Abstract
Introduction
Stereotactic radiosurgery (SRS) is an emerging treatment for patients with multiple brain metastases (BM). The present work compares the SRS of multiple brain metastases with whole-brain radiotherapy (WBRT).
Methods
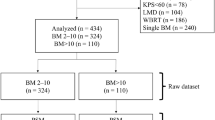
We performed a matched-pair analysis for 128 patients with multiple BM treated with either SRS or WBRT over a 5-year period. Patients were matched pairwise for seven potential prognostic factors. A mixed Cox Proportional Hazards model with univariate and multivariate analysis was fitted for overall survival (OS). Distant intracranial progression-free survival (icPFS) and local control were assessed using a Fine and Gray subdistribution hazard model and considering death as competing event.
Results
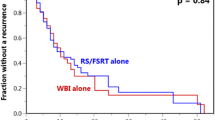
Patients undergoing SRS had a median of 4 BM (range 3–16). 1-year local control of individual BM following SRS was 91.7%. Median OS in the SRS subgroup was 15.7 months (IQR 9.7–36.4) versus 8.0 months (interquartile range, IQR 3.8–18.0) in the WBRT subgroup (HR 2.25, 95% CI [1.5; 3.5], p < 0.001). Median icPFS was 8.6 (IQR 3.4–18.0) versus 22.4 (IQR 5.6–28.6) months, respectively (HR for WBRT 0.41, 95% CI [0.24; 0.71], p = 0.001). Following SRS, synchronous BM diagnosis (HR 2.51, 95% CI [1.30; 4.70], p = 0.004), higher initial number of BM (HR 1.21, 95% CI [1.10; 1.40], p = 0.002) and lung cancer histology (HR 2.05, 95% CI [1.10; 3.80], p = 0.024) negatively impacted survival. Excellent clinical performance (KPI 90%) was a positive prognosticator (HR 0.38, 95% CI [0.20; 0.72], p = 0.003), as was extracerebral tumor control (HR 0.48, 95% CI [0.24; 0.97], p = 0.040). Higher initial (HR 1.19, 95% CI [1.00; 1.40], p < 0.013) and total number of BM (HR 1.23, 95% CI [1.10; 1.40], p < 0.001) were prognostic for shorter icPFS.
Conclusion
This is the first matched-pair analysis to compare SRS alone versus WBRT alone for multiple BM. OS was prolonged in the SRS subgroup and generally favorable in the entire cohort. Our results suggest SRS as a feasible and effective treatment for patients with multiple BM.

Similar content being viewed by others
References
Weller M (2015) Leitlinien für Diagnostik und Therapie in der Neurologie: Hirnmetastasen und Meningeosis neoplastica. DGN 30:1–42
National Comprehensive Cancer Network (2016) Central nervous system cancers V1.2019, p 123. https://www.nccn.org/professionals/physician_gls/pdf/cns.pdf
Yamamoto M, Serizawa T, Shuto T, Akabane A, Higuchi Y, Kawagishi J, Yamanaka K, Sato Y, Jokura H, Yomo S et al (2014) Stereotactic radiosurgery for patients with multiple brain metastases (JLGK0901): a multi-institutional prospective observational study. Lancet Oncol 15:387–395. https://doi.org/10.1016/S1470-2045(14)70061-0
Chang EL, Wefel JS, Hess KR, Allen PK, Lang FF, Kornguth DG, Arbuckle RB, Swint JM, Shiu AS, Maor MH et al (2009) Neurocognition in patients with brain metastases treated with radiosurgery or radiosurgery plus whole-brain irradiation: a randomised controlled trial. Lancet Oncol 10:1037–1044. https://doi.org/10.1016/S1470-2045(09)70263-3
Aoyama H, Tago M, Kato N, Toyoda T, Kenjyo M, Hirota S, Shioura H, Inomata T, Kunieda E, Hayakawa K et al (2007) Neurocognitive function of patients with brain metastasis who received either whole brain radiotherapy plus stereotactic radiosurgery or radiosurgery alone. Int J Radiat Oncol Biol Phys 68:1388–1395. https://doi.org/10.1016/j.ijrobp.2007.03.048
Brown PD, Ballman KV, Cerhan JH, Anderson SK, Carrero XW, Whitton AC, Greenspoon J, Parney IF, Laack NNI, Ashman JB et al (2017) Postoperative stereotactic radiosurgery compared with whole brain radiotherapy for resected metastatic brain disease (NCCTG N107C/CEC·3): a multicentre, randomised, controlled, phase 3 trial. Lancet Oncol 18:1049–1060. https://doi.org/10.1016/S1470-2045(17)30441-2
