Abstract
Objective
The pleth variability index (PVI), which is calculated from respiratory variations in the perfusion index (PI), reportedly predicts fluid responsiveness. However, vasomotor tone fluctuations induced by nociceptive stimuli change the PI and may reduce the accuracy of PVI. The aim of this study was to confirm the effects of surgical stimuli on PVI.
Methods
Twenty-four patients were examined after the induction of general anesthesia. Heart rate (HR), mean arterial blood pressure (MBP), PI, PVI, stroke volume variation (SVV), and cardiac index (CI) were recorded before and after the skin incision. PI and PVI were calculated using a Radical 7 pulse oximeter, and SVV and CI were calculated using the FloTrac/Vigileo system.
Results
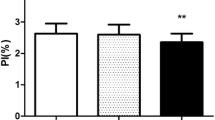
After the skin incision, the PI decreased significantly from 5.3 (4.0–6.2%) to 3.6% (1.8–4.7%), whereas the PVI increased significantly from 9.5 (7.0–12.0%) to 13.5% (9.0–16.0%). A significant negative correlation was observed between the changes in PI and PVI before and after the skin incision. The skin incision did not affect the HR, CI, or SVV but increased the MBP.
Conclusion
This study showed a significant increase in the PVI and a negative correlation between the changes in PVI and PI before and after the skin incision. The PVI can be calculated from the variations in the PI caused not by mechanical ventilation, but rather by fluctuations in vasomotor tone. When using the PVI as an indicator for fluid responsiveness, it is crucial to pay attention to fluctuations in vasomotor tone induced by nociceptive stimuli.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Michard F. Changes in arterial pressure during mechanical ventilation. Anesthesiology. 2005;103:419–28.
Marik PE, Cavallazzi R, Vasu T, Hirani A. Dynamic changes in arterial waveform derived variables and fluid responsiveness in mechanically ventilated patients: a systematic review of the literature. Crit Care Med. 2009;37:2642–7.
Hofer CK, Müller SM, Furrer L, Klaghofer R, Genoni M, Zollinger A. Stroke volume and pulse pressure variation for prediction of fluid responsiveness in patients undergoing off-pump coronary artery bypass grafting. Chest. 2005;128:848–54.
Cannesson M, Musard H, Desebbe O, Boucau C, Simon R, Hénaine R, Lehot JJ. The ability of stroke volume variations obtained with Vigileo/FloTrac system to monitor fluid responsiveness in mechanically ventilated patients. Anesth Analg. 2009;108:513–7.
Wyffels PA, Durnez PJ, Helderweirt J, Stockman WM, De Kegel D. Ventilation-induced plethysmographic variations predict fluid responsiveness in ventilated postoperative cardiac surgery patients. Anesth Analg. 2007;105:448–52.
Feissel M, Teboul JL, Merlani P, Badie J, Faller JP, Bendjelid K. Plethysmographic dynamic indices predict fluid responsiveness in septic ventilated patients. Intensive Care Med. 2007;33:993–9.
Cannesson M, Attof Y, Rosamel P, Desebbe O, Joseph P, Metton O, Bastien O, Lehot JJ. Respiratory variations in pulse oximetry plethysmographic waveform amplitude to predict fluid responsiveness in the operating room. Anesthesiology. 2007;106:1105–11.
Cannesson M, Desebbe O, Rosamel P, Delannoy B, Robin J, Bastien O, Lehot JJ. Pleth variability index to monitor the respiratory variations in the pulse oximeter plethysmographic waveform amplitude and predict fluid responsiveness in the operating theatre. Br J Anaesth. 2008;101:200–6.
Cannesson M, Delannoy B, Morand A, Rosamel P, Attof Y, Bastien O, Lehot JJ. Does the Pleth variability index indicate the respiratory-induced variation in the plethysmogram and arterial pressure waveforms? Anesth Analg. 2008;106:1189–94.
Shelley KH. Photoplethysmography: beyond the calculation of arterial oxygen saturation and heart rate. Anesth Analg. 2007;105:S31–6.
Korhonen I, Yli-Hankala A. Photoplethysmography and nociception. Acta Anaesthesiol Scand. 2009;53:975–85.
Ezri T, Steinmetz A, Geva D, Szmuk P. Skin vasomotor reflex as a measure of depth of anesthesia. Anesthesiology. 1998;89:1281–2.
