Abstract
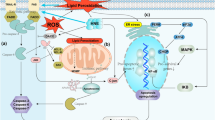
We previously found that homocysteine (Hcy) induced plasma membrane flip-flop, apoptosis, and necrosis in cardiomyocytes. Inactivation of flippase by Hcy induced membrane flip-flop, while apoptosis was induced via a NOX2-dependent mechanism. It has been suggested that S-adenosylhomocysteine (SAH) is the main causative factor in hyperhomocysteinemia (HHC)-induced pathogenesis of cardiovascular disease. Therefore, we evaluated whether the observed cytotoxic effect of Hcy in cardiomyocytes is SAH dependent. Rat cardiomyoblasts (H9c2 cells) were treated under different conditions: (1) non-treated control (1.5 nM intracellular SAH with 2.8 μM extracellular l-Hcy), (2) incubation with 50 μM adenosine-2,3-dialdehyde (ADA resulting in 83.5 nM intracellular SAH, and 1.6 μM extracellular l-Hcy), (3) incubation with 2.5 mM d,l-Hcy (resulting in 68 nM intracellular SAH and 1513 μM extracellular l-Hcy) with or without 10 μM reactive oxygen species (ROS)-inhibitor apocynin, and (4) incubation with 100 nM, 10 μM, and 100 μM SAH. We then determined the effect on annexin V/propodium iodide positivity, flippase activity, caspase-3 activity, intracellular NOX2 and p47phox expression and localization, and nuclear ROS production. In contrast to Hcy, ADA did not induce apoptosis, necrosis, or membrane flip-flop. Remarkably, both ADA and Hcy induced a significant increase in nuclear NOX2 expression. However, in contrast to ADA, Hcy additionally induced nuclear p47phox expression, increased nuclear ROS production, and inactivated flippase. Incubation with SAH did not have an effect on cell viability, nor on flippase activity, nor on nuclear NOX2-, p47phox expression or nuclear ROS production. HHC-induced membrane flip-flop and apoptosis in cardiomyocytes is due to increased Hcy levels and not primarily related to increased intracellular SAH, which plays a crucial role in nuclear p47phox translocation and subsequent ROS production.






Similar content being viewed by others
References
Chao CL, Kuo TL, Lee YT (2000) Effects of methionine-induced hyperhomocysteinemia on endothelium-dependent vasodilation and oxidative status in healthy adults. Circulation 101:485–490
Verhoef P, Stampfer MJ, Buring JE, Gaziano JM, Allen RH, Stabler SP, Reynolds RD, Kok FJ, Hennekens CH, Willett WC (1996) Homocysteine metabolism and risk of myocardial infarction: relation with vitamins B6, B12, and folate. Am J Epidemiol 143:845–859
Wang H, Jiang X, Yang F, Gaubatz JW, Ma L, Magera MJ, Yang X, Berger PB, Durante W, Pownall HJ, Schafer AI (2003) Hyperhomocysteinemia accelerates atherosclerosis in cystathionine beta-synthase and apolipoprotein E double knock-out mice with and without dietary perturbation. Blood 101:3901–3907
Chen C, Halkos ME, Surowiec SM, Conklin BS, Lin PH, Lumsden AB (2000) Effects of homocysteine on smooth muscle cell proliferation in both cell culture and artery perfusion culture models. J Surg Res 88:26–33
Rasmussen LM, Hansen PR, Ledet T (2004) Homocysteine and the production of collagens, proliferation and apoptosis in human arterial smooth muscle cells. APMIS 112:598–604
Heydrick SJ, Weiss N, Thomas SR, Cap AP, Pimentel DR, Loscalzo J, Keaney JF Jr (2004) l-Homocysteine and l-homocystine stereospecifically induce endothelial nitric oxide synthase-dependent lipid peroxidation in endothelial cells. Free Radic Biol Med 36:632–640
