Abstract
Ischemia is one of the main etiological factors of stroke and is associated with the development of energy deficiency, oxidative stress, and inflammation. An abrupt restoration of blood flow, called reperfusion, can worsen the effects of ischemia. In our study, we assessed the neuroprotective potential of 1-benzoyl-6-hydroxy-2,2,4-trimethyl-1,2-dihydroquinoline (BHDQ) in cerebral ischemia/reperfusion (CIR) in rats. Wistar rats, divided into 4 groups were used in the study: sham-operated animals; animals with CIR caused by occlusion of the common carotid arteries and subsequent removal of the occlusions; rats treated with BHDQ at a dose of 50 mg/kg in the presence of pathology; sham-operated animals treated with BHDQ. The analysis of the state of energy metabolism in the brain, the level of the S100B protein and the histological assessment of the brain tissue were carried out. The antioxidant potential of BHDQ was assessed by measuring biochemiluminescence parameters, analysing the level of 8-isoprostane, products of lipid and protein oxidation, concentration of α-tocopherol and citrate, and aconitate hydratase activity during CIR in rats. A study of the effect of BHDQ on the regulation of the enzymatic antioxidant system and the inflammatory processes was performed. We demonstrated that BHDQ has a neuroprotective effect in CIR, reducing histopathological changes in the brain, normalizing pyruvate and lactate concentrations, and the transcripts level of Hif-1α gene. The positive effect of BHDQ was probably due to its antioxidant and anti-inflammatory activity, manifested in a decrease in the parameters of the oxidative stress, decreased mRNA of proinflammatory cytokines and NF-κB factor genes. In addition, BHDQ reduced the load on antioxidant protection enzymes, contributing to a change in their activities, decreased the level of antioxidant gene transcripts and expression of Nrf2 and Foxo1 factors toward control. Thus, BHDQ exhibited a neuroprotective effect due to a decrease in the level of oxidative stress and inflammation and the normalization of redox homeostasis on CIR in rats.







Similar content being viewed by others
Availability of data and material
All data generated or analysed during this study are included in this published article.
Code Availability
Not applicable.
References
Arteaga O, Álvarez A, Revuelta M, Santaolalla F, Urtasun A, Hilario E (2017) Role of Antioxidants in Neonatal Hypoxic–Ischemic Brain Injury: New Therapeutic Approaches. Int J Mol Sci 18(2):265. https://doi.org/10.3390/ijms18020265
Benedusi V, Martorana F, Brambilla L, Maggi A, Rossi D (2012) The Peroxisome Proliferator-activated Receptor γ (PPARγ) Controls Natural Protective Mechanisms against Lipid Peroxidation in Amyotrophic Lateral Sclerosis. J Biol Chem 287:35899–35911. https://doi.org/10.1074/jbc.M112.366419
Błaszczyk A, Augustyniak A, Skolimowski J (2013) Ethoxyquin: An Antioxidant Used in Animal Feed. Int J Food Sci 2013:585931. https://doi.org/10.1155/2013/585931
Burka LT, Sanders JM, Matthews HB (1996) Comparative metabolism and disposition of ethoxyquin in rat and mouse. II Metabolism Xenobiotica 26:597–611. https://doi.org/10.3109/00498259609046736
