Abstract
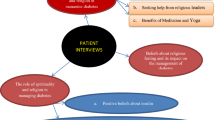
This study aims to reveal the feelings, difficulties, attitudes, and spiritual coping status of Turkish patients with Type 2 diabetes mellitus toward fasting during Ramadan. The sample of this descriptive qualitative study consists of 14 patients diagnosed with Type 2 diabetes. We determined two main themes and relevant sub-themes. The first was “the feelings and difficulties experienced due to diabetes mellitus" with the sub-themes of "negative emotions" and “difficulties in fasting." The second theme was identified as "religious and spiritual coping" with the sub-themes of "believing the disease comes from God," “having difficulty in adhering to disease-specific practices while fasting," and "feeling that fasting facilitates coping and provides relief." In conclusion, it was determined that the patients continued to fast despite the difficulties and that fasting facilitated coping and provided relaxation.

Similar content being viewed by others
References
Abid, M., Hsairi, M., Elleuch, M., & Ben, A. E. (2018). Survey on diabetic patients treated with insulin during the fasting month of Ramadan. International Journal of General Medicine, 11, 33–40. https://doi.org/10.2147/IJGM.S131308
Ahmad, A., Khan, M. U., & Aslani, P. (2021). The role of religion, spirituality and fasting in coping with diabetes among Indian migrants in Australia: A qualitative exploratory study. Journal of Religion and Health. https://doi.org/10.1007/s10943-021-01438-9
Al-Arouj, M., Khalil, S. A., Buse, J., Fahdil, I., Fahmy, M., Hafez, S., et al. (2010). Recommendations for management of diabetes during ramadan: Update 2010. Diabetes Care, 33(8), 1895–1902. https://doi.org/10.2337/dc10-0896
Aravind, S. R., Tayeb, H. A., İsmail, S. B., Shehadeh, N., Kaddaha, G., Liu, R., et al. (2011). Hypoglycaemia in sulphonylurea-treated subjects with type 2 diabetes undergoing ramadan fasting: A five-country observational study. Current Medical Research and Opinion, 27(6), 1237–1242. https://doi.org/10.1185/03007995.2011.578245
Arifin, B., Probandari, A., Purba, A. K. R., Perwitasari, D. A., Veninga, C. C. M. S., Atthobari, J., et al. (2020). Diabetes is a gift from God’ a qualitative study coping with diabetes distress by Indonesian outpatients. Quality of Life Research, 29(1), 109–125. https://doi.org/10.1007/s11136-019-02299-2
Arli, K. S., Bakan, A. B., & Erisik, E. (2016). An investigation of the relationship between nurses views on spirituality and spiritual care and their level of burnout. Journal of Holistic Nursing, 30(201), 1–7. https://doi.org/10.1177/0898010116652974
Azizi, F. (2002). Research in islamic fasting and health. Annals of Saudi Medicine, 22(3–4), 186–191. https://doi.org/10.5144/0256-4947.2002.186
Baek, R. N., Tanenbaum, M. L., & Gonzalez, J. S. (2014). Diabetes burden and diabetes distress: The buffering effect of social support. Annals of Behavioral Medicine, 48(2), 145–155. https://doi.org/10.1007/s12160-013-9585-4
Bahijri, S., Borai, A., Ajabnoor, G., Khalig, A. A., AlQassas, I., Shehri, D. A., et al. (2013). Relative metabolic stability, but disrupted circadian cortisol secretion during the fasting month of ramadan. PLoS ONE, 8(4), 1–6. https://doi.org/10.1371/journal.pone.0060917
Bener, A., Hamak, A. O. A., Öztürk, M., Çatan, F., Haris, P. I., Rajput, K. U., et al. (2018). Effect of ramadan fasting on glycemic control and other essential variables in diabetic patients. Annals of African Medicine, 17(4), 196–202. https://doi.org/10.4103/aam.aam_63_17
Berenguera, A., Inesta, A. M., Cases, M. M., Nadal, J. F., Bolibar, B., Rubinat, E., et al. (2016). Understanding the physical, social, and emotional experiences of people with uncontrolled Type 2 diabetes: A qualitative study. Patient Preference and Adherence, 10, 2323–2332. https://doi.org/10.2147/PPA.S116173
Berg, B. L., & Lune, H. (2012). Qualitative research methods for social sciences (8th edn.). Boston, MA: Pearson Education.
