Abstract
Purpose
To test whether improvement in glycosylated haemoglobin (HbA1c) as a marker of glycaemic control, following intensifying insulin therapy, is associated with improvements in HRQoL.
Methods
Dutch sub-optimally controlled (HbA1c > 7%) type 2 diabetes patients (N = 447, mean age 59 ± 11) initiated insulin glargine therapy. Data were collected at baseline, 3 and 6 months, and included HbA1c and measures of HRQoL: diabetes symptom distress (Diabetes Symptom Checklist-revised; DSC-r), fear of hypoglycaemia (Hypoglycaemia Fear Survey; HFS-w) and emotional well-being (WHO-5 wellbeing index).
Results
HbA1c decreased from 8.8 ± 1.4% to 8.0 ± 1.2% and 7.7 ± 1.3% at 3 and 6 months follow-up, respectively (P < 0.001), DSC-r score improved from 17.7 ± 14.7 to 14.3 ± 13.3 and 13.6 ± 13.3 (P < 0.001). HFS-w score did not significantly change. WHO-5 score increased from 56 ± 23 to 62 ± 23 and 65 ± 22 P < 0.001). A modest, significant association was found between HbA1c and WHO-5 score (B = −1.8, 95% CI: −2.7 to −0.8) and HbA1c and DSC-r score (B = 1.0, 95% CI: 0.4 to 1.6). No such association was found for HFS-w score.
Conclusions
An association between improvement in HbA1c by means of optimising insulin therapy and improvement in HRQoL in type 2 diabetes patients has been observed. A weak, yet significant longitudinal association was found between improved HbA1c and emotional well-being and diabetes symptom distress.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
It is estimated that worldwide 220 million people have type 2 diabetes mellitus [1], a chronic illness characterised by hyperglycaemia due to insulin resistance and beta-cell dysfunction. Diabetes is a burdensome disease that can seriously impair the quality of life of patients and is accompanied by huge economical costs mainly caused by debilitating micro- and macrovascular complications [2]. Hyperglycaemia plays a crucial role in the pathogenesis of diabetes-related complications [2]. Diabetes treatment should therefore aim for optimal glycaemic control (usually defined as HbA1c ≤ 7%), while preserving patients’ quality of life [3, 4]. To this end, different pharmacological interventions are available. Due to progressive beta-cell failure, most type 2 diabetes patients will require insulin therapy at some point [4], exposing them to an increased risk of hypoglycaemia and death [5, 6].
In the past, NPH (Neutral Protamine Hagedorn) insulin was commonly used as long-acting insulin, which has a pronounced insulin peak 4–8 h post-injection. In the past decades, so-called long-acting basal insulin analogues, insulin glargine and insulin detemir, have been developed. Such insulins are relatively easy to use and have a prolonged, consistent duration of action, covering 18–24 h, with low rates of hypoglycaemia [7]. Favourable effects on health-related quality of life (HRQoL) have been reported after initiation of long-acting insulin therapy [7, 8], but evidence is scarce.
While a modest association has been found between depression and higher HbA1c [9], an important question in the context of diabetes treatment that remains unresolved pertains to the relationship between glycaemic control and patients’ HRQoL. Improved glycaemic control can directly positively affect HRQoL by reducing burdensome symptoms, such as fatigue, cognitive distress and blurred vision, and indirectly by reduced worries about secondary diabetes complications, the presence of which is being regarded as the largest threat to HRQoL in patients with diabetes [10, 11]. On the other hand, stricter glycaemic control can also negatively affect HRQoL due to a higher risk of hypoglycaemia and concomitant anxieties [12]. A landmark study in type 2 diabetes, the United Kingdom Prospective Diabetes Study (UKPDS) has shown that optimisation of treatment with the aim to achieve strict glycaemic control did not negatively affect patients’ well-being. However, the experience of severe hypoglycaemic episodes was found to be related to a deterioration of quality of life, particularly in the domain of mood [13].
Another study into the relationship between glycaemic control and HRQoL in older male type 2 diabetes patients found no cross-sectional or longitudinal relation [14]. However, a Dutch cross-sectional study did find a correlation between HbA1c and mood status (r = 0.23, P < 0.01) [15]. This study also used a diabetes-specific measure (diabetes symptom distress), which showed a negative association with better glycaemic control, i.e. less symptom burden with lower HbA1c (−1 point on DSC-r score for each per cent of HbA1c reduction). In addition, improving glycaemic control in sub-optimally controlled type 2 diabetes patients on oral medication has been demonstrated to improve quality of life, which was defined by the authors as 5 visual analogue scales: perceived health, mental and emotional health, self reported cognitive function, general health perceptions and symptom distress. Patients improved 0.2 SD on the sum of these scales [16].