Cetinkaya-Fisgin A, Zhu J, Luan X, Kim JS, Oh B, Brayton C, Alt J, Rais R, Slusher B, Höke A (2021) Development of EQ-6, a Novel Analogue of Ethoxyquin to Prevent Chemotherapy-Induced Peripheral Neuropathy. Neurotherapeutics 8:2061–2072. https://doi.org/10.1007/s13311-021-01093-8
Chacko S, Samanta S (2017) A novel approach towards design, synthesis and evaluation of some Schiff base analogues of 2-aminopyridine and 2-aminobezothiazole against hepatocellular carcinoma. Biomed Pharmacother 89:162–176. https://doi.org/10.1016/j.biopha.2017.01.108
Chamorro A (2018) Neuroprotectants in the Era of Reperfusion Therapy. J Stroke 20:197–207. https://doi.org/10.5853/jos.2017.02901
Desai ID, Martinez FE (1986) Bilirubin interference in the colorimetric assay of plasma vitamin E. Clin Chim Acta 154:247–250. https://doi.org/10.1016/0009-8981(86)90040-9
EFSA Panel On Additives And Products Or Substances Used In Animal Feed (2015) Safety and efficacy of ethoxyquin (6-ethoxy-1,2-dihydro-2,2,4-trimethylquinoline) for all animal species. EFSA J 13:4272. https://doi.org/10.2903/j.efsa.2015.4272
Ellman GL (1959) Tissue sulfhydryl groups. Arch Biochem Biophys 82:70–77. https://doi.org/10.1016/0003-9861(59)90090-6
Góth L (1991) A simple method for determination of serum catalase activity and revision of reference range. Clin Chim Acta 196:143–151. https://doi.org/10.1016/0009-8981(91)90067-m
Gu JH, Ge JB, Li M, Wu F, Zhang W, Qin ZH (2012) Inhibition of NF-κB activation is associated with anti-inflammatory and anti-apoptotic effects of Ginkgolide B in a mouse model of cerebral ischemia/reperfusion injury. Eur J Pharm Sci 47:652–660. https://doi.org/10.1016/j.ejps.2012.07.016
Gu M, Iravani MM, Cooper JM, King D, Jenner P, Schapira AH (2004) Pramipexole protects against apoptotic cell death by non-dopaminergic mechanisms. J Neurochem 91:1075–1081. https://doi.org/10.1111/j.1471-4159.2004.02804.x
He Y, Yang Q, Liu H, Jiang L, Liu Q, Lian W, Huang J (2020) Effect of blood pressure on early neurological deterioration of acute ischemic stroke patients with intravenous rt-PA thrombolysis may be mediated through oxidative stress induced blood-brain barrier disruption and AQP4 upregulation. J Stroke Cerebrovasc Dis 29:104997. https://doi.org/10.1016/j.jstrokecerebrovasdis.2020.104997
Hoke A, Reed N, Zhu J (2014) Ethoxyquin Prevents Development Of Neuropathy In Rodent Models Of Diabetic Peripheral Neuropathy And HIV-Associated Neuropathy. Neurology 82:S46004
Huang Z, Mou T, Luo Y, Pu X, Pu J, Wan L, Gong J, Yang H, Liu Y, Li Z, Shen A, Wu Z (2020) Inhibition of miR-450b-5p ameliorates hepatic ischemia/reperfusion injury via targeting CRYAB. Cell Death Dis 11:455. https://doi.org/10.1038/s41419-020-2648-0
Iskusnykh IY, Kryl’skii ED, Brazhnikova DA, Popova TN, Shikhaliev KhS, Shulgin KK, Matasova LV, Popov SS, Zhaglin DA, Zakharova AA, Popova NR, Fattakhov N (2021) Novel Antioxidant, Deethylated Ethoxyquin, Protects against Carbon Tetrachloride Induced Hepatotoxicity in Rats by Inhibiting NLRP3 Inflammasome Activation and Apoptosis. Antioxidants 10:122. https://doi.org/10.3390/antiox10010122
Kahl A, Stepanova A, Konrad C, Anderson C, Manfredi G, Zhou P, Iadecola C, Galkin A (2018) Critical Role of Flavin and Glutathione in Complex I–Mediated Bioenergetic Failure in Brain Ischemia/Reperfusion Injury. Stroke 49:1223–1231. https://doi.org/10.1161/STROKEAHA.117.019687
