Abstract
Purpose
Glioblastoma (GBM) is a fatal primary brain tumor with extremely poor clinical outcomes. The anticancer efficiency of tyrosine kinase inhibitors (TKIs) has been shown in GBM and other cancer, with limited therapeutic outcomes. In the current study, we aimed to investigate the clinical impact of active proline-rich tyrosine kinase-2 (PYK2) and epidermal growth factor receptor (EGFR) in GBM and evaluate its druggability by a synthetic TKI-Tyrphostin A9 (TYR A9).
Methods
The expression profile of PYK2 and EGFR in astrocytoma biopsies (n = 48) and GBM cell lines were evaluated through quantitative PCR, western blots, and immunohistochemistry. The clinical association of phospho-PYK2 and EGFR was analyzed with various clinicopathological features and the Kaplan–Meier survival curve. The phospho-PYK2 and EGFR druggability and subsequent anticancer efficacy of TYR A9 was evaluated in GBM cell lines and intracranial C6 glioma model.
Results
Our expression data revealed an increased phospho-PYK2, and EGFR expression aggravates astrocytoma malignancy and is associated with patients’ poor survival. The mRNA and protein correlation analysis showed a positive association between phospho-PYK2 and EGFR in GBM tissues. The in-vitro studies demonstrated that TYR A9 reduced GBM cell growth, cell migration, and induced apoptosis by attenuating PYK2/EGFR-ERK signaling. The in-vivo data showed TYR A9 treatment dramatically reduced glioma growth with augmented animal survival by repressing PYK2/EGFR-ERK signaling.
Conclusion
Altogether, this study report that increased phospho-PYK2 and EGFR expression in astrocytoma was associated with poor prognosis. The in-vitro and in-vivo evidence underlined translational implication of TYR A9 by suppressing PYK2/EGFR-ERK modulated signaling pathway.
Graphical abstract
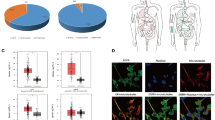
The schematic diagram displayed proof of concept of the current study indicating activated PYK2 either through the Ca2+/Calmodulin-dependent protein kinase II (CAMKII) signaling pathway or autophosphorylation at Tyr402 induces association to the SH2 domain of c-Src that leads to c-Src activation. Activated c-Src in turn activates PYK2 at other tyrosine residues that recruit Grb2/SOS complex and trigger ERK½ activation. Besides, PYK2 interaction with c-Src acts as an upstream of EGFR transactivator that can activate the ERK½ signaling pathway, which induces cell proliferation and cell survival by increasing anti-apoptotic proteins or inhibiting pro-apoptotic proteins. TYR A9 treatment attenuate GBM cell proliferation and migration; and induce GBM cell death by inhibiting PYK2 and EGFR-induced ERK activation.






Similar content being viewed by others
Data availability
All data corresponding to this study is available in this paper or its supplementary files.
Abbreviations
- GBM:
-
Glioblastoma
- PYK2:
-
Proline-rich kinase-2
- EGFR:
-
Epidermal growth factor receptor
- TKI:
-
Tyrosine kinase inhibitor
- TYR A9:
-
Tyrphostin A9
- AO:
-
Acridine orange
- EtBr:
-
Ethidium bromide
References
Ostrom QT, Cioffi G, Gittleman H, Patil N, Waite K, Kruchko C, Barnholtz-Sloan JS (2019) CBTRUS Statistical Report: primary brain and other Central Nervous System Tumors diagnosed in the United States in 2012–2016. Neuro Oncol 21:v1–v100. https://doi.org/10.1093/neuonc/noz150
Bondy ML, Scheurer ME, Malmer B, Barnholtz-Sloan JS, Davis FG, Il’yasova D, Kruchko C, McCarthy BJ, Rajaraman P, Schwartzbaum JA, Sadetzki S, Schlehofer B, Tihan T, Wiemels JL, Wrensch M, Buffler PA (2008) Brain tumor epidemiology: consensus from the Brain Tumor Epidemiology Consortium. Cancer 113:1953–1968. https://doi.org/10.1002/cncr.23741
