Abstract
Disturbances in emotion regulation among opioid users receiving methadone maintenance treatment (MMT) was reported in a few small studies. We aimed to evaluate the prevalence and characteristics of patients in MMT with impaired emotion regulation. We studied a cross-sectional sample of 121 patients by means of the Difficulties in Emotion Regulation Scale (DERS). Data on clinical, sociodemographic and addiction variables were reviewed, including results of random observed urine testing for opioids, alcohol, cocaine, cannabis, and benzodiazepine (BDZ). The prevalence of a high DERS score (> 90) was 39%. Characteristics associated with high DERS scores (logistic regression model) were benzodiazepine misuse and 20 years of opioid use before admission to MMT. Among the subscales, IMPULSE and STRATEGIES were independently related to substance use (logistic regression). Greater cocaine usage was also more prevalent only in univariate analyses. The DERS score correlated inversely with years of education among patients with negative urine test. The DERS subscale score for AWARENESS was lower in females than in males as among patients with suicide attempts or involvement in physical violence. Since the IMPULSE and STRATEGIES scores predict drug use, these aspects of emotional regulation should be targeted first in third-wave cognitive-behavioral intervention in MMT.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The term “emotional regulation” has received considerable attention in the literature over the last few decades (Sheppes et al., 2015; Weiss et al., 2022). In fact, it has become an integral research topic across various areas of psychology, including biological, cognitive, social, developmental, clinical and health branches (Gross, 2014). Emotions are a set of physiological, cognitive, behavioral and subjective reactions, which are the result of an automatic/unconscious, or conscious evaluation of either an internal or external stimulus, framed within the context and goals of a given moment in life (Murphy & Young, 2018). This process is guided by a positive or negative assessment that an individual makes of the situation, when a positive assessment will determine the frequent appearance of the behavior, while a negative assessment will be integrated, in order to avoid similar contexts (Cotrufo & Bares, 2018).
Emotion regulation changes throughout the lifespan, and it should be noted that at all ages, emotions and their regulation cannot be understood outside of their social context (Cole, 2014). Emotion regulation capacities are acquired throughout childhood and puberty when adult caregivers serve as important models in shaping children’s ability to process and manage their emotions (Maughan & Cicchetti, 2002). From infancy to adolescence, there is development of executive functions, cognitive complexity, and emotion understanding which are vital for monitoring and evaluating one’s emotional reactions (Thompson, 2011), and individuals become more aware of their emotions, as well as of the importance of planning long-term goals (Zimmermann et al., 2014). Throughout life, individuals are often required to use emotion regulation skills, and Helion et al. (2019) noted that being able to flexibly regulate one’s emotions is critical for adaptive functioning across the life span.
Two decades ago, Gratz and Roemer (2004) proposed that emotional regulation is composed of four elements: (a) awareness and understanding of emotions, (b) acceptance of emotions, (c) the ability to control impulses and behave in accordance with goals in the presence of negative affect, and (d) access to emotion regulation strategies that are perceived to be effective for feeling better. They also published a questionnaire they termed Difficulties in Emotion Regulation Scale (DERS) which was designed to measure emotion regulation problems (Gratz & Roemer, 2004). The article which presented this model and validated the DERS has been cited more than 11,000 times to date, and translated into several languages as well.
A substantial body of research has shown positive associations between high total scores on the DERS and psychopathology. Specifically, high DERS scores were associated with generalized anxiety disorder (Mennin et al., 2002), social anxiety (Rusch et al., 2012), post-traumatic stress disorder (Ehring & Quack, 2010), borderline personality disorder (Gratz et al., 2006), and bipolar disorder (Van Rheenen et al., 2015).
Similarly, a significant number of studies indicated positive associations between high DERS scores and substance use. Specifically, a robust association has been found between high DERS scores and alcohol use among community samples (Roeser et al., 2019), and clinical samples (Brem et al., 2021). Regarding the association between DERS scores and opioid use, studies yielded mixed results; while in some studies, high DERS scores were associated with greater risk of opioid misuse (Lutz et al., 2018), and also with opioid-related problems in chronic pain patients (Rogers et al., 2020), in other study among individuals admitted to a residential substance use disorder (SUD) treatment, high DERS scores were not associated with opioid misuse (Richmond et al., 2020).
The few studies which examined the association between DERS scores and misuse of sedative medications clearly indicated that difficulties in emotion regulation are positively associated with nonprescription sedative use in patients admitted to residential SUD treatment (Richmond et al., 2020), as well as with benzodiazepine use disorder in treatment-seeking individuals with alcohol use disorder (Cavicchioli, 2019). Likewise, individuals with cocaine use disorder reported significant difficulties in emotion regulation (Tull et al., 2016). In this context, Fox et al. (2007) found that individuals with cocaine dependence reported difficulties relating to understanding emotions, managing emotions and impulse control in the first week of abstinence compared to a community control group. Interestingly, with continued abstinence, those individuals showed continued difficulties only in impulse control (Fox et al., 2007).
A thorough examination of the academic literature on the relationship between DERS scores and substance use among methadone maintenance patients (MMT) revealed that it has received somewhat less attention than the relationship between DERS scores and substance use in community samples. A study conducted among methadone maintenance patients (MMT) found that among the varied dimensions of emotion regulation difficulties, only the nonacceptance of emotional responses (meaning negative reactions to one’s own negative emotions or nonacceptance of emotional distress) was uniquely predictive of coping motives for substance use (Gold et al., 2020). However, that study included 68 participants, and the authors noted that they cannot be certain that this sample size is highly representative of the broader demographic of opioid users. Azizi et al. (2019) found higher scores on all the DERS subscales among MMT patients in comparison with controls, but their study also included a relatively a small number of both MMT patients (n = 43) and controls (n = 45).
In the current study, we studied a correctional representative large number of MMT patients to examine the association between emotional regulation difficulties and substance use. The objectives of this exploratory study were therefore two-folded: (1) to examine the characteristics of MMT patients with high DERS scores; and (2) to determine whether high DERS scores are associated positively with substance use among the patients. Our hypothesis was that patients who use substances, will have higher DERS scores than patients who do not use substances.
Method
Participants
Overall, 121 (92 males and 29 females) patients participated in this study. The average age of the participants was 54.41 years (SD = 10.26), with a mean of 10.13 years of education (SD = 3.2). Ninety nine patients defined themselves as Jewish, 17 as Christian, and 5 as Muslims.
