Abstract
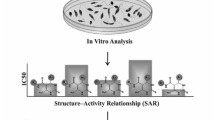
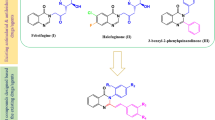
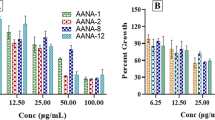
Due to the lack of effective vaccine(s) against leishmania and also pharmacokinetics issues of current drugs, it is necessary to discover new antileishmanial agents. Within this particular study, a series of novel 1-aryl/alkyl-3-benzoyl/cyclopropanoyl thiourea derivatives were synthesized (yields 69–84%) and evaluated as antileishmanial compounds (1–11). Synthetic derivatives were subjected to in vitro antileishmanial assessment against Leishmania major promastigotes by colorimetric MTT assay. Compounds 3 (IC50 38.54 µg/mL), 5 (IC50 84.75 µg/mL) and 10 (IC50 70.31 µg/mL) exhibited higher activities after 48 h but were less potent than amphotericin B (IC50 0.19 µg/mL). Antileishmanial activities indicated priority of 5-methyl-4-phenyl thiazole over furyl methyl substituents and 4-phenyl thiazole on thiourea nitrogen. N-myristoyltransferase (NMT) was selected as a validated L. major target for molecular docking studies. In silico results indicated the contribution of hydrophobic, π-stacking and H-bond interactions in binding to target. Most of the synthesized derivatives had lower binding affinities to human NMT (hNMT) than leishmanial enzyme. Docking conformations of top-ranked selective binders (compounds 3 and 5) were subjected to 50 ns MD simulations inside L. major HMT (LmNMT) active site. MD trajectories were used to extract RMSD, RMSF, Rg and durability of intramolecular/intermolecular H-bonds of the complex. It was observed that compound 3 escaped from LmNMT binding site during simulation period and no stable complex could be envisaged. Unlike 3, compound 5 attained stable binding conformation with converged stability parameters. Although mechanistic details for antileishmanial effects of synthesized derivatives are to be explored, current results may be implicated in further structure-guided approach toward potent antileishmanial agents.
Graphical abstract











Similar content being viewed by others
Data availability
All the data are available and can be offered on request.
Code availability
Not applicable.
References
WHO (n.d.) Neglected tropical diseases. World Health Organization. https://www.who.int/neglected_diseases/diseases/en. Accessed 10 Oct 2020
The Lancet (2019) 2020: A crucial year for neglected tropical diseases. Lancet 394(10215):2126. https://doi.org/10.1016/S0140-6736(19)33070-3
Tzani M, Barrasa A, Vakali A, Georgakopoulou T, Mellou K, Pervanidou D (2021) Surveillance data for human leishmaniasis indicate the need for a sustainable action plan for its management and control, Greece, 2004 to 2018. Euro Surveill 26(18):2000159. https://doi.org/10.2807/1560-7917.ES.2021.26.18.2000159
Mukhopadhyay D, Dalton JE, Kaye PM, Chatterjee M (2014) Post kala-azar dermal leishmaniasis: an unresolved mystery. Trends Parasitol 30:65–74. https://doi.org/10.1016/j.pt.2013.12.004
Ortalli M, Ilari A, Colotti G, De Ionna I, Battista T, Bisi A, Gobbi S, Rampa A, Di Martino RMC, Gentilomi GA, Varani S, Belluti F (2018) Identification of chalcone-based antileishmanial agents targeting trypanothione reductase. Eur J Med Chem 152:527–541. https://doi.org/10.1016/j.ejmech.2018.04.057
