). Meaning-focused coping, pain, and affect: A diary study of hospitalized women with rheumatoid arthritis. Quality Of Life Research: An International Journal Of Quality Of Life Aspects Of Treatment, Care & Rehabilitation, 24, 2873–2883. doi:10.1007/s11136-015-1031-6.
Hobfoll, S. E. (2002). Social and psychological resources and adaptation. Review of General Psychology, 6(4), 307–324. doi:10.1037/1089-2680.6.4.307.
Schuler, M. S., Leoutsakos, J.-M. S., & Stuart, E. A. (2014). Addressing confounding when estimating the effects of latent classes on a distal outcome. Health Services and Outcomes Research Methodology, 14(4), 232–254. doi:10.1007/s10742-014-0122-0.
Vermunt, J. K. (2010). Latent class modelling with covariates: Two improved three-step approaches. Political Analysis, 18, 450–469.
Watson, D., Clark, L., & Tellegen, A. (1988). Development and validation of brief measures of positive and negative affect. The PANAS Scales. Journal of Personality and Social Psychology, 54, 1063–1070.
Carver, C., & Scheier, M. (1994). Situational coping and coping dispositions in a stressful transaction. Journal of Personality and Social Psychology, 66, 184–195.
Nolen-Hoeksema, S., Wisco, B. E., & Lyubomirsky, S. (2008). Rethinking rumination. Perspectives on Psychological Science, 3, 400–424. doi:10.1111/j.1745-6924.2008.00088.x.
Treynor, W., Gonzalez, R., & Nolen-Hoeksema, S. (2003). Rumination reconsidered: A psychometric analysis. Cognitive Therapy and Research, 27, 247–259. doi:10.1023/A:1023910315561.
Endler, N., Parker, J., & Summerfeldt, L. (1998). Coping with health problems: Developing a reliable and valid multidimensional measure. Psychological Assessment, 10, 195–205. doi:10.1037/1040-3590.10.3.195.
Lubke, G. H., & Neale, M. C. (2006). Distinguishing between latent classes and continuous factors: Resolution by maximum likelihood. Multivariate Behavioral Research, 4, 499–532. doi:10.1207/s15327906mbr4104_4.
Tofghi, D., & Enders, C. K. (2007). Identifying the correct number of classes in mixture models. In G. R. Hancock & K. M. Samulelsen (Eds.), Advances in latent variable mixture models (pp. 317–341). Greenwich, CT: Information Age.
McLachlan, G. J., & Peel, D. (2000). Finite mixture models. New York: Wiley.
Hipp, J. R., & Bauer, D. J. (2006). Local solutions in the estimation of growth mixture models. Psychological Methods, 11, 36–53. doi:10.1037/1082-989X.11.1.36.
Asparouhov, T., & Muthén, B. (2014). Variable-specific entropy contribution. Retrieved from https://www.statmodel.com/download/UnivariateEntropy.pdf.
Lanza, S. T., Tan, X., & Bray, B. C. (2013). Latent class analysis with distal outcomes: A flexible model-based approach. Structural Equation Modeling, 20(1), 1–26. doi:10.1080/10705511.2013.742377.
Vermunt, J. K., & Magidson, J. (2004). Latent class analysis. In M. S. Lewis-Beck, A. Bryman, & T. F. Liao (Eds.), The sage encyclopedia of social sciences research methods (pp. 549–553). Thousand Oaks, CA: Sage Publications.
Vermunt, J. K., & Magidson, J. (2016). Technical guide for latent GOLD 5.1: Basic, advanced, and syntax. Belmont, MA: Statistical Innovations Inc.
Gruszczyńska, E. (2013). State affect and emotion-focused coping: Examining correlated change and causality. Anxiety, Stress & Coping: An International Journal, 26, 103–119. doi:10.1080/10615806.2011.633601.
Pearlin, L., & Schooler, C. (1978). The structure of coping. Journal of Health and Social Behavior, 19, 2–21.
Keiser, O., Spycher, B., Rauch, A., Calmy, A., Cavassini, M., Glass, T., et al. (2012). Outcomes of antiretroviral therapy in the Swiss HIV cohort study: Latent class analysis. AIDS and Behavior, 16, 244–255. doi:10.1007/s10461-011-9971-5.
Armon, C., & Lichtenstein, K. (2012). The associations among coping, nadir CD4 + T-cell count, and non-HIV-related variables with health-related quality of life among an ambulatory HIV-positive patient population. Quality of Life Research, 21, 993–1003. doi:10.1007/s11136-011-0017.