Measures
Difficulties in Emotion Regulation Scale (DERS; Gratz & Roemer, 2004) The DERS is a 36-item self-report questionnaire designed to assess multiple aspects of emotional dysregulation. The measure yields a total score as well as scores on the six subscales derived through factor analysis: Nonacceptance of emotional responses (NONACCEPTANCE), difficulties in engaging in goal-directed behavior (GOALS), impulse control difficulties (IMPULSE), lack of emotional awareness (AWARENESS), limited access to emotion regulation strategies (STRATEGIES), and lack of emotional clarity (CLARITY). The items are statements to which the individual responds according to a five-point Likert scale whose response options range from “almost never” (0–10%) to “almost always (91–100%). Scores are presented as a total score as well as a separate score for each of the six subscales. Higher scores suggest greater problems with emotion regulation. Salters-Pedneault et al. (2006) reported good internal consistency for the total score (α = .89) and for the subscale scores (α = .77). In the current study, Cronbach’s alpha for the total score was (α = .95) NONACCEPTANCE (α = .85), GOALS (α = .74), IMPULSE (α = .89), STRATEGIES (α = .90), CLARITY (α = .82) and AWARENESS (α = .55).
The DERS has no cutoff which distinguishes between effective and non-effective emotional regulation. In a study among adults presenting at an outpatient clinic diagnosed with one or more DSM-5 disorders, Hallion et al. (2018) found that the mean of the total score of the DERS was 89.3 (SD = 22.6). Since studies among MMT patients report high rates of psychiatric comorbidity (Carpentier et al., 2009; Zhu et al., 2021), we used this score as a cutoff for examining differences between the patients.
Urine Toxicology
At least two randomized observed urine tests per month were provided by each study participant throughout their entire course of treatment. All urine samples were analyzed for opioids, cocaine metabolite (benzoylecgonine), benzodiazepines (BDZ), cannabis (THC), alcohol, methadone or its metabolite and amphetamines. A positive result was defined by at least one of the urine samples testing positive for the substance one month before filling-in the questionnaires.
Demographics and History of Addiction
Data on demographics and history of addiction were collected as part of the routine intake interview, which is conducted at each patient’s entrance to treatment (Modified ASI Questionnaire – McLellan et al., 1984).
Procedure
The study was approved by the institutional Helsinki Committee (IRB) of the Tel-Aviv Sourasky Medical Center (TASMC) (0657 − 20). Following the approval,
of the total of 330 patients enrolled in our MMT clinic in November 2021, 157 were randomly selected to participate in the study. The included patients met the criteria similar to those of the U.S. Federal Regulations for entering methadone treatment (i.e., DSM-5 criteria of dependence with multiple self-administrations of heroin per day for at least one year), adults (18 years of age or above), and with two failed trials of institutional detoxification and abstinence programs (a specific request of the Israeli Ministry of Health. There were no exclusion criteria.
Of the 157 selected patients, 121 participated (77.1%). Thirty six did not participate due to various reasons; eight patients had died before filling-in the questionnaire, one was incarcerated, and five dropped out of treatment. The first author (DP), approached the patients, and presented them with information about the study’s aim and importance. Twenty two patients refused, yielding an 89.3% compliance rate for the 135 eligible patients. After having signed their informed consent, the DERS was administered to the patients, and substance use was recorded during the month prior to filling-in the questionnaire.
Statistical Analysis
Statistical analyses were performed using the SPSS-22 package. Results were compared by means of the Chi-square or Fisher’s exact test for categorical variables and one-way analysis of variance (ANOVA) for continuous variables. Correlations between continuous variables were carried out with the Pearson correlation coefficient, and those between categorical and continuous variables were by biserial correlations. A logistic regression multivariance analysis models to characterize patients with high DERS (≥ 90) scores, and to characterize patients with any substance, were used, and included all the variables that were found to be significantly (p < 0.05) in the univariate analyses. The adequacy of the model was determined with the Hosmer and Lemeshow goodness-of-fit test (Chi-square = 0.4, p = 0.7) and (Chi-square = 8.8, p = 0.4) respectively (Hosmer and Lemeshow, 1980).
Results
Comparison Between Patients Who Participated in the Study and Those Who Did Not
More of the non-participants tested positive to cannabis compared to the participants (16.7% vs. 4.1%, respectively, p(chi square = 6.7) = 0.001). The non-participants did not differ from the participants in the rate of involvement in physical violence (40% vs. 48.7%, p(chi square = 0.8) = 0.44), suicide attempts (37.1% vs. 24.3%, p(chi square = 2.12) = 0.19), self-harm (17.1% vs. 27.8%, p(chi square = 1.6) = 0.26), and victim of rape (20% vs. 12.3%, p(chi square = 1.3) = 0.27).
Difficulties in Emotion Regulation Scale
The mean total DERS score of the entire study group was 86.2 (SD = 27.9). The mean scores of the DERS subscales were: 13.3 (SD = 5.8) for NON-ACCEPTANCE, 14.7 (SD = 5.1) for GOALS, 13.9 (SD = 6.6) for IMPULSE, 15.9 (SD = 3.5) for AWARENESS, 18.1 (SD = 7.8) for STRATEGIES, and 11.1 (SD = 4.6) for CLARITY. The mean total score of the male population did not differ significantly from the female population [87.8 (SD = 27.8) and 80.1 (SD = 28.3), F = 1.3, p = 0.251, respectively]. The mean DERS scores did not differ by years of education, ethnic origin, marital status (alone or in a relationship), age of opioid use onset, route of substance use (injecting and non-injecting), trauma related to a history of involvement in physical violence, suicide attempts, self-harm or victim of rape.
However, in a comparison of the DERS’s subscales scores by gender, only the differences in the AWARENESS subscale were found significant, as males scored higher than females [16.5 (SD = 3.4) and 14.1 (SD = 3.3), F = 11.5, p < 0.0001]. The AWARENESS subscale score was also significantly lower among the 28 patients (24.3%) who had history of suicide attempts compared to those without such history (14.3 ± 3.4 vs. 16.4 ± 3.5, p(F = 7.8) = 0.006). A suicide attempt history was twice as prevalent among females (39.3%) compared to males (19.5%, p = 0.04). Specifically, the males who had a history of suicide attempt scored lower than those with no history of suicide attempt (14.6 ± 2.9 vs. 17 ± 3.4, p=(F = 7)0.01), while there were no comparable differences among the females (13.9 ± 4.1 vs. 14.2 ± 2.9, p = 0.8). The AWARENESS score was also significantly lower for the 56 patients who were involved in physical violence (15.2 ± 3.7 vs. 16.6 ± 3.3, p(F = 4.3) = 0.04), with no sex-related difference.
