Abstract
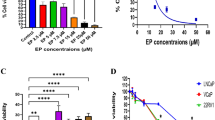
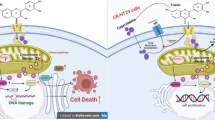
Urothelial bladder cancer is rapidly spreading across Western countries, and therapy has shown little-to-moderate effects on bladder cancer. Thus, focusing on curbing cancer incidence has become crucial. The aim of the present study was to investigate the anticancer effects of Tannic acid (TA) in human bladder cancer. UMUC3 bladder cancer cells were treated with different concentrations of TA (0–100 µM) and tested for cell viability, colony formation, and apoptosis. The involvement of the phosphoinositide-3 kinase (PI3K)/Akt pathway in the action of TA was examined. TA treatment significantly inhibited the viability and increased percentage of apoptotic cells, thereby decreasing antiapoptotic proteins (BCL2, MCL-1, and BCL-XL) expression, resulting in the Caspase-3 activation. TA treatment decreased stem cell markers expression such as SOX2, OCT4, and NANOG. Additionally, TA treatment significantly reduced the phosphorylation levels of Akt in bladder cancer cells. Our study demonstrates the growth inhibitory effects of TA in bladder cancer cells, and highlights its potential as an anticancer agent for bladder cancer.



Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article.
References
Dobruch J, Daneshmand S, Fisch M, Lotan Y, Noon AP, Resnick MJ, Shariat SF, Zlotta AR, Boorjian SA (2016) Gender and bladder cancer: a collaborative review of etiology, biology, and outcomes. Eur Urol 69:300–310. https://doi.org/10.1016/j.eururo.2015.08.037
May M, Bastian PJ, Brookman-May S, Fritsche HM, Tilki D, Otto W, Bolenz C, Gilfrich C, Trojan L, Herrmann E, Moritz R, Tiemann A, Muller SC, Ellinger J, Buchner A, Stief CG, Wieland WF, Hofner T, Hohenfellner M, Haferkamp A, Roigas J, Zacharias M, Nuhn P, Burger M (2013) Gender-specific differences in cancer-specific survival after radical cystectomy for patients with urothelial carcinoma of the urinary bladder in pathologic tumor stage T4a. Urol Oncol 31:1141–1147. https://doi.org/10.1016/j.urolonc.2011.09.011
Richters A, Aben KKH, Kiemeney L (2020) The global burden of urinary bladder cancer: an update. World J Urol 38:1895–1904. https://doi.org/10.1007/s00345-019-02984-4
Cumberbatch MG, Rota M, Catto JW, La Vecchia C (2016) The role of tobacco smoke in bladder and kidney carcinogenesis: a comparison of exposures and meta-analysis of incidence and mortality risks. Eur Urol 70:458–466. https://doi.org/10.1016/j.eururo.2015.06.042
Burger M, Catto JW, Dalbagni G, Grossman HB, Herr H, Karakiewicz P, Kassouf W, Kiemeney LA, La Vecchia C, Shariat S, Lotan Y (2013) Epidemiology and risk factors of urothelial bladder cancer. Eur Urol 63:234–241. https://doi.org/10.1016/j.eururo.2012.07.033
Kim DK, Lee JY, Jung JH, Hah YS, Cho KS (2019) Role of adjuvant cisplatin-based chemotherapy following radical cystectomy in locally advanced muscle-invasive bladder cancer: systematic review and meta-analysis of randomized trials. Investig Clin Urol 60:64–74. https://doi.org/10.4111/icu.2019.60.2.64
Surh YJ (2003) Cancer chemoprevention with dietary phytochemicals. Nat Rev Cancer 3:768–780. https://doi.org/10.1038/nrc1189
