Abstract
Purpose
Enhancing the penetration ability of the antifungal drug natamycin, known to possess poor penetration ability through the corneal epithelium, by complexing with cell penetrating peptides.
Methods
The drug, natamycin was conjugated to a cell penetrating peptide, Tat-dimer (Tat2). The uptake ability of the conjugate in human corneal epithelial cells and its antifungal activity against filamentous fungi, F.solani has been elucidated.
Results
The cellular penetration ability of natamycin increased upon conjugation with Tat2. The conjugation between natamycin and Tat2 also lead to enhanced solubility of the drug in aqueous medium. The antifungal activity of the conjugate increased two- folds in comparison to unconjugated natamycin against clinical isolates of F.solani.
Conclusion
The formation of CPP-natamycin complex is clinically significant as it may enhance the bioavailability of natamycin in corneal tissues and aid in efficient management of fungal keratitis.









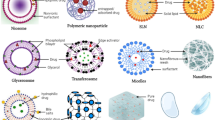
Similar content being viewed by others
Abbreviations
- CPP:
-
Cell penetrating peptide
- FDA:
-
Food and drug administration
- FITC:
-
Fluorescein isothiocyanate
- IV:
-
Intravenous
- MIC:
-
Minimum inhibitory concentration
References
Thomas PA. Fungal infections of the cornea. Eye. 2003;17(8):852–62.
Thomas PA, Kaliamurthy J. Mycotic Keratitis: epidemiology, diagnosis and management. Clin Microbiol Infect. 2013;19(3):210–20.
Al-Badriyeh D, Neoh CF, Stewart K, Kong DC. Clinical utility of voriconazole eye drops in ophthalmic fungal keratitis. Clin Ophthalmol. 2010;4:391–405.
Leck AK, Thomas PA, Hagan M, Kaliamurthy J, Ackuaku E, John M, et al. Aetiology of suppurative corneal ulcers in Ghana and south India, and epidemiology of fungal keratitis. Br J Ophthalmol. 2002;86(11):1211–5.
Gopinathan U, Garg P, Fernandes M, Sharma S, Athmanathan S, Rao GN. The epidemiological features and laboratory results of fungal keratitis: a 10-year review at a referral eye care center in South India. Cornea. 2002;21(6):555–9.
Gopinathan U, Sharma S, Garg P, Rao GN. Review of epidemiological features, microbiological diagnosis and treatment outcome of microbial keratitis: experience of over a decade. Indian J Ophthalmol. 2009;57(4):273–9.
Whitcher JP, Srinivasan M, Upadhyay P. Corneal blindness: a global perspective. Bull World Health Organ. 2001;79(3):214–21.
Lalitha P, Sun CQ, Prajna NV, Karpagam R, Geetha M, O’Brien KS, et al. In vitro susceptibility of filamentous fungal isolates from a corneal ulcer clinical trial. Am J Ophthalmol. 2014;157(2):318–26.
Burton MJ, Pithuwa J, Okello E, Afwamba I, Onyango JJ, Oates F, et al. Microbial Keratitis in East Africa: why are the outcomes so poor? Ophthalmic Epidemiol. 2011;18(4):158–63.
Keay LJ, Gower EW, Lovieno A, Oechsler RA, Alfonso EC, Matoba A, et al. Clinical and microbiological characteristics of Fungal Keratitis in the United States, 2001-2007: A Multicenter Study. Ophthalmology. 2011;118(5):920–6.
Phan CM, Subbaraman LN, Jones L. In vitro uptake and release of natamycin from conventional and silicone hydrogel contact lens materials. Eye Contact Lens. 2013;39(2):162–8.
Ciolino JB, Hudson SP, Mobbs AN, Hoare TR, Iwata NG, Fink GR, et al. A prototype antifungal contact lens. Invest Ophthalmol Vis Sci. 2011;52(9):6286–91.
Loh AR, Hong K, Lee S, Mannis M, Acharya NR. Practice patterns in the management of fungal corneal ulcers. Cornea. 2009;28(8):856–9.
O’day DM, Ray WA, Head WS, Robinson RD. Influence of the corneal epithelium on the efficacy of topical antifungal agents. Invest Ophthalmol Vis Sci. 1984;25(7):855–9.
O’day DM, Head WS, Robinson RD, Clanton JA. Corneal penetration of topical amphotericin B and natamycin. Curr Eye Res. 1986;5(11):877–82.
Waltman SR, Kaufman HE. Use of hydrophilic contact lenses to increase ocular penetration of topical drugs. Invest Ophthalmol Vis Sci. 1970;9(4):250–5.
Xie L, Zhong W, Shi W, Sun S. Spectrum of fungal keratitis in north China. Ophthalmology. 2006;113(11):1943–8.
Phan CM, Subbaraman L, Liu S, Gu F, Jones L. In vitro uptake and release of natamycin Dex-b-PLA nanoparticles from model contact lens materials. J Biomater Sci Polym Ed. 2014;25(1):18–31.
Panyam J, Labhasetwar V. Dynamics of endocytosis and exocytosis of poly(D, L-lactide-co-glycolide) nanoparticles in vascular smooth muscle cells. Pharm Res. 2003;20(2):212–20.
Vasir JK, Labhasetwar V. Quantification of the force of nanoparticle-cell membrane interactions and its influence on intracellular trafficking of nanoparticles. Biomaterials. 2008;29(31):4244–52.