To date, research examining the relationship between (improving) glycaemic control and HRQoL is limited and inconsistent. Therefore, we set out to study the relationship between glycaemic control and HRQoL in type 2 diabetes.
Data were derived from an observational cohort study carried out in the Netherlands, aimed to study the impact of initiating long-acting insulin on HRQoL in type 2 diabetes patients.
Patients and methods
Study sample
In the present analysis, data from the observational ESPRIT (Effect Study on Patient-Reported outcomes in Insulin glargine Treatment) study were used. The study was conducted between 2005 and 2008 in the Netherlands. In this study, diabetes specialists invited patients with type 2 diabetes who were in sub-optimal control (HbA1c > 7%) to participate. Inclusion criteria were: type 2 diabetes mellitus, an age of 18 years or older, current treatment with basal insulin and a clinical need to initiate insulin glargine. The decision to initiate treatment with insulin glargine as basal therapy was made at the discretion of the treating diabetes specialist. The study did not interfere with clinical practice and only included filling out a questionnaire booklet that took about 15 min at three consecutive periodic consultations. The questionnaire booklet was provided to the patient by the treating physician. Clinical data were retrieved from the medical chart. In view of the observational and non-invasive nature, the present study was not subject to the Dutch Medical Research Involving Human Subjects Act. Standardised study information and informed consent were provided to all patients and diabetes specialists.
In total, 510 type 2 diabetes patients from 116 out-patient clinics were included. Refusal rates were unknown. Sixty-three patients were found to be in good glycaemic control upon inclusion (HbA1c ≤ 7%) and were therefore excluded from analysis, resulting in a study population of N = 447 in sub-optimal glycaemic control. Fifty-two per cent of the patients (N = 233) received NPH insulin as basal therapy prior to initiating insulin glargine, 29% (N = 130) of the patients received premixed insulin and 19% (N = 84) received insulin detemir as basal therapy. Of the total population, 240 patients (54%) also received rapid-acting (meal-time related) insulin as co-therapy prior to therapy optimisation.
Measures
Demographic and clinical data were obtained at baseline, 3 and 6 months by means of self report and included age, gender, weight, height, time since diagnosis, previous medication use, hypoglycaemic episodes, the presence of diabetes-related complications, and co-morbidities. HbA1c and Fasting Blood Glucose (FBG), measured according to DCCT standards were retrieved from the medical chart. Adverse events were recorded by the treating physician, treated accordingly and reported to the researchers.
HRQoL is a multi-dimensional concept [17], in this study operationalised as a low level of diabetes symptom distress and fear of hypoglycaemia and a high level of emotional well-being.
Diabetes-related symptom distress was measured using the revised version of the Diabetes Symptom Checklist (DSC-r), that has been shown to have good psychometric properties [18, 19]. The DSC-r consists of 34 items grouped into eight symptom sub-scales: Hyperglycaemia, Hypoglycaemia, Cognitive distress, Fatigue, Cardiovascular distress, Neuropathic pain, Neuropathic sensibility and Ophthalmologic function. Each item asks about the presence of complaints (yes/no) and if present, to score the level of distress on a 5-point Likert type scale (i.e. ‘Have you experienced numbness in the hands?’ (yes/no), ‘How troublesome was this symptom for you?’ (Likert scale)). Scores are then transformed to a 0–100 score to obtain the DSC-r total distress score, with higher scores indicating more diabetes symptom distress. This transformation was also applied to the DSC-r sub-scales.
The Dutch version of the 13 item Worry sub-scale of the Hypoglycaemia Fear Survey (HFS-w) [20] was used to measure worries about hypoglycaemia. To facilitate interpretation of data, HFS-w scores were also transformed to a 0–100 scale, with higher scores indicating higher worry about hypoglycaemia.
The WHO-5 well-being index [21], a validated 5-item instrument, was used to assess general emotional well-being. The WHO-5 covers positive mood (good spirits, relaxation), vitality (being active and waking-up fresh and rested), and general interests (being interested in things). Item scores are summated to provide a total well-being score, transformed to a 0–100 scale, with lower scores indicating poorer well-being.
In the present study, the Cronbach’s alpha’s for the HFS, DSC-r total score and WHO-5 were 0.88, 0.94 and 0.90, respectively, confirming high internal consistency.