Bonakdaran, S. H., & Dalouie, M. K. (2011). The effects of fasting during ramadan on glycemic excursions detected by continuous glucose monitoring system (CGMS) in patients with type 2 diabetes. Medical Journal of Malaysia, 66(5), 447–450. PMID: 22390099.
Buono, J. L., Carson, R. T., & Flores, N. M. (2017). Health-related quality of life, work productivity, and indirect costs among patients with irritable bowel syndrome with diarrhea. Health and Quality of Life Outcomes, 15(1), 35. https://doi.org/10.1186/s12955-017-0611-2
Centers for Disease Control and Prevention (CDC). (2020). National Diabetes Statistics Report, 2020. Atlanta, GA: Centers for Disease Control and Prevention, U.S. Dept of Health and Human Services.
Chamberlain, J. J., Rhinehart, A. S., Shaefer, C. F., & Neuman, A. (2016). Diagnosis and management of diabetes: Synopsis of the 2016 American Diabetes Association Standards of Medical Care in Diabetes. Annals of Internal Medicine, 164(8), 542–552. https://doi.org/10.7326/M15-3016
Çelik, S., Pinar, R., Üzüm, A. K., & Salman, S. (2013). Effects of ramadan fasting on daily life and metabolic condition in patients with type 2 diabetes. Turkiye Klinikleri Journal of Medical Sciences, 33(5), 1266–1273. https://doi.org/10.5336/medsci.2012-33028
Devlin, H., Roberts, M., Okaya, A., & Xiong, Y. M. (2006). Our lives were healthier before: Focus groups with African American, American Indian, Hispanic/Latino, and Hmong People With Diabetes. Health Promotion Practice, 7(1), 47–55. https://doi.org/10.1177/1524839905275395
Funa, A. N., Muilenburg, J., & Wilson, M. (2013). The role of religion and spirituality in coping with type 2 diabetes: A qualitative study among black men. Journal of Religion and Health, 54(1), 242–252. https://doi.org/10.1007/s10943-013-9812-0
Graneheim, U. H., & Lundman, B. (2004). Qualitative content analysis in nursing research: Concepts, procedures and measures to achieve trustworthiness. Nurse Education Today, 24(2), 105–112. https://doi.org/10.1016/j.nedt.2003.10.001
Hamid, A. M. E., Ghaleb, M., Aljadhey, H., & Aslanpour, Z. (2017). Factors contributing to medicine-related problems in adult patients with diabetes and/or cardiovascular diseases in Saudi Arabia: A qualitative study. British Medical Journal Open, 7(11), 1–8. https://doi.org/10.1136/bmjopen-2017-017664
Haouari, M., Oukerre, F. H., Sfaxi, A., Rayana, M. C. H. B., Kaabachi, N., & Mbazaa, A. (2008). How ramadan fasting affects caloric consumption, body weight, and circadian evolution of cortisol serum levels in young, healthy male volunteers. Hormone and Metabolic Research, 40(8), 575–577. https://doi.org/10.1055/s-2008-1065321
Hassanein, M., Echtay, A. S., Malek, R., Omar, M., Saikh, S. S., Ekelund, M., et al. (2018). Original paper: Efficacy and safety analysis of insulin degludec/insulin aspart compared with biphasic insulin aspart 30: A Phase 3, multicentre, international, open-label, randomised, treat-to-target trial in patients with type 2 diabetes fasting during. Diabetes Research and Clinical Practice, 135, 218–226. https://doi.org/10.1016/j.diabres.2017.11.027
Haydardedeoğlu, F. E., Bağır, G. Ş, & Özşahin, A. K. (2019). Impact of fasting during Ramadan in patients with type 2 diabetes mellitus. Cukurova Medical Journal, 44(3), 758–763. https://doi.org/10.17826/cumj.496374
Hernandez, M. R. (2016). Religiosity, social support and care associated with health in older Mexicans with diabetes. Journal of Religion and Health, 55(4), 1394–1410. https://doi.org/10.1007/s10943-015-0105-7
How, C. B., Ming, K. E., & Chin, C. Y. (2011). Does religious affiliation influence glycaemic control in primary care patients with type 2 diabetes mellitus? Mental Health in Family Medicine, 8(1), 21–28. PMID: 22479289.