Adler JR, Chang SD, Murphy MJ, Doty J, Geis P, Hancock SL (1997) The Cyberknife: a frameless robotic system for radiosurgery. Stereotact Funct Neurosurg 69:124–128
Leksell L (1951) The stereotaxic method and radiosurgery of the brain. Acta Chir Scand 102:316–319
Gregucci F, Fiorentino A, Corradini S, Figlia V, Mazzola R, Ricchetti F, Ruggieri R, Alongi F (2018) Linac-based radiosurgery or fractionated stereotactic radiotherapy with flattening filter-free volumetric modulated arc therapy in elderly patients. Strahlentherapie und Onkol. https://doi.org/10.1007/s00066-018-1405-0
Thomas EM, Popple RA, Wu X, Clark GM, Markert JM, Guthrie BL, Yuan Y, Dobelbower MC, Spencer SA, Fiveash JB (2014) Comparison of plan quality and delivery time between volumetric arc therapy (rapidarc) and gamma knife radiosurgery for multiple cranial metastases. Neurosurgery 75:409–417. https://doi.org/10.1227/NEU.0000000000000448
Hofmaier J, Bodensohn R, Garny S, Hadi I, Fleischmann DF, Eder M, Dinc Y, Reiner M, Corradini S, Parodi K et al (2019) Single isocenter stereotactic radiosurgery for patients with multiple brain metastases: dosimetric comparison of VMAT and a dedicated DCAT planning tool. Radiat Oncol 14:103. https://doi.org/10.1186/s13014-019-1315-z
Rades D, Janssen S, Bajrovic A, Khoa MT, Veninga T, Schild SE (2017) A matched-pair analysis comparing whole-brain radiotherapy with and without a stereotactic boost for intracerebral control and overall survival in patients with one to three cerebral metastases. Radiat Oncol 12:10–15. https://doi.org/10.1186/s13014-017-0804-1
Kessel KA, Bohn C, Engelmann U, Oetzel D, Bougatf N, Bendl R, Debus J, Combs SE (2014) Five-year experience with setup and implementation of an integrated database system for clinical documentation and research. Comput Methods Prog Biomed 114:206–217. https://doi.org/10.1016/j.cmpb.2014.02.002
Kocher M, Wittig A, Piroth MD, Treuer H, Seegenschmiedt H, Ruge M, Grosu AL, Guckenberger M (2014) Stereotactic radiosurgery for treatment of brain metastases: a report of the DEGRO working group on stereotactic radiotherapy. Strahlentherapie und Onkol 190:521–532. https://doi.org/10.1007/s00066-014-0648-7
Soffietti R, Abacioglu U, Baumert B, Combs SE, Kinhult S, Kros JM, Marosi C, Metellus P, Radbruch A, Freixa SSV et al (2017) Diagnosis and treatment of brain metastases from solid tumors: guidelines from the European Association of neuro-oncology (EANO). Neuro Oncol 19:162–174. https://doi.org/10.1093/neuonc/now241
Rief H, Bischof M, Bruckner T, Welzel T, Askoxylakis V, Rieken S, Lindel K, Combs S, Debus J (2013) The stability of osseous metastases of the spine in lung cancer—a retrospective analysis of 338 cases. Radiat Oncol 8:200. https://doi.org/10.1186/1748-717X-8-200
Scharp M, Hauswald H, Bischof M, Debus J, Combs SE (2014) Re-irradiation in the treatment of patients with cerebral metastases of solid tumors: retrospective analysis. Radiat Oncol 9:4. https://doi.org/10.1186/1748-717X-9-4
Schemper M, Smith TL (1996) A note on quantifying follow-up in studies of failure time. Control Clin Trials 17:343–346
Levin VA, Bidaut L, Hou P, Kumar AJ, Wefel JS, Bekele BN, Prabhu S, Loghin M, Gilbert MR, Jackson EF (2011) Randomized double-blind placebo-controlled trial of bevacizumab therapy for radiation necrosis of the central nervous system. Int J Radiat Oncol 79:1487–1495. https://doi.org/10.1016/j.ijrobp.2009.12.061
Shuto T, Akabane A, Yamamoto M, Serizawa T, Higuchi Y, Sato Y, Kawagishi J, Yamanaka K, Jokura H, Yomo S et al (2018) Multiinstitutional prospective observational study of stereotactic radiosurgery for patients with multiple brain metastases from non–small cell lung cancer (JLGK0901 study—NSCLC). J Neurosurg 129:86–94. https://doi.org/10.3171/2018.7.GKS181378
