Abstract
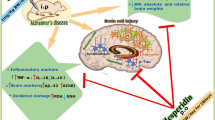
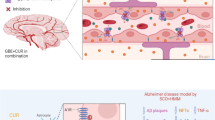
Background and Aim: Traditionally, Celastrus paniculatus Willd. (CP) oil has been utilized as a tranquilizer and memory enhancer. The present study investigated the neuropharmacological activity and efficacy of CP oil in ameliorating scopolamine-induced cognitive impairment in rats. Experimental procedure: Cognitive deficiency was induced in rats by administration of scopolamine (2 mg/kg intraperitoneal injection) for a period of 15 days. Donepezil served as a reference drug and CP oil was tested as both preventive and curative treatments. Animals’ behaviour was assessed through the Morris water maze (MWM), novel object preference (NOR), and conditioned avoidance (CA) tests. Oxidative stress parameters, bioamine concentration (dopamine, noradrenaline, and 5-hydroxytryptamine), nerve growth factor (NGF), interleukin-6 (IL-6), nuclear factor kappa B (NF-кB), and tumor necrosis factor-alpha (TNFα) were estimated. Synaptophysin immunohistochemistry was performed. Results: Our results showed that CP oil ameliorated behavioural deficits. It reduced latency to find a hidden platform in MWM. Reduced novel object exploration time and discrimination index (p < 0.05) in the NOR. Reduced step-down latency and normalized conditioned avoidance response (p < 0.001) in the CA test. CP oil increased dopamine, serotonin, norepinephrine, superoxide dismutase (SOD), glutathione, and catalase levels. It decreased malondialdehyde (MDA), acetylcholinesterase activity, IL-6, NF-кB (P < 0.001), TNFα, and NGF levels. Treatment showed approximate typical reactivity to synaptophysin. Conclusion: Our data is suggestive that CP oil treatment improves behavioural test outcomes, increases biogenic amine concentration, and decreases acetylcholinesterase activity, and neuroinflammatory biomarkers. It also restores synaptic plasticity. It thus improves cognitive functions against scopolamine-induced amnesia in rats by improving cholinergic function.







Similar content being viewed by others
Data Availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
Change history
24 April 2023
A Correction to this paper has been published: https://doi.org/10.1007/s11011-023-01215-5
References
Abdelghany AK, El-Nahass ES, Ibrahim MA et al (2022) Neuroprotective role of medicinal plant extracts evaluated in a scopolamine-induced rat model of Alzheimer. https://doi.org/10.1080/1354750X.2022.2112975. ’s diseasehttps://doi.org/101080/1354750X20222112975
Ademosun AO, Adebayo AA, Popoola TV, Oboh G (2020) Shaddock (Citrus maxima) peels extract restores cognitive function, cholinergic and purinergic enzyme systems in scopolamine-induced amnesic rats. Drug Chem Toxicol 0:1–8. https://doi.org/10.1080/01480545.2020.1808668
Aleem M (2021) Phytochemistry and pharmacology of Celastrus paniculatus Wild.: a nootropic drug. J Complement Integr Med. https://doi.org/10.1515/JCIM-2021-0251/MACHINEREADABLECITATION/RIS
Alzheimer’s Association R (2021) 2021 Alzheimer’s disease facts and figures. Alzheimer’s Dement 17:327–406. https://doi.org/10.1002/alz.12328
Bhanumathy M, Harish MS, Shivaprasad HN, Sushma G (2010) Nootropic activity of Celastrus paniculatus seed. Pharm Biol 48:324–327. https://doi.org/10.3109/13880200903127391
Bhattarai P, Cosacak MI, Mashkaryan V et al (2020) Neuron-glia interaction through Serotonin-BDNF-NGFR axis enables regenerative neurogenesis in Alzheimer’s model of adult zebrafish brain. PLoS Biol 18:1–27. https://doi.org/10.1371/journal.pbio.3000585
