Abstract
Purpose
To compare treatment results between fractionated gamma knife radiosurgery (f-GKRS) and staged gamma knife radiosurgery (s-GKRS) for mid-to-large brain metastases (BMs).
Methods
We retrospectively analyzed data of patients with medium (4–10 mL) to large (> 10 mL) BMs who underwent s-GKRS or f-GKRS between March 2008 and September 2022. Patients were treated with (i) s-GKRS before May 2018 and (ii) f-GKRS after May 2018. Patients who underwent follow-up magnetic resonance imaging at least once were enrolled. Case-matched studies were conducted by applying propensity score matching to minimize treatment selection bias and potential confounding. Local control (LC) was set as the primary endpoint and overall survival (OS) as the secondary endpoint.
Results
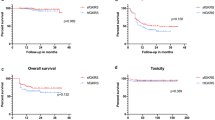
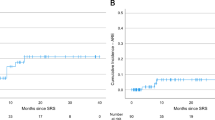
This study included 129 patients with 136 lesions and 70 patients with 78 lesions who underwent s-GKRS and f-GKRS, respectively. Overall, 124 lesions (62 lesions in each group) were selected in the case-matched group. No differences were observed in the 6-month and 1-year cumulative incidences of LC failure between the s-GKRS and f-GKRS groups (15.6% vs. 15.9% at 6 months and 25.6% vs. 25.6% at 1 year; p = 0.617). One-year OS rates were 62.6% (95% confidence interval [CI]: 45.4–75.7%) and 73.9% (95% CI: 58.8–84.2%) in the s-GKRS and f-GKRS groups, respectively. The post-GKRS median survival time was shorter in the s-GKRS group than in the f-GKRS group (17 vs. 36 months), without significance (p = 0.202).
Conclusions
This is the first study to compare f-GKRS and s-GKRS in large BMs. Fractionation is as effective as staged GKRS for treating mid-to-large BMs.

Similar content being viewed by others
Data Availability
The datasets generated and/or analyzed during the current study are available by contacting the corresponding author (R.N., rnrn46_8447@yahoo.co.jp).
References
Serizawa T, Higuchi Y, Nagano O (2013) Stereotactic radiosurgery for brain metastases. Neurosurg Clin N Am 24:597–603. https://doi.org/10.1016/j.nec.2013.05.007
Chon H, Yoon K, Lee D, Kwon DH, Cho YH (2019) Single-fraction versus hypofractionated stereotactic radiosurgery for medium-sized brain metastases of 2.5 to 3 cm. J Neurooncol 145:49–56. https://doi.org/10.1007/s11060-019-03265-1
Zimmerman AL, Murphy ES, Suh JH et al (2016) Treatment of large brain metastases with stereotactic radiosurgery. Technol Cancer Res Treat 15:186–195. https://doi.org/10.1177/1533034614568097
Han JH, Kim DG, Chung HT, Paek SH, Park CK, Jung HW (2012) Radiosurgery for large brain metastases. Int J Radiat Oncol Biol Phys 83:113–120. https://doi.org/10.1016/j.ijrobp.2011.06.1965
Yang HC, Kano H, Lunsford LD, Niranjan A, Flickinger JC, Kondziolka D (2011) What factors predict the response of larger brain metastases to radiosurgery. Neurosurgery 68:682–690 discussion 690. https://doi.org/10.1227/NEU.0b013e318207a58b
Higuchi Y, Serizawa T, Nagano O et al (2009) Three-staged stereotactic radiotherapy without whole brain irradiation for large metastatic brain tumors. Int J Radiat Oncol Biol Phys 74:1543–1548. https://doi.org/10.1016/j.ijrobp.2008.10.035
Serizawa T, Higuchi Y, Yamamoto M et al (2018) Comparison of treatment results between 3- and 2-stage Gamma Knife radiosurgery for large brain metastases: a retrospective multi-institutional study. J Neurosurg 131:227–237. https://doi.org/10.3171/2018.4.JNS172596