Yamamoto M, Serizawa T, Higuchi Y, Sato Y, Kawagishi J, Yamanaka K, Shuto T, Akabane A, Jokura H, Yomo S et al (2017) A multi-institutional prospective observational study of stereotactic radiosurgery for patients with multiple brain metastases (JLGK0901 study update): irradiation-related complications and long-term maintenance of mini-mental state examination scores. Int J Radiat Oncol Biol Phys 99:31–40. https://doi.org/10.1016/j.ijrobp.2017.04.037
Karlsson B, Hanssens P, Wolff R, Söderman M, Lindquist C, Beute G (2009) Thirty years’ experience with Gamma Knife surgery for metastases to the brain: clinical article. J Neurosurg 111:449–457. https://doi.org/10.3171/2008.10.JNS08214
Harris KB, Corbett MR, Mascarenhas H, Lee KS, Arastu H, Leinweber C, Ju AW (2017) A single-institution analysis of 126 patients treated with Stereotactic radiosurgery for brain metastases. Front Oncol 7:1–6. https://doi.org/10.3389/fonc.2017.00090
Nagtegaal S, Claes A, Suijkerbuijk K, Schramel F, Snijders T, Verhoeff J (2019) Comparing survival predicted by the diagnosis-specific graded prognostic assessment (DS-GPA) to actual survival in patients with 1–10 brain metastases treated with stereotactic radiosurgery. Radiother Oncol 138:173–179. https://doi.org/10.1016/j.radonc.2019.06.033
Hamel-Perreault E, Mathieu D, Masson-Cote L (2019) Factors influencing the outcome of stereotactic radiosurgery in patients with five or more brain metastases. Curr Oncol 26:e64–e69. https://doi.org/10.3747/co.26.4244
Fritz C, Borsky K, Stark LS, Tanadini-Lang S, Kroeze SGC, Krayenbühl J, Guckenberger M, Andratschke N (2018) Repeated courses of radiosurgery for new brain metastases to defer whole brain radiotherapy: feasibility and outcome with validation of the new prognostic metric brain metastasis velocity. Front Oncol 8:1–9. https://doi.org/10.3389/fonc.2018.00551
Ali MA, Hirshman BR, Wilson B, Carroll KT, Proudfoot JA, Goetsch SJ, Alksne JF, Ott K, Aiyama H, Nagano O et al (2017) Survival patterns of 5750 stereotactic radiosurgery-treated patients with brain metastasis as a function of the number of lesions. World Neurosurg 107(944–951):e1. https://doi.org/10.1016/j.wneu.2017.07.062
Andrews DW, Scott CB, Sperduto PW, Flanders AE, Gaspar LE, Schell MC, Werner-Wasik M, Demas W, Ryu J, Bahary J et al (2004) Whole brain radiation therapy with or without stereotactic radiosurgery boost for patients with one to three brain metastases: phase III results of the RTOG 9508 randomised trial. Lancet 363:1665–1672. https://doi.org/10.1016/S0140-6736(04)16250-8
Kocher M, Soffietti R, Abacioglu U, Villà S, Fauchon F, Baumert BG, Fariselli L, Tzuk-Shina T, Kortmann RD, Carrie C et al (2011) Adjuvant whole-brain radiotherapy versus observation after radiosurgery or surgical resection of one to three cerebral metastases: Results of the EORTC 22952–26001 study. J Clin Oncol 29:134–141. https://doi.org/10.1200/JCO.2010.30.1655
Reungwetwattana T, Nakagawa K, Cho BC, Cobo M, Cho EK, Bertolini A, Bohnet S, Zhou C, Lee KH, Nogami N et al (2018) CNS response to osimertinib versus standard epidermal growth factor receptor tyrosine kinase inhibitors in patients with untreated EGFR-mutated advanced non-small-cell lung cancer. J Clin Oncol 36:3290–3297. https://doi.org/10.1200/JCO.2018.78.3118
Long GV, Atkinson V, Lo S, Sandhu S, Guminski AD, Brown MP, Wilmott JS, Edwards J, Gonzalez M, Scolyer RA et al (2018) Combination nivolumab and ipilimumab or nivolumab alone in melanoma brain metastases: a multicentre randomised phase 2 study. Lancet Oncol 19:672–681. https://doi.org/10.1016/S1470-2045(18)30139-6
Rulli E, Legramandi L, Salvati L, Mandala M (2019) The impact of targeted therapies and immunotherapy in melanoma brain metastases: a systematic review and meta-analysis. Cancer. https://doi.org/10.1002/cncr.32375
