Abstract
Background
Early administration of intravenous (IV) caffeine (initiation within 2 days of life) is an effective treatment strategy for the management of apnoea of prematurity among infants. However, the safety and effectiveness of early administration of oral caffeine treatment is not be fully established.
Aim
We aimed to compare the effectiveness and safety of early versus late caffeine therapy on preterm infants’ clinical outcomes.
Method
A retrospective matched cohort study was conducted using data of patients admitted to neonatal intensive care units of two tertiary care hospitals between January 2016 and December 2018. The clinical outcomes and mortality risk between early caffeine (initiation within 2 days of life) and late caffeine (initiation ≥ 3 days of life) were compared.
Results
Ninety-five pairs matched based on gestational age were included in the study. Compared to late initiation, preterm infants with early caffeine therapy had: a shorter duration of non-invasive mechanical ventilation (median 5 days vs. 12 days; p < 0.001); shorter length of hospital stay (median 26 days vs. 44 days; p < 0.001); shorter duration to achieve full enteral feeding (median 5 days vs. 11 days; p < 0.001); and lower frequency of bronchopulmonary dysplasia (BPD) (4.5% vs. 12.9%; p = 0.045). They also had a reduced risk of osteopenia of prematurity (OP) (OR 0.209; 95% CI 0.085–0.509; p = 0.001).
Conclusion
Early oral caffeine therapy can potentially improve respiratory outcomes among infants with apnoea of prematurity. However, an increase in mortality associated with early caffeine therapy requires further investigation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Impact statements
-
Early administration of oral caffeine (initiation within 2 days of life) can be an effective treatment strategy for the management of apnoea of prematurity among infants, especially in settings where IV caffeine is not available.
-
Safety of early administration of oral caffeine treatment cannot be fully established and requires further investigation using well-designed randomized controlled trials.
-
Infant developmental milestones need to be carefully monitored among perterm infants who had received oral caffeine.
Introduction
Preterm birth complications are the leading cause of mortality among under-5 years old, accounting for approximately 16% of 5.9 million under-5 deaths [1]. Apnoea of prematurity (AOP) is a preterm complication due to a developmental disorder that frequently affects preterm infants [2]. AOP is defined as an interruption of breathing for more than 20 s, or a shorter respiratory cessation period but associated with oxygen desaturation and/or bradycardia in preterm infants younger than 37 weeks of gestation [3]. Prolonged apnoea, bradycardia and reduced cerebral blood flow may lead to hypoxic-ischaemic harm to the infant’s developing brain [4].
Methylxanthines such as caffeine citrate or theophylline are the primary pharmacological agents used to treat AOP [5]. Caffeine citrate is the preferred therapy for AOP due to its pharmacokinetic profile of long half-life and good oral absorption [6, 7]. The Caffeine for Apnoea of Prematurity trial concluded that early caffeine therapy (initiation within 2 days of life) is associated with fewer intubation episodes and reduced use of positive pressure ventilation compared to late caffeine therapy (initiation from day 3 of life onwards) [8]. Caffeine has interethnic pharmacokinetic differences. CYP1A2 is the main caffeine metabolism enzyme encoded by the CYP1A2 gene which has gene polymorphism leading to interindividual variability [9, 10]. Although a recent study concluded that there was no significant association between CYP1A2 gene variation and caffeine pharmacokinetic parameters [10], the genetic polymorphisms in caffeine targeting the adenosine receptor induced different clinical responses to caffeine therapy [11, 12].
In Malaysia, the fourth report of the National Obstetrics Registry stated that 8.9% of the total number of deliveries in 15 state hospitals were preterm in 2017 [13]. The routine practice for managing AOP in a neonatal intensive care unit (NICU) in Malaysia is to initiate methylxanthines prophylatically with a loading dose of IV aminophylline, followed by a maintenance dose of IV aminophylline, and then to switch to oral caffeine after initiation of oral feeding in infants with gestational age less than 32 weeks. For those infants with gestational age between 32 and 34 weeks, treatment is given if present with apnoea symptoms. This practice has been adopted due to the non-availability of caffeine citrate injections in the majority of the Malaysian government hospitals, as the drug is not listed in the Malaysian Ministry of Health (MOH) National Drug Formulary, and there is a lack of safety data on the early initiation of an oral caffeine solution. Hospital pharmacists make an oral caffeine solution from caffeine powder as an alternative to caffeine citrate injections. Therefore, the caffeine therapy initiation is usually onwards from day three of life, which is classified as late caffeine therapy. Owing to the fact that caffeine is the preferred therapy in the management of AOP [3], some NICUs adopted the practice of off-label early oral caffeine therapy in preterm infants. The safety of administering oral caffeine to preterm infants before initiation of oral feeding is uncertain, however, as the published studies on early caffeine therapy were carried out with intravenous administration of caffeine.