Yomo S, Oda K, Oguchi K (2020) Single- versus 2-session gamma knife surgery for symptomatic midsize brain metastases: a propensity score-matched analysis. J Neurosurg 133:1646–1654. https://doi.org/10.3171/2019.7.JNS191193
Lehrer EJ, Peterson JL, Zaorsky NG et al (2019) Single versus multifraction stereotactic radiosurgery for large brain metastases: an international meta-analysis of 24 trials. Int J Radiat Oncol Biol Phys 103:618–630. https://doi.org/10.1016/j.ijrobp.2018.10.038
Samanci Y, Sisman U, Altintas A et al (2021) Hypofractionated frameless gamma knife radiosurgery for large metastatic brain tumors. Clin Exp Metastasis 38:31–46. https://doi.org/10.1007/s10585-020-10068-6
Park HR, Park KW, Lee JM et al (2019) Frameless fractionated gamma knife radiosurgery with ICON™ for large metastatic brain tumors. J Korean Med Sci 34:e57. https://doi.org/10.3346/jkms.2019.34.e57
Noda R, Akabane A, Kawashima M, Oshima A, Tsunoda S, Segawa M, Inoue T (2022) Fractionated gamma knife radiosurgery after cyst aspiration for large cystic brain metastases: case series and literature review. Neurosurg Rev 45:3457–3465. https://doi.org/10.1007/s10143-022-01835-y
Kawashima M, Akabane A, Noda R, Segawa M, Tsunoda S, Inoue T (2022) Interfractional change of tumor volume during fractionated stereotactic radiotherapy using gamma knife for brain metastases. J Neurooncol 159:409–416. https://doi.org/10.1007/s11060-022-04075-8
Masucci GL (2018) Hypofractionated radiation therapy for large brain metastases. Front Oncol 8:379. https://doi.org/10.3389/fonc.2018.00379
van Leeuwen CM, Oei AL, Crezee J, Bel A, Franken NAP, Stalpers LJA, Kok HP (2018) The alfa and beta of tumours: a review of parameters of the linear-quadratic model, derived from clinical radiotherapy studies. Radiat Oncol 13:96. https://doi.org/10.1186/s13014-018-1040-z
Yomo S, Hayashi M, Nicholson C (2012) A prospective pilot study of two-session gamma knife surgery for large metastatic brain tumors. J Neurooncol 109:159–165. https://doi.org/10.1007/s11060-012-0882-8
Yomo S, Hayashi M (2014) A minimally invasive treatment option for large metastatic brain tumors: long-term results of two-session gamma knife stereotactic radiosurgery. Radiat Oncol 9:132. https://doi.org/10.1186/1748-717X-9-132
Hasegawa T, Kato T, Yamamoto T, Iizuka H, Nishikawa T, Ito H, Kato N (2017) Multisession gamma knife surgery for large brain metastases. J Neurooncol 131:517–524. https://doi.org/10.1007/s11060-016-2317-4
Angelov L, Mohammadi AM, Bennett EE et al (2018) Impact of 2-staged stereotactic radiosurgery for treatment of brain metastases ≥ 2 cm. J Neurosurg 129:366–382. https://doi.org/10.3171/2017.3.JNS162532
Dohm A, McTyre ER, Okoukoni C et al (2018) Staged stereotactic radiosurgery for large brain metastases: local control and clinical outcomes of a one-two punch technique. Neurosurgery 83:114–121. https://doi.org/10.1093/neuros/nyx355
Yamamoto M, Higuchi Y, Serizawa T et al (2018) Three-stage gamma knife treatment for metastatic brain tumors larger than 10 cm3: a 2-institute study including re-analyses of earlier results using competing risk analysis. J Neurosurg 129:77–85. https://doi.org/10.3171/2018.7.GKS181392
Ito D, Aoyagi K, Nagano O, Serizawa T, Iwadate Y, Higuchi Y (2020) Comparison of two-stage gamma knife radiosurgery outcomes for large brain metastases among primary cancers. J Neurooncol 147:237–246. https://doi.org/10.1007/s11060-020-03421-y