Statistical analyses
Generalised estimating equations (GEE) analysis was used for all longitudinal analyses. To test whether HbA1c, fasting blood glucose, hypoglycaemia, BMI, insulin dosage (insulin glargine and rapid-acting insulin) and scores on HFS-w, DSC-r and WHO-5 changed during the study period for the total population, time was modelled as an independent dummy variable and the outcome measure as dependent variable. For these analyses, effect sizes (Cohen’s d) for 6 month follow-up scores compared to baseline scores were calculated, to gain insight in clinical relevance.
To study whether improvement in HbA1c, by means of intensifying insulin therapy was related to improvement in HRQoL, GEE analyses were carried out with HbA1c as independent variable and HFS-w score, DSC-r score and WHO-5 score, respectively as dependent variable.
Variables with a right-skewed distribution (time since diagnosis, the number of diabetes complications, the number of co-morbidities, the number of symptomatic, nocturnal and severe hypoglycaemic episodes during the past 3 months, HFS-w total score and DSC-r total and sub-scores) were transformed with a natural logarithm for the purpose of statistical testing. In case of a right-skewed distribution, the median, 25th and 75th percentiles are presented.
We have studied the following variables as potential confounders: age, sex, time since diagnosis, BMI, the number of diabetes-related complications and the number of co-morbidities by adding them to the GEE model and looking if the coefficient of the main independent variable changed by more than ten per cent. Time-varying covariates (BMI and the number of symptomatic, nocturnal and severe hypoglycaemic episodes) were treated as such in the analysis. In case confounding, existed analyses were corrected for that specific variable. Moreover, we tested effect modification for sex, as a stronger association between glycaemic control and depression has previously been observed in women [22]. In case of effect modification, analyses were stratified for sex.
Observational studies run a high risk of missing data, due to the naturalistic setting and low level of monitoring. The present study was no exception; at the start of the study, 19% of patients had missing data on the HFS-w, 23% on the DSC-r and 10% on the WHO-5. At 3 month follow-up, these percentages increased to 35, 37 and 27%, respectively. At 6 month follow-up they further increased to 42, 40 and 33%. Missing data were imputed using multiple imputations [23, 24]. The imputation model consisted of age, sex, time since diagnosis, the number of complications, the number of co-morbidities, HbA1c, FBG, the number of symptomatic, nocturnal and severe hypoglycaemic episodes, type of insulin used, and scores on the remaining two HRQoL instruments. Five datasets were generated using this technique. Analyses on these datasets were combined using Rubin’s rules for multiple imputations [23].
Results
Baseline characteristics of the study population and changes over time in clinical and HRQoL-related outcome variables are presented in Table 1. At insulin therapy optimisation, 382 (85%) patients received rapid-acting insulin as co-therapy. At 3 months, this increased to 442 (99%) patients and remained unchanged at 6 months.
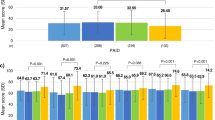
Two adverse events were related to glargine treatment; one patient experienced an allergic reaction and another patient was hospitalised as consequence of a severe hypoglycaemic episode. Prior to insulin therapy optimisation, mean HbA1c for the total patient population was 8.8 ± 1.4% which decreased to 8.0 ± 1.2% and 7.7 ± 1.3% at 3 and 6 month follow-up, respectively (P < 0.001). Additionally, FBG improved from 10.2 ± 3.7 mmol/l to 8.5 ± 2.8 and 8.4 ± 2.9 mmol/l (P < 0.001). The number of symptomatic hypoglycaemic events patients reported to have experienced during the past 3 months decreased from a median of 3 (25th percentile 0, 75th percentile 7) to 2 (0, 6; P = 0.042) at 3 month follow-up, after which it remained stable, though statistical significance did not remain (median 2, 25th percentile 0, 75th percentile 6; p between baseline and 6 month follow-up 0.052). The percentage of patients who had experienced one or more symptomatic hypoglycaemic event(s) decreased significantly during the follow-up period from 74% to 67 and 67% (P = 0.044). The number of nocturnal hypoglycaemic events significantly decreased from 1.5 ± 3.9 to 1.0 ± 2.4 and 0.8 ± 2.1, respectively (P = 0.001), along with the percentage of patients who had experienced one or more nocturnal events (from 39% to 29 and 24%, respectively; P = 0.001). Eleven per cent of the patients (n = 48) reported to have experienced at least one severe hypoglycaemic event 3 months prior to glargine initiation. This percentage did not significantly change during the study period.