Desai P, Patlolla RR, Singh M. Interaction of nanoparticles and cell penetrating peptides with skin for transdermal drug delivery. Mol Membr Biol. 2010;27(7):247–59.
Trabulo S, Cardoso AL, Mano M, De Lima Pedroso MC. Cell-penetrating peptides—mechanisms of cellular uptake and generation of delivery systems. Pharmaceuticals. 2010;3:961–93.
Gupta B, Levchenko TS, Torchilin VP. Intracellular delivery of large molecules and small particles by cell-penetrating proteins and peptides. Adv Drug Deliv Rev. 2005;57(4):637–51.
Simeoni F, Morris MC, Heitz F, Divita G. Insight into the mechanism of the peptide-based gene delivery system MPG: implications for delivery of siRNA into mammalian cells. Nucleic Acids Res. 2003;31(11):2717–24.
Aroui S, Brahim S, Waard MD, Kenani A. Cytotoxicity, intracellular distribution and uptake of doxorubicin and doxorubicin coupled to cell-penetrating peptides in different cell lines: a comparative study. Biochem Biophys Res Commun. 2010;391(1):419–25.
Ruan G, Agrawal A, Marcus AI, Nie S. Imaging and tracking of tat peptide-conjugated quantum dots in living cells: new insights into nanoparticle uptake, intracellular transport, and vesicle shedding. J Am Chem Soc. 2007;129(47):14759–66.
Liu L, Guo K, Lu J, Venkatraman SS, Luo D, Ng KC, et al. Biologically active core/shell nanoparticles self-assembled from cholesterol-terminated PEG–TAT for drug delivery across the blood–brain barrier. Biomaterials. 2008;29(10):1509–17.
Cohen-Avrahami M, Shames A, Ottaviani MF, Aserin A, Garti N. HIV-Tat enhances the transdermal delivery of NSAID drugs from liquid crystalline mesophases. J Phys Chem B. 2014;118(23):6277–87.
Ookubo N, Michiue H, Kitamatsu M, Kamamura M, Nishiki T, Ohmori I, et al. The transdermal inhibition of melanogenesis by a cell-permeable peptide delivery system based on poly-arginine. Biomaterials. 2014;35(15):4508–16.
Wang Y, Su W, Li Q, Li C, Wang H, Li Y, et al. Preparation and evaluation of lidocaine hydrochloride loaded TAT-conjugated polymeric liposomes for transdermal delivery. Int J Pharm. 2013;441(1–2):748–56.
Manosroi J, Khositsuntiwong N, Manosroi W, Gotz F, Werner RG, Manosroi A. Potent enhancement of transdermal absorption and stability of human tyrosinase plasmid (pAH7/Tyr) by Tat peptide and an entrapment in elastic cationic niosomes. Drug Deliv. 2013;20(1):10–8.
Clinical and Laboratory Standards Institute, Reference method for broth dilution antifungal susceptibility testing of filamentous fungi. Approved standard CLSI document M38-A2, Clinical and Laboratory Standards Institute, Wayne, PA (2008)
Badhani A, Dabral P, Rana V, Upadhyaya K. Evaluation of cyclodextrins for enhancing corneal penetration of natamycin eye drops. J Pharm Bioallied Sci. 2012;4 Suppl 1:S29–30.
Salvosa FAM, Cubillan LP. In vitro evaluation of natamycin 5% suspension against Aspergillus flavus, Fusarium solani, and Candida parasilopsis. Ophthalmology. 2004;29(1):26–8.
Chugh A, Eudes F. Translocation and nuclear accumulation of monomer and dimer of HIV-1 Tat basic domain in triticale mesophyll protoplasts. Biochim Biophys Acta. 2007;1768(3):419–26.
Kanduser M, Sentjurc M, Miklavcic D. The temperature effect during pulse application on cell membrane fluidity and permeabilization. Bioelectrochemistry. 2008;74(1):52–7.
Zhu WL, Shin SY. Effects of dimerization of the cell penetrating peptide Tat analog on antimicrobial activity and mechanism of bactericidal action. J Pept Sci. 2009;15(5):345–52.
Jung HJ, Park Y, Hahm KS, Lee DG. Biological activity of Tat (47–58) peptide on human pathogenic fungi. Biochem Biophys Res Commun. 2006;345(1):222–8.
Acknowledgments and Disclosures
The authors are thankful to the Department of Biotechnology, Government of India and Kusuma Trust, UK for funding the project and procurement of BD FACS Aria III, respectively. The authors are also thankful to Professor Harpal Singh, Centre for Biomedical Engineering and Professor Aditya Mittal, Kusuma School of Biological Sciences, at Indian Institute of Technology Delhi, India for providing the facility of confocal microscopy and epifluorescence microscopy, respectively. Aastha Jain is thankful to Council for Scientific and Industrial Research, Government of India for the award of Junior and Senior Research Fellowship. The authors would also like to thank Bausch & Lomb, USA and Sight Life, for providing Optisol GS medium.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jain, A., Shah, S.G. & Chugh, A. Cell Penetrating Peptides as Efficient Nanocarriers for Delivery of Antifungal Compound, Natamycin for the Treatment of Fungal Keratitis. Pharm Res 32, 1920–1930 (2015). https://doi.org/10.1007/s11095-014-1586-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-014-1586-x