Abstract
Background
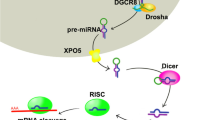
Micro RNAs (miRNAs) are small non-coding RNAs known as essential regulators of cell–cell communication. Recent studies have revealed that miRNAs are secreted by a blastocyst in culture media. We hypothesized that endometrial epithelial cells take up embryo-derived miRNAs as well as other soluble factors and regulate their receptivity-related gene expression.
Methods and results
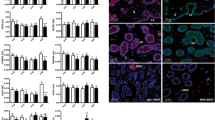
Blastocyst culture media (BCM) were collected from the individually cultured embryos, while human endometrial epithelial cells (HEECs) were collected from healthy fertile volunteers. To evaluate the effect of BCM on the endometrial receptivity gene expression, HEECs were co-cultured with implanted BCM, non-implanted BCM, and a control culture medium. After determining altered gene expression in the HEECs, the miRNAs-related genes through bioinformatics databases were identified and evaluated in the BCM. Co-culture of primary HEECs with BCM significantly stimulated the expression levels of VEGFA, HBEGF, HOXA10, and LIF in the implanted group compared with non-implanted and control groups. The fold changes of miR-195 significantly diminished in the implanted BCM group compared with the non-implanted BCM group. Reduced fold changes of miR‐29b, 145 and increased miR-223 were also observed in the implanted BCM group compared with the non-implanted ones.
Conclusion
miRNAs could function as potential gene expression regulators during implantation. These molecules are secreted by human blastocyst, taken up by endometrial epithelial cells, and cause a change in the endometrial function. We found that BCMs can be effective in implantation process by stimulating related receptivity gene expression.


Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article.
References
Tan Q et al (2020) MicroRNAs in small extracellular vesicles indicate successful embryo implantation during early pregnancy. Cells 9(3):645
Quenby S, Brosens JJ (2013) Human implantation: a tale of mutual maternal and fetal attraction. Biol Reprod 88(3):1–2
Luddi A et al (2021) Emerging role of embryo secretome in the paracrine communication at the implantation site: a proof of concept. Fertil Steril 115(4):1054–1062
Haouzi D et al (2011) Transcriptome analysis reveals dialogues between human trophectoderm and endometrial cells during the implantation period. Hum Reprod 26(6):1440–1449
Wang H et al (2018) Correlation of IL-1 and HB-EGF with endometrial receptivity. Exp Ther Med 16(6):5130–5136
Guo X et al (2021) Role of vascular endothelial growth factor (VEGF) in human embryo implantation: clinical implications. Biomolecules 11(2):253
Bi Y et al (2022) HOXA10 improves endometrial receptivity by upregulating E-cadherin. Biol Reprod 106(5):992–999
Whitby S, Zhou W, Dimitriadis E (2020) Alterations in epithelial cell polarity during endometrial receptivity: a systematic review. Front Endocrinol 11:596324
Fukui Y et al (2022) Uterine receptivity is reflected by LIF expression in the Cervix. Reproductive Sci 29(5):1457–1462
Edgell TA et al (2018) Assessment of potential biomarkers of pre-receptive and receptive endometrium in uterine fluid and a functional evaluation of the potential role of CSF3 in fertility. Cytokine 111:222–229
Wu F et al (2018) Decreased MUC1 in endometrium is an independent receptivity marker in recurrent implantation failure during implantation window. Reprod Biol Endocrinol 16(1):1–7
Rani V, Sengar RS (2022) Biogenesis and mechanisms of microRNA-mediated gene regulation. Biotechnol Bioeng 119(3):685–692
Cuman C et al (2015) Human blastocyst secreted microRNA regulate endometrial epithelial cell adhesion. EBioMedicine 2(10):1528–1535
Mouillet J-F et al (2015) MicroRNAs in placental health and disease. Am J Obstet Gynecol 213(4):S163–S172
Valadi H et al (2007) Exosome-mediated transfer of mRNAs and microRNAs is a novel mechanism of genetic exchange between cells. Nat Cell Biol 9(6):654–659
Nahand JS et al (2020) Exosomal microRNAs: novel players in cervical cancer. Epigenomics 12(18):1651–1660