DERS Scores and Substance Use
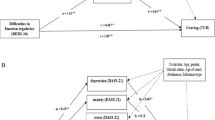
The total DERS score was significantly higher in the 38 patients with positive urine tests for any substance use compared to the 83 patients who tested negative for any substance use (111.4 ± 27.7 VS. 74.5 ± 19.1, F = 72.2, respectively, p = 0.001). Similarly, the subscale scores of patients with positive tests for any substance use were significantly higher than those of patients with negative tests for any substance use (Fig. 1). The specific scores were as follows: NONACCEPTANCE (18.1 ± 5.9 VS. 11.2 ± 4.3, F = 51.3, p = 0.001), GOALS (18.1 ± 5.4 VS. 13.1 ± 4.3, F = 31.4, p = 0.001), IMPULSE (19.4 ± 6.8 VS. 11.4 ± 4.6, F = 57.1, p = 0.001), AWARENESS (17.3 ± 3.8 VS. 15.3 ± 3.1, F = 9.4, p = 0.003), STRATEGIES (24.8 ± 7.9 VS. 15.08 ± 5.57, F = 59.9p = 0.001), and CLARITY (14.3 ± 4.6 VS. 9.6 ± 3.7, F = 72.4, p = 0.001). Urine analysis showed that only four patients used alcohol. None of the subscales also differed by any other sociodemographic or addiction variables (data not shown), including trauma from a history of involvement in physical violence, suicide attempts, self-harm or victim of rape.
Characteristics of High DERS Scores
Using a cutoff score of 90 (DERS ≥ 90), we compared 47 patients with high DERS scores to 74 patients who had a lower DERS score (Table 1). High DERS score had higher duration of opioids use, higher methadone dose, any substance use, and specifically cocaine use and BDZ misuse.
Linear Correlation
The total DERS score linearly correlated with age at admission to treatment (R = 0.26, p = 0.01), and with current age (R = 0.35, p = 0.001) for the 83 patients with positive urine tests for any substance use. In the 38 patients with negative urine tests for any substance use, the total DERS score correlated linearly with the methadone dose (R = 0.37, p = 0.02), and inversely with years of education (R = -0.41, p = 0.01) (Table 2).
Multivariate Analyses
The presence of a DERS score ≥ 90 (using logistic regression) was significantly more likely to be associated with BDZ misuse (Odds Ratio (OR) = 61.8, 95% Confidence Interval (CI) 7.5–507.8, p = 0.001), and with 20 years of opioid use before being admitted to MMT (OR = 2.8, 95% CI 1–7.5, p = 0.03).
To examine which of the subscales is mostly related to substance use, a logistic regression with no vs. any substance use as dependent variable, and all variables that significantly (p < 0.05) differed in univariate analyses was performed. Specifically, we included all the six DERS subscales and the variable having children (22(57.9%) of any substance vs. 67(77.9%) of no use group, p = 0.03), and self-harm (15(42.9%) of any substance vs. 17(20.2%) of no use group, p = 0.02), were included.
The presence of any substance use was significantly more likely to be associated with IMPULSE (OR = 1.0, 95% CI 1.0–1.3, p = 0.054) and with STRATEGIES (OR = 1.1, 95% CI 1.0–1.3, p = 0.014).
Discussion
The current study analyzes the relationship between difficulties in emotion regulation and substance use among MMT patients. The first objective of the study was to examine the characteristics of individuals with high DERS scores (DERS score > 90). We demonstrated that the 39% of the sample that had high DERS scores, were characterized as having an average of 20 years of opioid use, were maintained on a high methadone dose, had any substance use, used cocaine, and misused BDZ. The first central finding of this study concerns the association between difficulties in emotion regulation and many years of opioid use before admission to MMT. This finding is in line with other studies among individuals who used opioids for prolonged periods, which indicated ineffective emotion regulation strategies, with a possible explanation that opioid use may occasion top-down deficits in emotional regulation (Ding et al., 2021; Hudak et al., 2022).
The second central finding of this study concerns the positive association between high DERS score (DERS score > 90) and high methadone dose.
Maremmani et al. (2019) suggested that high methadone dose seemed to be related to psychopathological symptomatology, unexpressed aggression, irritability and violence, and that it may have a mood stabilization effect. This explanation is supported by studies indicating that MMT patients with depression, receive higher methadone doses (Malik et al., 2019; Peles et al., 2007).
A third finding of this study relates to the positive association between high DERS score (DERS score > 90) and any substance use, cocaine use, and BDZ misuse. Previous studies among MMT patients suggested that there is a subgroup in this population that uses illicit substances and misuses medications with dependence potential despite the treatment (Potik et al., 2020; Rutherford et al., 1999). Those studies suggested that this subgroup is characterized by high psychopathy level, any substance use, cocaine use, and BDZ misuse, and perhaps significant deficits in emotional regulation is additional characteristic of this subgroup.
A fourth finding of this study concerns a positive correlation between high DERS score and older age. This finding is in line with a similar finding of a meta-analysis that found that most aspects of negative emotion regulation abilities were more strongly related to substance use by older adults (Weiss et al., 2022). There are few possible explanations for this finding. First, older MMT patients are characterized by a non-stable financial status, as their income comes either from invalidity pensions or social benefits (Gutiérrez-Cáceres, 2023), and studies found that low income is associated with deficits in self-regulation (Raver, 2004; Zvolensky et al., 2017). A second possible explanation concerns the mental and physical health of MMT patients. Meaning, older MMT patients suffer from depression and anxiety disorders (Rosen et al., 2008), and studies indicate that difficulties in emotion regulation are associated with these mental conditions (Campbell-Sills & Barlow, 2007; Hofmann et al., 2012).
A fifth finding of this study which relates to demographics concerns the inverse correlation between the high DERS score (DERS score > 90) among patients with negative urine tests for any substance use and years of education. A possible explanation or this finding is that schooling is an emotionally laden process for students (Schutz et al., 2006), and emotions are intimately involved in learning processes and achievement (Pekrun & Linnenbrink-Garcia, 2012; Schutz & Pekrun, 2007). Therefore, individuals with lower education levels will have more difficulties in emotional regulation. Studies across various ages indicated that emotion regulation is positively associated with higher levels of education and academic success (Boekaerts & Pekrun, 2015; Graziano et al., 2007).
A sixth finding of our study concerns the significant association between higher DERS score with age at admission to MMT treatment. In this study, we found that one of the characteristics of patients with high DERS score involves 20 years average of opioid use, and it has been suggested that opioid use may occasion top-down deficits in emotional regulation (Ding et al., 2021; Hudak et al., 2022). Meaning, individuals who enter methadone programs at an older age have deficits in emotion regulation as well as many years of opioid use.
In this context, it should be noted that an alternative explanation to the emotional regulation deficits in MMT patients as well as in individuals who chronically use substance concerns brain atrophy (Hampton et al., 2019). Specifically, individuals with chronic opioid use have variable degrees of cerebral atrophy, when both age and the duration are correlated to each other and are significantly associated with cerebral atrophy (Singla et al., 2020). Another explanation for the findings of the current study may be due to the co-occurrence of traumatic brain injury (TBI) and prolonged substance use (Miller & Adams, 2005), as both of these phenomena are associated with risky behaviors, diminished inhibitory results, impaired executive functioning, and impulsivity (Huhn et al., 2019; Olson-Madden, 2012).