The median number of symptoms patients reported on the DSC-r at baseline was 13 (25th percentile 8, 75th percentile 19). This decreased to 12 (6, 19) and 10 (5, 18) at 3 and 6 months, respectively (P < 0.001). The DSC-r total distress score was already relatively low prior to glargine initiation (median 14, 25th percentile 6, 25th percentile 26) but nevertheless decreased at 3 (11, 4, 21) and 6 months (10, 4, 20), respectively (Cohen’s d 0.27; P < 0.001). The largest improvements were observed in the sub-domains Fatigue (from 25 (6, 50) to 19 (6, 44) and 19 (0, 38), respectively; Cohen’s d 0.29; P < 0.001), Cognitive distress (from 13 (0, 31) to 6 (0, 25) and 6 (0, 25); Cohen’s d 0.24; P < 0.001) and Hyperglycaemia (from 13 (6, 31) to 6 (0, 19) and 6 (0, 19); Cohen’s d 0.30; P = 0.003).
Mean Worries about hypo’s (HFS-w) score showed a slight, non-significant decrease during the study period (from a median of 15 (25th percentile 4, 75th percentile 27) to 12 (4, 29) and 13 (4, 35); Cohen’s d 0.17; P = 0.610).
Mean emotional well-being (WHO-5) score was 56 ± 23 at baseline, which improved to 62 ± 23 at 3 and 65 ± 22 at 6 month follow-up (Cohen’s d 0.39; P < 0.001).
Longitudinal analyses revealed a modest, statistically significant association between change in HbA1c and change in WHO-5 score (standardised B = −2.6, 95% CI: −3.6 to −1.5; P < 0.001, Table 2). Adjustment for demographic variables (age, sex, educational level, time since diagnosis, the number of diabetes complications and the number of co-morbidities) and baseline WHO-5 score showed that the association was still significant, albeit somewhat lower (standardised B = −1.7 (95% CI: −2.6 to −0.8; P < 0.001). Further adjustment for hypoglycaemia did not alter these coefficients (standardised B = −1.8 (95% CI: −2.7 to −0.8; P < 0.001). For DSC-r total score, the uncorrected coefficient was B = 1.4 (95% CI: 0.8 to 2.0; P < 0.001). After correction for demographic variables and baseline DSC-r score, the association became B = 1.0 (95% CI: 0.4 to 1.5; P = 0.010). Further adjustment for hypoglycaemia did not change the coefficient further. For the HFS-w, no significant association with HbA1c was found.
Discussion
In this 6 month observational study conducted in multiple secondary care practices in the Netherlands, significant improvement in HbA1c was observed following insulin therapy optimisation in sub-optimally controlled type 2 diabetes patients. However, mean HbA1c at study endpoint was still sub-optimal. Also, a decrease in symptomatic and nocturnal hypoglycaemia was observed, in line with previous findings [7]. Importantly, significant improvements in two of the three chosen HRQOL outcomes were observed. Diabetes symptom distress (DSC-r) scores were relatively low at baseline compared to other studies [15, 25], but nevertheless improved slightly. Whether this improvement is clinically relevant (4 points) is not clear, but it does exceed previously reported changes in DSC-r score at a follow-up period of one year, in the range of −0.11–0.25 SD (the change in the present study was 0.28 SD) [26]. Cohen’s d for change in DSC-r total score was 0.27, which can be interpreted as a ‘small’ effect. Emotional well-being improved 9.4 points on the WHO-5 well-being index, close to a clinically relevant improvement of 10 points, as defined by the authors of the instrument [21]. Cohen’s d for WHO-5 improvement was 0.39, which can be interpreted as a ‘moderate’ effect.
The results of our study confirm that glycaemic improvement is associated with positive effects on patients’ HRQoL at least over the first 6 months. While statistical significant longitudinal associations between HbA1c and WHO-5 and DSC-r score were found, they were not strong. However, the association remained, even after corrections for demographic and clinical variables and hypoglycaemia. To establish longer-term effects, further research is warranted. We should of course recognize that establishing a longitudinal association does not provide us with a mechanistic explanation or proof of causation. Physiological, emotional and behavioural factors are likely to play a role.
