Abstract
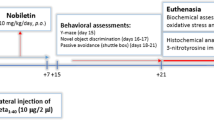
Alzheimer’s disease (AD) is a chronic, progressive, multifactorial, and the most common neurodegenerative disease which causes dementia and mental deterioration in the elderly. The available treatments for AD are not disease-modifying drugs and only provide symptomatic relief. Astaxanthin (ATX), a second-generation antioxidant, is a dark red carotenoid and exhibits the highest antioxidant capacity, anti-inflammatory, neuroprotective, and antiapoptotic effects. In this study, we investigated the therapeutic effect of different doses of ATX on the cerebral cortex and hippocampus of AD-like rats. The AD-like model was induced in rats using hydrated aluminum chloride (AlCl3.6H2O) solution that was given orally at a dose of 75 mg/kg daily for 6 weeks. Morris water maze (MWM) behavioral test was performed to confirm the cognitive dysfunction then AD-like rats were orally treated with different doses of ATX (5, 10, and 15 mg/kg) dissolved in dimethyl sulfoxide (DMSO) for six weeks. The results indicated that ATX significantly and dose-dependently improved the performance of AD-like rats treated with ATX during MWM and suppress the accumulation of amyloid β1-42 and malondialdehyde. Also, significantly inhibit acetylcholinesterase and monoamine oxidase activities and the expression of β-site amyloid precursor protein cleaving enzyme 1 (BACE 1). ATX also significantly elevated the content of acetylcholine, serotonin, and nuclear factor erythroid-2-related factor 2 (Nrf2) and miRNA-124 expression. The effect of ATX treatment was confirmed by histopathological observations using H&E stain and morphometric tissue analysis. From this study, we concluded that ATX may be a promising therapeutic agent for AD through targeting different pathogenic pathways.
Graphic abstract






Similar content being viewed by others
References
Association A (2018) 2018 Alzheimer’s disease facts and figures. Alzheimer’s and Dementia 14(3):367–429
International AsD (2019) World Alzheimer report 2019: attitudes to dementia. Alzheimer’s Disease International London, UK
Elshahidi MH, Elhadidi MA, Sharaqi AA, Mostafa A, Elzhery MA (2017) Prevalence of dementia in Egypt: a systematic review. J Neurol Neurosurg Psychiatry 13:715–720. https://doi.org/10.2147/NDT.S127605
Abyad A (2016) Alzheimer’s the Road Ahead in the Middle East. J Alzheimer’s Dis Parkinsonism 6(3):1000241. https://doi.org/10.4172/2161-0460.1000241
Guerriero F, Sgarlata C, Francis M, Maurizi N, Faragli A, Perna S, Rondanelli M, Rollone M, Ricevuti G (2017) Neuroinflammation, immune system and Alzheimer disease: searching for the missing link. Aging Clin Exp Res 29(5):821–831
Sanabria-Castro A, Alvarado-Echeverria I, Monge-Bonilla C (2017) Molecular Pathogenesis of Alzheimer’s Disease: An Update. Ann Neurosci 24(1):46–54. https://doi.org/10.1159/000464422
Selkoe DJ, Hardy J (2016) The amyloid hypothesis of Alzheimer’s disease at 25 years. EMBO Mol Med 8(6):595–608. https://doi.org/10.15252/emmm.201606210
Zhang DD, Lo SC, Cross JV, Templeton DJ, Hannink M (2004) Keap1 is a redox-regulated substrate adaptor protein for a Cul3-dependent ubiquitin ligase complex. Mol Cell Biol 24(24):10941–10953. https://doi.org/10.1128/mcb.24.24.10941-10953.2004
Rajmohan R, Reddy PH (2017) Amyloid-Beta and Phosphorylated Tau Accumulations Cause Abnormalities at Synapses of Alzheimer’s disease Neurons. J Alzheimers Dis 57(4):975–999. https://doi.org/10.3233/JAD-160612
Francis PT, Palmer AM, Snape M, Wilcock GK (1999) The cholinergic hypothesis of Alzheimer’s disease: a review of progress. J Neurol Neurosurg Psychiatry 66(2):137–147
Rodriguez JJ, Noristani HN, Verkhratsky A (2012) The serotonergic system in ageing and Alzheimer’s disease. Prog Neurobiol 99(1):15–41. https://doi.org/10.1016/j.pneurobio.2012.06.010
Bagyinszky E, Youn YC, An SSA, Kim S (2014) The genetics of Alzheimer’s disease. Clin Interv Aging 9:535–551
Sun Y, Luo ZM, Guo XM, Su DF, Liu X (2015) An updated role of microRNA-124 in central nervous system disorders: a review. Front Cell Neurosci 9:193. https://doi.org/10.3389/fncel.2015.00193
Ambati RR, Phang SM, Ravi S, Aswathanarayana RG (2014) Astaxanthin: sources, extraction, stability, biological activities and its commercial applications–a review. Marine drugs 12(1):128–152. https://doi.org/10.3390/md12010128
Tso MO, Lam T-T (1996) Method of retarding and ameliorating central nervous system and eye damage.