The second objective of this study was to determine whether high DERS scores are associated with substance use in among MMT patients. In accordance with our hypothesis, we found that higher DERS scores were positively associated with any substance use, opioid use, cocaine use, THC use and BDZ misuse, while lower DERS scores were associated with substance abstinence. In other words, higher DERS scores were associated with polysubstance use in MMT patients. Since we could not compare this finding to other studies among MMT patients, we looked at studies among individuals who used various substances. Two large meta-analyses which examined the association between emotion regulation and substance use clearly showed that difficulties in emotion regulation and substance use are significantly related, and that individuals with substance use disorder (SUD) diagnosis are characterized by polysubstance use (Stellern et al., 2023; Weiss et al., 2022).
A possible explanation is that MMT patients constitute socioeconomically.
disadvantaged population that suffers from high rates of mental distress (Harris et al., 2006; Potik et al., 2014), and individuals with deficits in emotion regulation who experience distress from a wider range of sources, may use different substances to modulate the psychic pain associated with these unique experiences (Potik, 2021; Weiss et al., 2022). In other words, difficulties in emotion regulation are related significantly to polysubstance use both in individuals with SUD and also in MMT patients.
In the current study, the presence of a high DERS score (DERS ≥ 90) was significantly more likely to be associated with BDZ misuse. This not surprising finding is consistent with the literature. BDZ misuse in MMT has been a well-documented problem for years (Gelkopf et al., 1999; Peles et al., 2014), with possible hazardous consequences, such as overdoses and concurrent substance use (Brands et al., 2008; Oliver et al., 2007). However, only few studies offered possible solutions (Potik et al., 2020).
Although all the subscales were associated with any substance use, only the IMPULSE and the STRATEGIES subscales were predictive of substance use. Interestingly, this finding also corresponds with that of two large meta-analyses which showed that individuals with SUDs demonstrated poorer emotion regulation skills, when the largest deficits are in impulsivity and maladaptive strategies (Stellern et al., 2023; Weiss et al., 2022). Impulsivity appears to function as both a determinant and a consequence of substance use (De Wit, 2009), so there is not an unambiguous explanation for this finding. Thus, a recent study in MMT patients found that they were characterized by a faster, but more inaccurate response style than the controls, suggesting a specific motoric inhibition deficit following a buildup of cortical preparedness (Weidacker et al., 2023).
Regarding the association between the STRATEGIES subscale and substance use, the STRATEGIES subscale assesses whether an individual feels that he has healthy approaches to manage distress (Gratz & Roemer, 2004), and studies showed that perceived stress in MMT patients was associated positively and significantly with cocaine use, as well as BDZ misuse (Moitra et al., 2013). Meaning, MMT patients who lack healthy approaches to manage stress turn to substance use to regulate their emotions.
An interesting finding of the current study is the sex-related differences in the scores of the AWARENESS subscale. This subscale represents the tendency to attend to and acknowledge emotions, as well as awareness of one’s emotional responses (Gratz & Roemer, 2004). In our study, male patients with either positive or negative urine tests for any substance use had significantly higher scores on the AWARENESS subscale compared to female patients with either positive or negative urine tests for substance use. This subscale measures the tendency to attend and acknowledge emotions (Gratz & Roemer, 2004), and a possible explanation for this finding is that women have advantage over males in emotion recognition (Abbruzzese et al., 2019; Demenescu et al., 2014).
A prior study in MMT population did not report any similar sex-related differences (Azizi et al., 2019), although the study that operationalized the DERS found sex-related differences for only the AWARENESS subscale (Gratz & Roemer, 2004). Specifically, the men had significantly higher scores than the women, suggesting that men reported lower levels of emotional awareness than women. The same pattern was also observed in a Greek validation study of the DERS, wherein men and women differed only in the AWARENESS subscale and produced comparable scores on all the other dimensions (Mitsopoulou et al., 2013). However, this finding is not consistent, and therefore Giromini et al. (2017) recommended retaining the parameter of sex in the equation formulas for determining the adjusted, normative reference scores for the DERS.
Additional interesting findings concerning the AWRENESS subscale were related to suicidality. For example, like in community samples (Bommersbach et al., 2022), women were more likely to attempt suicide than men. Studies among women in MMT patients indicate that they have higher depression rates than men, and that depression is a risk factor for suicide (Chen et al., 2020; Peles et al., 2007).
A surprising finding concerned the significantly lower scores on the AWARENESS subscale among patients who were involved in physical violence, in comparison to those who were not involved in such behavior. It should be noted that the information concerning the history of physical violence relates to the patients’ history prior starting treatment. Meaning, all patients fill the modified ASI questionnaire upon admission to the clinic, and therefore the reports on involvement in physical violence refer to the time during which they used substance and were not enrolled in any treatment program.
A possible explanation for the association between greater emotional awareness and violence may relate to efficacy of the psychosocial treatment in MMT.
Kalantarkousheh et al. (2015) found that MMT patients had better emotion regulation skills than controls, and explained that the first have available psychological services. In accordance with this explanation, Potik et al. (2020) suggested that individual psychotherapy (Potik et al., 2007), and group psychotherapy (Potik et al., 2011) can lead to behavioral changes in MMT patients.
Our study adds also significant knowledge concerning the psychometric properties of the DERS. We want to emphasize that the AWARENESS subscale had the relatively poor internal consistency in comparison to the other subscales. The AWARENESS subscale had also shown relatively poor psychometric properties in other studies (Hallion et al., 2018; Osborne et al., 2017), and some researchers found that a five-factor DERS model (exclusion of the AWARENESS factor) to be equivalent to the original six-factor DERS model (Bardeen et al., 2012; Fowler et al., 2014). Therefore, future studies in MMT patients should use a five-factor DERS model to examine if it has better psychometric features.
Finally, the DERS score relies upon a theoretical model which has its roots in the “third-wave cognitive-behavioral therapies (CBT)” (Hallion et al., 2018). The term third-wave CBT refers to a group of psychological therapies that target the process of thoughts rather than their content, helping people to become aware of their thoughts and to accept them in a non-judgmental way (Churchill et al., 2013). Third-wave methods emphasize such issues as mindfulness, emotions, acceptance, values, goals and meta‐cognition (Hayes & Hofmann, 2017). These models and intervention approaches include acceptance and commitment therapy (Hayes et al., 2013), dialectical behavior therapy (Linehan, 1993), mindfulness‐based cognitive therapy (Teasdale et al., 1995) and several others.