IDF Diabetes Atlas. (2019). 463 million people living with diabetes. Ninth edition. https://diabetesatlas.org/upload/resources/material/20200302_133351_IDFATLAS9e-final-web.pdf
Jaleel, M. A., Raza, S. A., Fathima, F. N., & Jaleel, B. N. F. (2011). Ramadan and diabetes: As-saum (the fasting). Indian Journal of Endocrinology and Metabolism, 15(4), 268–273. https://doi.org/10.4103/2230-8210.85578
Kalra, S., Jena, B. N., & Yeravdekar, R. (2018). Emotional and psychological needs of people with diabetes. Indian Journal of Endocrinology and Metabolism, 22(5), 696–704. https://doi.org/10.4103/ijem.IJEM_579_17
Khan, N. B., Khan, M. H., Shaikh, M. Z., Khanani, M. R., & Rasheed, A. (2012). Effects of ramadan fasting and physical activity on glucose levels and serum lipid profile among type 2 diabetic patients. Pakistan Journal of Medical Sciences, 28(1), 91–96.
Koenig, H. G., Cohen, H. J., Blazer, D. G., Pieper, C., Meador, K. G., Shelp, F., et al. (1992). Religious coping and depression in elderly hospitalized medically ill men. American Journal of Psychiatry, 149(12), 1693–1700. https://doi.org/10.1176/ajp.149.12.1693
Koenig, H. G., George, L. K., Titus, P., & Meador, K. G. (2004). Religion, spirituality, and acute care hospitalization and long-term care use by older patients. Archives of Internal Medicine, 164(14), 1579–1585. https://doi.org/10.1001/archinte.164.14.1579
Lee, J. Y., Wong, C. P., Tan, C. S. S., Nasir, N. H., & Lee, S. W. H. (2017). Type 2 diabetes patient’s perspective on Ramadan fasting: A qualitative study. BMJ Open Diabetes Research and Care, 5(1), 1–6. https://doi.org/10.1136/bmjdrc-2016-000365
Leininger, M. (1998). Qualitative research methods in nursing. Greyden Press.
Li, C., Ford, E. S., Zhao, G., Balluz, L. S., Berry, J. T., & Mokdad, A. H. (2010). undertreatment of mental health problems in adults with diagnosed diabetes and serious psychological distress: The Behavioral risk factor surveillance system, 2007. Diabetes Care, 33(5), 1061–1064. https://doi.org/10.2337/dc09-1515
Lynch, C. P., Hernandez-Tejada, M. A., Strom, J. L., & Egede, L. E. (2012). Association between spirituality and depression in adults with type 2 diabetes. The Diabetes Educator, 38(3), 427–435. https://doi.org/10.1177/0145721712440335
Mohamed, M. A. R., Gida, N. I. M., & Sobeh, D. E. S. (2019). Experiences and needs of patients with type 2 diabetes during ramadan: A qualitative study. Journal of Diabetes Nursing, 23(6), 1–7.