Blokland A (2022) Cholinergic models of memory impairment in animals and man: scopolamine vs. biperiden. Behav Pharmacol 33:231–237. https://doi.org/10.1097/FBP.0000000000000670
Boligon AA, de Freitas RB, de Brum TF et al (2014) Antiulcerogenic activity of Scutia buxifolia on gastric ulcers induced by ethanol in rats. Acta Pharm Sin B 4:358–367. https://doi.org/10.1016/j.apsb.2014.05.001
Brandeis R, Brandys Y, Yehuda S (1989) The use of the Morris water maze in the study of memory and learning. Int J Neurosci 48:29–69. https://doi.org/10.3109/00207458909002151
Chakrabarty M, Bhat P, Kumari S et al (2012) Cortico-hippocampal salvage in chronic aluminium induced neurodegeneration by Celastruspaniculatus seed oil: neurobehavioural, biochemical, histological study. J Pharmacol Pharmacother 3:161–171. https://doi.org/10.4103/0976-500X.95520
Chalermpalanupap T, Kinkead B, Hu WT et al (2013) Targeting norepinephrine in mild cognitive impairment and Alzheimer’s disease. Alzheimer’s Res Ther. https://doi.org/10.1186/alzrt175. 5:
Chan KW, Chin VK, Ismail N et al (2022) Biological activities and therapeutic effects of Celastrus paniculatus seed oil. Mult Biol Act Unconv Seed Oils 29–41. https://doi.org/10.1016/B978-0-12-824135-6.00024-6
Cheon SY, Koo BN, Kim SY et al (2021) Scopolamine promotes neuroinflammation and delirium-like neuropsychiatric disorder in mice. Sci Rep 2021 111 11:1–13. https://doi.org/10.1038/s41598-021-87790-y
Deture MA, Dickson DW (2019) The neuropathological diagnosis of Alzheimer’s disease. Mol Neurodegener 2019 141 14:1–18. https://doi.org/10.1186/S13024-019-0333-5
Dhanasekaran S, Perumal P, Palayan M (2015) In-vitro screening for acetylcholinesterase enzyme inhibition potential and antioxidant activity of extracts of Ipomoea aquatica Forsk: therapeutic lead for Alzheimer’s disease. J Appl Pharm Sci 5:12–16. https://doi.org/10.7324/JAPS.2015.50203
El-Khadragy MF, Al-Olayan EM, Abdel Moneim AE (2014) Neuroprotective effects of Citrus reticulata in scopolamine-induced dementia oxidative stress in rats. CNS Neurol Disord Drug Targets 13:684–690
Faldu KG, Shah JS (2022) Alzheimer’s disease: a scoping review of biomarker research and development for effective disease diagnosis. 22:681–703. https://doi.org/10.1080/14737159.2022.2104639
Faldu, Patel SS, Shah JS (2021) Celastrus paniculatus oil ameliorates synaptic plasticity in a rat model of attention deficit hyperactivity disorder. Asian Pac J Trop Biomed 11:105. https://doi.org/10.4103/2221-1691.306690
Falsafi SK, Deli A, Höger H et al (2012) Scopolamine administration modulates muscarinic, nicotinic and NMDA receptor systems. PLoS ONE 7:e32082. https://doi.org/10.1371/journal.pone.0032082
Farooqui AA (2019) Potential treatment strategies of Dementia with Ayurvedic Medicines. Mol Mech Dement 287–328. https://doi.org/10.1016/B978-0-12-816347-4.00009-X
Gattu M, Boss KL, Terry AV, Buccafusco JJ (1997) Reversal of scopolamine-induced deficits in navigational memory performance by the seed oil of Celastrus paniculatus. Pharmacol Biochem Behav 57:793–799. https://doi.org/10.1016/S0091-3057(96)00391-7
Giovannini MG, Spignoli G, Carla V, Pepeu G (1991) A decrease in brain catecholamines prevents oxiracetam antagonism of the effects of scopolamine on memory and brain acetylcholine. Pharmacol Res 24:395–405. https://doi.org/10.1016/1043-6618(91)90044-X