The increase in emotional well-being might very well be related to factors that are not measured in this study, such as the increased sense of freedom patients may experience with their new treatment regimen. At the end of the study, almost all patients received insulin glargine and a rapid-acting insulin analogue, allowing for more dietary freedom in their daily life, which has previously been shown to increase treatment satisfaction and quality of life in type 1 diabetes patients [27]. Unfortunately, the intensity of care that patients received was not documented in the study. When intensified insulin therapy is instituted, the amount of visits is possibly increased, which may have contributed to improved satisfaction with care and well-being.
The observational design of our study invokes four noteworthy other limitations: A Hawthorne effect cannot be excluded, missing data was present, the lack of blinding and the lack of a control group. Another limitation of the study is that refusal rates and reasons for refusal were not documented. It would, however, seem very unlikely that the observed improvements in emotional well-being following therapy optimisation at 3 months, sustained at 6 months are merely due to an expectancy effect, because the observed decrease nearly reached clinical relevance, defined as a change in WHO-5 score of 10 points [30]. Furthermore, missing data were addressed using a state of the art technique [24].
Our findings add to the literature pointing at the complex relation between glycaemic control (HbA1c) and patient-reported outcomes. In this context, we should recognize that HbA1c is not an instant measure of blood glucose, but rather an indication of mean blood glucose values over a longer period of time (6–8 weeks). While a high HbA1c is an important risk factor for long-term vascular complications in diabetes patients, HbA1c does not directly translate into tangible symptoms, because it is a weighted measure of mean blood glucose over the preceding 120 day period [28]. Indeed many patients are unaware of their HbA1c level [29]. More research on the subject is warranted, incorporating measures of treatment burden and patient satisfaction [30].
Conclusions
In this study, an association is observed between improving HbA1c, by optimising insulin therapy in type 2 diabetes patients and improvement in HRQoL. A weak, yet significant longitudinal association was found between improved HbA1c and emotional well-being. Our findings add to the literature on the complex relationship between glycaemic control and quality of life.
References
King, H., Aubert, R. E., & Herman, W. H. (1998). Global burden of diabetes, 1995–2025: Prevalence, numerical estimates, and projections. Diabetes Care, 21, 1414–1431.
Turner, R., Cull, C., & Holman, R. (1996). United Kingdom prospective diabetes study 17: A 9-year update of a randomized, controlled trial on the effect of improved metabolic control on complications in non-insulin-dependent diabetes mellitus. Annals of Internal Medicine, 124, 136–145.
U.K. Prospective Diabetes Study Group. (1998). Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet, 352, 837–853.
(2010). Standards of medical care in diabetes–2010. Diabetes Care, 33(Suppl 1), S11–S61.
UK Hypoglycaemia Study Group. (2007). Risk of hypoglycaemia in types 1 and 2 diabetes: Effects of treatment modalities and their duration. Diabetologia, 50, 1140–1147.
Dluhy, R. G., & McMahon, G. T. (2008). Intensive glycemic control in the ACCORD and ADVANCE trials. The New England Journal of Medicine, 358, 2630–2633.
Horvath, K., Jeitler, K., Berghold, A., Ebrahim, S. H., Gratzer, T. W., Plank, J. et al. (2007). Long-acting insulin analogues versus NPH insulin (human isophane insulin) for type 2 diabetes mellitus. Cochrane database of systematic reviews, 2 Art. no. CD005613.
Swinnen, S. G., Dain, M. P., Aronson, R., Davies, M., Gerstein, H. C., Pfeiffer, A. F., et al. (2010). A 24-week, randomized, treat-to-target trial comparing initiation of insulin glargine once-daily with insulin detemir twice-daily in patients with type 2 diabetes inadequately controlled on oral glucose-lowering drugs. Diabetes Care, 33, 1176–1178.
Lustman, P. J., Anderson, R. J., Freedland, K. E., de, G. M., Carney, R. M., & Clouse, R. E. (2000). Depression and poor glycemic control: A meta-analytic review of the literature. Diabetes Care, 23, 934–942.
Rubin, R. R., & Peyrot, M. (1999). Quality of life and diabetes. Diabetes/Metabolism Research and Reviews, 15, 205–218.
Lloyd, A., Sawyer, W., & Hopkinson, P. (2001). Impact of long-term complications on quality of life in patients with type 2 diabetes not using insulin. Value Health, 4, 392–400.
Gonder-Frederick, L. A., Clarke, W. L., & Cox, D. J. (1997). The emotional, social, and behavioral implications of insulin-induced hypoglycemia. Seminars in Clinical Neuropsychiatry, 2, 57–65.
