Abstract
Background
Tumor necrosis factor-alpha (TNF-α) is one of the crucial inflammatory factors in alveolar bone metabolism during the process of periodontitis. Autophagy is indispensable for proper osteoblast function. However, the effects of autophagy on osteogenic differentiation of human periodontal ligament stem cells (hPDLSCs) in inflammatory microenvironment and the underlying mechanisms remain to be clarified. The aim of the present study was to investigate whether autophagy participates in hPDLSCs differentiation after treated with TNF-α and explore the underlying mechanisms.
Methods and results
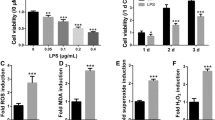
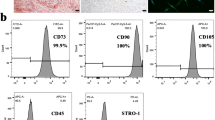
Characterizations of hPDLSCs were evaluated by Alizarin-red S staining, Oil red staining and flow cytometry. hPDLSCs were treated with various concentrations of TNF-α. Rapamycin or 3MA was used to achieve or inhibit autophagy activation. AKT signaling was inhibited using ARQ092. Cell proliferation was evaluated using Cell Counting Kit-8 (CCK8) assay. Real-time reverse transcriptase-polymerase chain reaction assay (RT-PCR), western blot, alkaline phosphatase (ALP) staining and Alizarin Red S staining were applied to evaluate levels of osteogenic differentiation and autophagy. CCK8 showed that low concentrations of TNF-α had no influence on cell proliferation, while high concentrations of TNF-α inhibited proliferation. Low concentrations of TNF-α promoted osteogenic differentiation and autophagy, while high concentrations of TNF-α inhibited osteogenic differentiation and autophagy in hPDLSCs. The levels of osteogenic differentiation in hPDLSCs were partly effected after co-incubation with 0.1 ng/mL TNF-α with 3MA or Rapamycin. ARQ092 enhanced 0.1 ng/mL TNF-α-induced ALP expression and mineral nodule formation.
Conclusion
Low concentrations of TNF-α promote hPDLSCs osteogenic differentiation by activation of autophagy via inhibition of AKT/mTOR signaling.






Similar content being viewed by others
References
Cunha-Cruz J, Hujoel PP, Kressin NR (2007) Oral health-related quality of life of periodontal patients. J Periodontal Res 42(2):169–176. https://doi.org/10.1111/j.1600-0765.2006.00930.x
Southerland JH, Taylor GW, Moss K, Beck JD, Offenbacher S (2006) Commonality in chronic inflammatory diseases: periodontitis, diabetes, and coronary artery disease. Periodontol 2000 40:130–143. https://doi.org/10.1111/j.1600-0757.2005.00138.x
Petersen PE, Baehni PC (2012) Periodontal health and global public health. Periodontol 2000 60(1):7–14. https://doi.org/10.1111/j.1600-0757.2012.00452.x
Wang HL, Greenwell H, Fiorellini J, Giannobile W, Offenbacher S, Salkin L et al (2005) Periodontal regeneration. J Periodontol 76(9):1601–1622. https://doi.org/10.1902/jop.2005.76.9.1601
Seo BM, Miura M, Gronthos S, Bartold PM, Batouli S, Brahim J et al (2004) Investigation of multipotent postnatal stem cells from human periodontal ligament. Lancet 364(9429):149–155. https://doi.org/10.1016/s0140-6736(04)16627-0
Zhu W, Liang M (2015) Periodontal ligament stem cells: current status, concerns, and future prospects. Stem Cells Int 2015:972313. https://doi.org/10.1155/2015/972313
Xie H, Liu H (2012) A novel mixed-type stem cell pellet for cementum/periodontal ligament-like complex. J Periodontol 83(6):805–815. https://doi.org/10.1902/jop.2011.110267
Soheilifar S, Amiri I, Bidgoli M, Hedayatipanah M (2016) Comparison of Periodontal ligament stem cells isolated from the Periodontium of Healthy Teeth and Periodontitis-Affected Teeth. J Dent (Tehran) 13(4):271–278
Zheng W, Wang S, Wang J, Jin F (2015) Periodontitis promotes the proliferation and suppresses the differentiation potential of human periodontal ligament stem cells. Int J Mol Med 36(4):915–922. https://doi.org/10.3892/ijmm.2015.2314
Kong X, Liu Y, Ye R, Zhu B, Zhu Y, Liu X et al (2013) GSK3beta is a checkpoint for TNF-alpha-mediated impaired osteogenic differentiation of mesenchymal stem cells in inflammatory microenvironments. Biochim Biophys Acta 1830(11):5119–5129. https://doi.org/10.1016/j.bbagen.2013.07.027