Ballester-Arnal, R., Martı´nez, S., Fumaz, C., Gonza´lez-Garcı´a, G., Remor, E., & Fuste, M. (2016). A Spanish study on psychological predictors of quality of life in people with HIV. AIDS and Behavior, 20, 281–291. doi:10.1007/s10461-015-1208-6.
Preau, M., Marcellin, F., Carrieri, M., Lert, F., Obadia, Y., & Spire, B. (2007). Health-related quality of life in French people living with HIV in 2003: Results from the national ANRS-EN12-VESPA Study. AIDS, 21, 19–27.
Hansen, N., Vaughan, A., Cavanaugh, C., & Connell, C. (2009). Health-related quality of life in bereaved HIV-positive adults: Relationships between HIV symptoms, grief, social support, and axis II indication. Health Psychology, 28, 249–257. doi:10.1037/a0013168.
Liu, C., Ostrow, D., Detels, R., Hu, Z., Johnson, L., Kingsley, L., et al. (2006). Impacts of HIV infection and HAART use on quality of life. Quality of Life Research, 15, 941–949. doi:10.1007/s11136-005-5913-x.
Breet, E., Kagee, A., & Seedat, S. (2014). HIV-related stigma and symptoms of post-traumatic stress disorder and depression in HIV-infected individuals: Does social support play a mediating or moderating role? AIDS Care, 26, 947–951. doi:10.1080/09540121.2014.901486.
O’Leary, A., Jemmott, J. B., Stevens, R., et al. (2014). Optimism and education buffer the effects of syndemic conditions on HIV status among African American Men who have sex with men. AIDS and Behavior, 18, 2080–2088. doi:10.1007/s10461-014-0708-0.
Simmons, Z., Bremer, B., Robbins, R., Walsh, S. M., & Fischer, B. (2000). Quality of life in ALS depends on factors other than strength and physical function. Neurology, 55, 388–392. doi:10.1212/WNL.55.3.388.
Duangdao, K., & Roesch, S. (2008). Coping with diabetes in adulthood: A meta-analysis. Journal of Behavioral Medicine, 31, 291–300. doi:10.1007/s10865-008-9155-6.
Prati, G., & Pietrantoni, L. (2009). Optimism, social support, and coping strategies as factors contributing to posttraumatic growth: A meta-analysis. Journal of Loss and Trauma, 14, 364–368. doi:10.1080/15325020902724271.
Roesch, S., & Weiner, B. (2001). A meta-analytic review of coping with illness: Do causal attributions matter? Journal of Psychosomatic Research, 50, 205–219. doi:10.1007/76-007667.
Söllner, W., Maislinger, S., DeVries, D., Steixner, E., Rumpold, G., & Lukas, P. (2000). Use of complementary and alternative medicine by cancer patients is not associated with perceived distress or poor compliance with standard treatment but with active coping behavior. Cancer, 89, 873–880.
Fleishman, J. A., Sherbourne, C. D., Cleary, P. D., Wu, A. W., Crystal, S., & Hays, R. D. (2003). Patterns of coping among persons with HIV infection: Configurations, correlates, and change. American Journal of Community Psychology, 32, 187–204.
Bor, J., Rosen, S., Chimbindi, N., Haber, N., Herbst, K., Mutevedzi, T., et al. (2015). Mass HIV treatment and sex disparities in life expectancy: Demographic surveillance in rural south Africa. PLOS Medicine. doi:10.1371/journal.pmed.1001905.
Ashton, E., Vosvick, M., Chesney, M., Gore-Felton, C., Koopman, C., O’Shea, K., et al. (2005). Social support and maladaptive coping as predictors of the change in physical health symptoms among persons living with HIV/AIDS. AIDS Patient Care STDS, 19, 587–598. doi:10.1089/apc.2005.19.587.
Gore-Felton, C., Koopman, C., Turner-Cobb, J. M., Duran, R. E., Israelski, D., & Spiegel, D. (2002). The influence of social support, coping, and mood on sexual risk behavior among HIV-positive men and women. Journal of Health Psychology, 7, 713–722. doi:10.1177/1359105302007006874.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The corresponding author declares that he has no conflict of interest. The second author declares that she has no conflict of interest. The third author also declares that she has no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Rzeszutek, M., Gruszczyńska, E. & Firląg-Burkacka, E. Coping profiles and subjective well-being among people living with HIV: less intensive coping corresponds with better well-being. Qual Life Res 26, 2805–2814 (2017). https://doi.org/10.1007/s11136-017-1612-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-017-1612-7