Aim
In order to inform local practice and policy with regards to the management of AOP, this multicentre study was carried out by a group of clinical pharmacists to investigate the effectiveness and safety of early oral caffeine therapy on preterm infants’ clinical outcomes.
Ethics approval
This research project was given ethical approvalby the Ministry of Health Medical Research Ethical Committee (MREC) [Approval number: NMRR-19-423-45654; reference number KKM/NIHSEC/P19-769(5), dated 26 April 2019]. The study adhered fully to the guidelines outlined in the Declaration of Helsinki.
Method
This retrospective cohort study was carried out at two Level III NICUs in Malaysia. Level III (subspecialty) NICUs have the personnel (neonatologists, neonatal nurses, respiratory therapists) and equipment to provide life support for as long as needed. The study population included all preterm infants born at less than 37 weeks gestational age and admitted to an NICU within 24 h of life between January 2016 and December 2018. Infants with major congenital malformation, treated with an inappropriate caffeine dosing regimen (not adhering to local practice protocol of oral caffeine dose range of 5–10 mg/kg daily), and infants with missing data on caffeine therapy were excluded from the study.
Sample size
Sample size was calculated using two population proportions formulae [14, 15]. The sample size was calculated based on the incidence of diagnosis of bronchopulmonary dysplasia (BPD). Previous data indicated that the proportion of BPD in the early group was 0.20 and the proportion of the late group was 0.346 [14]. Thus, the minimum sample size of 145 samples per group was required with 80% power and a p-value of 0.05. According to finite population of 417 patients in Hospital Putrajaya and 363 patients in Hospital Serdang respectively, the corrected sample size of patients for Hospital Putrajaya and Hospital Serdang was 108 and 104 samples respectively. With an additional of 20% dropout samples due to incomplete data, the sample size was at least 130 samples per group [15].
Data collection
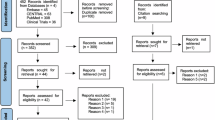
A random sampling method was conducted to select samples for this study. The relevant patients’ registry numbers extracted from the hospital databases were randomly selected by using random numbers generated by the Microsoft Excel program. All data were extracted from the electronic medical records database. Data were collected until death or discharge from the NICU. The flow of patient selection during the study is shown in Figure S1. Based on the timing of caffeine therapy initiation, preterm infants were divided into 2 groups: early caffeine therapy (caffeine initiation within 2 days of life) and late caffeine therapy (caffeine initiation ≥ 3 days of life). The baseline demographics and clinical outcomes were compared between the two groups. A structured pilot-tested data collection form was used to standardize data collection. The outcomes measured included: BPD, ventilation days, length of hospital stay (LOS), average weight gain, osteopenia of prematurity (OP), death, duration to reach full enteral feeding, and necrotising enterocolitis.
Outcome measures: key definitions
BPD was defined as the need for a continuous supplemental oxygen concentration > 21% by nasal cannula, nasal catheter, face mask or respiratory support for at least 28 continuous days or by corrected age of 36 weeks, or more than 56 days of postnatal age for infants born after more than 32 weeks gestation [16].
The duration of mechanical ventilation was defined as the total number of days preterm infants required mechanical ventilation support, whereas non-invasive respiratory ventilation support includes continuous positive airway pressure (CPAP), bilevel positive airway pressure (BiPAP), or high-flow nasal cannula (HFNC) [17].
Extubation failure was defined as the need to resume mechanical ventilation within less than 72 h. Reintubation was defined as the need for reintubation at any time after 72 h of extubation [18].
The length of hospital stay was defined as the total number of NICU admission days.
Necrotising enterocolitis was defined according to Bell criteria: it was diagnosed clinically or radiologically by a ward neonatologist [19].
OP was diagnosed biochemically with the elevation of serum ALP > 500U/L or serum phosphate < 1.8 mmol/L [20, 21].