Kanavaki A, Spengos K, Moraki M, Delaporta P, Kariyannis C, Papassotiriou I, Kattamis A (2017) Serum Levels of S100b and NSE Proteins in Patients with Non-Transfusion-Dependent Thalassemia as Biomarkers of Brain Ischemia and Cerebral Vasculopathy. Int J Mol Sci 18:2724. https://doi.org/10.3390/ijms18122724
Kryl’skii ED, Chupandina EE, Popova TN, Shikhaliev KhS, Mittova VO, Popov SS, Verevkin AN, Filin AA (2021) Neuroprotective effect of 6-hydroxy-2,2,4-trimethyl-1,2-dihydroquinoline mediated via regulation of antioxidant system and inhibition of inflammation and apoptosis in a rat model of cerebral ischemia/reperfusion. Biochimie 186:130–146. https://doi.org/10.1016/j.biochi.2021.04.010
Li HS, Zhou YN, Li L, Li SF, Long D, Chen XL, Zhang JB, Feng L, Li YP (2019) HIF-1α protects against oxidative stress by directly targeting mitochondria. Redox Biol 25:101109. https://doi.org/10.1016/j.redox.2019.101109
Liu HB, Wang L, Su WW, Xie X-Q (2014) ALzPlatform: An Alzheimer’s Disease Domain-Specific Chemogenomics Knowledgebase for Polypharmacology and Target Identification Research. J Comput Info Modeling 54:1050–1060. https://doi.org/10.1021/ci500004h
Liu L, Locascio LM, Doré S (2019) Critical Role of Nrf2 in Experimental Ischemic Stroke. Front Pharmacol 10:153. https://doi.org/10.3389/fphar.2019.00153
Liu Y, Sun Y, Ewaleifoh O, Wei J, Mi R, Zhu J, Hoke A, Polydefkis M (2021) Ethoxyquin is neuroprotective and partially prevents somatic and autonomic neuropathy in db/db mouse model of type 2 diabetes. Sci Rep 11:10749. https://doi.org/10.1038/s41598-021-89781-5
Lockhart B, Bonhomme N, Roger A, Dorey G, Casara P, Lestage P (2001) Protective effect of the antioxidant 6-ethoxy-2,2-pentamethylen-1,2-dihydroquinoline (S 33113) in models of cerebral neurodegeneration. Eur J Pharmacol 416:59–68. https://doi.org/10.1016/S0014-2999(01)00862-7
Marchi N, Cavaglia M, Fazio V, Bhudia S, Hallene K, Janigro D (2004) Peripheral markers of blood–brain barrier damage. Clin Chim Acta 342:1–12. https://doi.org/10.1016/j.cccn.2003.12.008
Matasova LV, Popova TN (2008) Aconitate hydratase of mammals under oxidative stress. Biochem (Moscow) 73:957–964. https://doi.org/10.1134/S0006297908090010
Medvedeva SM, Krugovov DA, Mengele EA, Shikhaliev KhS (2013) New derivatives of 6-hydroxy-2,2,4-trimethylhydroquinolines. Vestnik VGU, Seriya: Khimiya. Biologiya. Farmatsiya 2:49-52. (In Russian)
Mendes L, Angélica S, Schiavon P, Milani H, Maria R, Oliveira W (2013) Cognitive impairment and persistent anxiety-related responses following bilateral common carotid artery occlusion in mice. Behav Brain Res 249:28–37. https://doi.org/10.1016/j.bbr.2013.04.010
Ng KT-P, Yeung O W-H, Lam YF, Liu J, Liu H, Pang L, Yang XX, ZhuJ, Zhang W, Lau MYH, Qiu WQ, Shiu HC, Lai MK, Lo CM, Man K (2021) Glutathione S-transferase A2 promotes hepatocellular carcinoma recurrence after liver transplantation through modulating reactive oxygen species metabolism. Cell death discovery 7:188. https://doi.org/10.1038/s41420-021-00569-y
Nishikimi M, Rao NA, Yagi K (1972) The occurrence of superoxide anion in the reaction of reduced phenazine methosulphate and molecular oxygen. Biochem Biophys Res Co 46:849–864. https://doi.org/10.1016/S0006-291X(72)80218-3