Ohgaki H, Kleihues P (2005) Epidemiology and etiology of gliomas. Acta Neuropathol 109:93–108. https://doi.org/10.1007/s00401-005-0991-y
Ramirez YP, Weatherbee JL, Wheelhouse RT, Ross AH (2013) Glioblastoma multiforme therapy and mechanisms of resistance. Pharmaceuticals (Basel) 6:1475–1506. https://doi.org/10.3390/ph6121475
Minniti G, Muni R, Lanzetta G, Marchetti P, Enrici RM (2009) Chemotherapy for glioblastoma: current treatment and future perspectives for cytotoxic and targeted agents. Anticancer Res 29:5171–5184
Du Z, Lovly CM (2018) Mechanisms of receptor tyrosine kinase activation in cancer. Mol Cancer 17:58. https://doi.org/10.1186/s12943-018-0782-4
McDonell LM, Kernohan KD, Boycott KM, Sawyer SL (2015) Receptor tyrosine kinase mutations in developmental syndromes and cancer: two sides of the same coin. Hum Mol Genet 24:R60-66. https://doi.org/10.1093/hmg/ddv254
Lemmon MA, Schlessinger J, Ferguson KM (2014) The EGFR family: not so prototypical receptor tyrosine kinases. Cold Spring Harb Perspect Biol 6:a020768. https://doi.org/10.1101/cshperspect.a020768
Eskilsson E, Rosland GV, Solecki G, Wang Q, Harter PN, Graziani G, Verhaak RGW, Winkler F, Bjerkvig R, Miletic H (2018) EGFR heterogeneity and implications for therapeutic intervention in glioblastoma. Neuro Oncol 20:743–752. https://doi.org/10.1093/neuonc/nox191
Avraham H, Park SY, Schinkmann K, Avraham S (2000) RAFTK/Pyk2-mediated cellular signalling. Cell Signal 12:123–133. https://doi.org/10.1016/s0898-6568(99)00076-5
Zhu X, Bao Y, Guo Y, Yang W (2018) Proline-Rich protein tyrosine kinase 2 in inflammation and Cancer. Cancers (Basel). https://doi.org/10.3390/cancers10050139
Ginnan R, Singer HA (2002) CaM kinase II-dependent activation of tyrosine kinases and ERK1/2 in vascular smooth muscle. Am J Physiol Cell Physiol 282:C754-761. https://doi.org/10.1152/ajpcell.00335.2001
Park SY, Li H, Avraham S (2007) RAFTK/Pyk2 regulates EGF-induced PC12 cell spreading and movement. Cell Signal 19:289–300. https://doi.org/10.1016/j.cellsig.2006.07.005
Behmoaram E, Bijian K, Jie S, Xu Y, Darnel A, Bismar TA, Alaoui-Jamali MA (2008) Focal adhesion kinase-related proline-rich tyrosine kinase 2 and focal adhesion kinase are co-overexpressed in early-stage and invasive ErbB-2-positive breast cancer and cooperate for breast cancer cell tumorigenesis and invasiveness. Am J Pathol 173:1540–1550. https://doi.org/10.2353/ajpath.2008.080292
Selitrennik M, Lev S (2015) PYK2 integrates growth factor and cytokine receptors signaling and potentiates breast cancer invasion via a positive feedback loop. Oncotarget 6:22214–22226. https://doi.org/10.18632/oncotarget.4257
Zhang B, Yin C, Li H, Shi L, Liu N, Sun Y, Lu S, Liu Y, Sun L, Li X, Chen W, Qi Y (2013) Nir1 promotes invasion of breast cancer cells by binding to chemokine (C–C motif) ligand 18 through the PI3K/Akt/GSK3beta/Snail signalling pathway. Eur J Cancer 49:3900–3913. https://doi.org/10.1016/j.ejca.2013.07.146
Gutenberg A, Bruck W, Buchfelder M, Ludwig HC (2004) Expression of tyrosine kinases FAK and Pyk2 in 331 human astrocytomas. Acta Neuropathol 108:224–230. https://doi.org/10.1007/s00401-004-0886-3
Lipinski CA, Tran NL, Bay C, Kloss J, McDonough WS, Beaudry C, Berens ME, Loftus JC (2003) Differential role of proline-rich tyrosine kinase 2 and focal adhesion kinase in determining glioblastoma migration and proliferation. Mol Cancer Res 1:323–332
Miao L, Xin X, Xin H, Shen X, Zhu YZ (2016) Hydrogen Sulfide Recruits Macrophage Migration by Integrin beta1-Src-FAK/Pyk2-Rac pathway in myocardial infarction. Sci Rep 6:22363. https://doi.org/10.1038/srep22363