Data analysis
Propensity score matching (PSM) was used minimize the impact of baseline characteristic differences between early and late caffeine therapy groups on the treatment outcomes[22]. The two groups were matched based on gestational age. All data were analyzed using the IBM Statistical Package for Social Sciences (SPSS) version 24.0 software. Comparison of numerical data (such as LOS, duration of mechanical ventilation etc.) between early caffeine therapy and late caffeine therapy groups that were normally distributed were analyzed using the independent t-test, while the Mann–Whitney test was used if the data for two independent groups were not normally distributed. To study the association between two sets of categorical data (such as BPD and study group, OP and study group etc.), Pearson's Chi-square test for Independence was used, while Fisher's exact test was used if the assumptions of Pearson's Chi-square test for independence were violated. Binary logistic regression was used to test for significant predictors among the independent variables. The risk was expressed as an odds ratio (OR) with 95% CI. A 2-sided p-value < 0.05 was considered statistically significant for all tests.
Results
Baseline characteristics
A total of 190 preterm infants meeting the inclusion criteria for the study were PS matched in 1:1 ratio based on gestational age. The mean gestational age between early and late caffeine therapy group was similar (31.23 weeks vs. 30.61 weeks; p-value = 0.055).. The median postnatal age caffeine therapy initiation was 1 day (range 0–1 day of life) and 13 days (range 6–13 days of life) in early and late caffeine therapy groups, respectively (Table 1). Study results showed that preterm infants treated with early caffeine had higher mean birth weight compared to those in the late caffeine group (1.53 kg vs. 1.33 kg; p-value = 0.001). There were no significant differences in ethnicity, gender, Apgar score, mode of delivery, maternal chorioamnionitis, maternal gestational diabetes and hypertension between the two groups. Antenatal steroid administration was higher in the early caffeine group. Nearly all mothers in the early caffeine commencement group were administered an antenatal steroid following the standard protocol of total dose of intramuscular administration of Dexamethasone 24 mg prior to delivery compared to only three-fifths of mothers in the late caffeine group.
Respiratory outcomes
Respiratory outcomes were studied among 182 infants, excluding those preterm infants who passed away prior to hospital discharge.. Preterm infants with early caffeine therapy had a shorter duration of non-invasive mechanical ventilation and were able to be weaned off oxygen support 9 days earlier than those in the late caffeine therapy group (p-value < 0.001) (Table 2). The number of infants who developed BPD was significantly lower in the early caffeine group compared with the late caffeine group (4.5% vs. 12.9%; p-value = 0.045). We analyzed 131 intubated preterm infants. The results showed that early caffeine therapy non-significantly reduces extubation failure among preterm infants as compared to late caffeine therapy (p-value = 0.690), with a difference of 2%. Preterm infants in both early and late caffeine therapy groups had similar duration of invasive mechanical ventilation (median 2, IQR (3), p-value = 0.219).
Direct multivariate logistic regression analysis was performed to identify the factors that predict BPD among preterm infants (Table 3). The model contained five independent variables (gestational age, birth weight, small for gestational age, administered antenatal steroid and caffeine administration timing). Early caffeine therapy reduced the risk of developing BPD by nearly 1.5 times compared to late caffeine therapy among preterm infants, though this result was not statistically significant (OR 1.41; 95% CI 0.296–6.757, p-value = 0.664).
Early caffeine and neonatal outcomes
Preterm infants treated with early caffeine achieved full enteral feeding 6 days earlier and were discharged home 18 days earlier than those in the late caffeine therapy group (p-value < 0.001). On the other hand, early caffeine therapy was associated with significantly lower daily weight increment (p-value < 0.001). There was a higher proportion of preterm infants’ death in the early caffeine group compared to the late caffeine therapy group although this result was not statistically significant (6.3% vs. 2.1%, p-value = 0.279) (Table 4).
Adverse effects
Preterm infants treated with late caffeine therapy were more likely to be diagnosed with OP when compared to those treated with early caffeine initiation (29% vs. 7.9%, p-value < 0.001) (Table 4). The proportions of necrotising enterocolitis and tachycardia in these two groups were identical (p-value = 1).