Paglia DE, Valentine WN (1967) Studies on the quantitative and qualitative characterization of erythrocyte glutathione peroxidase. Lab Clin Med 70:158–169
Pan Z, Ma G, Kong L, Du G (2021) Hypoxia-inducible factor-1: Regulatory mechanisms and drug development in stroke. Pharmacol Res 170:105742. https://doi.org/10.1016/j.phrs.2021.105742
Piskarev IM, Trofimova SV, Ivanova IP, Burkhina OE (2015) Investigation of the level of free-radical processes in substrates and biological samples using induced chemiluminescence. Biophysics 60:400–408. https://doi.org/10.1134/S0006350915030148
ProTox-II - Prediction Of Toxicity Of Chemicals (2021) https://tox-new.charite.de/protox_II/ (accessed 11
Recknagel RO, Ghoshal AK (1966) Lipoperoxidation of rat liver microsomal lipids induced by carbon tetrachloride. Nature 210:1162–1163. https://doi.org/10.1038/2101162a0
Reznick AZ, Packer L (1994) Oxidative damage to proteins: spectrophotometric method for carbonyl assay. Methods Enzymol 233:357–363. https://doi.org/10.1016/S0076-6879(94)33041-7
Skaare J, Solheim E (1979) Studies on the metabolism of the antioxidant ethoxyquin, 6-ethoxy-2, 2, 4-trimethyl-1, 2-dihydroquinoline in the rat. Xenobiotica 9:649–657. https://doi.org/10.3109/00498257909042332
Stoeckelhuber M, Scherer M, Bracher F, Peschel O, Leibold E, Scherer G, Pluym N (2020) Development of a human biomonitoring method for assessing the exposure to ethoxyquin in the general population. Arch Toxicol 94:4209–4217. https://doi.org/10.1007/s00204-020-02871-7
Sun MS, Jin H, Sun X, Huang S, Zhang FL, Guo ZN, Yang Y (2018) Free Radical Damage in Ischemia-Reperfusion Injury: An Obstacle in Acute Ischemic Stroke after Revascularization Therapy. Oxid Med Cell Longev 2018:3804979. https://doi.org/10.1155/2018/3804979
Valdez JM, Johnstone AFM, Richards JE, Schmid JE, Royland JE, Kodavanti PRS (2018) Interaction of diet and ozone exposure on oxidative stress parameters within specific brain regions of male brown Norway rats. Int J Mol Sci 20:11. https://doi.org/10.3390/ijms20010011
Vilela P, Rowley HA (2017) Brain ischemia: CT and MRI techniques in acute ischemic stroke. Eur J Radiol 96:162–172. https://doi.org/10.1016/j.ejrad.2017.08.014
Warholm M, Guthenberg C, Von Bahr C, Mannervik B (1985) Glutathione transferases from human liver. Method Enzymol 113:499–504. https://doi.org/10.1016/s0076-6879(85)13065-x
Wu L, Xiong X, Wu X, Ye Y, Jian Z, Zhi Z, Gu L (2020) Targeting Oxidative Stress and Inflammation to Prevent Ischemia-Reperfusion Injury. Front Mol Neurosci 13:28. https://doi.org/10.3389/fnmol.2020.00028
Wu X, Dai H, Liu L, Xu C, Yin Y, Yi J, Bielec MD, Hana Y, Li S (2019) Citrate reduced oxidative damage in stem cells by regulating cellular redox signaling pathways and represent a potential treatment for oxidative stress-induced diseases. Redox Biol 21:101057. https://doi.org/10.1016/j.redox.2018.11.015
Xing YQ, Li A, Yang Y, Li XX, Zhang LN, Guo HC (2018) The regulation of FOXO1 and its role in disease progression. Life Sci 193:124–131. https://doi.org/10.1016/j.lfs.2017.11.030
Ya BL, Liu Q, Li HF, Cheng HJ, Yu T, Chen L, Wang Y, Yuan LL, Li WJ, Liu WY, Bai B (2018) Uric Acid Protects against Focal Cerebral Ischemia/Reperfusion-Induced Oxidative Stress via Activating Nrf2 and Regulating Neurotrophic Factor Expression. Oxid Med Cell Longev 2018:6069150. https://doi.org/10.1155/2018/6069150