Godkar PB, Gordon RK, Ravindran A, Doctor BP (2006) Celastrus paniculatus seed oil and organic extracts attenuate hydrogen peroxide- and glutamate-induced injury in embryonic rat forebrain neuronal cells. Phytomedicine 13:29–36. https://doi.org/10.1016/j.phymed.2003.11.011
Gutierres JM, Carvalho FB, Schetinger MRC et al (2014) Neuroprotective effect of anthocyanins on acetylcholinesterase activity and attenuation of scopolamine-induced amnesia in rats. Int J Dev Neurosci 33:88–97. https://doi.org/10.1016/j.ijdevneu.2013.12.006
Ivanova N, Liu Q, Agca C et al (2020) White matter inflammation and cognitive function in a co-morbid metabolic syndrome and prodromal Alzheimer’s disease rat model. J Neuroinflammation 17:1–18. https://doi.org/10.1186/s12974-020-1698-7
Jadhav K, Marathe P, Rege N et al (2015) Effect of Jyotiṣmatī seed oil on spatial and fear memory using scopolamine induced amnesia in mice. Anc Sci Life 34:130. https://doi.org/10.4103/0257-7941.157149
Jafarian S, Ling KH, Hassan Z et al (2019) Effect of zerumbone on scopolamine-induced memory impairment and anxiety-like behaviours in rats. Alzheimer’s Dement Transl Res Clin Interv 5:637–643. https://doi.org/10.1016/J.TRCI.2019.09.009
Kaur R, Mehan S et al (2015) Ameliorative treatment with Ellagic Acid in Scopolamine Induced Alzheimer’s type memory and cognitive dysfunctions in rats. Austin J Clin Neurol 2:415–430. https://doi.org/10.1007/s007020170063
Krashia P, Nobili A, D’amelio M (2019) Unifying hypothesis of dopamine neuron loss in neurodegenerative diseases: focusing on alzheimer’s disease. Front Mol Neurosci 12:1–8. https://doi.org/10.3389/fnmol.2019.00123
Lück H (1965) Catalase. Methods Enzym Anal 885–894. https://doi.org/10.1016/B978-0-12-395630-9.50158-4
Mendez MF (2021) The relationship between anxiety and Alzheimer’s Disease. J Alzheimer’s Dis Reports 5:171. https://doi.org/10.3233/ADR-210294
Mukhopadhyay S, Banerjee D, Kosagisharaf JR (2021) A primer on the evolution of Aducanumab: the first antibody approved for treatment of Alzheimer’s Disease. J Alzheimer’s Dis 83:1537–1552. https://doi.org/10.3233/JAD-215065
Morris R (1984) Developments of a water-maze procedure for studying spatial learning in the rat. J NeurosciMethods 11:47?60. https://doi.org/10.1016/0165-0270(84)90007-4
Nagpal K, Garg M, Arora D et al (2022) An extensive review on phytochemistry and pharmacological activities of indian medicinal plant Celastrus paniculatus Willd. Phyther Res 36:1930–1951. https://doi.org/10.1002/PTR.7424
Nalini K, Karanth KS, Rao A, Aroor AR (1995) Effects of Celastrus paniculatus on passive avoidance performance and biogenic amine turnover in albino rats. J Ethnopharmacol 47:101–108. https://doi.org/10.1016/0378-8741(95)01264-E
Patel P, Shah J (2021) Protective effects of hesperidin through attenuation of Ki67 expression against DMBA-induced breast cancer in female rats. Life Sci 285:119957. https://doi.org/10.1016/j.lfs.2021.119957
Rajkumar R, Kumar EP, Sudha S, Suresh B (2007) Evaluation of anxiolytic potential of Celastrus oil in rat models of behaviour. Fitoterapia 78:120–124. https://doi.org/10.1016/j.fitote.2006.09.028
Tang KS (2019) The cellular and molecular processes associated with scopolamine-induced memory deficit: a model of Alzheimer’s biomarkers. Life Sci 233:116695. https://doi.org/10.1016/j.lfs.2019.116695