A direct multivariate logistic regression was performed to assess the factors that predict OP among preterm infants. The final model contained 5 independent variables (gestational age, birth weight, TPN duration, cumulative caffeine dose and caffeine administration timing). The odds of a preterm infant being diagnosed as OP were about 2 times higher for the late caffeine therapy group compared to the early caffeine therapy group, though the association was not statistically significant (OR 0.532; 95% CI 0.156–1.820, p-value = 0.315) (Table 5).
More importantly, the odds of death prior to hospital discharge among preterm infants were about 8 times higher in the early caffeine therapy group compared to the late caffeine therapy group (OR 8.058; 95% CI 1.063–61.065, p-value = 0.043) (Table 6).
Discussion
The aim of this study was to compare the effectiveness and safety of early versus late caffeine therapy for the management of AoP on preterm infants’ clinical outcomes. This study adds to existing evidence on the safety and efficacy of oral caffience therapy and the time of initiation of oral caffeine. Our study findings are particularly useful in settings with limited availability of caffeine injections as this study provides safety evidence on the early commencement of oral caffeine in preterm infants.
Bronchopulmonary dysplasia is a chronic respiratory disease among preterm infants resulting in significant morbidity and mortality [23]. In this study, we found that early caffeine therapy was associated with a significantly lower incidence of BPD. The risk reduction associated with the early caffeine therapy was in line with the Caffeine for Apnoea of Prematurity trial that reported a 37% reduction in BPD compared to a 13% reduction in the late caffeine therapy group [8]. The proposed mechanism of caffeine in reducing the risk of BPD is caffeine blocking the Adenosine 2 receptor that leads to inflammation and remodelling in the lung [14]. Early caffeine therapy initiation may enhance lung function, reduce inflammation and thus prevent the development of BPD in preterm infants [24].
In this study, we noticed antenatal steroid administration was significantly higher in preterm infants treated with early caffeine therapy compared to late caffeine therapy. The wide variability in antenatal steroids between the two study centres is in concordance with the National statistics. The Malaysian National Neonatal Registry reported that there were marked differences in the use of antenatal steroids across the hospitals, ranging from 36.4 to 100.0% [19]. However, the significant difference in antenatal steroid administration practices between the two centres might not have significantly affected our study outcomes, particularly on BPD, as the previous research [25] showed no significant reduction in BPD with antenatal steroid therapy (RR 0.86, 95% CI 0.42–1.79).
In contrast to the Caffeine for Apnoea of Prematurity trial, Taha et al. concluded that early caffeine therapy increased the risk of necrotising enterocolitis in preterm infants (OR 1.41, 95% CI 1.04–1.91, p-value = 0.027) [24]. However, our data indicated that the incidence of necrotising enterocolitis was similar in both treatment groups. Earlier studies [26, 27] showed that caffeine therapy was a risk factor for feeding intolerance. In contrast, our data demonstrated early caffeine therapy was associated with a shorter duration to achieve full enteral feeding. Preterm infants need to develop skills in sucking–swallowing–breathing coordination to facilitate full enteral feeding [28]. We noticed that early caffeine improved respiratory outcomes and reduced the duration of mechanical ventilation and subsequent, reduction in breathing instability improved sucking–swallowing–breathing coordination in preterm infants, resulting in the early caffeine group achieving full enteral feeding earlier than those in the late caffeine group.
The risk of osteopenia of prematurity was inversely proportional to gestational age and directly related to TPN therapy. A study reported fractures in 30% of premature neonates with osteopenia of prematurity [29]. Our study reported that early caffeine therapy was associated with lower osteopenia of prematurity risk. Furthermore, the osteopenia of prematurity risk was strongly associated with an increment in cumulative caffeine dose in line with earlier results [29].. In this study, we collected data retrospectively, without taking into account maternal caffeine intake during the breastfeeding period or during pregnancy. Furthermore, in this study, the early caffeine therapy group, caffeine was prescribed at 5 mg/kg, compared to 10 mg/kg in the late caffeine therapy group. Nonetheless, both practices were in line with dose recommendations, as the optimum lowest effective dose of caffeine has yet to be investigated.