Third-wave CBT treatments have been found to be promising complementary therapies for individuals who use substances (Balandeh et al., 2021), including MMT patients (Cooperman et al., 2019; Hayes et al., 2004; Stotts et al., 2012). One of the most meaningful findings of this study concerns the significance of IMPULSE and STRSTAGIES in predicting substance use. Therefore, treatment interventions in MMT settings should target these emotional regulation aspects first.
Limitations
The study has three main limitations. The first relates to its cross-sectional design. Although such studies examine causal associations, the evidence for causality is typically not all conclusive (Savitz & Wellenius, 2023). Therefore, future research in MMT should include administration of the DERS at the beginning of treatment and include follow-up. Second, emotional regulation difficulties are related to psychopathology and stress (Sheppes et al., 2015), and the current study did not measure these variables. Since MMT patients are characterized by high levels of psychopathology and stress (Jaremko et al., 2015; Potik et al., 2014), future studies should assess psychopathology next to emotion regulation. A third limitation concerns the use of self-reports measures in some patients who do not have high emotional awareness, and a possible influence on the results. A possible solution is administration of the questionnaire by a researcher, who makes sure that the participants understand the questions of this measure.
Data Availability
The data that support the findings of this study are not openly available due to reasons of sensitivity and are available from the corresponding author upon reasonable request. Data are located in controlled access data storage at the Adelson clinic.
References
Abbruzzese, L., Magnani, N., Robertson, I. H., & Mancuso, M. (2019). Age and gender differences in emotion recognition. Frontiers in Psychology, 10, 2371. https://doi.org/10.3389/fpsyg.2019.02371
Azizi, S., Maghsoudloo, A., & Baheshmat, S. (2019). Comparison of coping strategies and emotion regulation tendencies among opium users, methadone maintenance treatment clients and normal individuals. Journal of Research and Health, 9(6), 533–543.
Balandeh, E., Omidi, A., & Ghaderi, A. (2021). A narrative review of third-wave cognitive behavioral therapies in addiction. Addiction and Health, 13(1), 52–65. https://doi.org/10.22122/ahj.v13i1.298
Bardeen, J. R., Fergus, T. A., & Orcutt, H. K. (2012). An examination of the latent structure of the difficulties in emotion regulation scale. Journal of Psychopathology and Behavioral Assessment, 34, 382–392. https://doi.org/10.1007/s10862-012-9280-y
Boekaerts, M., & Pekrun, R. (2015). Emotions and emotion regulation in academic settings. In L. Corno, & E. M. Anderson (Eds.), Handbook of educational psychology (pp. 90–104). Routledge.
Bommersbach, T. J., Rosenheck, R. A., Petrakis, I. L., & Rhee, T. G. (2022). Why are women more likely to attempt suicide than men? Analysis of lifetime suicide attempts among US adults in a nationally representative sample. Journal of Affective Disorders, 311, 157–164. https://doi.org/10.1016/j.jad.2022.05.096
Brands, B., Blake, J., Marsh, D. C., Sproule, B., Jeyapalan, R., & Li, S. (2008). The impact of benzodiazepine use on methadone maintenance treatment outcomes. Journal of Addictive Diseases, 27(3), 37–48. https://doi.org/10.1080/10550880802122620
Brem, M. J., Stuart, G. L., Cornelius, T. L., & Shorey, R. C. (2021). A longitudinal examination of alcohol problems and cyber, psychological, and physical dating abuse: The moderating role of emotion dysregulation. Journal of Interpersonal Violence, 36(19–20), NP10499–NP10519. https://doi.org/10.1177/0886260519876029
Campbell-Sills, L., & Barlow, D. H. (2007). Incorporating emotion regulation in to conceptualizations and treatments of anxiety and mood disorders. In J. J. Gross (Ed.), Handbook of emotion regulation (pp. 542–559). Guilford.
Carpentier, P. J., Krabbe, P. F., van Gogh, M. T., Knapen, L. J., Buitelaar, J. K., & de Jong, C. A. (2009). Psychiatric comorbidity reduces quality of life in chronic methadone maintained patients. The American Journal on Addictions, 18(6), 470–480. https://doi.org/10.3109/10550490903205652
Cavicchioli, M., Prudenziati, F., Movalli, M., Ramella, P., & Maffei, C. (2019). The severity of personality pathology: A risk factor for concurrent substance use disorders in alcohol use disorder. Journal of Dual Diagnosis, 15(3), 159–171. https://doi.org/10.1080/15504263.2019.1612131
Chen, W. T., Wang, S. C., Wang, I. A., Tsay, J. H., & Chen, C. Y. (2020). Suicide attempts and death among heroin-involved women seeking methadone treatment in Taiwan. Drug and Alcohol Dependence, 217, 108277. https://doi.org/10.1016/j.drugalcdep.2020.108277
Churchill, R., Moore, T. H., Furukawa, T. A., Caldwell, D. M., Davies, P., Jones, H., Shinohara, K., Imai, H., Lewis, G., & Hunot, V. (2013). Third wave’ cognitive and behavioural therapies versus treatment as usual for depression. The Cochrane Database of Systematic Reviews, (10). https://doi.org/10.1002/14651858.CD008705.pub2
Cole, P. M. (2014). Moving ahead in the study of the development of emotion regulation. International Journal of Behavioral Development, 38(2), 203–207. https://doi.org/10.1177/0165025414522170
Cooperman, N. A., Rizvi, S. L., Hughes, C. D., & Williams, J. M. (2019). Field test of a dialectical behavior therapy skills training-based intervention for smoking cessation and opioid relapse prevention in methadone treatment. Journal of Dual Diagnosis, 15(1), 67–73. https://doi.org/10.1080/15504263.2018.1548719
Cotrufo, T., & Bares, J. M. U. (2018). O cérebro e as emoções: sentir, pensar, decidir. In A. C. Caldas (Ed.), Neurociência & Psicologia (pp. 1–144). Atlântico Press I.
Demenescu, L. R., Mathiak, K. A., & Mathiak, K. (2014). Age- and gender-related variations of emotion recognition in pseudowords and faces. Experimental Aging Research, 40(2), 187–207. https://doi.org/10.1080/0361073X.2014.882210
de Wit H. (2009). Impulsivity as a determinant and consequence of drug use: a review of underlying processes. Addiction Biology, 14(1), 22–31. https://doi.org/10.1111/j.1369-1600.2008.00129.x
Ding, X., Jiang, H., Xu, M., Li, Y., Liang, J., & Xie, R. (2021). The ineffective emotion regulation strategies of heroin use disorder patients: An event-related potential study. Drug and Alcohol Dependence, 228, 109076. https://doi.org/10.1016/j.drugalcdep.2021.109076
Ehring, T., & Quack, D. (2010). Emotion regulation difficulties in trauma survivors: The role of trauma type and PTSD symptom severity. Behavior Therapy, 41,(4), 587–598.
