Abstract
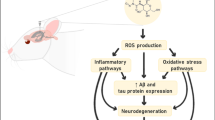
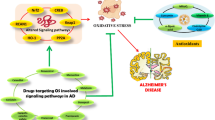
Parkinson’s disease (PD) is the second most common neurodegenerative disorder. Progressive loss of dopaminergic neurons in the substantia nigra (SN) is one of the major pathological changes. However, the reasons for the dopaminergic neuron loss are still ambiguous and further studies are needed to evaluate the in-depth mechanisms of neuron death. Oxidative stress is a significant factor causing neuronal damage. Dopaminergic neurons in the SN are susceptible to oxidative stress, which is closely associated with iron dyshomeostasis in the brain. Ginsenoside Rg1 from ginseng plays a crucial role in neuroprotective effects through anti-inflammation and attenuating the aggregation of abnormal α-synuclein. In our study, we established a chronic PD mouse model by 1-methyl-4-phenyl-1, 2, 3, 6-tetrahydropyridine combined with probenecid and explored the effect of Rg1 on the oxidative stress and brain iron homeostasis. Rg1 was verified to improve the level of tyrosine hydroxylase and anti-oxidant stress. In addition, Rg1 maintained the iron-regulated protein homeostasis by increasing the expression of ferritin heavy chain and decreasing ferritin light chain in oligodendrocytes, especially the mature oligodendrocytes (OLs). Furthermore, Rg1 had a positive effect on the myelin sheath protection and increased the number of mature oligodendrocytes, proved by the increased staining of myelin basic protein and CC-1. In conclusion, Rg1 could play a neuroprotective role through remitting the iron-regulated protein dyshomeostasis by ferritin and against lipid peroxidation stress in oligodendrocytes.









Similar content being viewed by others
Data Availability
Enquiries about data availability should be directed to the authors.
Abbreviations
- BBB:
-
Blood–brain barrier
- BCA:
-
Bicinchoninic acid
- BSA:
-
Bovine serum albumin
- CNS:
-
Central nervous system
- DA:
-
Dopamine
- DAB:
-
3,3′-Diamino-benzidine
- DHE:
-
Dihydroethidium
- ECL:
-
Chemiluminescence
- ELISA:
-
Enzyme-linked immunosorbent assay
- FTH:
-
Ferritin heavy chain
- FTL:
-
Ferritin light chain
- IHC:
-
Immunohistochemistry
- IF:
-
Immunofluorescence
- LBs:
-
Lowy bodies
- MAO-B:
-
Monoamine oxidase B
- MBP:
-
Myelin basic protein
- MPP+ :
-
1-Methyl-4-phenylpyridinium
- MRI:
-
Magnetic resonance imaging
- aOPCs:
-
Adult oligodendrocyte precursor cells
- OS:
-
Oxidative stress
- PBS:
-
Phosphate buffer saline
- PD:
-
Parkinson’s disease
- PVDF:
-
Polyvinylidene difluoride
- PFA:
-
Paraformaldehyde
- ROS:
-
Reactive oxygen species
- SNpc:
-
Substantia nigra pars compacta
- SPNs:
-
Spiny projection neurons
- TEM:
-
Transmission electron microscopy
- 4-HNE:
-
4-Hydroxynonenal
References
Michel PP, Hirsch EC, Hunot S (2016) Understanding dopaminergic cell death pathways in Parkinson disease. Neuron 90:675–691
Emamzadeh FN, Surguchov A (2018) Parkinson’s disease: biomarkers treatment, and risk factors. Front Neurosci 12:612
Surmeier DJ, Obeso JA, Halliday GM (2017) Selective neuronal vulnerability in Parkinson disease. Nat Rev Neurosci 18:101–113
Braak H, Del Tredici K, Rub U, de Vos RA, Jansen Steur EN, Braak E (2003) Staging of brain pathology related to sporadic Parkinson’s disease. Neurobiol Aging 24:197–211
Aitken RJ, Bennetts L, De Jonge CJ, Barratt C (2006) Reactive oxygen species: friend or foe, The Sperm Cell, pp 170–193
McGeer PL, McGeer EG (2004) Inflammation and neurodegeneration in Parkinson’s disease. Parkinsonism Relat Disord 10:S3–S7
Jiang H, Wang J, Rogers J, Xie J (2017) Brain iron metabolism dysfunction in Parkinson’s disease. Mol Neurobiol 54:3078–3101