A randomized control trial on the benefit of early caffeine in weaning of mechanical ventilation among premature infants born at a gestational age between 23 and 30 weeks found a non-significant increase in mortality with early caffeine initiation [30]. The finding concurred with our study results. However, the mean gestational age of 26 weeks and the mean birth weight of less than 750 g in Amaro et al.'s [30] study were lower than our studied population. We further investigated all mortality cases in our study population. The deaths were due to sepsis and other complications of prematurity. None of the causes of death was directly related to caffeine therapy. Another possible contributing reason to the higher mortality in the early caffeine group is survival bias. In this study, the median postnatal age of preterm infants initiated with caffeine therapy in the late caffeine group was on day 13 of life, compared to day 1 of life in the early caffeine group. Preterm infants often have a lower survival rate during the first 24 h of life. The World Health Organization (WHO) reported that 75% of neonatal deaths occur during the first 7 days of life. Thus, it is possible that preterm infants in the early caffeine group have a lower survival rate compared to the late caffeine group who start caffeine therapy after passing through the high mortality risk period during the first week of life.
Limitations
There were some limitations to the study owing to the retrospective study design and availability of data. Some relevant clinical data in patient monitoring (e.g. blood gas results) were not available in the hospital databases. This study did not include infants’ comorbidities. Patients’ clinical condition and concurrent drug therapy could be strong confounding factors affecting clinical outcomes, therefore the results need to be carefully interpreted.. Despite our attempts to match the two groups by gestational age, other baseline clinical characteristics were not matched statistically. The impact of baseline differences on study outcomes should be further investraged and a well-designed randomized controlled trial should be conducted to confirm the safety and effectiveness of early caffeine therapy among preterm infants with AOP. Furthermore, our study was never set out to identify optimal dose of oral caffeiene and future studies are required to investigate optimum caffeine duration and the lowest effective caffeine dose in the management of AOP. The long-term safety of caffeine therapy in preterm infants particularly on the growth and development should also be investigated.
Conclusion
Overall, our study found that early caffeine therapy improved respiratory outcomes, shortened the duration of hospital stay and reduced the time taken to achieve full enteral feeding without increasing gastrointestinal adverse events in preterm infants. Moreover, early caffeine therapy was associated with lower weight gain and increased mortality risk. However, given the study design limitations, no definitive conculsions can be drawn on the safety and efficacy of oral caffeine. We suggest providing individualized treatment by weighing the benefits against the risks in terms of the appropriate timing of caffeine therapy in preterm infants until further study confirms the safety profile of early commencement of oral caffeine therapy.
References
World Health Organization. Preterm birth. 2018. Available from: https://www.who.int/news-room/fact-sheets/detail/preterm-birth. Accessed 07 Aug 2019.
Henderson‐Smart DJ, Steer PA. Caffeine versus theophylline for apnea in preterm infants. Cochrane Database Syst Rev. 2000;(2):CD000273. doi: https://doi.org/10.1002/14651858.CD000273
Eichenwald EC, Watterberg KL, Aucott S, et al. Apnea of prematurity. Pediatrics. 2016;137(1).
Zhao J, Gonzalez F, Mu D. Apnea of prematurity: from cause to treatment. Eur J Pediatr. 2011;170(9):1097–105.
Martin R, Garcia-Prats JA, Mallory GB. Management of apnea of prematurity – UpToDate. 2018 Available from: https://www.uptodate.com/contents/management-of-apnea-of-prematurity/print. Accessed 14 Nov 2018.
Abdel-Hady H, Nasef N, Abd Elazeez Shabaan IN. Caffeine therapy in preterm infants. World J Clin Pediatr 2015;4(4):81.
Shrestha B, Jawa G. Caffeine citrate: Is it a silver bullet in neonatology? Pediatr Neonatol. 2017;58(5):391–7.
Davis PG, Schmidt B, Roberts RS, et al. Caffeine for Apnea of Prematurity trial: benefits may vary in subgroups. J Paediatr 2010;156(3):382–7.
Lim MS, Son MJ, Shin JE, et al. Clinical pharmacokinetics of caffeine in Korean preterm infants with apnea of prematurity. Neonatal Med. 2017;24(1):20–5.
Gao XB, Zheng Y, Yang F, et al. Developmental population pharmacokinetics of caffeine in Chinese premature infants with apnoea of prematurity: a post-marketing study to support paediatric labelling in China. Br J Clin Pharmacol. 2021;87(3):1155–64.
Kumral A, Tuzun F, Yesilirmak DC, et al. Genetic basis of apnoea of prematurity and caffeine treatment response: role of adenosine receptor polymorphisms: genetic basis of apnoea of prematurity. Acta Paediatr. 2012;101(7):e299–303.