Naeem, A. G. (2003). The role of culture and religion in the management of diabetes: A Study of Kashmiri men in leeds. Journal of the Royal Society for the Promotion of Health, 123(2), 110–116. https://doi.org/10.1177/146642400312300216
Nageeb, S., Vu, M., Malik, S., Quinn, M. T., Cursio, J., & Padela, A. I. (2018). Adapting a religious health fatalism measure for use in Muslim populations. PLoS ONE, 13(11), 1–12. https://doi.org/10.1371/journal.pone.0206898
Newlin, K., Melkus, G. D., Tappen, R., Chyun, D., & Koenig, H. G. (2008). Relationships of religion and spirituality to glycemic control in black women with type 2 diabetes. Nursing Research, 57(5), 331–339. https://doi.org/10.1097/01.NNR.0000313497.10154.66
Patel, N. R., Kennedy, A., Blickem, C., Rogers, A., Reeves, D., & Graham, C. C. (2015). Having diabetes and having to fast: A qualitative study of British Muslims with diabetes. Health Expectations, 18(5), 1698–1708. https://doi.org/10.1111/hex.12163
Péres, D. S., Santos, M. A., Zanetti, M. L., & Ferronato, A. A. (2007). Difficulties of diabetic patients in the illness control: Feelings and behaviors. Revista Latino-Americana de Enfermagem, 15(6), 1105–1112. https://doi.org/10.1590/s0104-11692007000600008
Permana, I., Ormandy, P., & Ahmed, A. (2019). Maintaining harmony: How religion and culture are interwoven in managing daily diabetes self-care. Journal of Religion and Health, 58(4), 1415–1428. https://doi.org/10.1007/s10943-019-00819-5
Petznick, A. M. (2013). Identifying and addressing barriers to insulin acceptance and adherence in patients with type 2 diabetes mellitus. The Journal of the American Osteopathic Association, 113(4 Suppl 2), 6–16. https://doi.org/10.1007/s12325-009-0061-2
Quinn, M. T., Cook, S., Nash, K., & Chin, M. H. (2001). Adressing religion and spirituality in African Americans with diabetes. The Diabetes Educator, 27(5), 643–655. https://doi.org/10.1177/014572170102700505
Reach, G., Consoli, S. M., Halimi, S., Colas, C., Duclos, M., Fontaine, P., et al. (2015). The multinational second diabetes, attitudes, wishes and needs study: Results of the French survey. Patient Preference and Adherence, 9, 289–297. https://doi.org/10.2147/PPA.S68941
Rushforth, B., McCrorie, C., Glidewell, L., Midgley, E., & Foy, R. (2016). Barriers to effective management of type 2 diabetes in primary care: Qualitative systematic review. British Journal of General Practice, 66(643), 114–127. https://doi.org/10.3399/bjgp16X683509
Rowe, M., & Allen, R. G. (2004). Spirituality as a means of coping with chronic illness. American Journal of Health Studies, 19(1), 62–67.
Salti, I., Benard, E., Detournay, B., Biscay, M. B., Brigand, C. L., Voinet, C., et al. (2004). A population-based study of diabetes and its characteristics during the fasting month of ramadan in 13 countries: Results of the Epidemiology of Diabetes and Ramadan 1422/2001 (EPIDIAR) Study. Diabetes Care, 27(10), 2306–2311. https://doi.org/10.2337/diacare.27.10.2306
Satman, I., Omer, B., Tutuncu, Y., Kalaca, S., Gedik, S., Dinccağ, N., et al. (2013). Twelve-year trends in the prevalence and risk factors of diabetes and prediabetes in Turkish adults. European Journal of Epidemiology, 28(2), 169–180. https://doi.org/10.1007/s10654-013-9771-5
Savaş, E. (2018). Attitudinal determinants of Turkish diabetic patients and physicians about ramadan fasting. Journal of Religion and Health, 57(1), 47–56. https://doi.org/10.1007/s10943-016-0327-3
Schneider, A., Rosenberger, S., Bobardt, J., Bungartz-Catak, J., Atmann, O., Haller, B., et al. (2017). Self-help guidebook improved quality of life for patients with irritable bowel syndrome. PLoS ONE, 12(7), e0181764. https://doi.org/10.1371/journal.pone.0181764
