Abstract
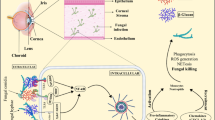
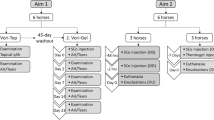
The aim of this study was to assess the efficacy of topical application of a liposomal formulation of itraconazole for the treatment of experimental keratitis with endophthalmitis caused by Aspergillus flavus. The liposomes were obtained by the lipid film hydration method followed by sonication. Adult female Wistar rats (weighing 200–220 g) were immunosuppressed by intraperitoneal injection of 150 mg/kg of cyclophosphamide 3 days before infection by exposure to the fungus A. flavus (107 spores/ml). Forty-eight hours later, the animals were treated with the liposomal formulation. For comparison, one group of animals (n = 6) was treated with the same drug not encapsulated. At the end of the experiment, the animals were evaluated for clinical signs and number of colony forming units (CFU/g), along with direct microscopic examination. The results indicated that the liposomal formulation of itraconazole has better antifungal activity than the unencapsulated drug in the treatment of fungal keratitis with endophthalmitis caused experimentally by A. flavus in Wistar rats.

Similar content being viewed by others
References
Hahn YH, Ahearn DG, Wilson LA. Comparative efficacy of amphotericin B, clotrimazole and itraconazole against Aspergillus spp. Mycopathologia. 1993;123:135–40.
Kalavathy CM, Parmar P, Kaliamurthy J, et al. Comparison of topical itraconazole 1% with topical natamycin 5% for the treatment of filamentous fungal keratitis. Cornea. 2005;24:449–52.
Ramos MM, Claros-B JA, Oviedo MAV, et al. Effect of the vehicle on the topical itraconazole efficacy for treating corneal ulcers caused by Aspergillus fumigatus. Clin Exp Ophthalmol. 2008;36:335–8.
Tang J, Wei H, Liu H, et al. Pharmacokinetics and biodistribution of itraconazole in rats and mice following intravenous administration in a novel liposome formulation. Drug Deliv. 2010;17:223–30.
Andrade CA, Correia MT, Coelho LC, Nascimento SC, Santos-Magalhães NS. Antitumor activity of Cratylia mollis lectin encapsulated into liposomes. Int J Pharm. 2004;278:435–45.
Parikh SK, Daves JB, Patel CN, Ramalingan B. Stability-indicating high-performance thin-layer chromatographic method for analysis of itraconazole in bulk drug and in pharmaceutical dosage form. Pharm Methods. 2011;2:88–94.
Clinical and Laboratory Standars Institute (CLSI). Reference method for broth dilution antifungal susceptibility testing of filamentous fungi; Approved standar second edition M38-A2, Wayne, PA, USA, 2008.
Henry CR, Flynn HW, Miller D, et al. Infectious keratitis progressing to endophthalmitis. Ophthalmology. 2012;119:2443–9.
Yavas GF, Ozturk F, Kusbeci T, et al. Antifungal efficacy of voriconazole, itraconazole and amphotericin B in experimental Fusarium solani keratitis. Graefes Arch Clin Exp Ophthalmol. 2008;246:275–9.
Prajna NV, Mascarenhas J, Krishnan T, et al. Comparison of natamycin and voriconazole for the treatment of fungal keratitis. Arch Ophthalmol. 2010;128:672–8.
Morand K, Bartoletti AC, Bochot A, et al. Liposomal amphotericin B eye drops to treat fungal keratitis: physico-chemical and formulation stability. Int J Pharm. 2007;344:150–3.
Mishara GP, Bagui M, Tamboli V, Mitra AK. Recent applications of liposomes in ophthalmic drug delivery. J Drug Deliv. 2011;2011:1–14.
Ebrahim S, Peyman GA, Lee PJ. Applications of liposomes in ophthalmology. Surv Ophthalmol. 2005;50:167–82.
Habib FS, Fouad EA, Rhaman MSA, Fathalla D. Liposome as an ocular delivery system of fluconazole: in vitro studies. Acta Ophthalmol. 2010;88:901–4.
Shibata N, Okawa Y. Structure of fungal cell wall polysaccharides. Jpn J Med Mycol. 2006;47:179–84.
Acknowledgments
This work was supported by the Pernambuco State Research Foundation (FACEPE) and National Council for Research Development (CNPq).
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Leal, A.F.G., Leite, M.C., Medeiros, C.S.Q. et al. Antifungal Activity of a Liposomal Itraconazole Formulation in Experimental Aspergillus flavus Keratitis with Endophthalmitis. Mycopathologia 179, 225–229 (2015). https://doi.org/10.1007/s11046-014-9837-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11046-014-9837-2