Abstract
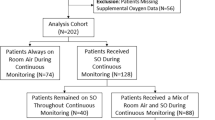
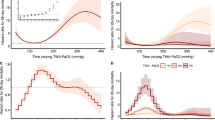
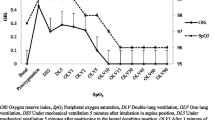
Episodic postoperative desaturation occurs predominantly from respiratory depression or airway obstruction. Monitor display of desaturation is typically delayed by over 30 s after these dynamic inciting events, due to perfusion delays, signal capture and averaging. Prediction of imminent critical desaturation could aid development of dynamic high-fidelity response systems that reduce or prevent the inciting event from occurring. Oxygen therapy is known to influence the depth and duration of desaturation epochs, thereby potentially influencing the accuracy of forecasting of desaturation. In this study, postoperative pulse oximetry data were retrospectively modeled using autoregressive methods to create prediction models for \({\hbox {SpO}}_2\) and imminent critical desaturation in the postoperative period. The accuracy of these models in predicting near future \({\hbox {SpO}}_2\) values was tested using root mean square error. The model accuracy for prediction of critical desaturation (\({\hbox {SpO}}_2\) \(\le 89\,\%\)) was evaluated using meta-analytical methods (sensitivity, specificity, likelihood ratios, diagnostic odds ratios and area under summary receiver operating characteristic curves). Between-study heterogeneity was used as a measure of reliability of the model across different patients and evaluated using the tau-squared statistic. Model performance was evaluated in \(20\) patients who received postoperative oxygen supplementation and \(20\) patients who did not receive oxygen. Our results show that model accuracy was high with root mean square errors between 0.2 and 2.8 %. Prediction accuracy as defined by area under the curve for critical desaturation events was observed to be greater in patients receiving oxygen in the 60-s horizon (\(0.95\pm 0.04\) vs. \(0.76\pm 0.16\)). This was likely related to the higher frequency of events in this group (median [IQR] \(133.0\) \([31.5, 508.2]\)) than patients who were not treated with oxygen (\(0\) \([0,110]\); \(p<0.001\)). Model reliability was reflected by the homogeneity of the prediction models which were homogenous across both prediction horizons and oxygen treatment groups. In conclusion, we report the use of autoregressive models to predict \({\hbox {SpO}}_2\) and forecast imminent critical desaturation events in the postoperative period with high degree of accuracy. These models reliably predict critical desaturation in patients receiving supplemental oxygen therapy. While high-fidelity prophylactic interventions that could modify these inciting events are in development, our current study offers proof of concept that the afferent limb of such a system can be modeled with a high degree of accuracy.


Similar content being viewed by others
References
Ramachandran SK, Haider N, Saran KA, Mathis M, Kim J, Morris M, O’Reilly M. Life-threatening critical respiratory events: a retrospective study of postoperative patients found unresponsive during analgesic therapy. J Clin Anesth. 2011;23(3):207–13.
Taylor S, Kirton OC, Staff I, Kozol RA. Postoperative day one: a high risk period for respiratory events. Am J Surg. 2005;190(5):752–6.
Hamber EA, Bailey PL, James SW, Wells DT, Lu JK, Pace NL. Delays in the detection of hypoxemia due to site of pulse oximetry probe placement. J Clin Anesth. 1999;11(2):113–8.
Rheineck-Leyssius AT, Kalkman CJ. Advanced pulse oximeter signal processing technology compared to simple averaging II. Effect on frequency of alarms in the postanesthesia care unit. J Clin Anesth. 1999;11(3):196–200.
Rheineck-Leyssius AT, Kalkman CJ. Advanced pulse oximeter signal processing technology compared to simple averaging I. Effect on frequency of alarms in the operating room. J Clin Anesth. 1999;11(3):192–5.
Trivedi NS, Ghouri AF, Shah NK, Lai E, Barker SJ. Pulse oximeter performance during desaturation and resaturation: a comparison of seven models. J Clin Anesth. 1997;9(3):184–8.
Trivedi NS, Ghouri AF, Shah NK, Lai E, Barker SJ. Effects of motion, ambient light, and hypoperfusion on pulse oximeter function. J Clin Anesth. 1997;9(3):179–83.
Claure N, Bancalari E, D’Ugard C, Nelin L, Stein M, Ramanathan R, Hernandez R, Donn SM, Becker M, Bachman T. Multicenter crossover study of automated control of inspired oxygen in ventilated preterm infants. Pediatrics. 2011;127(1):e76–83.
ElMoaqet H, Tilbury DM, Ramachandran S-K. Predicting oxygen saturation levels in blood using autoregressive models: a threshold metric for evaluating predictive models. Proceedings of American control conference, 2013. p. 734–739.
ElMoaqet H, Tilbury D, Ramachandran SK. Evaluating predictions of critical oxygen desaturation events. Physiol Meas. 2014;35(4):639–55.
Bremer T, Gough DA. Is blood glucose predictable from previous values? A solicitation for data. Diabetes. 1999;48(1):403–22.