Okigaki M, Davis C, Falasca M, Harroch S, Felsenfeld DP, Sheetz MP, Schlessinger J (2003) Pyk2 regulates multiple signaling events crucial for macrophage morphology and migration. Proc Natl Acad Sci U S A 100:10740–10745. https://doi.org/10.1073/pnas.1834348100
Shen T, Guo Q (2018) Role of Pyk2 in human cancers. Med Sci Monit 24:8172–8182. https://doi.org/10.12659/MSM.913479
Shen T, Guo Q (2019) EGFR signaling pathway occupies an important position in cancer-related downstream signaling pathways of Pyk2. Cell Biol Int. https://doi.org/10.1002/cbin.11209
Lipinski CA, Tran NL, Menashi E, Rohl C, Kloss J, Bay RC, Berens ME, Loftus JC (2005) The tyrosine kinase pyk2 promotes migration and invasion of glioma cells. Neoplasia 7:435–445
Hojjat-Farsangi M (2014) Small-molecule inhibitors of the receptor tyrosine kinases: promising tools for targeted cancer therapies. Int J Mol Sci 15:13768–13801. https://doi.org/10.3390/ijms150813768
Tilak M, Holborn J, New LA, Lalonde J, Jones N (2021) Receptor tyrosine kinase signaling and targeting in Glioblastoma Multiforme. Int J Mol Sci 22:1831. https://doi.org/10.3390/ijms22041831
Fuortes M, Melchior M, Han H, Lyon GJ, Nathan C (1999) Role of the tyrosine kinase pyk2 in the integrin-dependent activation of human neutrophils by TNF. J Clin Invest 104:327–335. https://doi.org/10.1172/JCI6018
Levitzki A, Gazit A, Osherov N, Posner I, Gilon C (1991) Inhibition of protein-tyrosine kinases by tyrphostins. Methods Enzymol 201:347–361. https://doi.org/10.1016/0076-6879(91)01031-v
Park SJ, Park YJ, Shin JH, Kim ES, Hwang JJ, Jin DH, Kim JC, Cho DH (2011) A receptor tyrosine kinase inhibitor, tyrphostin A9 induces cancer cell death through Drp1 dependent mitochondria fragmentation. Biochem Biophys Res Commun 408:465–470. https://doi.org/10.1016/j.bbrc.2011.04.053
Thyberg J (1998) Tyrphostin A9 and wortmannin perturb the golgi complex and block proliferation of vascular smooth muscle cells. Eur J Cell Biol 76:33–42. https://doi.org/10.1016/S0171-9335(98)80015-0
Joy ME, Vollmer LL, Hulkower K, Stern AM, Peterson CK, Boltz RC, Roy P, Vogt A (2014) A high-content, multiplexed screen in human breast cancer cells identifies profilin-1 inducers with anti-migratory activities. PLoS ONE 9:e88350. https://doi.org/10.1371/journal.pone.0088350
Block ER, Tolino MA, Klarlund JK (2010) Pyk2 activation triggers epidermal growth factor receptor signaling and cell motility after wounding sheets of epithelial cells. J Biol Chem 285:13372–13379. https://doi.org/10.1074/jbc.M109.083089
Tan AC, Vyse S, Huang PH (2017) Exploiting receptor tyrosine kinase co-activation for cancer therapy. Drug Discov Today 22:72–84. https://doi.org/10.1016/j.drudis.2016.07.010
Louis DN, Perry A, Reifenberger G, von Deimling A, Figarella-Branger D, Cavenee WK, Ohgaki H, Wiestler OD, Kleihues P, Ellison DW (2016) The 2016 World Health Organization classification of tumors of the Central Nervous System: a summary. Acta Neuropathol 131:803–820. https://doi.org/10.1007/s00401-016-1545-1
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) method. Methods 25:402–408. https://doi.org/10.1006/meth.2001.1262
Babu D, Mudiraj A, Yadav N, Y BVKC, Panigrahi M, Prakash Babu P (2021) Rabeprazole has efficacy per se and reduces resistance to temozolomide in glioma via EMT inhibition. Cell Oncol (Dordr) 44:889–905. https://doi.org/10.1007/s13402-021-00609-w
Sareddy GR, Panigrahi M, Challa S, Mahadevan A, Babu PP (2009) Activation of Wnt/beta-catenin/Tcf signaling pathway in human astrocytomas. Neurochem Int 55:307–317. https://doi.org/10.1016/j.neuint.2009.03.016
