ABSTRACT
Purpose
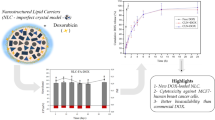
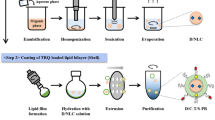
To develop a nanostructured lipid carrier (NLC) co-loaded with doxorubicin and docosahexaenoic acid (DHA) and to evaluate its potential to overcome drug resistance and to increase antitumoral effect in MCF-7/Adr cancer cell line.
Methods
The NLC was prepared by a hot homogenization method and characterized for size, zeta potential, entrapment efficiency (EE) and drug loading (DL). Drug release was evaluated by dialysis in complete DMEM, and NLC aggregation was assayed in the presence of serum. The cytotoxicity of formulations, doxorubicin uptake or penetration were evaluated in MCF-7 and MCF-7/Adr as monolayer or spheroid models.
Results
The formulation had a size of about 80 nm, negative zeta potential, EE of 99%, DL of 31 mg/g, a controlled drug release in DMEM and no particles aggregation in presence of serum. The NLC loaded with doxorubicin and DHA showed the same activity as free drugs against MCF-7 but a stronger activity against MCF-7/Adr cells. In monolayer model, the doxorubicin uptake as free and encapsulated form was similar in MCF-7 but higher for the encapsulated drug in MCF-7/Adr, suggesting a bypassing of P-glycoprotein bomb efflux. For spheroids, the NLC loaded with doxorubicin and DHA showed a prominent cytotoxicity and a greater penetration of doxorubicin.
Conclusions
These findings suggest that the co-encapsulation of doxorubicin and DHA in NLC enhances the cytotoxicity and overcomes the doxorubicin resistance in MCF-7/Adr.

ᅟ






Similar content being viewed by others
Abbreviations
- DDS:
-
Drug delivery system
- DHA:
-
Docosahexaenoic acid
- DL:
-
Drug loading
- DOX:
-
Doxorubicin
- EE:
-
Entrapment efficiency
- EPR:
-
Enhanced permeability and retention
- NE:
-
Nanoemulsion
- NLC:
-
Nanostructured lipid carrier
- PO:
-
Peanut oil
- SLN:
-
Solid lipid nanoparticles
- TEA:
-
Triethanolamine
REFERENCES
Livi L, Meattini I, Cardillo Cde L, Mangoni M, Greto D, Petrucci A, et al. Non-pegylated liposomal doxorubicin in combination with cyclophosphamide or docetaxel as first-line therapy inmetastatic breast cancer: a retrospective analysis. Tumori. 2009;95(4):422–6.
Shi Y, Moon M, Dawood S, McManus B, Liu PP. Mechanisms and management of doxorubicin cardiotoxicity. Herz. 2011;36(4):296–305.
Primeau AJ, Rendon A, Hedley D, Lilge L, Tannock IF. The distribution of the anticancer drug doxorubicin in relation to blood vessels in solid tumors. Clin Cancer Res. 2005;11(24 Pt 1):8782–8.
Trédan O, Galmarini CM, Patel K, Tannock IF. Drug resistance and the solid tumor microenvironment. J Natl Cancer Inst. 2007;99(19):1441–54.
Jassem J, Pieńkowski T, Płuzańska A, Jelic S, Gorbunova V, Mrsic-Krmpotic Z, et al. Doxorubicin and paclitaxel versus fluorouracil, doxorubicin, and cyclophosphamide as first-line therapy for women with metastatic breast cancer: final results of a randomized phase III multicenter trial. J Clin Oncol. 2001;19(6):1707–15.
Germain E, Chajès V, Cognault S, Lhuillery C, Bougnoux P. Enhancement of doxorubicin cytotoxicity by polyunsaturated fatty acids in the human breast tumor cell line MDA-MB-231: relationship to lipid peroxidation. Int J Cancer. 1998;75(4):578–83.
Colas S, Mahéo K, Denis F, Goupille C, Hoinard C, Champeroux P, et al. Sensitization by dietary docosahexaenoic acid of rat mammary carcinoma to anthracycline: a role for tumor vascularization. Clin Cancer Res. 2006;12(19):5879–86.