Tiwari V, Chopra K (2013) Resveratrol abrogates alcohol-induced cognitive deficits by attenuating oxidative–nitrosative stress and inflammatory cascade in the adult rat brain. Neurochem Int 62:861–869. https://doi.org/10.1016/J.NEUINT.2013.02.012
Tiwari V, Chopra K (2012) Attenuation of oxidative stress, neuroinflammation, and apoptosis by curcumin prevents cognitive deficits in rats postnatally exposed to ethanol. Psychopharmacol 2012 2244 224:519–535. https://doi.org/10.1007/S00213-012-2779-9
Tiwari V, Kuhad A, Chopra K (2009) Suppression of neuro-inflammatory signaling cascade by tocotrienol can prevent chronic alcohol-induced cognitive dysfunction in rats. Behav Brain Res 203:296–303. https://doi.org/10.1016/J.BBR.2009.05.016
Tohda C, Naito R, Joyashiki E (2008) Kihi-to, a herbal traditional medicine, improves Abeta(25–35)-induced memory impairment and losses of neurites and synapses. BMC Complement Altern Med 8:49. https://doi.org/10.1186/1472-6882-8-49
Topuz RD, Gunduz O, Tastekin E, Karadag CH (2020) Effects of hippocampal histone acetylation and HDAC inhibition on spatial learning and memory in the Morris water maze in rats. Fundam Clin Pharmacol 34:222–228. https://doi.org/10.1111/fcp.12512
Valecha R, Dhingra D (2016) Behavioral and biochemical evidences for antidepressant-like activity of Celastrus Paniculatus seed oil in mice. Basic Clin Neurosci 7:49
Vogel HG, Vogel WH (1998) Drug Discovery and Evaluation edited by HG Vogel and WH Vogel
Vorhees CV, Williams MT (2006) Morris water maze: procedures for assessing spatial and related forms of learning and memory. Nat Protoc 1:848–858. https://doi.org/10.1038/nprot.2006.116
Yamamoto Y, Gaynor R (2001) Role of the NF-kB pathway in the pathogenesis of Human Disease States. Curr Mol Med 1:287–296. https://doi.org/10.2174/1566524013363816
Zaki HF, Abd-El-Fattah MA, Attia AS (2014) Naringenin protects against scopolamine-induced dementia in rats. Bull Fac Pharmacy Cairo Univ 52:15–25. https://doi.org/10.1016/j.bfopcu.2013.11.001
Funding
This research project was supported by the grant (GUJCOST/MRP/2014-15/2592) from Gujarat Council for Science and Technology (GUJCOST) received by the author Dr Jigna Samir Shah.
Author information
Authors and Affiliations
Contributions
KGF contributed to the background literature review, animal studies, data acquisition, and manuscript preparation. SSP contributed to data analysis, drafting, and revision of the manuscript. JSS contributed to the conception, design of the study, supervision of the work, and critical revision of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors have no relevant financial or non-financial interests to disclose.
Ethics approval
The experiments were conducted as per the approved experimental protocol (IP/PCOL/MPH/17/003). The protocol was approved the Institutional Animal Ethics Committee of Nirma University, Ahmedabad, India in accordance with the guidance of Committee for Control and Supervision of Experiments on Animal (CPCSEA), Ministry of Social justice and Empowerment, Government of India.
Consent to participate
Not Applicable.
Consent to publish
Not Applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Faldu, K.G., Patel, S.S. & Shah, J.S. Celastrus paniculatus oil ameliorates NF-KB mediated neuroinflammation and synaptic plasticity in the scopolamine-induced cognitive impairment rat model. Metab Brain Dis 38, 1405–1419 (2023). https://doi.org/10.1007/s11011-023-01186-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11011-023-01186-7