He X, Qiu J-C, Lu K-Y, et al. Therapy for apnoea of prematurity: a retrospective study on effects of standard dose and genetic variability on clinical response to caffeine citrate in Chinese preterm infants. Adv Ther. 2021;38(1):607–26.
Ministry of Health. Malaysia: National obstetrics registry; 2016–2017. p. 9.
Park HW, Lim G, Chung S-H, et al. Early caffeine use in very low birth weight infants and neonatal outcomes: a systematic review and meta-analysis. J Korean Med Sci. 2015;30(12):1828–35.
Rubin A. Statistics for evidence-based practice and evaluation. Cengage Learning; 2012. p.107.
Kair LR, Leonard DT, Anderson JM. Bronchopulmonary dysplasia. Pediatr Rev. 2012;33(6):255–64.
Lodha A, Seshia M, McMillan DD, et al. Association of early caffeine administration and neonatal outcomes in very preterm neonates. JAMA Pediatr. 2015;169(1):33–8.
Costa ACDO, Schettino RDC, Ferreira SC. Predictors of extubation failure and reintubation in newborn infants subjected to mechanical ventilation. Rev Bras Ter Intensiva. 2014;26:51–6.
Ministry of Health. Malaysia: Malaysian National Neonatal Registry (NMRR); 2017.
Backström M, Kouri T, Kuusela AL, et al. Bone isoenzyme of serum alkaline phosphatase and serum inorganic phosphate in metabolic bone disease of prematurity. Acta Pediatr. 2000;89(7):867–73.
Abdallah EA, Said RN, Mosallam DS, et al. Serial serum alkaline phosphatase as an early biomarker for osteopenia of prematurity. Medicine. 2016;95(37).
Walsh MC, Trentham-Dietz A, Newcomb PA, et al. Using propensity scores to reduce case-control selection bias. Epidemiology (Cambridge, MA). 2012;23(5):772–3.
Eichenwald EC, Stark AR. Bronchopulmonary dysplasia: Definition, pathogenesis, and clinical features - UpToDate. 2019. https://www.uptodate.com/contents/bronchopulmonary-dysplasia-definition-pathogenesis-and-clinical-features#H1. Accessed 14 Nov 2019.
Taha D, Kirkby S, Nawab U, et al. Early caffeine therapy for prevention of bronchopulmonary dysplasia in preterm infants. J Matern Fetal Neonatal Med. 2014;27(16):1698–702.
Roberts D, Brown J, Medley N, et al. Antenatal corticosteroids for accelerating fetal lung maturation for women at risk of preterm birth. Cochrane Database Syst Rev.2017; 3(3):CD004454. doi: https://doi.org/10.1002/14651858.CD004454.pub3.
Gounaris AK, Grivea IN, Baltogianni M, et al. Caffeine and gastric emptying time in very preterm neonates. J Clin Med. 2020;9(6):1676.
Huang X, Chen Q, Peng W. Clinical characteristics and risk factors for feeding intolerance in preterm infants. Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2018;43(7):797–804. https://doi.org/10.11817/j.issn.1672-7347.2018.07.016.
Dodrill P. Feeding difficulties in preterm infants. ICAN: Infant, Child, & Adolescent Nutrition. 2011;3(6):324–31.
Ali E, Rockman-Greenberg C, Moffatt M, et al. Caffeine is a risk factor for osteopenia of prematurity in preterm infants: a cohort study. BMC Pediatr. 2018;18(1):1–7.
Amaro CM, Bello JA, Jain D, et al. Early caffeine and weaning from mechanical ventilation in preterm infants: a randomized, placebo-controlled trial. J Pediatr. 2018;196:52–7.
Acknowledgements
The authors would like to acknowledge the pediatricians and nurses at NICU for supporting this study. The authors would like to thank Director General, Ministry of Health, Malaysia for the permission to publish this paper.
Funding
Open Access funding provided by the Qatar National Library. No specific funding was received.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflicts of interest
The authors have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Yun, W.Z., Kassab, Y.W., Yao, L.M. et al. Effectiveness and safety of early versus late caffeine therapy in managing apnoea of prematurity among preterm infants: a retrospective cohort study. Int J Clin Pharm 44, 1140–1148 (2022). https://doi.org/10.1007/s11096-022-01437-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11096-022-01437-0