Bamorovat M, Sharifi I, Tavakoli Oliaee R, Jafarzadeh A, Khosravi A (2021) Determinants of unresponsiveness to treatment in cutaneous leishmaniasis: a focus on anthroponotic form due to Leishmania tropica. Front Microbiol 12:1143. https://doi.org/10.3389/fmicb.2021.638957
Croft SL, Coombs GH (2003) Leishmaniasis—current chemotherapy and recent advances in the search for novel drugs. Trends Parasitol 19:502–508. https://doi.org/10.1016/j.pt.2003.09.008
Mitropoulos P, Konidas P, Durkin-Konidas M (2010) New world cutaneous leishmaniasis: updated review of current and future diagnosis and treatment. J Am Acad Dermatol 63:309–322. https://doi.org/10.1016/j.jaad.2009.06.088
Gervazoni LFO, Barcellos GB, Ferreira-Paes T, Almeida-Amaral EE (2020) Use of natural products in leishmaniasis chemotherapy: an overview. Front Chem 8:1031. https://doi.org/10.3389/fchem.2020.579891
Razzaghi-Asl N, Sepehri S, Ebadi A, Karami P, Nejatkhah N, Johari-Ahar M (2019) Insights into the current status of privileged N-heterocycles as antileishmanial agents. Mol Divers 24:525–569. https://doi.org/10.1007/s11030-019-09953-4
Ronchetti R, Moroni G, Carotti A, Gioiello A, Camaioni E (2021) Recent advances in urea- and thiourea-containing compounds: focus on innovative approaches in medicinal chemistry and organic synthesis. RSC Med Chem 12:1046–1064. https://doi.org/10.1039/D1MD00058F
Upadhayaya RS, Dixit SS, Földesi A, Chattopadhyaya J (2013) New antiprotozoal agents: their synthesis and biological evaluations. Bioorg Med Chem Lett 23(9):2750–2758. https://doi.org/10.1016/j.bmcl.2013.02.054
Díaz M, de Lucio H, Moreno E, Espuelas S, Aydillo C, Ruiz AJ, Toro MA, Gutiérrez KJ, Merino VM, Cornejo A, Palop JA, Sanmartín C, Plano D (2019) Synthesis and leishmanicidal activity of novel urea, thiourea, and selenourea derivatives of diselenides. Antimicrob Agents Chemother 63(5):e02200-e2218. https://doi.org/10.1128/AAC.02200-18
Viana GM, Soares DC, Santana MV, do Amaral LH, Meireles PW, Nunes RP, da Silva LCRP, Aguiar LCS, Rodrigues CR, de Sousa VP, Castro HC, Abreu PA, Sathler PC, Saraiva EM, Cabral LM (2017) Antileishmanial thioureas: synthesis, biological activity and in silico evaluations of new promising derivatives. Chem Pharm Bull (Tokyo) 65(10):911–919. https://doi.org/10.1248/cpb.c17-00293
Mohammadi-ghalehbin B, Najafi S, Razzaghi-Asl N (2020) Synthesis and antileishmanial effect of a few cyclic and non-cyclic n-aryl enamino amide derivatives. Res Pharm Sci 15(4):340–349. https://doi.org/10.4103/1735-5362.293512
Rauf MK, Yaseen S, Badshah A, Zaib S, Arshad R, Imtiaz-Ud-Din TMN, Iqbal J (2015) Synthesis, characterization and urease inhibition, in vitro anticancer and antileishmanial studies of Ni(II) complexes with N, N, N′-trisubstituted thioureas. J Biol Inorg Chem 20(3):541–554. https://doi.org/10.1007/s00775-015-1239-5
White CA Jr (2004) Nitazoxanide: a new broad spectrum antiparasitic agent. Expert Rev Anti-infect Ther 2(1):43–49. https://doi.org/10.1586/14787210.2.1.43
Mohammadi-Ghalehbin B, Sepehri S, Nejatkhah N, Safari S, Hosseinali Z, Sabour S, Razzaghi-Asl N (2022) Synthesis, antileishmanial activity and molecular docking study of new 3, 4 dihydropyrimidinones/thiones. Pharm Chem J 55(10):1052–1058. https://doi.org/10.1007/s11094-021-02536-4
Brannigan JA, Roberts SM, Bell AS, Hutton JA, Hodgkinson MR, Tate EW, Leatherbarrow RJ, Smith DF, Wilkinson AJ (2014) Diverse modes of binding in structures of Leishmania major N-myristoyltransferase with selective inhibitors. IUCrJ 1(Pt 4):250–260. https://doi.org/10.1107/S2052252514013001