Fowler, J. C., Charak, R., Elhai, J. D., Allen, J. G., Frueh, B. C., & Oldham, J. M. (2014). Construct validity and factor structure of the difficulties in emotion regulation scale among adults with severe mental illness. Journal of Psychiatric Research, 58, 175–180. https://doi.org/10.1016/j.jpsychires.2014.07.029
Fox, H. C., Axelrod, S. R., Paliwal, P., Sleeper, J., & Sinha, R. (2007). Difficulties in emotion regulation and impulse control during cocaine abstinence. Drug and Alcohol Dependence, 89(2–3), 298–301. https://doi.org/10.1016/j.drugalcdep.2006.12.026
Gelkopf, M., Bleich, A., Hayward, R., Bodner, G., & Adelson, M. (1999). Characteristics of benzodiazepine abuse in methadone maintenance treatment patients: A 1 year prospective study in an Israeli clinic. Drug and Alcohol Dependence, 55(1–2), 63–68. https://doi.org/10.1016/S0376-8716(98)00175-6
Giromini, L., Ales, F., De Campora, G., Zennaro, A., & Pignolo, C. (2017). Developing age and gender adjusted normative reference values for the difficulties in emotion regulation scale (DERS). Journal of Psychopathology and Behavioral Assessment, 39(4), 705–714.
Gold, A. K., Stathopoulou, G., & Otto, M. W. (2020). Emotion regulation and motives for illicit drug use in opioid-dependent patients. Cognitive Behaviour Therapy, 49(1), 74–80. https://doi.org/10.1080/16506073.2019.1579256
Gratz, K. L., & Roemer, L. (2004). Multidimensional assessment of emotion regulation and dysregulation: Development, factor structure, and initial validation of the difficulties in emotion regulation scale. Journal of Psychopathology and Behavioral Assessment, 26(1), 41–54.
Gratz, K. L., Rosenthal, M. Z., Tull, M. T., Lejuez, C. W., & Gunderson, J. G. (2006). An experimental investigation of emotion dysregulation in borderline personality disorder. Journal of Abnormal Psychology, 115(4), 850–855.
Graziano, P. A., Reavis, R. D., Keane, S. P., & Calkins, S. D. (2007). The role of emotion regulation and children’s early academic success. Journal of School Psychology, 45(1), 3–19. https://doi.org/10.1016/j.jsp.2006.09.002
Gross, J. J. (Ed.). (2014). Handbook of emotion regulation (2nd ed.).). The Guilford Press.
Gutiérrez-Cáceres, S., Serrano-Gallardo, P., & Pedraz Marcos, A. (2023). Older adult in methadone treatment: Socio-economic status and chronicity. Health and Addictions / Salud Y Drogas, 23(1), 183–202. https://doi.org/10.21134/haaj.v23i1.726
Hallion, L. S., Steinman, S. A., Tolin, D. F., & Diefenbach, G. J. (2018). Psychometric properties of the difficulties in emotion regulation scale (DERS) and its short forms in adults with emotional disorders. Frontiers in Psychology, 9, 539. https://doi.org/10.3389/fpsyg.2018.00539
Hampton, W. H., Hanik, I. M., & Olson, I. R. (2019). Substance abuse and white matter: Findings, limitations, and future of diffusion tensor imaging research. Drug and Alcohol Dependence, 197, 288–298. https://doi.org/10.1016/j.drugalcdep.2019.02.005
Harris, K. A., Jr, Arnsten, J. H., Joseph, H., Hecht, J., Marion, I., Juliana, P., & Gourevitch, M. N. (2006). A 5-year evaluation of a methadone medical maintenance program. Journal of Substance Abuse Treatment, 31(4), 433–438. https://doi.org/10.1016/j.jsat.2006.05.018
Hayes, S. C., & Hofmann, S. G. (2017). The third wave of cognitive behavioral therapy and the rise of process-based care. World Psychiatry, 16(3), 245–246. https://doi.org/10.1002/wps.20442
Hayes, S. C., Levin, M. E., Plumb-Vilardaga, J., Villatte, J. L., & Pistorello, J. (2013). Acceptance and commitment therapy and contextual behavioral science: Examining the progress of a distinctive model of behavioral and cognitive therapy. Behavior Therapy, 44(2), 180–198. https://doi.org/10.1016/j.beth.2009.08.002
Hayes, S. C., Wilson, K. G., Gifford, E. V., Bissett, R., Piasecki, M., Batten, S. V., Byrd, M., & Gregg, J. (2004). A preliminary trial of twelve-step facilitation and acceptance and commitment therapy with polysubstance-abusing methadone-maintained opiate addicts. Behavior Therapy, 35(4), 667–688. https://doi.org/10.1016/S0005-7894(04)80014-5
Helion, C., Krueger, S. M., & Ochsner, K. N. (2019). Emotion regulation across the life span. In J. W. Swanson & M. Matharu (Eds.), Handbook of clinical neurology (257–280). https://doi.org/10.1016/B978-0-12-804281-6.00014-8. PMID: 31590734.
Hofmann, S. G., Sawyer, A. T., Fang, A., & Asnaani, A. (2012). Emotion dysregulation model of mood and anxiety disorders. Depression and Anxiety, 29(5), 409–416. https://doi.org/10.1002/da.21888
Hosmer, D. W., & Lemesbow, S. (1980). Goodness of fit tests for the multiple logistic regression model. Communications in Statistics - Theory and Methods, 9(10), 1043–1069. https://doi.org/10.1080/03610928008827941
Hudak, J., Bernat, E. M., Fix, S. T., Prince, K. C., Froeliger, B., & Garland, E. L. (2022). Neurophysiological deficits during reappraisal of negative emotional stimuli in opioid misuse. Biological Psychiatry, 91(12), 1070–1078. https://doi.org/10.1016/j.biopsych.2022.01.019
Huhn, A. S., Brooner, R. K., Sweeney, M. M., Yip, S. W., Ayaz, H., & Dunn, K. E. (2019). Increased neural activity in the right dorsolateral prefrontal cortex during a risky decision-making task is associated with cocaine use in methadone-maintained patients. Drug and Alcohol Dependence, 205, 107650. https://doi.org/10.1016/j.drugalcdep.2019.107650
Jaremko, K. M., Sterling, R. C., & Van Bockstaele, E. J. (2015). Psychological and physiological stress negatively impacts early engagement and retention of opioid-dependent individuals on methadone maintenance. Journal of Substance Abuse Treatment, 48(1), 117–127. https://doi.org/10.1016/j.jsat.2014.08.006
Kalantarkousheh, D., & Godini, A. (2015). Cognitive emotion regulation strategies among regular persons and participants in methadone or Narcotics Anonymous treatment programs. Studies in Social Sciences and Humanities, 2(3), 131–138.