Shepard MJ, Xu Z, Donahue J, Eluvathingal Muttikkal TJ, Cordeiro D, Hansen L, Mohammed N, Gentzler RD, Larner J, Fadul CE et al (2019) Stereotactic radiosurgery with and without checkpoint inhibition for patients with metastatic non-small cell lung cancer to the brain: a matched cohort study. J Neurosurg. https://doi.org/10.3171/2019.4.jns19822
Singh C, Qian JM, Yu JB, Chiang VL (2019) Local tumor response and survival outcomes after combined stereotactic radiosurgery and immunotherapy in non-small cell lung cancer with brain metastases. J Neurosurg. https://doi.org/10.3171/2018.10.jns181371
Rades D, Kueter JD, Veninga T, Gliemroth J, Schild SE (2009) Whole brain radiotherapy plus stereotactic radiosurgery (WBRT + SRS) versus surgery plus whole brain radiotherapy (OP + WBRT) for 1–3 brain metastases: results of a matched pair analysis. Eur J Cancer 45:400–404. https://doi.org/10.1016/j.ejca.2008.10.033
Rades D, Kueter JD, Pluemer A, Veninga T, Schild SE (2009) A matched-pair analysis comparing whole-brain radiotherapy plus stereotactic radiosurgery versus surgery plus whole-brain radiotherapy and a boost to the metastatic site for one or two brain metastases. Int J Radiat Oncol Biol Phys 73:1077–1081. https://doi.org/10.1016/j.ijrobp.2008.05.035
Rades D, Janssen S, Dziggel L, Blanck O, Bajrovic A, Veninga T, Schild SE (2017) A matched-pair study comparing whole-brain irradiation alone to radiosurgery or fractionated stereotactic radiotherapy alone in patients irradiated for up to three brain metastases. BMC Cancer 17:1–7. https://doi.org/10.1186/s12885-016-2989-3
Viani G, Godoi Da Silva L, Viana B, Rossi B, Suguikawa E, Zuliani G (2016) Whole brain radiotherapy and stereotactic radiosurgery for patients with recursive partitioning analysis i and lesions < 5 cm3: a matched pair analysis. J Cancer Res Ther 12:770–774. https://doi.org/10.4103/0973-1482.179092
Malouff T, Bennion NR, Verma V, Martinez GA, Balkman N, Bhirud A, Smith T, Lin C (2016) Which prognostic index is most appropriate in the setting of delayed stereotactic radiosurgery for brain metastases? Front Oncol 6:1–8. https://doi.org/10.3389/fonc.2016.00248
Badakhshi H, Engeling F, Budach V, Ghadjar P, Zschaeck S, Kaul D (2018) Are prognostic indices for brain metastases of melanoma still valid in the stereotactic era? Radiat Oncol 13:1–6. https://doi.org/10.1186/s13014-017-0951-4
Goldberg SB, Gettinger SN, Mahajan A, Chiang AC, Herbst RS, Sznol M, Tsiouris AJ, Cohen J, Vortmeyer A, Jilaveanu L et al (2016) Pembrolizumab for patients with melanoma or non-small-cell lung cancer and untreated brain metastases: early analysis of a non-randomised, open-label, phase 2 trial. Lancet Oncol 17:976–983. https://doi.org/10.1016/S1470-2045(16)30053-5
Kluger HM, Chiang V, Mahajan A, Zito CR, Sznol M, Tran T, Weiss SA, Cohen JV, Yu J, Hegde U et al (2019) Long-Term Survival of Patients With Melanoma With Active Brain Metastases Treated With Pembrolizumab on a Phase II Trial. J Clin Oncol 37:52–60. https://doi.org/10.1200/JCO.18.00204
Gaspar L, Scott C, Rotman M, Asbell S, Phillips T, Wasserman T, McKenna WG, Byhardt R (1997) Recursive partitioning analysis (RPA) of prognostic factors in three Radiation Therapy Oncology Group (RTOG) brain metastases trials. Int J Radiat Oncol Biol Phys 37:745–751. https://doi.org/10.1016/S0360-3016(96)00619-0
Sperduto PW, Berkey B, Gaspar LE, Mehta M, Curran W (2008) A new prognostic index and comparison to three other indices for patients with brain metastases: an analysis of 1,960 patients in the RTOG database. Int J Radiat Oncol Biol Phys 70:510–514. https://doi.org/10.1016/j.ijrobp.2007.06.074
Yamamoto M, Kawabe T, Higuchi Y, Sato Y, Nariai T, Watanabe S, Barfod BE, Kasuya H (2014) Validity of prognostic grading indices for brain metastasis patients undergoing repeat radiosurgery. World Neurosurg 82:1242–1249. https://doi.org/10.1016/j.wneu.2014.08.008