Niapour A, Amirshahrokhi K, Azari Rad M, Mohammadi-Ghalehbin B (2019) Evaluation of the paraquat effect on Leishmania major promastigotes and HUVECs viability under in vitro condition. J Ardabil Univ Med Sci 19(1):61–70. https://doi.org/10.29252/jarums.19.1.61
Morris GM, Huey R, Lindstrom W, Sanner MF, Belew RK, Goodsell DS, Olson AJ (2009) AutoDock4 and AutoDockTools4: automated docking with selective receptor flexibility. J Comput Chem 30:2785–2791. https://doi.org/10.1002/jcc.21256
Sanner M (1999) Python: a programming language for software integration and development. J Mol Graph Model 17(1):57–61
Bell AS, Yu Z, Hutton JA, Wright MH, Brannigan JA, Paape D, Roberts SM, Sutherell CL, Ritzefeld M, Wilkinson AJ, Smith DF, Leatherbarrow RJ, Tate EW (2020) Novel thienopyrimidine inhibitors of Leishmania N-myristoyltransferase with on-target activity in intracellular amastigotes. J Med Chem 63(14):7740–7765. https://doi.org/10.1021/acs.jmedchem.0c00570
Qiu W, Hutchinson A, Wernimont A, Lin Y-H, Kania A, Ravichandran M, Kozieradzki I, Cossar D, Schapira M, Arrowsmith CH, Bountra C, Weigelt J, Edwards AM, Wyatt PG, Ferguson MAJ, Frearson JA, Brand SY, Robinson DA, Bochkarev A, Hui, R (Latest revision on 2011) Crystal structure of human type-I N-myristoyltransferase with bound myristoyl-CoA and inhibitor. https://doi.org/10.2210/pdb3jtk/pdb
Ghanbarimasir Z, Bekhradnia A, Rafiei A, Razzaghi-Asl N, Kardan M (2018) Design, synthesis, biological assessment and molecular docking studies of new 2-aminoimidazole-quinoxaline hybrids as potential anticancer agents. Spectrochim Acta A 194:21–35. https://doi.org/10.1016/j.saa.2017.12.063
Schöning-Stierand K, Diedrich K, Fährrolfes R, Flachsenberg F, Meyder A, Nittinger E, Steinegger R, Rarey M (2020) ProteinsPlus: interactive analysis of protein–ligand binding interfaces. Nucleic Acids Res 48(W1):W48–W53. https://doi.org/10.1093/nar/gkaa235
Daina A, Michielin O, Zoete V (2017) SwissADME: a free web tool to evaluate pharmacokinetics, drug-likeness and medicinal chemistry friendliness of small molecules. Sci Rep 7:42717. https://doi.org/10.1038/srep42717
Van Der Spoel D, Lindahl E, Hess B, Groenhof G, Mark AE, Berendsen HJ (2005) GROMACS: fast, flexible, and free. J Comput Chem 26(16):1701–1718. https://doi.org/10.1002/jcc.20291
Schüttelkopf AW, van Aalten DM (2004) PRODRG: a tool for high-throughput crystallography of protein–ligand complexes. Acta Crystallogr D 60:1355–1356. https://doi.org/10.1107/S0907444904011679
Berendsen HJC, Postma JPM, Van Gunsteren WF, Hermans J (1981) Interaction models for water in relation to protein hydration. In: Pullman B (ed) Intermolecular forces. D. Reidel Publishing Company, Dordrecht, pp 331–342. https://doi.org/10.1007/978-94-015-7658-1_21
Parrinello M, Rahman A (1981) Polymorphic transitions in single crystals: a new molecular dynamics method. J Appl Phys 52:7182–7190. https://doi.org/10.1063/1.328693
Hess B, Bekker H, Berendsen HJC, Fraaije JGEM (1997) LINCS: a linear constraint solver for molecular simulations. J Comput Chem 18:1463–1472. https://doi.org/10.1002/(SICI)1096-987X(199709)18:12%3c1463::AID-JCC4%3e3.0.CO;2-H
Darden T, York D, Pedersen L (1993) Particle mesh Ewald: an N log (N) method for Ewald sums in large systems. J Chem Phys 98:10089–10092. https://doi.org/10.1063/1.464397