Hernández-Marin E, Barbosa A, Martínez A (2012) The metal cation chelating capacity of astaxanthin Does this have any influence on antiradical activity? Molecules 17(1):1039–1054
Ali AA, Ahmed HI, Abu-Elfotuh K (2016) Modeling stages mimic Alzheimer’s disease induced by different doses of aluminum in rats: focus on progression of the disease in response to time. J Alzheimer’s Parkinsonism Dementia 1(1):2
Vorhees CV, Williams MT (2006) Morris water maze: procedures for assessing spatial and related forms of learning and memory. Nat Protoc 1(2):848–858. https://doi.org/10.1038/nprot.2006.116
Balietti M, Giannubilo SR, Giorgetti B, Solazzi M, Turi A, Casoli T, Ciavattini A, Fattorettia P (2016) The effect of astaxanthin on the aging rat brain: gender-related differences in modulating inflammation. J Sci Food Agric 96(2):615–618. https://doi.org/10.1002/jsfa.7131
Ellman GL, Courtney KD, Andres V Jr, Featherstone RM (1961) A new and rapid colorimetric determination of acetylcholinesterase activity. Biochem Pharmacol 7(2):88–95
Udenfriend S, Weissbach H, Brodie BB (1958) Assay of serotonin and related metabolites, enzymes, and drugs. Methods of biochemical analysis:95–130
Osman MY, Osman HM (2008) Inhibitory effect of acetylcholine on monoamine oxidase A and B activity in different parts of rat brain. Arzneimittelforschung 58(10):493–496
Draper HH, Hadley M (1990) Malondialdehyde determination as index of lipid peroxidation. Methods Enzymol 186:421–431
Bancroft JD, Gamble M (2008) Theory and practice of histological techniques. Elsevier health sciences,
Kumar A, Singh A, Ekavali, (2015) A review on Alzheimer’s disease pathophysiology and its management: an update. Pharmacol Rep 67(2):195–203. https://doi.org/10.1016/j.pharep.2014.09.004
Nampoothiri M, John J, Kumar N, Mudgal J, Nampurath GK, Chamallamudi MR (2015) Modulatory role of simvastatin against aluminium chloride-induced behavioural and biochemical changes in rats. Behav Neurol 2015:210169. https://doi.org/10.1155/2015/210169
Rather MA, Thenmozhi AJ, Manivasagam T, Bharathi MD, Essa MM, Guillemin GJ (2018) Neuroprotective role of Asiatic acid in aluminium chloride induced rat model of Alzheimer’s disease. Fronti Biosci (Scholar edition) 10:262–275
Yokel RA (2000) The toxicology of aluminum in the brain: a review. Neurotoxicology 21(5):813–828
Zatta P, Zambenedetti P, Bruna V, Filippi B (1994) Activation of acetylcholinesterase by aluminium (III): the relevance of the metal species. NeuroReport 5(14):1777–1780
Kumar V, Gill KD (2014) Oxidative stress and mitochondrial dysfunction in aluminium neurotoxicity and its amelioration: a review. Neurotoxicology 41:154–166
Kim Y, Olivi L, Cheong JH, Maertens A, Bressler JP (2007) Aluminum stimulates uptake of non-transferrin bound iron and transferrin bound iron in human glial cells. Toxicol Appl Pharmacol 220(3):349–356
Geremia E, Baratta D, Zafarana S, Giordano R, Pinizzotto MR, La Rosa MG, Garozzo A (1990) Antioxidant enzymatic systems in neuronal and glial cell-enriched fractions of rat brain during aging. Neurochem Res 15(7):719–723
Xie H, Hou S, Jiang J, Sekutowicz M, Kelly J, Bacskai BJ (2013) Rapid cell death is preceded by amyloid plaque-mediated oxidative stress. Proc Natl Acad Sci 110(19):7904–7909
Hritcu L, Noumedem JA, Cioanca O, Hancianu M, Kuete V, Mihasan M (2014) Methanolic extract of Piper nigrum fruits improves memory impairment by decreasing brain oxidative stress in amyloid beta (1–42) rat model of Alzheimer’s disease. Cell Mol Neurobiol 34(3):437–449
Cioanca O, Hritcu L, Mihasan M, Hancianu M (2013) Cognitive-enhancing and antioxidant activities of inhaled coriander volatile oil in amyloid β (1–42) rat model of Alzheimer’s disease. Physiol Behav 120:193–202
Ponomarev ED, Veremeyko T, Barteneva N, Krichevsky AM, Weiner HL (2011) MicroRNA-124 promotes microglia quiescence and suppresses EAE by deactivating macrophages via the C/EBP-α–PU 1 pathway. Nat Med 17(1):64