Siddiqui RA, Harvey KA, Xu Z, Bammerlin EM, Walker C, Altenburg JD. Docosahexaenoic acid: a natural powerful adjuvant that improves efficacy for anticancer treatment with no adverse effects. Biofactors. 2011;37(6):399–412.
Mahéo K, Vibet S, Steghens JP, Dartigeas C, Lehman M, Bougnoux P, et al. Differential sensitization of cancer cells to doxorubicin by DHA: a role for lipoperoxidation. Free Radic Biol Med. 2005;39(6):742–51.
Hardman WE, Avula CP, Fernandes G, Cameron IL. Three percent dietary fish oil concentrate increased efficacy of doxorubicin against MDA-MB 231 breast cancer xenografts. Clin Cancer Res. 2001;7(7):2041–9.
Hajjaji N, Besson P, Bougnoux P. Tumor and non-tumor tissues differential oxidative stress response to supplemental DHA and chemotherapy in rats. Cancer Chemother Pharmacol. 2012;70(1):17–23.
Bougnoux P, Hajjaji N, Ferrasson MN, Giraudeau B, Couet C, Le Floch O. Improving outcome of chemotherapy of metastatic breast cancer by docosahexaenoic acid: a phase II trial. Br J Cancer. 2009;101(12):78–85.
Parhi P, Mohanty C, Sahoo SK. Nanotechnology-based combinational drug delivery: an emerging approach for cancer therapy. Drug Discov Today. 2012;17(17–18):1044–52.
Okuda T, Kidoaki S. Multidrug delivery systems with single formulation—current status and future perspective. J Biomater Nanobiotechnol. 2012;3(1):50–60.
Maeda H, Wu J, Sawa T, Matsumura Y, Hori K. Tumor vascular permeability and the EPR effect in macromolecular therapeutics: a review. J Control Release. 2000;65(1–2):271–84.
Torchilin V. Tumor delivery of macromolecular drugs based on the EPR effect. Adv Drug Deliv Rev. 2011;63(3):131–5.
Li Y, Wang J, Wientjes MG, Au JL. Delivery of nanomedicines to extracellular and intracellular compartments of a solid tumor. Adv Drug Deliv Rev. 2012;64(1):29–39.
Mehnert W, Mäder K. Solid lipid nanoparticles: production, characterization and applications. Adv Drug Deliv Rev. 2001;47(2–3):165–96.
Müller RH, Radtke M, Wissing SA. Nanostructured lipid matrices for improved microencapsulation of drugs. Int J Pharm. 2002;242(1–2):121–8.
Wissing SA, Kayser O, Müller RH. Solid lipid nanoparticles for parenteral drug delivery. Adv Drug Deliv Rev. 2004;56(9):1257–72.
Radtke M, Müller RH. NLC-nanostructured lipid carriers: the new generation of lipid drug carriers. New Drugs. 2001;2:48–52.
Serpe L, Satalano MG, Cavalli R, Ugazio E, Bosco O, Canaparo R, et al. Cytotoxicity of anticancer drugs incorporated in solid lipid nanoparticles on HT-29 colorectal cancer cell line. Eur J Pharm Biopharm. 2004;58(3):673–80.
Wong HL, Rauth AM, Bendayan R, Manias JL, Ramaswamy M, Liu Z, et al. A new polymer-lipid hybrid nanoparticle system increases cytotoxicity of doxorubicin against multidrug-resistant human breast cancer cells. Pharm Res. 2006;23(7):1574–85.
Mussi SV, Silva RC, Oliveira MC, Lucci CM, Azevedo RB, Ferreira LA. New approach to improve encapsulation and antitumor activity of doxorubicin loaded in solid lipid nanoparticles. Eur J Pharm Sci. 2013;48(1–2):282–90.
Elbayoumi T, Torchilin VP. Tumor-targeted immuno-liposomes for cancer therapy and imaging. J Pharm Innov. 2008;3:51–8.
Perche F, Patel NR, Torchilin VP. Accumulation and toxicity of antibody-targeted doxorubicin-loaded PEG-PE micelles in ovarian cancer cell spheroid model. J Control Release. 2012;164(1):95–102.