van Meerloo J, Kaspers GJ, Cloos J (2011) Cell sensitivity assays: the MTT assay. Methods Mol Biol 731:237–245. https://doi.org/10.1007/978-1-61779-080-5_20
Franken NA, Rodermond HM, Stap J, Haveman J, van Bree C (2006) Clonogenic assay of cells in vitro. Nat Protoc 1:2315–2319. https://doi.org/10.1038/nprot.2006.339
Geeviman K, Babu D, Prakash Babu P (2018) Pantoprazole induces mitochondrial apoptosis and attenuates NF-kappaB signaling in Glioma cells. Cell Mol Neurobiol 38:1491–1504. https://doi.org/10.1007/s10571-018-0623-4
Kim KH, Sederstrom JM (2015) Assaying cell cycle Status using Flow Cytometry. Curr Protoc Mol Biol 111(26 11):21–28. https://doi.org/10.1002/0471142727.mb2806s111
Kimata M, Matoba S, Iwai-Kanai E, Nakamura H, Hoshino A, Nakaoka M, Katamura M, Okawa Y, Mita Y, Okigaki M, Ikeda K, Tatsumi T, Matsubara H (2010) p53 and TIGAR regulate cardiac myocyte energy homeostasis under hypoxic stress. Am J Physiol Heart Circ Physiol 299:H1908-1916. https://doi.org/10.1152/ajpheart.00250.2010
Smilowitz HM, Weissenberger J, Weis J, Brown JD, O’Neill RJ, Laissue JA (2007) Orthotopic transplantation of v-src-expressing glioma cell lines into immunocompetent mice: establishment of a new transplantable in vivo model for malignant glioma. J Neurosurg 106:652–659. https://doi.org/10.3171/jns.2007.106.4.652
Babu D, Mudiraj A, Yadav N, Y BVKC, Panigrahi M, Prakash Babu P (2021) Rabeprazole has efficacy per se and reduces resistance to temozolomide in glioma via EMT inhibition. Cell Oncol (Dordr). https://doi.org/10.1007/s13402-021-00609-w
Mey U (1978) Foundations of the diagnosis and therapy of hemolytic anemias. Z Gesamte Inn Med 33:265–270
Camacho A, Segoviano-Ramirez JC, de Sanchez-Garcia A, la Rosa J, Garcia-Juarez J, Hernandez-Puente CA, Calvo-Anguiano G, Maltos-Uro SR, Olguin A, Gojon-Romanillos G, Gojon-Zorrilla G, Ortiz-Lopez R (2018) Tyrphostin AG17 inhibits adipocyte differentiation in vivo and in vitro. Lipids Health Dis 17:128. https://doi.org/10.1186/s12944-018-0784-7
Kim SJ, Kim HS, Seo YR (2019) Understanding of ROS-Inducing Strategy in Anticancer Therapy. Oxid Med Cell Longev 2019:5381692. https://doi.org/10.1155/2019/5381692
Happold C, Roth P, Wick W, Schmidt N, Florea AM, Silginer M, Reifenberger G, Weller M (2012) Distinct molecular mechanisms of acquired resistance to temozolomide in glioblastoma cells. J Neurochem 122:444–455. https://doi.org/10.1111/j.1471-4159.2012.07781.x
Tan AC, Ashley DM, Lopez GY, Malinzak M, Friedman HS, Khasraw M (2020) Management of glioblastoma: state of the art and future directions. CA Cancer J Clin 70:299–312. https://doi.org/10.3322/caac.21613
Rajaratnam V, Islam MM, Yang M, Slaby R, Ramirez HM, Mirza SP (2020) Glioblastoma: pathogenesis and current status of chemotherapy and other novel treatments. Cancers (Basel). https://doi.org/10.3390/cancers12040937
Gong J, Luk F, Jaiswal R, Bebawy M (2014) Microparticles mediate the intercellular regulation of microRNA-503 and proline-rich tyrosine kinase 2 to alter the migration and invasion capacity of breast cancer cells. Front Oncol 4:220
Garrido C, Galluzzi L, Brunet M, Puig PE, Didelot C, Kroemer G (2006) Mechanisms of cytochrome c release from mitochondria. Cell Death Differ 13:1423–1433. https://doi.org/10.1038/sj.cdd.4401950
Cadenas S (2018) Mitochondrial uncoupling, ROS generation and cardioprotection. Biochim Biophys Acta Bioenerg 1859:940–950. https://doi.org/10.1016/j.bbabio.2018.05.019
Sagara Y, Ishige K, Tsai C, Maher P (2002) Tyrphostins protect neuronal cells from oxidative stress. J Biol Chem 277:36204–36215