Yan H-F, Tuo Q-Z, Yin Q-Z, Lei P (2020) The pathological role of ferroptosis in ischemia/reperfusion-related injury. Zool Res 41:220–230. https://doi.org/10.24272/j.issn.2095-8137.2020.042
Yang C, Yang Y, DeMars KM, Rosenberg GA, Candelario-Jalil E (2020) Genetic Deletion or Pharmacological Inhibition of Cyclooxygenase-2 Reduces Blood-Brain Barrier Damage in Experimental Ischemic Stroke. Front Neurol 11:887. https://doi.org/10.3389/fneur.2020.00887
Yang J (2019) The role of reactive oxygen species in angiogenesis and preventing tissue injury after brain ischemia. Microvasc Res 123:62–67. https://doi.org/10.1016/j.mvr.2018.12.005
Zanetti G (1979) Rabbit liver glutathione reductase. Purification and properties. Arch Biochem Biophys 198:241–246. https://doi.org/10.1016/0003-9861(79)90415-6
Zhang Z, Yao L, Yang J, Wang Z, Du G (2018) PI3K/Akt and HIF–1 signaling pathway in hypoxia–ischemia (Review). Mol Med Rep 18(4):3547–3554. https://doi.org/10.3892/mmr.2018.9375
Zhao Z, Lu C, Li T, Wang W, Ye W, Zeng R, Ni L, Lai Z, Wang X, Liu C (2018) The protective effect of melatonin on brain ischemia and reperfusion in rats and humans: In vivo assessment and a randomized controlled trial. J Pineal Res 65:e12521. https://doi.org/10.1111/jpi.1252
Zhu J, Carozzi V, Reed N, Mi R, Marmiroli P, Cavaletti G, Hoke A (2016) Ethoxyquin provides neuroprotection against cisplatin-induced neurotoxicity. Sci Rep 6:28861. https://doi.org/10.1038/srep28861
Zhu J, Chen W, Mi R, Zhou C, Reed N, Höke A (2013) Ethoxyquin prevents chemotherapy-induced neurotoxicity via Hsp90 modulation. Ann Neurol 74:893–904. https://doi.org/10.1002/ana.24004
Funding
This work was supported by the grant of the President of the Russian Federation for young scientists-candidates of sciences MK-254.2020.4.
Author information
Authors and Affiliations
Contributions
E.D. Kryl’skii: Investigation, writing—original draft, methodology, funding acquisition; E.E. Chupandina: writing—original draft, investigation; T.N. Popova: conceptualization, data curation, validation; Kh.S. Shikhaliev: methodology, resources, investigation; S.M. Medvedeva: methodology, resources, investigation; A.N. Verevkin: data curation, validation, investigation; S.S. Popov: validation, formal analysis, investigation; V.O. Mittova: visualization, writing—review and editing. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Ethics approval
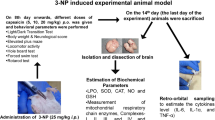
The study’s protocols were approved by the Institutional Animal Care and Use Committee of Voronezh State University (Voronezh, Russia) and correspond to EU Directive 2010/63/EU for animal experiments. For the induction of CIR, anesthetised rats were placed in a supine position on an operating table.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kryl’skii, E.D., Chupandina, E.E., Popova, T.N. et al. 1-benzoyl-6-hydroxy-2,2,4-trimethyl-1,2-dihydroquinoline exerts a neuroprotective effect and normalises redox homeostasis in a rat model of cerebral ischemia/reperfusion. Metab Brain Dis 37, 1271–1282 (2022). https://doi.org/10.1007/s11011-022-00928-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11011-022-00928-3