Abstract
Background and purpose
Nonmuscle myosin heavy chain IIA, played an essential role in the promotion of tight junction injury in vascular endothelial cells under oxygen glucose deprivation condition. Rat microvascular endothelial cells had been confirmed to have the susceptibility to ox-LDL stimulation under OGD condition. We proposed the hypothesis that lipid metabolic reprogramming might be the root cause for damage to RBMCs tight junction.
Methods
Untargeted shotgun and targeted lipid metabolomics mass spectrometry approaches combined with principal component analysis was applied to better define the lipids contributing to the variance observed between control and different OGD time. The protein expression of tight junction of RBMCs: occludin, claudin-5, and ZO-1 were detected with immunofluorescence staining and western blot. The proof of the interaction between NMMHC IIA and SREBP1 was investigated via GST-pull down, while their specific binding fragments were also confirmed. The regulation mechanism of NMMHC IIA on SREBP1 was investigated to explore downstream regulatory signaling pathways.
Results
Untargeted and targeted shotgun lipidomics data revealed that OGD might be the conditional factor in reshaping lipid components. Mechanistic studies showed that with the increase of OGD time, PCA analysis of lipidomics obtained from RBMCs indicated their specificity in reshaping lipid components, while ≥80% major lipid components phospholipids and sphingolipids transferred from phospholipids, sphingolipids, and neutral lipids, of which neutral lipids taken the largest proportion with OGD time course. Perturbing reprogramming of lipid composition was less susceptible to OGD condition via knockdown of NMMHC IIA of vascular endothelial cells. Knockdown of NMMHC IIA could promote tight junction defense to OGD condition. NMMHC IIA could directly bind with SREBP1, then could affect sterol regulatory element binding protein-1 to adjust lipid metabolize reprogramming of RBMCs.
Conclusions
Mechanistic studies showed that perturbing reprogramming of lipid composition could enhance tight junction damage, which was mediated by the opposing effects of NMMHC IIA.





Similar content being viewed by others
References
Lv YN, Liu W, Ruan ZH, Xu ZX, Fu LS (2019) Myosin IIA regulated tight junction in oxygen glucose deprivated brain endothelial cells via activation of TLR4/PI3K/Akt/JNK1/2/14-3-3ε/NF-κB/MMP9 signal transduction pathway. Cell Mol Neurobiol 39(2):301–319. https://doi.org/10.1007/s10571-019-00654-y
Lv YN, Fu LS (2018) The potential mechanism for Hydroxysafflor yellow A attenuating blood-brain barrier dysfunction via tight junction signaling pathways excavated by an integrated serial affinity chromatography and shotgun proteomics analysis approach. Neurochem Int 112:38–48. https://doi.org/10.1016/j.neuint.2017.10.012
Lv YN, Fu LS, Qian YS (2018) Effects of circulating microvesicles containing microrNA-27a on blood brain barrier tight junction injury of ischemia stroke mice. Chinese Pharmacol Bullet 34(6): 814–819. (in Chinese).
van Dongen MME, Aarnio K, Martinez-Majander N, Pirinen J, Sinisalo J, Lehto M, Kaste M, Tatlisumak T, de Leeuw FE, Putaala J (2019) Use of statins after ischemic stroke in young adults and its association with long-term outcome. Stroke 50(12):3385–3392. https://doi.org/10.1161/STROKEAHA.119.026992
Sun Y, Cui FF, Li DM, Li H, Qiu HL, Li YL, Shi QY (2020) The expression levels of ox-LDL, hs-CRP, Hcy, FIB in patients with acute cerebral infarction and their correlation carotid artery stenosis. Chinese J Gerontol 40(2):250–254. (in Chinese). https://doi.org/10.3969/j.issn.1005-9202.2020.02.008.