Kerkeni M, Tnani M, Chuniaud L, Miled A, Maaroufi K, Trivin F (2006) Comparative study on in vitro effects of homocysteine thiolactone and homocysteine on HUVEC cells: evidence for a stronger proapoptotic and proinflammative homocysteine thiolactone. Mol Cell Biochem 291:119–126
Suhara T, Fukuo K, Yasuda O, Tsubakimoto M, Takemura Y, Kawamoto H, Yokoi T, Mogi M, Kaimoto T, Ogihara T (2004) Homocysteine enhances endothelial apoptosis via upregulation of Fas-mediated pathways. Hypertension 43:1208–1213
Lu SC (2000) S-Adenosylmethionine. Int J Biochem Cell Biol 32:391–395
Rozen R (1996) Molecular genetics of methylenetetrahydrofolate reductase deficiency. J Inherit Metab Dis 19:589–594
Yi P, Melnyk S, Pogribna M, Pogribny IP, Hine RJ, James SJ (2000) Increase in plasma homocysteine associated with parallel increases in plasma S-adenosylhomocysteine and lymphocyte DNA hypomethylation. J Biol Chem 275:29318–29323
Castro R, Rivera I, Martins C, Struys EA, Jansen EE, Clode N, Graca LM, Blom HJ, Jakobs C, Tavares de Almeida I (2005) Intracellular S-adenosylhomocysteine increased levels are associated with DNA hypomethylation in HUVEC. J Mol Med 83:831–836
James SJ, Melnyk S, Pogribna M, Pogribny IP, Caudill MA (2002) Elevation in S-adenosylhomocysteine and DNA hypomethylation: potential epigenetic mechanism for homocysteine-related pathology. J Nutr 132:2361S–2366S
Brandes RP, Schroder K (2008) Differential vascular functions of Nox family NADPH oxidases. Curr Opin Lipidol 19:513–518
Krijnen PA, Meischl C, Hack CE, Meijer CJ, Visser CA, Roos D, Niessen HW (2003) Increased Nox2 expression in human cardiomyocytes after acute myocardial infarction. J Clin Pathol 56:194–199
Meischl C, Krijnen PA, Sipkens JA, Cillessen SA, Munoz IG, Okroj M, Ramska M, Muller A, Visser CA, Musters RJ, Simonides WS, Hack CE, Roos D, Niessen HW (2006) Ischemia induces nuclear NOX2 expression in cardiomyocytes and subsequently activates apoptosis. Apoptosis 11:913–921
Xiao L, Pimentel DR, Wang J, Singh K, Colucci WS, Sawyer DB (2002) Role of reactive oxygen species and NAD(P)H oxidase in alpha(1)-adrenoceptor signaling in adult rat cardiac myocytes. Am J Physiol Cell Physiol 282:C926–C934
Sipkens JA, Krijnen PA, Meischl C, Cillessen SA, Smulders YM, Smith DE, Giroth CP, Spreeuwenberg MD, Musters RJ, Muller A, Jakobs C, Roos D, Stehouwer CD, Rauwerda JA, van Hinsbergh VW, Niessen HW (2007) Homocysteine affects cardiomyocyte viability: concentration-dependent effects on reversible flip-flop, apoptosis and necrosis. Apoptosis 12:1407–1418
Krijnen PA, Sipkens JA, Molling JW, Rauwerda JA, Stehouwer CD, Muller A, Paulus WJ, van Nieuw Amerongen GP, Hack CE, Verhoeven AJ, van Hinsbergh VW, Niessen HW (2010) Inhibition of Rho-ROCK signaling induces apoptotic and non-apoptotic PS exposure in cardiomyocytes via inhibition of flippase. J Mol Cell Cardiol 49:781–790
Sundstrom J, Vasan RS (2005) Homocysteine and heart failure: a review of investigations from the Framingham Heart Study. Clin Chem Lab Med 43:987–992
Verhoeven AJ, Bolscher BG, Meerhof LJ, van ZR, Keijer J, Weening RS, Roos D (1989) Characterization of two monoclonal antibodies against cytochrome b558 of human neutrophils. Blood 73:1686–1694
Afman LA, Blom HJ, Drittij MJ, Brouns MR, van Straaten HW (2005) Inhibition of transmethylation disturbs neurulation in chick embryos. Brain Res Dev Brain Res 158:59–65
Huang Y, Lu ZY, Brown KS, Whitehead AS, Blair IA (2007) Quantification of intracellular homocysteine by stable isotope dilution liquid chromatography/tandem mass spectrometry. Biomed Chromatogr 21:107–112
