Abstract
The purpose of the research was an evaluation of removable partial dentures (RPDs) influence on temperature values registered in the area of mental foramen. Initial assumption was made that temperature is proportional to blood flow in mental artery. Additionally, the research objective was an assessment of application of infrared thermovision technique in the field of dental prosthodontics. Two independent groups of patients were examined. Test group consisted of 30 patients using RPD, and control group was composed of 33 patients partially edentulous in mandibular dental arch. The mean age in the test group was 68.8 years, standard deviation (SD) = 10.6, whereas in control group 62.3, SD = 11.9. Temperature values were recorded with thermovision camera. Test group patients underwent two examinations (with denture and 45 min after denture removal), and control group patients were examined once. Results showed decreased temperature values in case of test group patients. The differences were statistically significant (p < 0.05); however, the dentures negative influence was transient as 45 min after RPD removal temperature values were similar in both groups.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Atrophy of maxillary and mandibular alveolar process is the problem frequently occurring in case of the patients undergoing dental prosthodontic and implant prosthodontic treatment. It contributes to deterioration of mastication, changes in face profile and face aesthetics, often causing psychological discomfort.
It is commonly assumed that atrophy is the consequence of teeth extraction (disuse atrophy—atrophia e inactivitate); however, it may be false reasoning, as the presence of teeth does not guarantee atrophy prevention and the extractions itself may cause thrombosis in mandibular artery, resulting in ischaemia and consequently atrophy of alveolar bone. Resorption processes are estimated to be four times more intensive in case of mandible comparing to maxilla [1].
There is a general consensus among dental prosthetics researchers that mucosa-supported removable partial dentures (RPDs) should be used possibly rarely and mainly as the temporary solution due to their influence on stomatognathic system structures. Authors mention increased caries risk, periodontopathy and alveolar bone atrophy. Nevertheless, removable partial dentures are still commonly used in many countries—being often the only economically available solution, financed by the public payer.
The research might contribute to better comprehension of the etiopathogenesis of alveolar bone atrophy as well as influence of RPD use on the atrophy. Discovering the etiopathogenesis of the atrophy would enable introducing adequate prophylaxis, which would be crucial for dental prosthodontic treatment.
Objectives
The aim of the research was evaluation of the influence of using acrylic removable partial dentures on the temperature values registered in mental foramen regions. The assumption was made that the registered temperature is proportional to mandibular blood flow in the region.
Additionally, the research was a pilot study of thermovision use in the field of dental prosthodontics.
Materials and methods
The infrared thermovision is a reliable technique commonly used in the researches in the areas of physiotherapy and general medicine [2–4]. Few studies were performed, using the method in the area of dentistry and in dental prosthodontics particularly [5–9].
The research was performed at the Department of Dental Prosthetics, Wroclaw Medical University, Poland, and was approved by the Bioethical Commission of Wroclaw Medical University.
Skin surface temperature was recorded in the mental regions. The Thermovision A20 camera (Flir Systems, USA) was used. Analysis of the recorded data was performed with ThermaCam Researcher Professional 2.9 software.
The studies were performed in a room with controlled air temperature range: 23–25 °C and a humidity range of 50–70 %. The circulation of air was minimal, and the room was smoke and dust free. Every patient undergone 20-min adaptation period after entering research room. During the thermovision recordings, patients remained in sitting upright position. The distance between the skin surface and the front of the camera was maintained at 2.0 m. The focus of the camera lens was targeted perpendicularly at the mid-point of area examined. The temperatures were recorded in the regions surrounding mental foramen, being the location where inferior alveolar artery leaves mandibular canal and runs superficially on the mandibular bone as mental artery. The examined areas were limited mesially by midline, laterally by the line running straight downwards from cheilion anthropometric point—located at the mouth angle. The upper limit was lower border of rubor labiorum. The lower limit was the lower border of the body of mandible (corpus mandibulae).
Two hundred and seventy curves were recorded on a computer hard disk as graphic files. The temperature scale (21–38 °C) was chosen to enable proper interpretation of the thermograms.