Cho A, Medvedeva K, Kranawetter B et al (2022) How to dose-stage large or high-risk brain metastases: an alternative two-fraction radiosurgical treatment approach. J Neurosurg 137:1666–1675. https://doi.org/10.3171/2022.2.JNS212440
Marcrom SR, McDonald AM, Thompson JW et al (2017) Fractionated stereotactic radiation therapy for intact brain metastases. Adv Radiat Oncol 2:564–571. https://doi.org/10.1016/j.adro.2017.07.006
Minniti G, Scaringi C, Paolini S et al (2016) Single-fraction versus multifraction (3 × 9 gy) stereotactic radiosurgery for large (> 2 cm) brain metastases: a comparative analysis of local control and risk of radiation-induced brain necrosis. Int J Radiat Oncol Biol Phys 95:1142–1148. https://doi.org/10.1016/j.ijrobp.2016.03.013
Navarria P, Pessina F, Cozzi L et al (2016) Hypo-fractionated stereotactic radiotherapy alone using volumetric modulated arc therapy for patients with single, large brain metastases unsuitable for surgical resection. Radiat Oncol 11:76. https://doi.org/10.1186/s13014-016-0653-3
Feuvret L, Vinchon S, Martin V et al (2014) Stereotactic radiotherapy for large solitary brain metastases. Cancer Radiother 18:97–106. https://doi.org/10.1016/j.canrad.2013.12.003
Jeong WJ, Park JH, Lee EJ, Kim JH, Kim CJ, Cho YH (2015) Efficacy and safety of fractionated stereotactic radiosurgery for large brain metastases. J Korean Neurosurg Soc 58:217–224. https://doi.org/10.3340/jkns.2015.58.3.217
Wegner RE, Leeman JE, Kabolizadeh P, Rwigema JC, Mintz AH, Burton SA, Heron DE (2015) Fractionated stereotactic radiosurgery for large brain metastases. Am J Clin Oncol 38:135–139. https://doi.org/10.1097/COC.0b013e31828aadac
Murai T, Ogino H, Manabe Y et al (2014) Fractionated stereotactic radiotherapy using CyberKnife for the treatment of large brain metastases: a dose escalation study. Clin Oncol (R Coll Radiol) 26:151–158. https://doi.org/10.1016/j.clon.2013.11.027
Lee EJ, Choi KS, Park ES, Cho YH (2021) Single- and hypofractionated stereotactic radiosurgery for large (> 2 cm) brain metastases: a systematic review. J Neurooncol 154:25–34. https://doi.org/10.1007/s11060-021-03805-8
Lindquist C, Paddick I (2007) The Leksell gamma knife perfexion and comparisons with its predecessors. Neurosurgery 61:130–140 discussion 140–141. https://doi.org/10.1227/01.neu.0000316276.20586.dd
Cao H, Xiao Z, Zhang Y et al (2019) Dosimetric comparisons of different hypofractionated stereotactic radiotherapy techniques in treating intracranial tumors > 3 cm in longest diameter. J Neurosurg 132:1024–1032. https://doi.org/10.3171/2018.12.JNS181578
Cui T, Weiner J, Danish S et al (2022) Evaluation of biological effective dose in gamma knife staged stereotactic radiosurgery for large brain metastases. Front Oncol 12:892139. https://doi.org/10.3389/fonc.2022.892139
Grimm MA, Köppen U, Stieler F et al (2020) Prospective assessment of mask versus frame fixation during gamma knife treatment for brain metastases. Radiother Oncol 147:195–199. https://doi.org/10.1016/j.radonc.2020.05.011
Pavlica M, Dawley T, Goenka A, Schulder M (2021) Frame-based and mask-based stereotactic radiosurgery: the patient experience, compared. Stereotact Funct Neurosurg 99:241–249. https://doi.org/10.1159/000511587
Régis J, Merly L, Balossier A et al (2022) Mask-based versus frame-based gamma knife ICON radiosurgery in brain metastases: a prospective randomized trial. Stereotact Funct Neurosurg 100:86–94. https://doi.org/10.1159/000519280