Farris M, McTyre ER, Cramer CK, Hughes R, Randolph DM, Ayala-Peacock DN, Bourland JD, Ruiz J, Watabe K, Laxton AW et al (2017) Brain metastasis velocity: a novel prognostic metric predictive of overall survival and freedom from whole-brain radiation therapy after distant brain failure following upfront radiosurgery alone. Int J Radiat Oncol Biol Phys 98:131–141. https://doi.org/10.1016/j.ijrobp.2017.01.201
Yamamoto M, Aiyama H, Koiso T, Watanabe S, Kawabe T, Sato Y, Higuchi Y, Kasuya H, Barfod BE (2019) Validity of a recently proposed Prognostic Grading Index, brain metastasis velocity, for patients with brain metastasis undergoing multiple radiosurgical procedures. Int J Radiat Oncol Biol Phys 103:631–637. https://doi.org/10.1016/j.ijrobp.2018.10.036
Fujimoto D, von Eyben R, Gibbs IC, Chang SD, Li G, Harsh GR, Hancock S, Fischbein N, Soltys SG (2018) Imaging changes over 18 months following stereotactic radiosurgery for brain metastases: both late radiation necrosis and tumor progression can occur. J Neurooncol 136:207–212. https://doi.org/10.1007/s11060-017-2647-x
Kohutek ZA, Yamada Y, Chan TA, Brennan CW, Tabar V, Gutin PH, Jonathan Yang T, Rosenblum MK, Ballangrud Å, Young RJ et al (2015) Long-term risk of radionecrosis and imaging changes after stereotactic radiosurgery for brain metastases. J Neurooncol 125:149–156. https://doi.org/10.1007/s11060-015-1881-3
Jagannathan J, Bourne TD, Schlesinger D, Yen CP, Shaffrey ME, Laws ER, Sheehan JP (2010) Clinical and pathological characteristics of brain metastasis resected after failed radiosurgery. Neurosurgery 66:208–217. https://doi.org/10.1227/01.NEU.0000359318.90478.69
Campos B, Neumann J-O, Hubert A, Adeberg S, El Shafie R, von Deimling A, Bendszus M, Debus J, Bernhardt D, Unterberg A (2020) Analysis of a surgical series of 21 cerebral radiation necroses. World Neurosurg. https://doi.org/10.1016/j.wneu.2020.02.005
Lohmann P, Kocher M, Ceccon G, Bauer EK, Stoffels G, Viswanathan S, Ruge MI, Neumaier B, Shah NJ, Fink GR et al (2018) Combined FET PET/MRI radiomics differentiates radiation injury from recurrent brain metastasis. NeuroImage Clin 20:537–542. https://doi.org/10.1016/j.nicl.2018.08.024
Peng L, Parekh V, Huang P, Lin DD, Sheikh K, Baker B, Kirschbaum T, Silvestri F, Son J, Robinson A et al (2018) Distinguishing true progression from radionecrosis after stereotactic radiation therapy for brain metastases with machine learning and radiomics. Int J Radiat Oncol Biol Phys 102:1236–1243. https://doi.org/10.1016/j.ijrobp.2018.05.041
Kim JM, Miller JA, Kotecha R, Xiao R, Juloori A, Ward MC, Ahluwalia MS, Mohammadi AM, Peereboom DM, Murphy ES et al (2017) The risk of radiation necrosis following stereotactic radiosurgery with concurrent systemic therapies. J Neurooncol 133:357–368. https://doi.org/10.1007/s11060-017-2442-8
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare they have no conflicts of interest relevant to the scope of this manuscript.
Ethical approval
All procedures and analyses performed in the present work were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments.
Informed consent
Ethics approval for the study and a waiver of written informed consent was granted by the Heidelberg University ethics committee on April 12th, 2018 (#S-172/2018). Patient confidentiality was maintained by anonymizing patient data to remove any identifying information.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
El Shafie, R.A., Celik, A., Weber, D. et al. A matched-pair analysis comparing stereotactic radiosurgery with whole-brain radiotherapy for patients with multiple brain metastases. J Neurooncol 147, 607–618 (2020). https://doi.org/10.1007/s11060-020-03447-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-020-03447-2