Siaw, M. Y. L., Chew, D. E. K., Dalan, R., Kader, S. A., Shakoor, K. A., Othman, N., et al. (2014). Evaluating the effect of ramadan fasting on Muslim patients with diabetes in relation to use of medication and lifestyle patterns: A prospective study. International Journal of Endocrinology, 2014, 1–7. https://doi.org/10.1155/2014/308546
Smith, K. J., Beland, M., Clyde, M., Gariépy, G., Page, V., Badawi, G., et al. (2013). Association of diabetes with anxiety: A systematic review and meta-analysis. Journal of Psychosomatic Research, 74(2), 89–99. https://doi.org/10.1016/j.jpsychores.2012.11.013
Tong, A., Sainsbury, P., & Craig, J. (2007). Consolidated criteria for reporting qualitative research (COREQ): A 32-item checklist for interviews and focus groups. International Journal for Quality in Health Care, 19(6), 349–357. https://doi.org/10.1093/intqhc/mzm042
Unantenne, N., Warren, N., Canaway, R., & Manderson, L. (2013). The strength to cope: Spirituality and faith in chronic disease. Journal of Religion and Health, 52(4), 1147–1161. https://doi.org/10.1007/s10943-011-9554-9
Underwood, L. G. (2000). A working model of health: Spirituality and religiousness as resources: Applications to persons with disability. Journal of Religion, Disability and Health, 3(3), 51–71. https://doi.org/10.1300/J095v03n03_05
Watkins, Y. J., Quinn, L. T., Ruggiero, L., Quinn, M. T., & Choi, Y. K. (2013). Spiritual and religious beliefs and practices and social support’s relationship to diabetes self-care activities in African Americans. The Diabetes Educator, 39(2), 231–239. https://doi.org/10.1177/0145721713475843
Yazla, E., Karadere, M. E., Küçükler, F. K., Karşıdağ, Ç., İnanç, L., Kankoç, E., et al. (2018). The effect of religious belief and forgiveness on coping with diabetes. Journal of Religion and Health, 57(3), 1010–1019. https://doi.org/10.1007/s10943-017-0504-z
Yılmaz, M., Gün, M., & Yaman, Z. (2019). Emotions, thoughts and experiences of diabetes patients: A qualitative study. International Journal of Caring Sciences, 12(3), 1806–1814.
Zareipour, M., Khazir, Z., Valizadeh, R., Mahmoodi, H., & Ghojogh, M. G. (2016). The association between spiritual health and blood sugar control in elderly patients with type 2 diabetes. Elderly Health Journal, 2(2), 67–72.
Acknowledgments
The authors would like to thank the volunteering patients who devoted their time for this research.
Funding
The authors received no financial support for the conduct, authorship, and/or publication of this article.
Author information
Authors and Affiliations
Contributions
All authors are in agreement with the content of the manuscript. Study conception and design were contributed by YA, SPK. Data collection, statistical expertise, analysis and interpretation of data were contributed by YA, SPK. Manuscript preparation, supervision, administrative support and critical revision of the paper were contributed by YA, SPK. YA, SPK contributed to final approval of the version to be published.
Corresponding author
Ethics declarations
Conflict of interest
The authors did not have any conflict of interest with regard to the author and/or publication of this article. No financial support was received for the research and/or writing of this article.
Ethical Approval
The study was approved by the Ethics Committee of the Medical Faculty of Kafkas University. Written permission was obtained from the institutions, and verbal and written informed consent was obtained from those who had agreed to participate.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Akkuş, Y., Kiliç, S.P. Feelings, Difficulties and Attitudes in relation to Fasting: A Qualitative Study on Spiritual Coping Among Turkish Patients with Type 2 Diabetes. J Relig Health 62, 4382–4398 (2023). https://doi.org/10.1007/s10943-022-01713-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10943-022-01713-3