Chen XY, Peng XP, Fu LS, Lv YN (2017) Susceptibility and mechanism of brain microvascular endothelial cells injury with ox-LDL stimulation under oxygen-glucose deprivation condition. J Clin Cardiol 33(11): 1111–1115. (in Chinese). https://doi.org/10.13201/j.issn.1001-1439.2017.11.02
Todorović Z, Đurašević S, Stojković M, Grigorov I, Pavlović S, Jasnić N, Tosti T, Macut JB, Thiemermann C, Đorđević J (2021) Lipidomics provides new insight into pathogenesis and therapeutic targets of the ischemia-reperfusion injury. Int J Mol Sci 22(6):2798. https://doi.org/10.3390/ijms22062798
Pfisterer SG, Gateva G, Horvath P, Pirhonen J, Salo VT, Karhinen L, Varjosalo M, Ryhänen SJ, Lappalainen P, Ikonen E (2017) Role for formin-like 1-dependent acto-myosin assembly in lipid droplet dynamics and lipid storage. Nat Commun 31:14858. https://doi.org/10.1038/ncomms14858
Bai M, Shu K, Li K, Zhang G, Jin Z, He F, Hermjakob H, Zhu Y (2019) iProX: an integrated proteome resource. Nucleic Acids Res 47(D1):D1211–D1217. https://doi.org/10.1093/nar/gky869
YN Lv, Fu LS, Li YM, Wen JH, Wei XH, Yisong Qian YS (2018) Microvesicles derived from LPS-induced microglia aggravate the injury of tight junction in rat brain microvascular endothelial cells under oxygen-glucose deprivation. Chin J Cell Mol Immunol 34(3):211–217. (in Chinese). https://doi.org/10.13423/j.cnki.cjcmi.008561.
Hsieh WY, Zhou QD, York AG, Williams KJ, Scumpia PO, Kronenberger EB, Hoi XP, Su BL, Chi X, Bui VL, Khialeeva E, Kaplan A, Son YM, Divakaruni AS, Sun J, Smale ST, Flavell RA, Bensinger SJ (2020) Toll-like receptors induce signal-specific reprogramming of the macrophage lipidome. Cell Metab 32(1):128–143. https://doi.org/10.1016/j.cmet.2020.05.003
Díaz-Coránguez M, Lin CM, Liebner S, Antonetti DA (2020) Norrin restores blood-retinal barrier properties after vascular endothelial growth factor-induced permeability. J Biol Chem 295(14):4647–4660. https://doi.org/10.1074/jbc.RA119.011273
Zhou Y, Fang XL, Zhang Y, Feng YN, Wang SS (2020) miR-20a-5p promotes pulmonary artery smooth muscle cell proliferation and migration by targeting ABCA1. J Biochem Mol Toxicol 34(12):e22589. https://doi.org/10.1002/jbt.22589
Chen M, Li W, Zhang Y, Yang JY (2018) MicroRNA-20a protects human aortic endothelial cells from Ox-LDL-induced inflammation through targeting TLR4 and TXNIP signaling. Biomed Pharmacother 103:191–197. https://doi.org/10.1016/j.biopha.2018.03.129
Li Y, Zheng L, Li YH, Wang YL, Li L (2020) MiR-20a ameliorates diabetic angiopathy in streptozotocin-induced diabetic rats by regulating intracellular antioxidant enzymes and VEGF. Eur Rev Med Pharmacol Sci 24(4):1948–1955. https://doi.org/10.26355/eurrev_202002_20397
Scioli MG, Storti G, D’Amico F, Guzmán RR, Centofanti F, Doldo E, Miranda EMC, Orlandi A (2020) Oxidative stress and new pathogenetic mechanisms in endothelial dysfunction: potential diagnostic biomarkers and therapeutic targets. J Clin Med 9(6):1995. https://doi.org/10.3390/jcm9061995
Ashraf APK, Gerke V (2021) Plasma membrane wound repair is characterized by extensive membrane lipid and protein rearrangements in vascular endothelial cells. Biochim Biophys Acta Mol Cell Res 1868(7):118991. https://doi.org/10.1016/j.bbamcr.2021.118991
Meeusen JW, Donato LJ, Kopecky SL, Vasile VC, Jaffe AS, Laaksonen R (2020) Ceramides improve atherosclerotic cardiovascular disease risk assessment beyond standard risk factors. Clin Chim Acta 511:138–142. https://doi.org/10.1016/j.cca.2020.10.005
Naseh M, Vatanparast J, Rafati A, Bayat M, Haghani M (2021) The emerging role of FTY720 as a sphingosine 1-phosphate analog for the treatment of ischemic stroke: The cellular and molecular mechanisms. Brain Behav 10:e02179. https://doi.org/10.1002/brb3.2179
Lonati E, Corsetto PA, Montorfano G, Zava S, Carrozzini T, Brambilla A, Botto L, Palestini P, Rizzo AM, Bulbarelli A (2019) Lipid reshaping and lipophagy are induced in a modeled ischemia-reperfusion injury of blood brain barrier. Int J Mol Sci 20(15):3752. https://doi.org/10.3390/ijms20153752