Celada A, Borràs FE, Soler C, Lloberas J, Klemsz M, Van Beveren C, McKercher S, Maki RA (1996) The transcription factor PU 1 is involved in macrophage proliferation. J Experi Med 184(1):61–69
Heneka MT, Carson MJ, El Khoury J, Landreth GE, Brosseron F, Feinstein DL, Jacobs AH, Wyss-Coray T, Vitorica J, Ransohoff RM (2015) Neuroinflammation in Alzheimer’s disease. Lancet Neurol 14(4):388–405
Lukiw WJ (2007) Micro-RNA speciation in fetal, adult and Alzheimer’s disease hippocampus. NeuroReport 18(3):297–300
Fang M, Wang J, Zhang X, Geng Y, Hu Z, Rudd JA, Ling S, Chen W, Han S (2012) The miR-124 regulates the expression of BACE1/beta-secretase correlated with cell death in Alzheimer’s disease. Toxicol Lett 209(1):94–105. https://doi.org/10.1016/j.toxlet.2011.11.032
Gaudet AD, Fonken LK, Watkins LR, Nelson RJ, Popovich PG (2018) MicroRNAs: Roles in Regulating Neuroinflammation. The Neuroscientist 24(3):221–245. https://doi.org/10.1177/1073858417721150
Wang LL, Min L, Guo QD, Zhang JX, Jiang HL, Shao S, Xing JG, Yin LL, Liu JH, Liu R, Guo SL (2017) Profiling microRNA from Brain by Microarray in a Transgenic Mouse Model of Alzheimer’s Disease. Biomed Res Int 2017:8030369. https://doi.org/10.1155/2017/8030369
Sumathi T, Shobana C, Thangarajeswari M, Usha R (2015) Protective effect of L-theanine against aluminium induced neurotoxicity in cerebral cortex, hippocampus and cerebellum of rat brain–histopathological, and biochemical approach. Drug Chem Toxicol 38(1):22–31
Haider S, Liaquat L, Ahmad S, Batool Z, Siddiqui RA, Tabassum S, Shahzad S, Rafiq S, Naz N (2020) Naringenin protects AlCl3/D-galactose induced neurotoxicity in rat model of AD via attenuation of acetylcholinesterase levels and inhibition of oxidative stress. PLoS ONE 15(1):e0227631
Gonçalves PP, Silva VS (2007) Does neurotransmission impairment accompany aluminium neurotoxicity? J Inorg Biochem 101(9):1291–1338
Harsha S, Anilakumar K (2013) Protection against aluminium neurotoxicity: a repertoire of lettuce antioxidants. Biomedicine & Aging Pathology 3(4):179–184
Buraimoh AA, Ojo S, Hambolu J, Adebisi S (2012) Effects of aluminium chloride exposure on the histology of the cerebral cortex of adult Wistar rats. Journal of Biology and Life Science. https://doi.org/10.5296/jbls.v3i1.1421
Slemmer JE, Shacka JJ, Sweeney M, Weber JT (2008) Antioxidants and free radical scavengers for the treatment of stroke, traumatic brain injury and aging. Curr Med Chem 15(4):404–414
Readnower RD, Chavko M, Adeeb S, Conroy MD, Pauly JR, McCarron RM, Sullivan PG (2010) Increase in blood–brain barrier permeability, oxidative stress, and activated microglia in a rat model of blast-induced traumatic brain injury. J Neurosci Res 88(16):3530–3539
Zhang X, Pan L, Wei X, Gao H, Liu J (2007) Impact of astaxanthin-enriched algal powder of Haematococcus pluvialis on memory improvement in BALB/c mice. Environ Geochem Health 29(6):483–489
Wu W, Wang X, Xiang Q, Meng X, Peng Y, Du N, Liu Z, Sun Q, Wang C, Liu X (2014) Astaxanthin alleviates brain aging in rats by attenuating oxidative stress and increasing BDNF levels. Food Funct 5(1):158–166. https://doi.org/10.1039/c3fo60400d
Rahman SO, Panda BP, Parvez S, Kaundal M, Hussain S, Akhtar M, Najmi AK (2019) Neuroprotective role of astaxanthin in hippocampal insulin resistance induced by Aβ peptides in animal model of Alzheimer’s disease. Biomed Pharmacother 110:47–58
Che H, Li Q, Zhang T, Wang D, Yang L, Xu J, Yanagita T, Xue C, Chang Y, Wang Y (2018) Effects of astaxanthin and docosahexaenoic-acid-acylated astaxanthin on Alzheimer’s disease in APP/PS1 double-transgenic mice. J Agri Food Chem 66(19):4948–4957
Chang C-H, Chen C-Y, Chiou J-Y, Peng RY, Peng C-H (2010) Astaxanthine secured apoptotic death of PC12 cells induced by β-amyloid peptide 25–35: its molecular action targets. J Med Food 13(3):548–556