Dua P, Doyle FJ, Pistikopoulos EN. Model-based blood glucose control for type 1 diabetes via parametric programming. IEEE Trans Biomed Eng. 2006;53(8):1478–91.
Gani A, Gribok A, Rajaraman S, Ward W, Reifman J. Predicting subcutaneous glucose concentration in humans: data-driven glucose modeling. IEEE Trans Biomed Eng. 2009;56(2):246–54.
Gani A, Gribok A, Lu Y, Ward W, Vigersky RA, Reifman J. Universal glucose models for predicting subcutaneous glucose concentration in humans. IEEE Trans Inf Technol Biomed. 2010;14(1):157–65.
Reifman J, Rajaraman S, Gribok A, Ward W. Predictive monitoring for improved management of glucose levels. Diabetes Sci Technol. 2007;1(4):478–86.
Sparacino G, Zanderigo F, Corazza S, Maran A, Facchinetti A, Cobelli C. Glucose concentration can be predicted ahead in time from continuous glucose monitoring sensor time-series. IEEE Trans Biomed Eng. 2007;54(5):931–7.
Sparacino G, Facchinetti A, Cobelli C. Smart continuous glucose monitoring sensors: on-line signal processing issues. Sensors. 2010;10(7):6751–72.
Trajanoski Z, Regittnig W, Wach P. Simulation studies on neural predictive control of glucose using the subcutaneous route. Comput Methods Programs Biomed. 1998;56(2):133–9.
Fu ES, Downs JB, Schweiger JW, Miguel RV, Smith RA. Supplemental oxygen impairs detection of hypoventilation by pulse oximetry. CHEST J. 2004;126(5):1552–8.
Voepel-Lewis T, Parker ML, Burke CN, Hemberg J, Perlin L, Kai S, Ramachandran SK. Pulse oximetry desaturation alarms on a general postoperative adult unit: a prospective observational study of nurse response time. Int J Nurs Stud. 2013;50(10):1351–8.
Centers for Medicare and Medicaid Services. National coverage determination (NCD) for home use of oxygen. 1993.
Astrom K, Wittenmark B. Computer controlled systems: theory and design. Upper Saddle River, NJ: Prentice Hall; 1997.
Ljung L. System identification: theory for the user. Upper Saddle River, NJ: Prentice-Hall; 1987.
Clarke WL. The original Clarke error grid analysis (EGA). Diabetes Technol Therapeutics. 2005;7(5):776–9.
Armstrong JS, Collopy F. Error measures for generalizing about forecasting methods: empirical comparisons. Int J Forecast. 1992;8(1):69–80.
Hyndman RJ, Koehler AB. Another look at measures of forecast accuracy. Int J Forecast. 2006;22:679–88.
Altman DG, Bland JM. Diagnostic tests 2: predictive values. Br Med J. 1994;309(6947):102.
Altman DG, Bland JM. Diagnostic tests 1: sensitivity and specificity. Br Med J. 1994;308(6943):1552.
Deeks JJ. Systematic reviews of evaluations of diagnostic and screening tests. BMJ. 2001;323(7305):157–62.
Glas AS, Lijmer JG, Prins MH, Bonsel GJ, Bossuyt PM. The diagnostic odds ratio: a single indicator of test performance. J Clin Epidemiol. 2003;56(11):1129–35.
Hanley JA, McNeil BJ. The meaning and use of the area under a receiver operating characteristic (roc) curve. Radiology. 1982;143(1):29–36.
Moses LE, Shapiro D, Littenberg B. Combining independent studies of a diagnostic test into a summary roc curve: data-analytic approaches and some additional considerations. Stat Med. 1993;12(14):1293–316.
Ramachandran SK, Josephs LA. A meta-analysis of clinical screening tests for obstructive sleep apnea. Anesthesiology. 2009;110(4):928–39.
Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. Br Med J. 2003;327(7414):557.
Higgins JP. Commentary: heterogeneity in meta-analysis should be expected and appropriately quantified. Int J Epidemiol. 2008;37(5):1158–60.
Mitchell MD. Validation of the summary ROC for diagnostic test meta-analysis: a monte carlo simulation. Acad Radiol. 2003;10(1):25–31.
Walter S. Properties of the summary receiver operating characteristic (sroc) curve for diagnostic test data. Stat Med. 2002;21(9):1237–56.
Leemis LM, Trivedi KS. A comparison of approximate interval estimators for the bernoulli parameter. Am Stat. 1996;50(1):63–8.
Taenzer AH, Pyke J, McGrath S, Blike G. Impact of pulse oximetry surveillance on rescue events and intensive care unit transfers: a before-and-after concurrence study. Anesthesiology. 2010;112(1):282–7.
Acknowledgments
Dr. Ramachandran has received honoraria from Merck for consulting and research support in the current year. This research was supported in part by the National Center for Advancing Translational Sciences of the National Institutes of Health under Award Number \(2UL1TR000433\). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
ElMoaqet, H., Tilbury, D.M. & Ramachandran, S.K. Effect of concurrent oxygen therapy on accuracy of forecasting imminent postoperative desaturation. J Clin Monit Comput 29, 521–531 (2015). https://doi.org/10.1007/s10877-014-9629-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-014-9629-8