Carminucci A, Nie K, Weiner J, Hargreaves E, Danish SF (2018) Assessment of motion error for frame-based and noninvasive mask-based fixation using the Leksell gamma knife icon radiosurgery system. J Neurosurg 129:133–139. https://doi.org/10.3171/2018.7.GKS181516
Yan M, Holden L, Wang M et al (2022) Gamma knife icon based hypofractionated stereotactic radiosurgery (GKI-HSRS) for brain metastases: impact of dose and volume. J Neurooncol 159:705–712. https://doi.org/10.1007/s11060-022-04115-3
Kim JW, Park HR, Lee JM et al (2016) Fractionated stereotactic gamma knife radiosurgery for large brain metastases: a retrospective, single center study. PLoS ONE 11:e0163304. https://doi.org/10.1371/journal.pone.0163304
Khan M, Spicer J (2019) The evolving landscape of cancer therapeutics. Handb Exp Pharmacol 260:43–79. https://doi.org/10.1007/164_2019_312
Funding
The authors declare that no funds, grants or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, and statistical analysis, figure preparation were performed by Ryuichi Noda. The first draft of the manuscript was written by Ryuichi Noda and all authors commented on previous versions of the manuscript. Statistical analysis was reviewed by Mariko Kawashima and Atsuya Akabane. Data collection was performed by Ryuichi Noda, Mariko Kawashima, Atsuya Akabane. The study was directed by Tomohiro Inoue and Atsuya Akabane. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
This study was conducted in accordance with the Declaration of Helsinki (revised version, 2013). The study protocol was approved by the Institutional Review Board of NTT Medical Center, Tokyo (approval number: 21‒71).
Consent to participate
Written informed consent was obtained from all patients.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplemental Digital Content 1
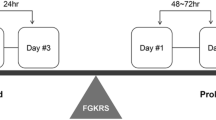
: Fig. a Schematic of staged gamma knife radiosurgery treatment protocol. The prescription dose of each fraction was set to 11.8–14.2 Gy for the two-staged GKRS and 9.0–11.0 Gy for the three-staged GKRS. The treatment intervals were completed within 6 weeks, with ≥ 12 days between each fraction. Fig. b Schematic of fractionated gamma knife radiosurgery treatment protocol. The prescription dose of each fraction for more than five-fraction cases were set to 3.0–5.0 Gy, and for five or fewer fraction cases were set to 6.0–9.5 Gy. Interfractional evaluation by MRI was performed when the treatment continued for more than five fractions (> 1 week), and the treatment plan was modified if necessary, as reported previously. GKRS, gamma knife radiosurgery; MRI, magnetic resonance images
Supplemental Digital content 2:
Table 1. Clinical characteristics of the 163 lesions of s-GKRS vs. f-GKRS (≤5 fr.) and the case-matched 46 lesions. Table 2. Clinical characteristics of the 187 lesions of s-GKRS vs. f-GKRS (>5 fr.) and the case-matched 84 lesions. Table 3. Summary of treatment parameters of f-GKRS (≤5 fr.) lesions and f-GKRS (>5 fr.) lesions
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Noda, R., Kawashima, M., Segawa, M. et al. Fractionated versus staged gamma knife radiosurgery for mid-to-large brain metastases: a propensity score-matched analysis. J Neurooncol 164, 87–96 (2023). https://doi.org/10.1007/s11060-023-04374-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-023-04374-8