Baffy G (2017) Mitochondrial uncoupling in cancer cells: liabilities and opportunities. Biochim Biophys Acta Bioenerg 1858:655–664. https://doi.org/10.1016/j.bbabio.2017.01.005
Childress ES, Alexopoulos SJ, Hoehn KL, Santos WL (2018) Small molecule mitochondrial uncouplers and their therapeutic potential. J Med Chem 61:4641–4655
Li SZ, Hu YY, Zhao J, Zhao YB, Sun JD, Yang YF, Ji CC, Liu ZB, Cao WD, Qu Y, Liu WP, Cheng G, Fei Z (2014) MicroRNA-34a induces apoptosis in the human glioma cell line, A172, through enhanced ROS production and NOX2 expression. Biochem Biophys Res Commun 444:6–12. https://doi.org/10.1016/j.bbrc.2013.12.136
Sullivan PG, Springer JE, Hall ED, Scheff SW (2004) Mitochondrial uncoupling as a therapeutic target following neuronal injury. J Bioenerg Biomembr 36:353–356
Lysechko TL, Cheung SM, Ostergaard HL (2010) Regulation of the tyrosine kinase Pyk2 by calcium is through production of reactive oxygen species in cytotoxic T lymphocytes. J Biol Chem 285:31174–31184. https://doi.org/10.1074/jbc.M110.118265
Xu C-S, Wang Z-F, Dai L-M, Chu S-H, Gong L-L, Yang M-H, Zhi-Qiang L (2014) Induction of proline-rich tyrosine kinase 2 activation-mediated C6 glioma cell invasion after anti-vascular endothelial growth factor therapy. J Translational Med 12:148. https://doi.org/10.1186/1479-5876-12-148
Yang Y, Li S, Wang Y, Zhao Y, Li Q (2022) Protein tyrosine kinase inhibitor resistance in malignant tumors: molecular mechanisms and future perspective. Signal Transduct Target Ther 7:329. https://doi.org/10.1038/s41392-022-01168-8
Singh N, Miner A, Hennis L, Mittal S (2021) Mechanisms of temozolomide resistance in glioblastoma - a comprehensive review. Cancer Drug Resist 4:17–43. https://doi.org/10.20517/cdr.2020.79
Acknowledgements
The authors thank Dr. Satish I. from the Department of Pathology, Krishna Institute of Medical Sciences, India, for their help in the clinicopathological assessment.
Funding
The financial assistance to the lab from the Ministry of Science and Technology, DST- SERB Core grant, file No. CRG/2020/005021 and financial support to the University of Hyderabad-IoE by the Ministry of Education, Govt. of India (F11/9/2019-U3 (A). BUILDER-DBT-BT/INF/22/SP41176/2020 to the school of life Sciences. NY thanks, CSIR-UGC for student fellowship (S.No. 2061630688 Ref. No: 19/06/2016(i) EU-V).
Author information
Authors and Affiliations
Contributions
NY and PPB designed the study. NY performed all experiments. NY, DB and PPB analyzed data. MP and SM surgically excised astrocytoma tumor and NY collected tumor biopsies and provided clinical information. SM and MP evaluate clinicopathological data. NY and DB prepared the manuscript. NY, DB and PPB finalized the manuscript. All authors read and approved its submission.
Corresponding author
Ethics declarations
Competing interest
The authors declare no competing interests.
Ethical approval
The use of clinical biopsies and clinicopathological information in the study was approved by the Institutional Ethics Committee (UH/IEC/2016/180), University of Hyderabad, India. All animal procedures followed the Institutional Animal Ethics Committee guidelines (UH/IAEC/PPB/2021-22/22) of the University of Hyderabad.
Consent to participants
Written informed consent was obtained from each patient or their relatives.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yadav, N., Babu, D., Madigubba, S. et al. Tyrphostin A9 attenuates glioblastoma growth by suppressing PYK2/EGFR-ERK signaling pathway. J Neurooncol 163, 675–692 (2023). https://doi.org/10.1007/s11060-023-04383-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-023-04383-7