Kapinova A, Kubatka P, Golubnitschaja O, Kello M, Zubor P, Solar P, Pec M (2018) Dietary phytochemicals in breast cancer research: anticancer effects and potential utility for effective chemoprevention. Environ Health Prev Med 23:36. https://doi.org/10.1186/s12199-018-0724-1
Kotecha R, Takami A, Espinoza JL (2016) Dietary phytochemicals and cancer chemoprevention: a review of the clinical evidence. Oncotarget 7:52517–52529. https://doi.org/10.18632/oncotarget.9593
Liskova A, Stefanicka P, Samec M, Smejkal K, Zubor P, Bielik T, Biskupska-Bodova K, Kwon TK, Danko J, Busselberg D, Adamek M, Rodrigo L, Kruzliak P, Shleikin A, Kubatka P (2020) Dietary phytochemicals as the potential protectors against carcinogenesis and their role in cancer chemoprevention. Clin Exp Med 20:173–190. https://doi.org/10.1007/s10238-020-00611-w
Nagesh PKB, Hatami E, Chowdhury P, Kashyap VK, Khan S, Hafeez BB, Chauhan SC, Jaggi M, Yallapu MM (2018) Tannic acid induces endoplasmic reticulum stress-mediated apoptosis in prostate cancer. Cancers (Basel). https://doi.org/10.3390/cancers10030068
Chung KT, Wong TY, Wei CI, Huang YW, Lin Y (1998) Tannins and human health: a review. Crit Rev Food Sci Nutr 38:421–464. https://doi.org/10.1080/10408699891274273
Ferreira D, Gross GG, Hagerman AE, Kolodziej H, Yoshida T (2008) Tannins and related polyphenols: perspectives on their chemistry, biology, ecological effects, and human health protection. Phytochemistry 69:3006–3008. https://doi.org/10.1016/j.phytochem.2008.10.018
Nam S, Smith DM, Dou QP (2001) Tannic acid potently inhibits tumor cell proteasome activity, increases p27 and bax expression, and induces G1 arrest and apoptosis. Cancer Epidemiol Biomarkers Prev 10:1083–1088
Karakurt S, Adali O (2016) Tannic acid inhibits proliferation, migration, invasion of prostate cancer and modulates drug metabolizing and antioxidant enzymes. Anticancer Agents Med Chem 16:781–789. https://doi.org/10.2174/1871520616666151111115809
Tikoo K, Sane MS, Gupta C (2011) Tannic acid ameliorates doxorubicin-induced cardiotoxicity and potentiates its anti-cancer activity: potential role of tannins in cancer chemotherapy. Toxicol Appl Pharmacol 251:191–200. https://doi.org/10.1016/j.taap.2010.12.012
Sun Y, Zhang T, Wang B, Li H, Li P (2012) Tannic acid, an inhibitor of poly(ADP-ribose) glycohydrolase, sensitizes ovarian carcinoma cells to cisplatin. Anticancer Drugs 23:979–990. https://doi.org/10.1097/CAD.0b013e328356359f
Darvin P, Joung YH, Kang DY, Sp N, Byun HJ, Hwang TS, Sasidharakurup H, Lee CH, Cho KH, Park KD, Lee HK, Yang YM (2017) Tannic acid inhibits EGFR/STAT1/3 and enhances p38/STAT1 signalling axis in breast cancer cells. J Cell Mol Med 21:720–734. https://doi.org/10.1111/jcmm.13015
Lee H-P, Wang S-W, Wu Y-C, Tsai C-H, Tsai F-J, Chung J-G, Huang C-Y, Yang J-S, Hsu Y-M, Yin M-C, Li T-M, Tang C-H (2019) Glucocerebroside reduces endothelial progenitor cell-induced angiogenesis. Food Agric Immunol 30:1033–1045. https://doi.org/10.1080/09540105.2019.1660623
Lee H-P, Wang S-W, Wu Y-C, Lin L-W, Tsai F-J, Yang J-S, Li T-M, Tang C-H (2020) Soya-cerebroside inhibits VEGF-facilitated angiogenesis in endothelial progenitor cells. Food Agric Immunol 31:193–204. https://doi.org/10.1080/09540105.2020.1713055
Lee H-P, Wu Y-C, Chen B-C, Liu S-C, Li T-M, Huang W-C, Hsu C-J, Tang C-H (2020) Soya-cerebroside reduces interleukin production in human rheumatoid arthritis synovial fibroblasts by inhibiting the ERK, NF-κB and AP-1 signalling pathways. Food Agric Immunol 31:740–750. https://doi.org/10.1080/09540105.2020.1766426