Sofic E, Paulus W, Jellinger K, Riederer P, Youdim MB (1991) Selective increase of iron in substantia nigra zona compacta of parkinsonian brains. J Neurochem 56:978–982
Drayer BP, Olanow W, Burger P, Johnson GA, Herfkens R, Riederer S (1986) Parkinson plus syndrome: diagnosis using high field MR imaging of brain iron. Radiology 159:493–498
Ryvlin P, Broussolle E, Piollet H, Viallet F, Khalfallah Y, Chazot G (1995) Magnetic resonance imaging evidence of decreased putamenal iron content in idiopathic Parkinson’s disease. Arch Neurol 52:583–588
Good PF, Olanow CW, Perl DP (1992) Neuromelanin-containing neurons of the substantia nigra accumulate iron and aluminum in Parkinson’s disease: a LAMMA study. Brain Res 593:343–346
Oakley AE, Collingwood JF, Dobson J, Love G, Perrott HR, Edwardson JA, Elstner M, Morris CM (2007) Individual dopaminergic neurons show raised iron levels in Parkinson disease. Neurology 68:1820–1825
Kaur D, Andersen J (2004) Does cellular iron dysregulation play a causative role in Parkinson’s disease? Ageing Res Rev 3:327–343
Jiang H, Song N, Xu H, Zhang S, Wang J, Xie J (2010) Up-regulation of divalent metal transporter 1 in 6-hydroxydopamine intoxication is IRE/IRP dependent. Cell Res 20:345–356
Ward RJ, Zucca FA, Duyn JH, Crichton RR, Zecca L (2014) The role of iron in brain ageing and neurodegenerative disorders. Lancet Neurol 13:1045–1060
Ayton S, Lei P (2014) Nigral iron elevation is an invariable feature of Parkinson’s disease and is a sufficient cause of neurodegeneration. BioMed Res Int 2014:581256
Tang D, Chen X, Kang R, Kroemer G (2021) Ferroptosis: molecular mechanisms and health implications. Cell Res 31:107–125
Hirschhorn T, Stockwell BR (2019) The development of the concept of ferroptosis. Free Radic Biol Med 133:130–143
Gaschler MM, Stockwell BR (2017) Lipid peroxidation in cell death. Biochem Biophys Res Commun 482:419–425
Wang H, Liu C, Zhao Y, Gao G (2020) Mitochondria regulation in ferroptosis. Eur J Cell Biol 99:151058
Zecca L, Stroppolo A, Gatti A, Tampellini D, Toscani M, Gallorini M, Giaveri G, Arosio P, Santambrogio P, Fariello RG, Karatekin E, Kleinman MH, Turro N, Hornykiewicz O, Zucca FA (2004) The role of iron and copper molecules in the neuronal vulnerability of locus coeruleus and substantia nigra during aging. Proc Natl Acad Sci USA 101:9843–9848
Radad K, Gille G, Moldzio R, Saito H, Rausch WD (2004) Ginsenosides Rb1 and Rg1 effects on mesencephalic dopaminergic cells stressed with glutamate. Brain Res 1021:41–53
Chen XC, Fang F, Zhu YG, Chen LM, Zhou YC, Chen Y (2003) Protective effect of ginsenoside Rg1 on MPP+-induced apoptosis in SHSY5Y cells. J Neural Transm 110:835–845
Jiang W, Wang Z, Jiang Y, Lu M, Li X (2015) Ginsenoside Rg1 ameliorates motor function in an animal model of Parkinson’s disease. Pharmacology 96:25–31
Chu SF, Zhang Z, Zhou X, He WB, Chen C, Luo P, Liu DD, Ai QD, Gong HF, Wang ZZ, Sun HS, Feng ZP, Chen NH (2019) Ginsenoside Rg1 protects against ischemic/reperfusion-induced neuronal injury through miR-144/Nrf2/ARE pathway. Acta Pharmacol Sin 40:13–25
Mou Z, Huang Q, Chu SF, Zhang MJ, Hu JF, Chen NH, Zhang JT (2017) Antidepressive effects of ginsenoside Rg1 via regulation of HPA and HPG axis. Biomed Pharmacother 92:962–971
Surguchov A, Bernal L, Surguchev AA (2021) Phytochemicals as regulators of genes involved in synucleinopathies. Biomolecules 11:624
Heng Y, Zhang QS, Mu Z, Hu JF, Yuan YH, Chen NH (2016) Ginsenoside Rg1 attenuates motor impairment and neuroinflammation in the MPTP-probenecid-induced parkinsonism mouse model by targeting alpha-synuclein abnormalities in the substantia nigra. Toxicol Lett 243:7–21