Resh MD (2012) Targeting protein lipidation in disease. Trends Mol Med 18:206–214. https://doi.org/10.1016/j.molmed.2012.01.007
Price HP, Güther ML, Ferguson MA, Smith DF (2010) Myristoyl-CoA: protein N-myristoyltransferase depletion in trypanosomes causes a virulence and endocytic defects. Mol Biochem Parasitol 169(1):55–58. https://doi.org/10.1016/j.molbiopara.2009.09.006
Price HP, Menon MR, Panethymitaki C, Goulding D, McKean PG, Smith DF (2003) Myristoyl-CoA: protein N-myristoyltransferase, an essential enzyme and potential drug target in kinetoplastid parasites. J Biol Chem 278(9):7206–7214. https://doi.org/10.1074/jbc.M211391200
Brannigan JA, Smith BA, Yu Z, Brzozowski AM, Hodgkinson MR, Maroof A, Price HP, Meier F, Leatherbarrow RJ, Tate EW, Smith DF, Wilkinson AJ (2010) N-myristoyltransferase from Leishmania donovani: structural and functional characterization of a potential drug target for visceral leishmaniasis. J Mol Biol 396:985–999. https://doi.org/10.1016/j.jmb.2009.12.032
Ferreira de Freitas R, Schapira M (2017) A systematic analysis of atomic protein–ligand interactions in the PDB. MedChemComm 8(10):1970–1981. https://doi.org/10.1039/C7MD00381A
Novoseletsky VN, Pyrkov TV, Efremov RG (2010) Analysis of hydrophobic interactions of antagonists with the beta2-adrenergic receptor. SAR QSAR Environ Res 21(1):37–55. https://doi.org/10.1080/10629360903560637
Rackham MD, Yu Z, Brannigan JA, Heal WP, Paape D, Barker KV, Wilkinson AJ, Smith DF, Leatherbarrow RJ, Tate EW (2015) Discovery of high affinity inhibitors of Leishmania donovani N-myristoyltransferase. Med Chem Commun 6:1761–1766. https://doi.org/10.1039/C5MD00241A
Liu K, Watanabe E, Kokubo H (2017) Exploring the stability of ligand binding modes to proteins by molecular dynamics simulations. J Comput Aided Mol Des 31(2):201–211. https://doi.org/10.1007/s10822-016-0005-2
Lobanov MY, Bogatyreva NS, Galzitskaya OV (2008) Radius of gyration as an indicator of protein structure compactness. Mol Biol 42:623–628. https://doi.org/10.1134/S0026893308040195
Pace CN, Fu H, Lee Fryar K, Landua J, Trevino SR, Schell D, Thurlkill RL, Imura S, Scholtz JM, Gajiwala K, Sevcik J, Urbanikova L, Myers JK, Takano K, Hebert EJ, Shirley BA, Grimsley GR (2014) Contribution of hydrogen bonds to protein stability. Protein Sci 23(5):652–661. https://doi.org/10.1002/pro.2449
Funding
The research leading to offered results received funding from Ardabil University of Medical Sciences (ARUMS) under Grant Number IR.ARUMS.REC.1398.595.
Author information
Authors and Affiliations
Contributions
All authors contributed equally in this work (concept, design, definition of intellectual content, literature search, experimental studies, data acquisition, data analysis, statistical analysis, manuscript preparation, manuscript editing and manuscript review).
Corresponding author
Ethics declarations
Conflict of interest
Authors declare to have no conflicts of interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mohammadi-Ghalehbin, B., Shiran, J.A., Gholizadeh, N. et al. Synthesis, antileishmanial activity and molecular modeling of new 1-aryl/alkyl-3-benzoyl/cyclopropanoyl thiourea derivatives. Mol Divers 27, 1531–1545 (2023). https://doi.org/10.1007/s11030-022-10508-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11030-022-10508-3