El-Agamy SE, Abdel-Aziz AK, Wahdan S, Esmat A, Azab SS (2018) Astaxanthin Ameliorates Doxorubicin-Induced Cognitive Impairment (Chemobrain) in Experimental Rat Model: Impact on Oxidative, Inflammatory, and Apoptotic Machineries. Mol Neurobiol 55(7):5727–5740. https://doi.org/10.1007/s12035-017-0797-7
Safarova G, Safarov N, Gasanov R (2016) Molecular docking of astaxanthin to monoamine oxidase. Adv Biol Earth Sci 1:45–50
Stahl SM, Felker A (2008) Monoamine oxidase inhibitors: a modern guide to an unrequited class of antidepressants. CNS Spectr 13(10):855–871
Jiang X, Yan Q, Liu F, Jing C, Ding L, Zhang L, Pang C (2018) Chronic trans-astaxanthin treatment exerts antihyperalgesic effect and corrects co-morbid depressive like behaviors in mice with chronic pain. Neurosci Lett 662:36–43. https://doi.org/10.1016/j.neulet.2017.09.064
Goda AA, Naguib KM, Mohamed MM, Amra HA, Nada SA, Abdel-Ghaffar ARB, Gissendanner CR, El Sayed KA (2016) Astaxanthin and Docosahexaenoic Acid Reverse the Toxicity of the Maxi-K (BK) Channel Antagonist Mycotoxin Penitrem A. Marine Drugs 14(11):18. https://doi.org/10.3390/md14110208
Wen X, Huang A, Hu J, Zhong Z, Liu Y, Li Z, Pan X, Liu Z (2015) Neuroprotective effect of astaxanthin against glutamate-induced cytotoxicity in HT22 cells: Involvement of the Akt/GSK-3β pathway. Neuroscience 303:558–568
Hu R, Xu C, Shen G, Jain MR, Khor TO, Gopalkrishnan A, Lin W, Reddy B, Chan JY, Kong A-NT (2006) Gene expression profiles induced by cancer chemopreventive isothiocyanate sulforaphane in the liver of C57BL/6J mice and C57BL/6J/Nrf2 (−/−) mice. Cancer Lett 243(2):170–192
Kanninen K, Malm TM, Jyrkkänen H-K, Goldsteins G, Keksa-Goldsteine V, Tanila H, Yamamoto M, Ylä-Herttuala S, Levonen A-L, Koistinaho J (2008) Nuclear factor erythroid 2-related factor 2 protects against beta amyloid. Mol Cell Neurosci 39(3):302–313
Tripathi DN, Jena GB (2010) Astaxanthin intervention ameliorates cyclophosphamide-induced oxidative stress, DNA damage and early hepatocarcinogenesis in rat: Role of Nrf2, p53, p38 and phase-II enzymes. Mutation Research/Genetic Toxicology and Environmental Mutagenesis 696(1):69–80. https://doi.org/10.1016/j.mrgentox.2009.12.014
Hébert SS, Horré K, Nicolaï L, Papadopoulou AS, Mandemakers W, Silahtaroglu AN, Kauppinen S, Delacourte A, De Strooper B (2008) Loss of microRNA cluster miR-29a/b-1 in sporadic Alzheimer’s disease correlates with increased BACE1/β-secretase expression. Proc Natl Acad Sci 105(17):6415–6420
Acknowledgements
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Funding
No funding was received for conducting this study.
Author information
Authors and Affiliations
Contributions
HA. Hafez was involved in experiments, interpretation of the data, and writing the article. MA.K and MY.O were involved in the design of the experiments, interpretation of the data, and writing the article, HMY. O was involved in experiments, SS.E was involved in the histopathological examination, interpretation of the data, and writing the article, and SA. M was involved in the design of the experiments, data analysis, and writing and revising the article.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare that are relevant to the content of this article.
Ethical approval
Approval was obtained from the Institutional Animal Care And Use Committee (IACUC)-Alexandria University, Egypt (Approval Number: AU0122081232). The study also follows ARRIVE guidelines and complies with the National Research Council’s guide for the care and use of laboratory animals.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hafez, H.A., Kamel, M.A., Osman, M.Y. et al. Ameliorative effects of astaxanthin on brain tissues of alzheimer’s disease-like model: cross talk between neuronal-specific microRNA-124 and related pathways. Mol Cell Biochem 476, 2233–2249 (2021). https://doi.org/10.1007/s11010-021-04079-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-021-04079-4