Roizen MF, Horrigan RW, Frazer BM. Anesthetic doses blocking adrenergic (stress) and cardiovascular responses to incision-MAC BAR. Anesthesiology. 1981;54:390–8.
Shelley K, Shelley S. Pulse oximeter waveform: photoelectric plethysmography, in clinical monitoring. In: Hines R, Blitt C, eds. Carol Lake. Philadeiphia: W.B. Saunders Company; 2001. p. 420–428.
Awad AA, Ghobashy MA, Ouda W, Stout RG, Silverman DG, Shelley KH. Different responses of ear and finger pulse oximeter wave form to cold pressor test. Anesth Analg. 2001;92:1483–6.
Reisner A, Shaltis PA, McCombie D, Asada HH. Utility of the photoplethysmogram in circulatory monitoring. Anesthesiology. 2008;108:950–8.
Lima AP, Beelen P, Bakker J. Use of a peripheral perfusion index derived from the pulse oximetry signal as a noninvasive indicator of perfusion. Crit Care Med. 2002;30:1210–3.
Lima A, Bakker J. Noninvasive monitoring of peripheral perfusion. Intensive Care Med. 2005;31:1316–26.
Tanaka G, Sawada Y, Yamakoshi K. Beat-by-beat double-normalized pulse volume derived photoplethysmographically as a new quantitative index of finger vascular tone in humans. Eur J Appl Physiol. 2000;81:148–54.
Mowafi HA, Ismail SA, Shafi MA, Al-Ghamdi AA. The efficacy of perfusion index as an indicator for intravascular injection of epinephrine-containing epidural test dose in propofol-anesthetized adults. Anesth Analg. 2009;108:549–53.
Manecke GR. Edwards FloTrac sensor and Vigileo monitor: easy, accurate, reliable cardiac output assessment using the arterial pulse wave. Exp Rev Med Dev. 2005;2:523–7.
Burton AC. Relation of structure to function of the tissues of the wall of blood vessels. Physiol Rev. 1954;34:619–42.
Graybeal JM, Petterson MT, Novak J. Perfusion index reflects physiologic changes in blood flow resulting from cold exposure. Society for Technology in Anesthesia 2005 Annual Meeting. Miami, FL: Anesth & Analg. and STA; 2005.
Derichard A, Robin E, Tavernier B, Costecalde M, Fleyfel M, Onimus J, Lebuffe G, Chambon JP, Vallet B. Automated pulse pressure and stroke volume variations from radial artery: evaluation during major abdominal surgery. Br J Anaesth. 2009;103:678–84.
Camporota L, Beale R. Pitfalls in haemodynamic monitoring based on the arterial pressure waveform. Crit Care. 2010;14:124.
Solus-Biguenet H, Fleyfel M, Tavernier B, Kipnis E, Onimus J, Robin E, Lebuffe G, Decoene C, Pruvot FR, Vallet B. Non-invasive prediction of fluid responsiveness during major hepatic surgery. Br J Anaesth. 2006;97:808–16.
Landsverk SA, Hoiseth LO, Kvandal P, Hisdal J, Skare O, Kirkeboen KA. Poor agreement between respiratory variations in pulse oximetry photoplethysmographic waveform amplitude and pulse pressure in intensive care unit patients. Anesthesiology. 2008;109:849–55.
Nijboer JA, Dorlas JC. Comparison of plethysmograms taken from finger and pinna during anaesthesia. Br J Anaesth. 1985;57:531–4.
Huiku M, Uutela K, van Gils M, Korhonen I, Kymäläinen M, Meriläinen P, Paloheimo M, Rantanen M, Takala P, Viertiö-Oja H, Yli-Hankala A. Assessment of surgical stress during general anaesthesia. Br J Anaesth. 2007;98:447–55.
Shelley KH, Jablonka DH, Awad AA, Stout RG, Rezkanna H, Silverman DG. What is the best site for measuring the effect of ventilation on the pulse oximeter waveform. Anesth Analg. 2006;103:372–7.
Author information
Authors and Affiliations
Corresponding author
Additional information
Takeyama M, Matsunaga A, Kakihana Y, Masuda M, Kuniyoshi T, Kanmura Y. Impact of skin incision on the pleth variability index.
Rights and permissions
About this article
Cite this article
Takeyama, M., Matsunaga, A., Kakihana, Y. et al. Impact of skin incision on the pleth variability index. J Clin Monit Comput 25, 215–221 (2011). https://doi.org/10.1007/s10877-011-9298-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-011-9298-9