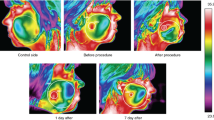
Figure 1 presents exemplary research curve from ThermaCam Researcher Professional 2.9.
The research was conducted in two groups: test group—composed of 30 patients—and control group—composed of 33 patients. Both group patients were partially edentulous in mandible. Test group was composed of 23 female and 7 male patients and control group of 20 and 13 patients, respectively. The mean age in the test group was 68.8 years, standard deviation (SD) = 10.6, whereas in control group 62.3, SD = 11.9. Patients using removable acrylic dentures were classified to the test group. Control group patients were not using dentures. Patients after traumas in the mandible region, cardiac infarction, with diabetes and vascular diseases were excluded from the research as the conditions mentioned above may influence blood flow parameters. Control group patients were examined only once. Test group patients underwent two examinations—first one with the denture present in oral cavity and the second one without the denture (45 min after removing denture). Additionally, general dental examination was made, including missing teeth configuration analysis according to Eichner’s classification and patients’ prosthodontic history.
Statistical analysis was performed with the use of STATISTICA version 10, StatSoft Inc., Tulsa, USA. Mean, minimum and maximum temperature levels and standard deviation were calculated. The statistical analysis of independent groups was based on Student’s t test which is resistant to derogation from the normal distribution. Among dependent groups (repeated examination), adequate t test for dependent groups (test differences) was used. Student’s t tests are resistant to failure to meet the assumptions of normality of the tested variable. The conclusions were also confirmed using the appropriate rank test (Man–Whitney U). As the result of verification of hypotheses was consistent in both tests, the Student’s t test results were finally presented (stronger one). Distribution of results of the dependent variable in each of the analysed groups is close to normal. An amendment to the Student’s t test was included when unfulfilled assumption of homogeneity of variance in the groups (compared by Levene’s test) was found.
To study the relations between variables, Pearson coefficient was used and then assessed by Student’s t test.
For all tests, the level of significance α = 0.05 was used. Tests and coefficients were considered statistically significant if p value was ≤0.05.
Results
In test group, the most common missing teeth configuration according to Eichner’s classification was B4 and C2 classes occurring in case of 37 and 30 % of patients, respectively. In control group, B3 and C2 classes were the most frequent types, occurring in case of 24 % of patients each. The research did not show significant correlations between Eichner class and temperature in analysed areas.
As far as prosthodontic history is concerned, no statistically significant correlations between time of dentures use and registered temperatures were found. The value of correlation coefficient was −0.26 (r-Pearson correlation between time of denture use (years) and mean temperature in test group).
The temperature did not also significantly correlate with patients’ age.
Comparison of the temperatures found in case of test group and control group patients showed statistically significant difference, however, only as far as the measurements with the RPD present in mouth are concerned. The registered temperatures are higher in case of the control group (p < 0.01). The situation changes, however, if the second measurements for the test group are concerned. After 45 min following RPD removal, temperature values in test group and control group were similar—no significant differences were observed. The comparison of first (with denture present in mouth) and second measurements (without denture) in test group showed higher temperature values without RPD in the mouth. See Tables 1–3.
Discussion
The study may contribute to verification of the hypothesis that alveolar process atrophy could result from ischaemia. Results cannot be directly compared to other researchers’ findings as authors were not able to find any similar study conducted before. Eiseman used ultrasound measurements to evaluate mandibular alveolar process blood supply [10]. In the research, blood flow parameters were measured at seven locations: inferior alveolar artery, mental artery, sublingual artery, inferior labial artery, submental artery, greater palatine artery and nasopalatine artery. Signals received by Doppler ultrasound device was divided into three groups: (1) strong pulse—allowing visual registration and measurement of its parameters, (2) undefined pulse—visual and acoustic signals were recorded, but it was not strong enough to measure the parameters and (3) no pulse—patients with reversed blood flow indicating collateral circulation were also qualified to this group. In case of mental artery, the study showed statistically significant difference between patients under and over 65 years old. Strong pulse was found in case of 92 % patients <65 years and 47 % >65 years. In case of sublingual artery, the results were 100 and 65 %, respectively. Though the main objective of the study was enhancing Doppler technique application, it exhibited interesting correlations between blood flow in mandibular vessels and patients’ age. Age-related changes were also object of other authors’ studies [11–13].