Linehan, M. M. (1993). Cognitive-behavioral treatment of borderline personality disorder. Guilford Press.
Lutz, J., Gross, R. T., & Vargovich, A. M. (2018). Difficulties in emotion regulation and chronic pain-related disability and opioid misuse. Addictive Behaviors, 87, 200–205. https://doi.org/10.1016/j.addbeh.2018.07.018
Malik, E., Adelson, M., Sason, A., Schreiber, S., & Peles, E. (2019). Outcome of patients with high depressive symptoms on admission to methadone maintenance treatment. Journal of Dual Diagnosis, 15(4), 281–290. https://doi.org/10.1080/15504263.2019.1656353
Maremmani, A. G. I., Pacini, M., & Maremmani, I. (2019). What we have learned from the methadone maintenance treatment of dual disorder heroin use disorder patients. International Journal of Environmental Research and Public Health, 16(3), 447. https://doi.org/10.3390/ijerph16030447
Maughan, A., & Cicchetti, D. (2002). Impact of child maltreatment and interadult violence on children’s emotion regulation abilities and socioemotional adjustment. Child Development, 73(5), 1525–1542.
McLellan, A. T., Luborsky, L., O’Brien, C. P., Barr, H. L., & Evans, F. (1984). The addiction severity index in three different populations. NIDA Research Monograph, 55, 217–223.
Mennin, D. S., Fresco, D. M., Heimberg, R. G., Schneier, F. R., Davies, S. O., & Liebowitz, M. R. (2002). Screening for social anxiety disorder in the clinical setting: Using the Liebowitz Social anxiety scale. Journal of Anxiety Disorders, 16(6), 661–673.
Miller, N. S., & Adams, B. S. (2005). Alcohol and drug disorders. In: J. M. Silver & T. W. McAllister & S. C. Yudofsky (Eds.), Textbook of traumatic brain injury American Psychiatric.
Mitsopoulou, E., Kafetsios, K., Karademas, E., Papastefanakis, E., & Simos, P. (2013). The Greek version of the difficulties in emotion regulation scale: Testing the factor structure, reliability and validity in an adult community sample. Journal of Psychopathology and Behavioral Assessment, 35(1), 123–131. https://doi.org/10.1007/s10862-012-9321-6
Moitra, E., Anderson, B. J., & Stein, M. D. (2013). Perceived stress and substance use in methadone-maintained smokers. Drug and Alcohol Dependence, 133(2), 785–788. https://doi.org/10.1016/j.drugalcdep.2013.08.010
Murphy, J., & Young, M. A. (2018). Dynamic processes in emotion regulation choice. Cognition and Emotion, 32(8), 1654–1662. https://doi.org/10.1080/02699931.2017.1419935
Oliver, P., Forrest, R., & Keen, J. (2007). Benzodiazepines and cocaine as risk factors in fatal opioid overdoses. National Treatment Agency for Substance Misuse (Research Briefing No. 3. (.
Olson-Madden, J. H., Brenner, L. A., Corrigan, J. D., Emrick, C. D., & Britton, P. C. (2012). Substance use and mild traumatic brain injury risk reduction and prevention: A novel model for treatment. Rehabilitation Research and Practice, 2012, 174579. https://doi.org/10.1155/2012/174579
Osborne, T. L., Michonski, J., Sayrs, J., Welch, S. S., & Anderson, L. K. (2017). Factor structure of the difficulties in emotion regulation scale (DERS) in adult outpatients receiving dialectical behavior therapy (DBT). Journal of Psychopathology and Behavioral Assessment, 39(2), 355–371. https://doi.org/10.1007/s10862-017-9586-x
Peles, E., Adelson, M., & Schreiber, S. (2014). Benzodiazepine usage during 19.5 years in methadone maintenance treatment patients and its relation to long-term outcome. Israel Journal of Psychiatry and Related Sciences, 51(4), 285–289.
Peles, E., Schreiber, S., Naumovsky, Y., & Adelson, M. (2007). Depression in methadone maintenance treatment patients: Rate and risk factors. Journal of Affective Disorders, 99(1–3), 213–220. https://doi.org/10.1016/j.jad.2006.09.017
Pekrun, R., & Linnenbrink-Garcia, L. (2012). Academic emotions and student engagement. In S. L. Christenson, A.L. Reschly, & C. Wylie (Eds.), Handbook of research on student engagement (pp. 259–282). Springer
Potik, D. (2021). Psychodynamic approaches for treatment of drug abuse and addiction - theory and treatment. Routledge.
Potik, D., Abramsohn, Y., Peles, E., Schreiber, S., & Adelson, M. (2011). Working in the cconflict-free sphere: Adaptation group in methadone mmaintenance ttreatment (MMT). Journal of Groups in Addiction and Recovery, 6(4), 285–306.
Potik, D., Abramsohn, Y., Schreiber, S., Adelson, M., & Peles, E. (2020). Drug abuse and behavioral transgressions during methadone maintenance treatment (MMT) are related to high psychopathy levels. Substance Use and Misuse, 55(3), 460–468. https://doi.org/10.1080/10826084.2019.1685546
Potik, D., Adelson, M., & Schreiber, S. (2007). Drug addiction from a psychodynam perspective: Methadone maintenance treatment (MMT) as transitional phenomena. Psychology and Psychotherapy, 80(2), 311–325. https://doi.org/10.1348/147608306X164806
Potik, D., Peles, E., Abramsohn, Y., Adelson, M., & Schreiber, S. (2014). The relationship between vulnerable attachment style, psychopathology, drug abuse, and retention in treatment among methadone maintenance treatment patients. Journal of Psychoactive Drugs, 46(4), 325–333. https://doi.org/10.1080/02791072.2014.944290
Raver, C. C. (2004). Placing emotional self-regulation in sociocultural and socioeconomic contexts. Child Development, 75(2), 346–353. https://doi.org/10.1111/j.1467-8624.2004.00676.x
Richmond, J. R., Tull, M. T., & Gratz, K. L. (2020). The roles of emotion regulation difficulties and impulsivity in the associations between borderline personality disorder symptoms and frequency of nonprescription sedative use and prescription sedative/opioid misuse. Journal of Contextual Behavioral Science, 16, 62–70. https://doi.org/10.1016/j.jcbs.2020.03.002
Roeser, K. A., Somers, C. L., & Mangus, L. R. (2019). Emerging adults’ risk-taking behaviors: Personal and social predictors. Journal of Adult Development, 26(4), 256–265. https://doi.org/10.1007/s10804-018-9318-9
Rogers, A. H., Gallagher, M. W., Jamison, R. N., & Zvolensky, M. J. (2020). Exploring the psychometric properties of the current opioid misuse measure among adults with chronic pain and opioid use. The Clinical Journal of Pain, 36(8), 578–583. https://doi.org/10.1097/AJP.0000000000000846
Rosen, D., Smith, M. L., & Reynolds, C. F. 3rd (2008). The prevalence of mental and physical health disorders among older methadone patients. The American Journal of Geriatric Psychiatry, 16(6), 488–497. https://doi.org/10.1097/JGP.0b013e31816ff35a
Rusch, S., Westermann, S., & Lincoln, T. M. (2012). Specificity of emotion regulation deficits in social anxiety: An internet study. Psychology and Psychotherapy, 85(3), 268–277.