Huang T et al (2019) The roles of extracellular vesicles in gastric cancer development, microenvironment, anti-cancer drug resistance, and therapy. Mol Cancer 18(1):1–11
Berkhout RP et al (2020) High-quality human preimplantation embryos stimulate endometrial stromal cell migration via secretion of microRNA hsa-miR-320a. Hum Reprod 35(8):1797–1807
Rosenbluth EM et al (2014) Human embryos secrete microRNAs into culture media—a potential biomarker for implantation. Fertil Steril 101(5):1493–1500
Fang F et al (2021) MicroRNAs secreted by human embryos could be potential biomarkers for clinical outcomes of assisted reproductive technology. J Adv Res 31:25–34
Capalbo A et al (2016) MicroRNAs in spent blastocyst culture medium are derived from trophectoderm cells and can be explored for human embryo reproductive competence assessment. Fertil Steril 105(1):225–235e3
Marwood M et al (2009) Interleukin-11 and leukemia inhibitory factor regulate the adhesion of endometrial epithelial cells: implications in fertility regulation. Endocrinology 150(6):2915–2923
Cuman C et al (2013) Preimplantation human blastocysts release factors that differentially alter human endometrial epithelial cell adhesion and gene expression relative to IVF success. Hum Reprod 28(5):1161–1171
Sugino N et al (2002) Expression of vascular endothelial growth factor (VEGF) and its receptors in human endometrium throughout the menstrual cycle and in early pregnancy. Reprod Cambridge 123(3):379–387
Torry DS et al (1996) Vascular endothelial growth factor expression in cycling human endometrium. Fertil Steril 66(1):72–80
Hannan N et al (2011) Analysis of fertility-related soluble mediators in human uterine fluid identifies VEGF as a key regulator of embryo implantation. Endocrinology 152(12):4948–4956
Sadekova ON et al (2015) Luteal phase defect is associated with impaired VEGF mRNA expression in the secretory phase endometrium. Reprod Biol 15(1):65–68
Das SK et al (1994) Heparin-binding EGF-like growth factor gene is induced in the mouse uterus temporally by the blastocyst solely at the site of its apposition: a possible ligand for interaction with blastocyst EGF-receptor in implantation. Development 120(5):1071–1083
Yoo HJ, Barlow DH, Mardon HJ (1997) Temporal and spatial regulation of expression of heparin-binding epidermal growth factor‐like growth factor in the human endometrium: a possible role in blastocyst implantation. Dev Genet 21(1):102–108
Lessey BA et al (2002) Regulated expression of heparin-binding EGF‐like growth factor (HB‐EGF) in the human endometrium: a potential paracrine role during implantation. Mol Reprod Dev 62(4):446–455
Satokata I, Benson G, Maas R (1995) Sexually dimorphic sterility phenotypes in Hoxa lO-deficient mice. Nature 374(6521):460–463
Taylor HS et al (1998) HOXA10 is expressed in response to sex steroids at the time of implantation in the human endometrium. J Clin Investig 101(7):1379–1384
Bagot CN, Kliman HJ, Taylor HS (2001) Maternal Hoxa10 is required for pinopod formation in the development of mouse uterine receptivity to embryo implantation. Dev Dyn 222(3):538–544
Sakkas D et al (2003) A soluble molecule secreted by human blastocysts modulates regulation of HOXA10 expression in an epithelial endometrial cell line. Fertil Steril 80(5):1169–1174
Shuya LL et al (2011) Leukemia inhibitory factor enhances endometrial stromal cell decidualization in humans and mice. PLoS ONE 6(9):e25288
Song H et al (2000) Dysregulation of EGF family of growth factors and COX-2 in the uterus during the preattachment and attachment reactions of the blastocyst with the luminal epithelium correlates with implantation failure in LIF-deficient mice. Mol Endocrinol 14(8):1147–1161
Dimitriadis E et al (2009) Local regulation of implantation at the human fetal-maternal interface. Int J Dev Biol 54(2–3):313–322
Aghajanova L (2004) Leukemia inhibitory factor and human embryo implantation. Ann N Y Acad Sci 1034(1):176–183
Stewart CL et al (1992) Blastocyst implantation depends on maternal expression of leukaemia inhibitory factor. Nature 359(6390):76–79
Surveyor GA et al (1995) Expression and steroid hormonal control of Muc-1 in the mouse uterus. Endocrinology 136(8):3639–3647