Zhou T, Zu G, Zhang X, Wang X, Li S, Gong X, Liang Z, Zhao J (2016) Neuroprotective effects of ginsenoside Rg1 through the Wnt/beta-catenin signaling pathway in both in vivo and in vitro models of Parkinson’s disease. Neuropharmacology 101:480–489
Matsuura K, Kabuto H, Makino H, Ogawa N (1997) Pole test is a useful method for evaluating the mouse movement disorder caused by striatal dopamine depletion. J Neurosci Methods 73:45–48
Ogawa N, Hirose Y, Ohara S, Ono T, Watanabe Y (1985) A simple quantitative bradykinesia test in MPTP-treated mice. Res Commun Chem Pathol Pharmacol 50:435–441
Yang Y, Guan D, Lei L, Lu J, Liu JQ, Yang G, Yan C, Zhai R, Tian J, Bi Y, Fu F, Wang H (2018) H6, a novel hederagenin derivative, reverses multidrug resistance in vitro and in vivo. Toxicol Appl Pharmacol 341:98–105
Langston JW, Ballard P, Tetrud JW, Irwin I (1983) Chronic Parkinsonism in humans due to a product of meperidine-analog synthesis. Science 219:979–980
Bove J, Perier C (2012) Neurotoxin-based models of Parkinson’s disease. Neuroscience 211:51–76
Petroske E, Meredith GE, Callen S, Totterdell S, Lau YS (2001) Mouse model of Parkinsonism: a comparison between subacute MPTP and chronic MPTP/probenecid treatment. Neuroscience 106:589–601
Schapira AHV, Chaudhuri KR, Jenner P (2017) Non-motor features of Parkinson disease. Nat Rev Neurosci 18:509
Howard CD, Li H, Geddes CE, Jin X (2017) Dynamic nigrostriatal dopamine biases action selection. Neuron 93:1436–1450
Yager LM, Garcia AF, Wunsch AM, Ferguson SM (2015) The ins and outs of the striatum: role in drug addiction. Neuroscience 301:529–541
Zhai S, Tanimura A, Graves SM, Shen W, Surmeier DJ (2018) Striatal synapses, circuits, and Parkinson’s disease. Curr Opin Neurobiol 48:9–16
Gerfen CR, Surmeier DJ (2011) Modulation of striatal projection systems by dopamine. Annu Rev Neurosci 34:441–466
Kravitz AV, Freeze BS, Parker PR, Kay K, Thwin MT, Deisseroth K, Kreitzer AC (2010) Regulation of parkinsonian motor behaviours by optogenetic control of basal ganglia circuitry. Nature 466:622–626
Mallet N, Ballion B, Le Moine C, Gonon F (2006) Cortical inputs and GABA interneurons imbalance projection neurons in the striatum of parkinsonian rats. J Neurosci 26:3875–3884
Brieger K, Schiavone S, Miller FJ Jr, Krause KH (2012) Reactive oxygen species: from health to disease. Swiss Medl Wkly 142:w13659
Lee DH, Gold R, Linker RA (2012) Mechanisms of oxidative damage in multiple sclerosis and neurodegenerative diseases: therapeutic modulation via fumaric acid esters. Int J Mol Sci 13:11783–11803
Shukla V, Mishra SK, Pant HC (2011) Oxidative stress in neurodegeneration. Adv Pharmacol Sci 2011:572634
Ho PW, Ho JW, Liu HF, So DH, Tse ZH, Chan KH, Ramsden DB, Ho SL (2012) Mitochondrial neuronal uncoupling proteins: a target for potential disease-modification in Parkinson’s disease. Transl Neurodegen 1:3
Zucca FA, Segura-Aguilar J, Ferrari E, Munoz P, Paris I, Sulzer D, Sarna T, Casella L, Zecca L (2017) Interactions of iron, dopamine and neuromelanin pathways in brain aging and Parkinson’s disease. Prog Neurobiol 155:96–119
Costa-Mallen P, Gatenby C, Friend S, Maravilla KR, Hu SC, Cain KC, Agarwal P, Anzai Y (2017) Brain iron concentrations in regions of interest and relation with serum iron levels in Parkinson disease. J Neurol Sci 378:38–44
Madenci G, Bilen S, Arli B, Saka M, Ak F (2012) Serum iron, vitamin B12 and folic acid levels in Parkinson’s disease. Neurochem Res 37:1436–1441
Crichton R, Ward R (2006) From molecular mechanisms to therapeutic strategies, 2nd edn