Rutherford, M. J., Cacciola, J. S., Alterman, A. I., McKay, J. R., & Cook, T. J. (1999). The 2-year test-retest reliability of the psychopathy checklist revised in methadone patients. Assessment, 3, 285–291. https://doi.org/10.1177/107319119900600308
Salters-Pedneault, K., Roemer, L., Tull, M. T., Rucker, L., & Mennin, D. S. (2006). Evidence of broad deficits in emotion regulation associated with chronic worry and generalized anxiety disorder. Cognitive Therapy and Research, 30(4), 469–480. https://doi.org/10.1007/s10608-006-9055-4
Savitz, D. A., & Wellenius, G. A. (2023). Can cross-sectional studies contribute to causal inference? it depends. American Journal of Epidemiology, 192(4), 514–516. https://doi.org/10.1093/aje/kwac037
Schutz, P. A., Hong, J., Cross, D., & Osbon, J. (2006). Reflections on investigating emotion in educational activity settings. Educational Psychology Review, 18(4), 406–413.
Schutz, P. A., & Pekrun, R. (Eds.). (2007). Emotion in education. Elsevier Academic.
Sheppes, G., Suri, G., & Gross, J. J. (2015). Emotion regulation psychopathology. Annual Review of Clinical Psychology, 11, 379–405. https://doi.org/10.1146/annurev-clinpsy-032814-112739
Singla, A., Singh, P., Panditrao, M., & Panditrao, M. M. (2020). Is chronic opioid abuse associated with cerebral atrophy? An observational study. Indian Journal of Critical Care Medicine, 24(4), 276–280. https://doi.org/10.5005/jp-journals-10071-23410
Stellern, J., Xiao, K. B., Grennell, E., Sanches, M., Gowin, J. L., & Sloan, M. E. (2023). Emotion regulation in substance use disorders: A systematic review and meta-analysis. Addiction, 118(1), 30–47. https://doi.org/10.1111/add.16001
Stotts, A. L., Green, C., Masuda, A., Graowski, J., Wilson, K., Northrup, T. F., Moeller, F. G., & Schmitz, J. M. (2012). A stage I pilot study of acceptance and commitment therapy for methadone detoxification. Drug and Alcohol Dependence, 125(3), 215–222. https://doi.org/10.1016/j.drugalcdep.2012.02.015
Teasdale, J. D., Segal, Z., & Williams, J. M. (1995). How does cognitive therapy prevent depressive relapse and why should attentional control (mindfulness) training help? Behaviour Research and Therapy, 33(1), 25–39. https://doi.org/10.1016/0005-7967(94)e0011-7
Thompson, R. A. (2011). Emotion and emotion regulation: Two sides of the developing coin. Emotion Review, 3(1), 53–61. https://doi.org/10.1177/1754073910380969
Tull, M. T., Gratz, K. L., McDermott, M. J., Bordieri, M. J., Daughters, S. B., & Lejuez, C. W. (2016). The role of emotion regulation difficulties in the relation between PTSD symptoms and the learned association between trauma-related and cocaine cues. Substance Use and Misuse, 51(10), 1318–1329. https://doi.org/10.3109/10826084.2016.1168445
Van Rheenen, T. E., Murray, G., & Rossell, S. L. (2015). Emotion regulation in bipolar disorder: Profile and utility in predicting trait mania and depression propensity. Psychiatry Research, 225(3), 425–432. https://doi.org/10.1016/j.psychres.2014.12.001
Weidacker, K., Zhao, Y., Zhang, Y., Whiteford, S., Ren, Q., Zhang, C., & Voon, V. (2023). Methadone maintenance treatment and impulsivity: Premature responding. Journal of Clinical and Experimental Neuropsychology, 45(6), 606–617. https://doi.org/10.1080/13803395.2023.2276483
Weiss, N. H., Thomas, E. D., Schick, M. R., Reyes, M. E., & Contractor, A. A. (2022). Racial and ethnic differences in emotion regulation: A systematic review. Journal of Clinical Psychology, 78(5), 785–808. https://doi.org/10.1002/jclp.23284
Zhu, Y., Mooney, L. J., Yoo, C., Evans, E. A., Kelleghan, A., Saxon, A. J., Curtis, M. E., & Hser, Y. I. (2021). Psychiatric comorbidity and treatment outcomes in patients with opioid use disorder: Results from a multisite trial of buprenorphine-naloxone and methadone. Drug and Alcohol Dependence, 228, 108996. https://doi.org/10.1016/j.drugalcdep.2021.108996
Zimmermann, P., & Iwanski, A. (2014). Emotion regulation from early adolescence to emerging adulthood and middle adulthood: Age differences, gender differences, and emotion-specific developmental variations. International Journal of Behavioral Development, 38(2), 182–194. https://doi.org/10.1177/01650241351540
Zvolensky, M. J., Paulus, D. J., Bakhshaie, J., Viana, A. G., Garza, M., Manning, K., Rogers, A. H., Cardoso, J. B., Reitzel, L. R., Valdivieso, J., Ochoa-Perez, M., & Lemaire, C. (2017). Subjective social status and anxiety and depressive symptoms and disorders among low income latinos in primary care: The role of emotion dysregulation. Cognitive Therapy and Research, 41(5), 686–698. https://doi.org/10.1007/s10608-017-9844-y
Acknowledgements
Ester Eshkol is thanked for editorial assistance.
Funding
Open access funding provided by Bar-Ilan University. The authors received no funding from an external source.
Open access funding provided by Bar-Ilan University.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Declaration of interest statement
The authors report there are no competing interests to declare.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Potik, D., Adelson, M., Schreiber, S. et al. Characteristics of Patients in Methadone Maintenance Treatment (MMT) Who Have Difficulties in Emotion Regulation. J Rat-Emo Cognitive-Behav Ther (2024). https://doi.org/10.1007/s10942-024-00562-1
Accepted:
Published:
DOI: https://doi.org/10.1007/s10942-024-00562-1