In the presented thermovision research, no correlation between age and registered temperatures occurred. Authors are presently conducting further research combining thermovision and Doppler techniques, so that the results could be more relevant.
Registered temperature also did not correlate with time of denture use. Due to multifactorial character of the atrophic processes, the interpretation of the result is difficult. Over 60 factors that may cause atrophy are listed in the studies, and additionally, it is sometimes suggested that the processes are determined individually [14, 15]. Morphology of the face, oral cavity hygiene, occlusal loads, parafunctions, dentures quality, general health condition, nutritional habits, etc. may influence atrophic processes [16–18]. Additionally, the way of denture use should be taken into consideration. Carlsson claims that the process of atrophy is slower in case of patients making night break in denture use [19]. Other researchers contradict these results, suggesting that 24 h a day denture use does not contribute to bone resorption [20]. Xie study leads to interesting conclusion that alcohol intake is favourable to alveolar ridge preservation [18]. In conclusion, conducting a well-designed prospective study would be necessary to obtain more conclusive results.
The results show ambiguous influence of RPDs use on temperature registered around mental foramen. Temperature is higher in control group; however, it reaches similar values in test group in just 45 min after denture removal. Authors performed PubMed analysis, which showed no studies we could compare the results with. Once again if an assumption is made that blood flow parameters correlate with temperature around the artery, we could refer to study performed with Doppler device by Kocabalkan and Turgut [21]. The study concerned influence of soft and hard relining of acrylic complete dentures on mandibular blood flow. Blood flow parameters were measured before prosthodontic treatment and after 1 week, 1, 3, 6 months of denture use. After 1 week, the values were lower than values preceding prosthodontic treatment, but after 6 months they returned to the initial levels. Researches results cannot be directly compared; nevertheless, authors’ conclusions are consistent. In both studies, prosthodontic treatment did not significantly influence registered parameters.
Analysis of numerous articles shows that RPDs are commonly considered a temporary solution and their long-time use should be possibly avoided [22–24]. Authors point out increased caries risk, periodontopathies, alveolar bone atrophy and low patients acceptance. However, as far as ischaemic etiopathogenesis of alveolar bone atrophy is concerned, our preliminary results do not confirm negative RPDs influence. Nevertheless once again the necessity for further research should be underlined.
Conclusions
-
1.
The influence of RPDs use on temperature values recorded in mental foramen area is negative, but transient. RPDs use causes decrease in temperature, however, only when the denture is present in oral cavity. Temperatures return to the values similar to control group in 45 min after denture removal.
-
2.
Thermovision is a non-invasive technique whose application in the field of dental prosthodontics seems promising, especially in research area; however, further studies should be performed.
References
Cawood JI, Howell RA. Reconstructive preprosthetic surgery. I. Anatomical considerations. Int J Oral Maxillofac Surg. 1991;20:75.
Cholewka A, Drzazga Z, Sieron A, Stanek A. Thermovision diagnostics in chosen spine diseases treated by whole body cryotherapy. J Therm Anal Calorim. 2010;102:113–9.
Cholewka A, Stanek A, Klimas A, Sieron A, Drzazga Z. Thermal imaging application in chronic venous disease. J Therm Anal Calorim. 2014;11:1609–18.
Ratajczak B, Boerner E. Application of thermovision in assessment of superficial tissue temperature changes under the influence of 1 and 3 MHz ultrasounds wave. J Therm Anal Calorim. 2015;120:269–75.
Al-Qudah AA, Mitchell CA, Biagioni PA, Hussey DL. Thermographic investigation of contemporary resin-containing dental materials. J Dent. 2005;33:593–602.