Chou SL, Ramesh S, Kuo CH, Ali A, Ho TJ, Chang KP, Hsieh DJ, Kumar VB, Weng YS, Kuo WW, Huang CY (2022) Tanshinone IIA inhibits Leu27IGF-II-induced insulin-like growth factor receptor II signaling and myocardial apoptosis via estrogen receptor-mediated Akt activation. Environ Toxicol 37:142–150. https://doi.org/10.1002/tox.23385
Sp N, Kang DY, Kim DH, Yoo JS, Jo ES, Rugamba A, Jang KJ, Yang YM (2020) Tannic acid inhibits Non-small cell lung cancer (NSCLC) stemness by inducing G(0)/G(1) cell cycle arrest and intrinsic apoptosis. Anticancer Res 40:3209–3220. https://doi.org/10.21873/anticanres.14302
Sp N, Kang DY, Jo ES, Rugamba A, Kim WS, Park Y-M, Hwang D-Y, Yoo J-S, Liu Q, Jang K-J, Yang YM (2020) Tannic acid promotes TRAIL-induced extrinsic apoptosis by regulating mitochondrial ROS in human embryonic carcinoma cells. Cells. https://doi.org/10.3390/cells9020282
Jordan LG, Booth BW (2018) HER2(+) breast cancer cells undergo apoptosis upon exposure to tannic acid released from remodeled cross-linked collagen type I. J Biomed Mater Res A 106:26–32. https://doi.org/10.1002/jbm.a.36205
Cosan D, Soyocak A, Basaran A, Degirmenci I, Gunes HV (2009) The effects of resveratrol and tannic acid on apoptosis in colon adenocarcinoma cell line. Saudi Med J 30:191–195
Geng N, Zheng X, Wu M, Yang L, Li X, Chen J (2019) Tannic acid synergistically enhances the anticancer efficacy of cisplatin on liver cancer cells through mitochondria-mediated apoptosis. Oncol Rep 42:2108–2116. https://doi.org/10.3892/or.2019.7281
Darvin P, Baeg SJ, Joung YH, Sp N, Kang DY, Byun HJ, Park JU, Yang YM (2015) Tannic acid inhibits the Jak2/STAT3 pathway and induces G1/S arrest and mitochondrial apoptosis in YD-38 gingival cancer cells. Int J Oncol 47:1111–1120. https://doi.org/10.3892/ijo.2015.3098
Moretti L, Li B, Kim KW, Chen H, Lu B (2010) AT-101, a pan-Bcl-2 inhibitor, leads to radiosensitization of non-small cell lung cancer. J Thorac Oncol 5:680–687. https://doi.org/10.1097/JTO.0b013e3181d6e08e
Manning BD, Cantley LC (2007) AKT/PKB signaling: navigating downstream. Cell 129:1261–1274. https://doi.org/10.1016/j.cell.2007.06.009
Tanel A, Averill‐Bates DA (2007) P38 and ERK mitogen‐activated protein kinases mediate acrolein‐induced apoptosis in Chinese hamster ovary cells. Cell Signal 19(5):968–977. https://doi.org/10.1016/j.cellsig.2006.10.014
Funding
This work was supported by China Medical University and Asia University, Taiwan (CMU107-ASIA-01).
Author information
Authors and Affiliations
Contributions
Conceptualization—M-CC, C-YH. Methodology—SAS. Validation—C-YH, VBK. Formal analysis—M-CC, C-HH. Investigation—C-YH, M-CC. Data curation—CHD, R-JC. Writing—original draft preparation—VBK. Writing—review and editing—T-FW, VPV, C–CL. Visualization—M-CC, C-YH. Supervision—C-YH. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declared no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, MC., Annseles Rajula, S., Bharath Kumar, V. et al. Tannic acid attenuate AKT phosphorylation to inhibit UMUC3 bladder cancer cell proliferation. Mol Cell Biochem 477, 2863–2869 (2022). https://doi.org/10.1007/s11010-022-04454-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-022-04454-9