Tan J, Zhou L, Xue P, An Y, Luo L, Zhang R et al (2016) Tumor necrosis factor-alpha attenuates the osteogenic differentiation capacity of Periodontal Ligament Stem cells by activating PERK Signaling. J Periodontol 87(8):e159–e171. https://doi.org/10.1902/jop.2016.150718
Chen X, Hu C, Wang G, Li L, Kong X, Ding Y et al (2013) Nuclear factor-kappab modulates osteogenesis of periodontal ligament stem cells through competition with beta-catenin signaling in inflammatory microenvironments. Cell Death Dis 4:e510. https://doi.org/10.1038/cddis.2013.14
Glick D, Barth S, Macleod KF (2010) Autophagy: cellular and molecular mechanisms. J Pathol 221(1):3–12. https://doi.org/10.1002/path.2697
Jaber FA, Khan NM, Ansari MY, Al-Adlaan AA, Hussein NJ, Safadi FF (2019) Autophagy plays an essential role in bone homeostasis. J Cell Physiol 234(8):12105–12115. https://doi.org/10.1002/jcp.27071
Oliver L, Hue E, Priault M, Vallette FM (2012) Basal autophagy decreased during the differentiation of human adult mesenchymal stem cells. Stem Cells Dev 21(15):2779–2788. https://doi.org/10.1089/scd.2012.0124
Nollet M, Santucci-Darmanin S, Breuil V, Al-Sahlanee R, Cros C, Topi M et al (2014) Autophagy in osteoblasts is involved in mineralization and bone homeostasis. Autophagy 10(11):1965–1977. https://doi.org/10.4161/auto.36182
Pilli M, Arko-Mensah J, Ponpuak M, Roberts E, Master S, Mandell MA et al (2012) TBK-1 promotes autophagy-mediated antimicrobial defense by controlling autophagosome maturation. Immunity 37(2):223–234. https://doi.org/10.1016/j.immuni.2012.04.015
Harris J, Hartman M, Roche C, Zeng SG, O’Shea A, Sharp FA et al (2011) Autophagy controls IL-1beta secretion by targeting pro-IL-1beta for degradation. J Biol Chem 286(11):9587–9597. https://doi.org/10.1074/jbc.m110.202911
Yang Y, Huang Y, Li W (2021) Autophagy and its significance in periodontal disease. J Periodontal Res 56(1):18–26. https://doi.org/10.1111/jre.12810
Chen D, Liu J, Lu L, Huang Y, Wang Y, Wang M et al (2016) Emodin attenuates TNF-alpha-induced apoptosis and autophagy in mouse C2C12 myoblasts though the phosphorylation of akt. Int Immunopharmacol 34:107–113. https://doi.org/10.1016/j.intimp.2016.02.023
Wang XH, Zhu L, Hong X, Wang YT, Wang F, Bao JP et al (2016) Resveratrol attenuated TNF-alpha-induced MMP-3 expression in human nucleus pulposus cells by activating autophagy via AMPK/SIRT1 signaling pathway. Exp Biol Med (Maywood) 241(8):848–853. https://doi.org/10.1177/1535370216637940
An Y, Liu W, Xue P, Zhang Y, Wang Q, Jin Y (2016) Increased autophagy is required to protect periodontal ligament stem cells from apoptosis in inflammatory microenvironment. J Clin Periodontol 43(7):618–625. https://doi.org/10.1111/jcpe.12549
Wei W, An Y, An Y, Fei D, Wang Q (2018) Activation of autophagy in periodontal ligament mesenchymal stem cells promotes angiogenesis in periodontitis. J Periodontol 89(6):718–727. https://doi.org/10.1002/jper.17-0341
Dosseva-Panova VT, Popova CL, Panov VE (2014) Subgingival microbial profile and production of proinflammatory cytokines in chronic periodontitis. Folia Med (Plovdiv) 56(3):152–160. https://doi.org/10.2478/folmed-2014-0022
Shaker OG, Ghallab NA (2012) IL-17 and IL-11 GCF levels in aggressive and chronic periodontitis patients: relation to PCR bacterial detection. Mediators Inflamm 2012:174764. https://doi.org/10.1155/2012/174764
Liu H, Li D, Zhang Y, Li M (2018) Inflammation, mesenchymal stem cells and bone regeneration. Histochem Cell Biol 149(4):393–404. https://doi.org/10.1007/s00418-018-1643-3
Wang X, Tang Y, Xiao R (2022) Chemerin contributes to inflammatory responses and suppresses osteogenic differentiation in chronic periodontitis. Oral Dis. https://doi.org/10.1111/odi.14130
Algate K, Haynes DR, Bartold PM, Crotti TN, Cantley MD (2016) The effects of tumour necrosis factor-alpha on bone cells involved in periodontal alveolar bone loss; osteoclasts, osteoblasts and osteocytes. J Periodontal Res 51(5):549–566. https://doi.org/10.1111/jre.12339
Wang L, Zhang J, Wang C, Qi Y, Du M, Liu W et al (2017) Low concentrations of TNF-alpha promote osteogenic differentiation via activation of the ephrinB2-EphB4 signalling pathway. Cell Prolif 50(1). https://doi.org/10.1111/cpr.12311