Perluigi M, Coccia R, Butterfield DA (2012) 4-Hydroxy-2-nonenal, a reactive product of lipid peroxidation, and neurodegenerative diseases: a toxic combination illuminated by redox proteomics studies. Antioxid Redox Signal 17:1590–1609
Mena NP, Urrutia PJ, Lourido F, Carrasco CM, Nunez MT (2015) Mitochondrial iron homeostasis and its dysfunctions in neurodegenerative disorders. Mitochondrion 21:92–105
Horowitz MP, Greenamyre JT (2010) Mitochondrial iron metabolism and its role in neurodegeneration. J Alzheimer’s Dis 20(Suppl 2):S551-568
Salazar J, Mena N, Hunot S, Prigent A, Alvarez-Fischer D, Arredondo M, Duyckaerts C, Sazdovitch V, Zhao L, Garrick LM, Nunez MT, Garrick MD, Raisman-Vozari R, Hirsch EC (2008) Divalent metal transporter 1 (DMT1) contributes to neurodegeneration in animal models of Parkinson’s disease. Proc Natl Acad Sci USA 105:18578–18583
Groger A, Berg D (2012) Does structural neuroimaging reveal a disturbance of iron metabolism in Parkinson’s disease? Implications from MRI and TCS studies. J Neural Transm 119:1523–1528
Connor JR, Menzies SL, St Martin SM, Mufson EJ (1990) Cellular distribution of transferrin, ferritin, and iron in normal and aged human brains. J Neurosci Res 27:595–611
Todorich B, Pasquini JM, Garcia CI, Paez PM, Connor JR (2009) Oligodendrocytes and myelination: the role of iron. Glia 57:467–478
Pinero DJ, Li NQ, Connor JR, Beard JL (2000) Variations in dietary iron alter brain iron metabolism in developing rats. J Nutr 130:254–263
Rosato-Siri MV, Marziali L, Guitart ME, Badaracco ME, Puntel M, Pitossi F, Correale J, Pasquini JM (2018) Iron availability compromises not only oligodendrocytes but also astrocytes and microglial cells. Mol Neurobiol 55:1068–1081
Franklin RJM, Ffrench-Constant C (2017) Regenerating CNS myelin—from mechanisms to experimental medicines. Nat Rev Neurosci 18:753–769
Xue W, Liu Y, Qi WY, Gao Y, Li M, Shi AX, Li KX (2016) Pharmacokinetics of ginsenoside Rg1 in rat medial prefrontal cortex, hippocampus, and lateral ventricle after subcutaneous administration. J Asian Nat Prod Res 18:587–595
Liu Y, Gao Y, Li KX, Xue W (2019) Pharmacokinetics and acetylcholine releasing effects of ginsenoside Rg1 in hippocampus of beta-amyloid model rats. J Asian Nat Prod Res 21:772–781
Sweeney MD, Zhao Z, Montagne A, Nelson AR, Zlokovic BV (2019) Blood-brain barrier: from physiology to disease and back. Physiol Rev 99:21–78
Acknowledgements
The authors acknowledge the support from the National Natural Science Foundation of China (81773925), the Beijing Natural Science Foundation (7212156) and CAMS Innovation Fund for Medical Sciences (CIFMS) (2021-I2M-1-026), the Fundamental Research Funds for the Central Universities (3332019154), NHC Key Laboratory of Drug Addiction Medicine, The First Affiliated Hospital of Kunming Medical University, Kunming, China (2020DAMOP-008).
Funding
The authors have not disclosed any funding.
Author information
Authors and Affiliations
Contributions
YY and NC designed the experiments; YL and YC wrote the manuscript and prepared the figures; YC, YL and SW performed the animal model and behavior tests; YC and TZ performed western blotting assays, IHC and IF assays. All authors reviewed the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chen, Y., Li, YY., Wang, S. et al. Ginsenoside Rg1 Plays a Neuroprotective Role in Regulating the Iron-Regulated Proteins and Against Lipid Peroxidation in Oligodendrocytes. Neurochem Res 47, 1721–1735 (2022). https://doi.org/10.1007/s11064-022-03564-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-022-03564-6