Benington IC, Biagioni PA, Crossey PJ, Hussey DL, Sheridan S, Lamey PJ. Temperature changes in bovine mandibular bone during implant site preparation: an assessment using infra-red thermography. J Dent. 1996;24:263–7.
Fornaini C, Merigo E, Vescovi P, Bonanini M, Antonietti W, Leoci L, Lagori G, Meleti M. Different laser wavelengths comparison in the second-stage implant surgery: an ex vivo study. Lasers Med Sci. 2014. [Epub ahead of print].
Gratt BM, Sickles EA, Ross JB, Wexler CE, Gornbein JA. Thermographic assessment of craniomandibular disorders: diagnostic interpretation versus temperature measurement analysis. J Orofac Pain. 1994;8:278–88.
Fikackova H, Ekberg E. Can infrared thermography be a diagnostic tool for arthralgia of the temporomandibular joint? Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2004;98:643–50.
Eiseman B, Johnson L, Coll J. Ultrasound measurement of mandibular arterial blood supply: techniques for defining ischemia in the pathogenesis of alveolar ridge atrophy and tooth loss in the elderly? Oral Maxillofac Surg. 2005;63:28–35.
Bradley J. Age changes of the inferior alveolar artery. Br J Maxillofac Surg. 1988;26:517–22.
Castelli WA, Najlet C, Diaz Perez R. Interruption of the arterial inferior alveolar flow and its effect on mandible collateral circulation and distal tissue. J Dent Res. 1975;54:708–14.
Heasman P, Adamson J. An investigation of possible age-related changes in the inferior alveolar artery in man. Br J Oral Maxillofac Surg. 1987;25:406–11.
Woelfel JB, Winter CM, Igarashi T. Five-year cephalometric study of mandibular ridge resorption with different posterior occlusal forms. Part I. Denture construction and initial comparison. J Prosthet Dent. 1976;36:602–23.
Reddy MS, Geurs NC, Wang IC. Mandibular growth following implant restoration: does Wolff’s law apply to residual ridge resorption? Int J Periodontics Restor Dent. 2002;22:315–21.
Douglass JB, Meader L, Kaplan A. Cephalometric evaluation of the changes in patients wearing complete dentures: a 20-year study. J Prosthet Dent. 1993;69:270–5.
Carlsson GE. Responses of jawbone to pressure. Gerodontology. 2004;21:65–70.
Xie Q, Ainamo A, Tilvis R. Association of residual ridge resorption with systemic factors in the homeliving elderly subjects. Acta Odontol Scand. 1997;55:299–305.
Carlsson GE, Persson G. Morphologic changes of the mandible after extraction and wearing of dentures. Odontol Rev. 1967;18:27–54.
Kalk W, de Baat C. Some factors connected with alveolar bone resorption. J Dent. 1989;17:162–5.
Kocabalkan E, Turgut M. Variation in blood flow of supporting tissue during use of mandibular complete dentures with hard acrylic resin base and soft relining: a preliminary study. Int J Prosthodont. 2005;18:210–3.
Eckert SE. Time to bid adieu to removable dental prostheses. Int J Oral Maxillofac Implant. 2014;29:535–40.
Wöstmann B, Budtz-Jørgensen E, Jepson N, Mushimoto E, Palmqvist S, Sofou A, Owall B. Indications for removable partial dentures: a literature review. Int J Prosthodont. 2005;18:139–45.
Preshaw PM, Walls AW, Jakubovics NS, Moynihan PJ, Jepson NJ, Loewy Z. Association of removable partial denture use with oral and systemic health. J Dent. 2011;11:711–9.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Bartczyszyn, M., Demidaś, A. & Więckiewicz, W. Evaluation of temperature values in mental foramen area in case of patients using removable partial dentures. J Therm Anal Calorim 123, 2207–2211 (2016). https://doi.org/10.1007/s10973-015-5000-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10973-015-5000-7