Wang LM, Zhao N, Zhang J, Sun QF, Yang CZ, Yang PS (2018) Tumor necrosis factor-alpha inhibits osteogenic differentiation of pre-osteoblasts by downregulation of EphB4 signaling via activated nuclear factor-kappab signaling pathway. J Periodontal Res 53(1):66–72. https://doi.org/10.1111/jre.12488
Qin Z, Fang Z, Zhao L, Chen J, Li Y, Liu G (2015) High dose of TNF-alpha suppressed osteogenic differentiation of human dental pulp stem cells by activating the Wnt/beta-catenin signaling. J Mol Histol 46(4–5):409–420. https://doi.org/10.1007/s10735-015-9630-7
Ceccariglia S, Cargnoni A, Silini AR, Parolini O (2020) Autophagy: a potential key contributor to the therapeutic action of mesenchymal stem cells. Autophagy 16(1):28–37. https://doi.org/10.1080/15548627.2019.1630223
Chen Z, Jin T, Lu Y (2016) AntimiR-30b inhibits TNF-alpha mediated apoptosis and attenuated cartilage degradation through enhancing Autophagy. Cell Physiol Biochem 40(5):883–894. https://doi.org/10.1159/000453147
Levine B, Mizushima N, Virgin HW (2011) Autophagy in immunity and inflammation. Nature 469(7330):323–335. https://doi.org/10.1038/nature09782
Ugwu EO, Iferikigwe ES, Obi SN, Eleje GU, Ozumba BC (2018) Effectiveness of antenatal perineal massage in reducing perineal trauma and post-partum morbidities: a randomized controlled trial. J Obstet Gynaecol Res 44(7):1252–1258. https://doi.org/10.1111/jog.13640
Chagin AS (2016) Effectors of mTOR-autophagy pathway: targeting cancer, affecting the skeleton. Curr Opin Pharmacol 28:1–7. https://doi.org/10.1016/j.coph.2016.02.004
Zheng L, Wang W, Ni J, Mao X, Song D, Liu T et al (2017) Role of autophagy in tumor necrosis factor-alpha-induced apoptosis of osteoblast cells. J Investig Med 65(6):1014–1020. https://doi.org/10.1136/jim-2017-000426
Chen L, Bao J, Yang Y, Wang Z, Xia M, Tan J et al (2020) Autophagy was involved in tumor necrosis factor-alpha-inhibited osteogenic differentiation of murine calvarial osteoblasts through Wnt/beta-catenin pathway. Tissue Cell 67:101401. https://doi.org/10.1016/j.tice.2020.101401
Xie S, Chen M, Yan B, He X, Chen X, Li D (2014) Identification of a role for the PI3K/AKT/mTOR signaling pathway in innate immune cells. PLoS ONE 9(4):e94496. https://doi.org/10.1371/journal.pone.0094496
Cheng Y, Huang L, Wang Y, Huo Q, Shao Y, Bao H et al (2019) Strontium promotes osteogenic differentiation by activating autophagy via the the AMPK/mTOR signaling pathway in MC3T3E1 cells. Int J Mol Med 44(2):652–660. https://doi.org/10.3892/ijmm.2019.4216
Lu DG, Lu MJ, Yao SH, Lin JJ, Luo S, Wei JH et al (2021) Long non-coding RNA TUG1 promotes the osteogenic differentiation of bone marrow mesenchymal stem cells by regulating the AMPK/mTOR/autophagy pathway. Biomed Res 42(6):239–246. https://doi.org/10.2220/biomedres.42.239
Zhao B, Peng Q, Poon EHL, Chen F, Zhou R, Shang G et al (2021) Leonurine promotes the osteoblast differentiation of rat BMSCs by activation of Autophagy via the PI3K/Akt/mTOR pathway. Front Bioeng Biotechnol 9:615191. https://doi.org/10.3389/fbioe.2021.615191
Funding
This work was supported by Shandong Provincial Natural Science Foundation of China (No. ZR2019BH081).
Author information
Authors and Affiliations
Contributions
Wang Limei and Qi Yuping contributed to the study conception and design. All authors contributed to material preparation, data collection and analysis. The first draft of the manuscript was written by Wang Limei and Qi Yuping, and all authors commented on previous of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
No competing interests declared.
Ethics approval
Written informed consent was given by the tooth donors and by the parents/legally authorized representatives of the minor subjects who donated teeth. Approval was granted by the Ethics Committee of Qilu Hospital of Shandong University (Date:2020.09.25/ No. KYLL-202008-148).
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yuping, Q., Yijun, L. & Limei, W. Low concentrations of tumor necrosis factor-alpha promote human periodontal ligament stem cells osteogenic differentiation by activation of autophagy via inhibition of AKT/mTOR pathway. Mol Biol Rep 50, 3329–3339 (2023). https://doi.org/10.1007/s11033-022-08173-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-022-08173-8