Azzu V, Vacca M, Kamzolas I, Hall Z, Leslie J, Carobbio S, Virtue S, Davies SE, Lukasik A, Dale M, Bohlooly-Y M, Acharjee A, Lindén D, Bidault G, Petsalaki E, Griffin JL, Oakley F, Allison MED, Vidal-Puig A (2021) Suppression of insulin-induced gene 1 (INSIG1) function promotes hepatic lipid remodelling and restrains NASH progression. Mol Metab 48:101210. https://doi.org/10.1016/j.molmet.2021.101210
Lai TW, Zhang S, Wang ST (2014) Excitotoxicity and stroke: identifying novel targets for neuroprotection. Prog Neurobiol 115:157–188. https://doi.org/10.1016/j.pneurobio.2013.11.006
Taghibiglou C, Martin HGS, Lai TW, Cho T, Prasad S, Kojic L, Lu J, Liu Y, Lo E, Zhang S, Wu JZZ, Li YP, Wen YH, Imm JH, Cynader MS, Wang YT (2009) Role of NMDA receptor-dependent activation of SREBP1 in excitotoxic and ischemic neuronal injuries. Nat Med 15(12):1399–1406. https://doi.org/10.1038/nm.2064
Funding
This study was funded by National Natural Science Foundation of China (No: 82100417, 81760094); The Foundation of Jiangxi Provincial Department of Science and Technology Project (No. 20202ACBL206001, No. 20212BAB206022); Youth Project of Jiangxi Provincial Department of Education (No: GJJ200217). The funder had no role in the study design, data collection and analysis, decision to publish or preparation of the manuscript. All funding body had no role in the design of the study and collection, analysis, and interpretation of data and in writing the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Author Yanni Lv declares that she has no conflict of interest. Author Daojun Hong declares that he has no conflict of interest. Author Longsheng Fu declares that he has no conflict of interest. Author Yisong Qian declares that she has no conflict of interest.
Ethical approval
All procedures performed in Ethical approval: This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Not applicable.
Research involving human and animal rights
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
11033_2021_7092_MOESM2_ESM.tif
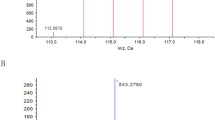
Supplementary file2—Supplement Figure 1. Lipidomics with high fold change via principal component analysis. A. Gravel figure. B. Load diagram. (TIF 808 kb)
11033_2021_7092_MOESM3_ESM.tif
Supplementary file3—Supplement Figure 2. Distinct lipid analysis of the vascular endothelial cells with different OGD time course. A. ox-LDL thermograph. B. Cholesterol ester thermograph. C. Fatty acid thermograph. D. Phosphatidic acid thermograph. E. Ceramides thermograph. F. Principal component analysis diagram. (TIF 1640 kb)
11033_2021_7092_MOESM4_ESM.tif
Supplementary file4—Supplement Figure 3. The protein expression change of tight junction proteins with different OGD time course. A Immunofluorescence staining. B. Western blot. RBECs with 1×105 cells/mL and then treated at OGD time 0 (control), 1, 3, 6, 12, and 24 h. The extracted proteins of RBECs were subjected to western blot assay. The extracted proteins of RBECs were subjected to Immunofluorescence staining or western blot assay. Western blot histogram were shown as the means±SD of four independent experiments. **P< 0.01 versus control RBECs. (TIF 1079 kb)
11033_2021_7092_MOESM5_ESM.tif
Supplementary file5—Supplement Figure 4. Distinct lipid analysis of the vascular endothelial cells after transfection with siRNA-MYH9 under OGD condition. A. ox-LDL thermograph. B. Cholesterol ester thermograph. C. Fatty acid thermograph. D. Phosphatidic acid thermograph. E. Ceramides thermograph. F. Principal component analysis diagram. (TIF 1885 kb)
Rights and permissions
About this article
Cite this article
Lv, Y., Hong, D., Fu, L. et al. NMMHC IIA triggered lipid metabolize reprogramming resulting in vascular endothelial cellular tight junction injury. Mol Biol Rep 49, 2805–2819 (2022). https://doi.org/10.1007/s11033-021-07092-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-021-07092-4