Daleke DL (2003) Regulation of transbilayer plasma membrane phospholipid asymmetry. J Lipid Res 44:233–242
Doerries C, Grote K, Hilfiker-Kleiner D, Luchtefeld M, Schaefer A, Holland SM, Sorrentino S, Manes C, Schieffer B, Drexler H, Landmesser U (2007) Critical role of the NAD(P)H oxidase subunit p47phox for left ventricular remodeling/dysfunction and survival after myocardial infarction. Circ Res 100:894–903
Qin F, Patel R, Yan C, Liu W (2006) NADPH oxidase is involved in angiotensin II-induced apoptosis in H9C2 cardiac muscle cells: effects of apocynin. Free Radic Biol Med 40:236–246
Reinehr R, Becker S, Braun J, Eberle A, Grether-Beck S, Haussinger D (2006) Endosomal acidification and activation of NADPH oxidase isoforms are upstream events in hyperosmolarity-induced hepatocyte apoptosis. J Biol Chem 281:23150–23166
Heymes C, Bendall JK, Ratajczak P, Cave AC, Samuel JL, Hasenfuss G, Shah AM (2003) Increased myocardial NADPH oxidase activity in human heart failure. J Am Coll Cardiol 41:2164–2171
El-Benna J, Dang PM, Gougerot-Pocidalo MA, Marie JC, Braut-Boucher F (2009) p47phox, the phagocyte NADPH oxidase/NOX2 organizer: structure, phosphorylation and implication in diseases. Exp Mol Med 41:217–225
Raad H, Paclet MH, Boussetta T, Kroviarski Y, Morel F, Quinn MT, Gougerot-Pocidalo MA, Dang PM, El-Benna J (2009) Regulation of the phagocyte NADPH oxidase activity: phosphorylation of gp91phox/NOX2 by protein kinase C enhances its diaphorase activity and binding to Rac2, p67phox, and p47phox. FASEB J 23:1011–1022
Alvarez-Maqueda M, El BR, Monteseirin J, Alba G, Chacon P, Vega A, Santa MC, Tejedo JR, Martin-Nieto J, Bedoya FJ, Pintado E, Sobrino F (2004) Homocysteine enhances superoxide anion release and NADPH oxidase assembly by human neutrophils. Effects on MAPK activation and neutrophil migration. Atherosclerosis 172:229–238
Dalton ML, Gadson PF Jr, Wrenn RW, Rosenquist TH (1997) Homocysteine signal cascade: production of phospholipids, activation of protein kinase C, and the induction of c-fos and c-myb in smooth muscle cells. FASEB J 11:703–711
Loehrer FM, Tschopl M, Angst CP, Litynski P, Jager K, Fowler B, Haefeli WE (2001) Disturbed ratio of erythrocyte and plasma S-adenosylmethionine/S-adenosylhomocysteine in peripheral arterial occlusive disease. Atherosclerosis 154:147–154
Devi S, Kennedy RH, Joseph L, Shekhawat NS, Melchert RB, Joseph J (2006) Effect of long-term hyperhomocysteinemia on myocardial structure and function in hypertensive rats. Cardiovasc Pathol 15:75–82
Castro R, Rivera I, Struys EA, Jansen EE, Ravasco P, Camilo ME, Blom HJ, Jakobs C, Tavares de Almeida I (2003) Increased homocysteine and S-adenosylhomocysteine concentrations and DNA hypomethylation in vascular disease. Clin Chem 49:1292–1296
Acknowledgments
This project was financed by the ICaR-VU (nr. 200370).
Author information
Authors and Affiliations
Corresponding author
Additional information
Jessica A. Sipkens and Paul A. J. Krijnen contributed equally to this manuscript.
Rights and permissions
About this article
Cite this article
Sipkens, J.A., Krijnen, P.A.J., Hahn, N.E. et al. Homocysteine-induced cardiomyocyte apoptosis and plasma membrane flip-flop are independent of S-adenosylhomocysteine: a crucial role for nuclear p47phox . Mol Cell Biochem 358, 229–239 (2011). https://doi.org/10.1007/s11010-011-0973-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-011-0973-4