U. K. Prospective Diabetes Study Group. (1999). Quality of life in type 2 diabetic patients is affected by complications but not by intensive policies to improve blood glucose or blood pressure control (UKPDS 37). Diabetes Care, 22, 1125–1136.
Weinberger, M., Kirkman, M. S., Samsa, G. P., Cowper, P. A., Shortliffe, E. A., Simel, D. L., et al. (1994). The relationship between glycemic control and health-related quality of life in patients with non-insulin-dependent diabetes mellitus. Medical Care, 32, 1173–1181.
Van der Does, F. E., De Neeling, J. N., Snoek, F. J., Kostense, P. J., Grootenhuis, P. A., Bouter, L. M., et al. (1996). Symptoms and well-being in relation to glycemic control in type II diabetes. Diabetes Care, 19, 204–210.
Testa, M. A., & Simonson, D. C. (1998). Health economic benefits and quality of life during improved glycemic control in patients with type 2 diabetes mellitus: A randomized, controlled, double-blind trial. The Journal of the American Medical Association, 280, 1490–1496.
Hunt, S. M. (1997). The problem of quality of life. Quality of Life Research, 6, 205–212.
Arbuckle, R. A., Humphrey, L., Vardeva, K., Arondekar, B., Danten-Viala, M., Scott, J. A., et al. (2009). Psychometric evaluation of the diabetes symptom checklist-revised (DSC-R)—a measure of symptom distress. Value Health, 12, 1168–1175.
Grootenhuis, P. A., Snoek, F. J., Heine, R. J., & Bouter, L. M. (1994). Development of a type 2 diabetes symptom checklist: A measure of symptom severity. Diabet Medicine, 11, 253–261.
Cox, D. J., Irvine, A., Gonder-Frederick, L., Nowacek, G., & Butterfield, J. (1987). Fear of hypoglycemia: Quantification, validation, and utilization. Diabetes Care, 10, 617–621.
Bech, P., Olsen, L. R., Kjoller, M., & Rasmussen, N. K. (2003). Measuring well-being rather than the absence of distress symptoms: a comparison of the SF-36 mental health subscale and the WHO-five well-being scale. International Journal of Methods in Psychiatric Research, 12, 85–91.
Pouwer, F., & Snoek, F. J. (2001). Association between symptoms of depression and glycaemic control may be unstable across gender. Diabet Medicine, 18, 595–598.
Rubin, D. B. (1987). Multiple imputation for nonresponse in surveys. New York: Wiley & Sons.
Schafer, J. L., & Graham, J. W. (2002). Missing data: Our view of the state of the art. Psychological Methods, 7, 147–177.
de Sonnaville, J. J., Snoek, F. J., Colly, L. P., Deville, W., Wijkel, D., & Heine, R. J. (1998). Well-being and symptoms in relation to insulin therapy in type 2 diabetes. Diabetes Care, 21, 919–924.
Arbuckle, R. A., Humphrey, L., Vardeva, K., Arondekar, B., nten-Viala, M. M., Scott, J. A. et al. (2009). Psychometric evaluation of the diabetes symptom Checklist-revised (DSC-R)—a measure of symptom distress. Value Health.
DAFNE Study Group. (2002). Training in flexible, intensive insulin management to enable dietary freedom in people with type 1 diabetes: dose adjustment for normal eating (DAFNE) randomised controlled trial. British Medical Journal, 325, 746.
Goldstein, D. E., Little, R. R., Lorenz, R. A., Malone, J. I., Nathan, D., & Peterson, C. M. (1995). Tests of glycemia in diabetes. Diabetes Care, 18, 896–909.
Heisler, M., Piette, J. D., Spencer, M., Kieffer, E., & Vijan, S. (2005). The relationship between knowledge of recent HbA1c values and diabetes care understanding and self-management. Diabetes Care, 28, 816–822.
Rubin, R. R., & Peyrot, M. (2010). Patient-reported outcomes and diabetes technology: A systematic review of the literature. Pediatric Endocrinology Reviews, 7(Suppl 3), 405–412.
Acknowledgments
This study was financially supported by an unrestricted grant of Sanofi-Aventis.
Open Access
This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License (https://creativecommons.org/licenses/by-nc/2.0), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Hajos, T.R.S., Pouwer, F., de Grooth, R. et al. The longitudinal association between glycaemic control and health-related quality of life following insulin therapy optimisation in type 2 diabetes patients. A prospective observational study in secondary care. Qual Life Res 21, 1359–1365 (2012). https://doi.org/10.1007/s11136-011-0051-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-011-0051-0