DeSouza MM et al (1998) Reduction of mucin-1 expression during the receptive phase in the rat uterus. Biol Reprod 58(6):1503–1507
Bowen JA, Bazer FW, Burghardt RC (1996) Spatial and temporal analyses of integrin and Muc-1 expression in porcine uterine epithelium and trophectoderm in vivo. Biol Reprod 55(5):1098–1106
Hild-Petito S et al (1996) Mucin (Muc-1) expression is differentially regulated in uterine luminal and glandular epithelia of the baboon (Papio anubis). Biol Reprod 54(5):939–947
DeSouza MM et al (2000) MUC1/episialin: a critical barrier in the female reproductive tract. J Reprod Immunol 45(2):127–158
Wang R et al (2013) MicroRNA-195 suppresses angiogenesis and metastasis of hepatocellular carcinoma by inhibiting the expression of VEGF, VAV2, and CDC42. Hepatology 58(2):642–653
Caramuta S et al (2013) Clinical and functional impact of TARBP2 over-expression in adrenocortical carcinoma. Endocrine-related Cancer 20(4):551–564
Zhu X-m et al (2009) Differential expression profile of microRNAs in human placentas from preeclamptic pregnancies vs normal pregnancies. Am J Obstet Gynecol 200(6):661. e1–661. e7
Bai Y et al (2012) Downregulated miR-195 detected in preeclamptic placenta affects trophoblast cell invasion via modulating ActRIIA expression. PLoS ONE 7(6):e38875
Bai X, Zheng C, Ren N (2019) Trophoblast proliferation, migration, and invasion is regulated by the miR-195/EGFR signaling pathway in recurrent spontaneous abortion patients. bioRxiv. https://doi.org/10.1101/630590
Choudhary A et al (2018) Identification of miR-29b targets using 3-cyanovinylcarbazole containing mimics. RNA 24(4):597–608
Rarani FZ, Borhani F, Rashidi B (2018) Endometrial pinopode biomarkers: molecules and microRNAs. J Cell Physiol 233(12):9145–9158
Wang X et al (2022) miRNA-29 aggravates myocardial infarction via inhibiting the PI3K/mTOR/HIF1α/VEGF pathway. Aging 14(7):3129
Revel A et al (2011) MicroRNAs are associated with human embryo implantation defects. Hum Reprod 26(10):2830–2840
Shekibi M et al (2022) Progesterone suppresses podocalyxin partly by up-regulating miR-145 and miR-199 in human endometrial epithelial cells to enhance receptivity in in-vitro models. Mol Hum Reprod. https://doi.org/10.1093/molehr/gaac034
Dong X et al (2016) MicroRNA-223-3p suppresses leukemia inhibitory factor expression and pinopodes formation during embryo implantation in mice. Am J Transl Res 8(2):1155
Acknowledgements
The authors would like to thank the Shahid Akbarabadi Clinical Research Development Unit (ShACRDU), Iran University of Medical Sciences, Tehran, Iran for cooperating throughout the study. This study was financed by Iran University of Medical Sciences (Grant No. 97-01-208-33115).
Funding
This study was financed by Iran University of Medical Sciences (Grant No. 33115).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
11033_2022_8121_MOESM2_ESM.tif
Supplementary file2 (TIF 832.5 kb)—Supplementary Fig. 2 Primary endometrial glandular epithelium cell culture. Representative endometrial glandular epithelium at (A) ×100, (B) ×100, (C) ×200 and (D) ×200 magnification. Black arrows indicate glandular epithelium cells.
11033_2022_8121_MOESM3_ESM.tif
Supplementary file3 (TIF 171.6 kb)—Supplementary Fig. 3 Endometrial cell purity. Purified populations of endometrial epithelial cells were stained for the intracellular epithelial and mesenchymal markers cytokeratin and vimentin, respectively. Flow cytometry histograms present data in blue for cells stained with vimentin and cytokeratin, and in red for the cognate isotype control.
11033_2022_8121_MOESM4_ESM.tif
Supplementary file4 (TIF 53.2 kb)—Supplementary Fig. 4 Target genes and related microRNAs were selected according to the miRTargetLink 2.0.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Eivazi, S., Tanhaye Kalate Sabz, F., Amiri, S. et al. MiRNAs secreted by human blastocysts could be potential gene expression regulators during implantation. Mol Biol Rep 50, 1375–1383 (2023). https://doi.org/10.1007/s11033-022-08121-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-022-08121-6