Flaherty KT, Infante JR, Daud A, Gonzalez R, Kefford RF, Sosman J, et al. Combined BRAF and MEK inhibition in melanoma with BRAF V600 mutations. N Engl J Med. 2012;367(18):1694–703.
Joshi MD, Müller RH. Lipid nanoparticles for parenteral delivery of actives. Eur J Pharm Biopharm. 2009;71(2):161–72.
Zhang X-g, Miao J, Dai Y-Q, Du Y-Z, Yuan H, Hu F-Q. Reversal activity of nanostructured lipid carriers loading cytotoxic drug in multi-drug resistant cancer cells. Int J Pharm. 2008;361(1–2):239–44.
Yang XY, Li YX, Li M, Zhang L, Feng LX, Zhang N. Hyaluronic acid-coated nanostructured lipid carriers for targeting paclitaxel to cancer. Cancer Lett. 2013;334(2):338–45.
Bunjes H. Lipid nanoparticles for the delivery of poorly water-soluble drugs. J Pharm Pharmacol. 2010;62(11):1637–45.
Rosenblatt KM, Douroumis D, Bunjes H. Drug release from differently structured monoolein/poloxamer nanodispersions studied with differential pulse polarography and ultrafiltration at low pressure. J Pharm Sci. 2007;96(6):1564–75.
Souto EB, Müller RH. Lipid nanoparticles: effect on bioavailability and pharmacokinetic changes. Handb Exp Pharmacol. 2010;197:115–41.
Subedi RK, Kang KW, Choi H. Preparation and characterization of solid lipid nanoparticles loaded with doxorubicin. Eur J Pharm Sci. 2009;37(3–4):508–13.
Needham D, Ponce A. Nanoscale drug delivery vehicles for solid tumors: a new paradigm for localized drug delivery using temperature sensitive liposomes. In: Amiji MM, editor. Nanotechnology for cancer therapy. Boca Raton: CRC Press, LLC (a subsidiary of Taylor and Francis); 2007. p. 677–719.
Miao J, Du YZ, Yuan H, Zhang XG, Hu FQ. Drug resistance reversal activity of anticancer drug loaded solid lipid nanoparticles in multi-drug resistant cancer cells. Colloids Surf B: Biointerfaces. 2013;110:74–80.
Hirschhaeuser F, Menne H, Dittfeld C, West J, Mueller-Klieser W, Kunz-Schughart LA. Multicellular tumor spheroids: an underestimated tool is catching up again. J Biotechnol. 2010;148(1):3–15.
Perche F, Torchilin VP. Cancer cell spheroids as a model to evaluate chemotherapy protocols. Cancer Biol Ther. 2012;13(12):1205–13.
Dufau I, Frongia C, Sicard F, Dedieu L, Cordelier P, Ausseil F, et al. Multicellular tumor spheroid model to evaluate spatio-temporal dynamics effect of chemotherapeutics: application to the gemcitabine/CHK1 inhibitor combination in pancreatic cancer. BMC Cancer. 2012;12(15):1–11.
Kim TH, Mount CW, Gombotz WR, Pun SH. The delivery of doxorubicin to 3-D multicellular spheroids and tumors in a murine xenograft model using tumor-penetrating triblock polymeric micelles. Biomaterials. 2010;31(28):7386–97.
ACKNOWLEDGMENTS AND DISCLOSURES
This study was supported by “Minas Gerais State Agency for Research and Development” (FAPEMIG, Brazil) and by the Brazilian agencies. The authors wish to kindly thank Dr. William Hartner for his helpful advice in editing this manuscript. The authors state no conflict of interest and have received no payment in preparation of this manuscript. All authors have approved the final article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mussi, S.V., Sawant, R., Perche, F. et al. Novel Nanostructured Lipid Carrier Co-Loaded with Doxorubicin and Docosahexaenoic Acid Demonstrates Enhanced in Vitro Activity and Overcomes Drug Resistance in MCF-7/Adr Cells. Pharm Res 31, 1882–1892 (2014). https://doi.org/10.1007/s11095-013-1290-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-013-1290-2