Abstract
Objectives
To re-evaluate the accuracy and precision of a non-invasive method for measurement of cardiac output based on the differential CO2 Fick approach using an automated change in respiratory rate delivered by a ventilator under control by a prototype measurement system.
Methods
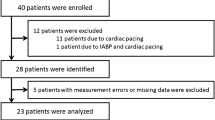
Twenty-four patients during coronary artery bypass surgery, pre- and postcardiopulmonary bypass were recruited. After routine cannulation including pulmonary artery catheter, relaxant general anesthesia was induced. After hemodynamic and ventilatory stability were achieved, simultaneous paired measurements were made by the differential Fick method and by bolus thermodilution. Measurements were generated by inducing a change in respiratory rate by the ventilator under computer control. In Group 1, this involved an␣increase in respiratory rate from 8 to 12 breaths/min. In Group 2, this involved a decrease from 12 to 6 breaths/min.
Results
Nineteen measurements were made in each Group, 12 pre-CPB and 7 post-CPB. In Group 1 mean␣bias was −0.06 l/min, with a precision of agreement of 0.87 l/min, r = 0.91. In Group 2 (excluding one outlier) mean bias was −0.07 l/min, with a precision of 1.12 l/min, r = 0.71.
Conclusions
Acceptable agreement with thermo- dilution during surgery was found, particularly where the ventilatory change involved an increase in respiratory rate from a lower baseline. This approach has potential to be readily integrated into modern anesthesia delivery platforms, allowing routine non-invasive cardiac output measurement.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Botero M, Lobato EB. 2001 Advances in noninvasive cardiac output monitoring: an update. J Cardiothorac Vasc Anesth 15(5): 631–640
Laszlo G. 2004 Respiratory measurements of cardiac output: from elegant idea to useful test. J Appl Physiol 96:428–437
Capek JM, Roy RJ. Encyclopedia of medical devices and instrumentation. J.G. Webster Ed. New York, Wiley publishers. pp. 1309–1310, 1988
Robinson GJB, Peyton PJ, Vartuli GM, Burfoot RB, Junor PA. 2003 Continuous measurement of cardiac output by inert gas throughflow – comparison with thermodilution. J Cardiothorac Vasc Anesth 17(2):204–210
Binder J, Parkin W. 2001 Non-invasive cardiac output determination: comparison of a new partial-rebreathing technique with thermodilution. Anaesth Intensive Care 29:19–23
Sakka S, Kozieras J, Thuemer O, van Nout N. 2007 Measurement of cardiac output: a comparison between transpulmonary thermodilution and uncalibrated pulse contour analysis. Br J Anaesth 99:337–342
Jhanji S, Dawson J, Pearse RM. 2008 Cardiac output monitoring: basic science and clinical application. Anaesthesia 63:172–181
Van den Oever H, Murphy E, Chrsitie-Taylor G. 2007 USCOM (Ultrasonic Cardiac Output Monitors) lacks agreement with thermodilution cardiac output and transoesophageal echocardiography valve measurement. Anaesth Intensive Care 35:903–910
Jaffe MB. 1999 Partial CO2 rebreathing cardiac output – operating principles of the NICOTM system. J Clin Monit 15: 387–401
Blomqvist H, Frostell C, Hedenstierna G. 1986 A non-invasive technique for measurement of lung perfusion. Intensive Care Med 12: 172–178
Capek JM, Roy RJ. 1988 Noninvasive measurement of cardiac output during partial CO2 rebreathing. IEEE Trans Biomed Eng 35: 653–661
Gedeon A, Forslund L, Hedenstierna G, Romano E. 1980 A new method for noninvasive bedside determination of pulmonary blood flow. Med Biol Eng Comput 18: 411–418
Bosman RJ, Stountenbeek CP, Zandstra DF. 1991 Non-invasive pulmonary blood flow measurement by means of CO2 analysis of expiratory gases. Intensive Care Med 17: 98–102
Noguchi H, Ogushi Y, Yoshiya I, Itakura N, Yamabayashi H. Breath-by-breath \( \dot {V}_{{{\rm{CO}}_{{\rm{2}}} }} \) and \( \dot {V}_{{{\rm{O}}_{{\rm{2}}} }} \) require compensation for transport delay and dynamic response. J Appl Physiol 1982; 52(1): 79–84
Beaver W, Lamarra N, Wasserman K. 1981 Breath-by-breath measurement of true alveolar gas exchange. J Appl Physiol 51(6): 1662–1675
Wessel HU, Stout RL, Bastanier CK, Paul MH. 1979 Breath-by breath variation of FRC: effect on VO2 and VCO2 measured at the mouth. J Appl Physiol Respirat Environ Exercise Physiol 46(6): 1122–1126
Kelman GR. 1966 Digital computer subroutine for the conversion of oxygen tension into saturation. J Appl Physiol 21(4): 1375–1376
Kelman GR. 1967 Digital computer procedure for the conversion of PCO2 into blood CO2 content. Respir Physiol 3: 111–115
Peyton P, Robinson G, Thompson B. 2001 The effect of ventilation-perfusion inhomogeneity and nitrous oxide on oxygenation in anesthesia: physiological modeling of gas exchange. J Appl Physiol 91: 17–25
Bland JM, Altman DG. Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1986; 1(8476): 307–310
Gueret G, Kiss G, Khaldi S, Le Jouan R, Le Grand A, Perrament Y, Lefevre C, Arvieux CC. 2007 Comparison of cardiac output measurements between NICO and the pulmonary artery catheter during repeat surgery for total hip replacement. Eur J Anaesth 24:1028–1033
Botero M, Kirby D, Lobato E, Staples E, Gravenstein N. 2004 measurement of cardiac output before and after cardiopulmonary bypass: comparison among aortic transit-time ultrasound, thermodilution, and noninvasive partial CO2 rebreathing. J Cardiothorac Vasc Anesth 18(5): 563–572
Manecke G, Auger W. 2007 Cardiac output determination from the arterial pressure wave: clinical testing of a novel algorithm that does not requires calibration. J Cardiothorac Vasc Anesth 21(1): 3–7
Cannesson M, Attof Y, Rosamel P, Joseph P, Bastien O, Lehot J-J. 2007 Comparison of FloTracTM cardiac output monitoring system in patients undergoing coronary artery bypass grafting with pulmonary artery cardiac output measurements. Eur J Anaesth 24: 832–839
Latson TW, Whitten CW, O’Flaherty D. 1993 Ventilation, thermal noise, and errors in cardiac output measurements after cardiopulmonary bypass. Anesthesiology 79: 1233–1243
Author information
Authors and Affiliations
Corresponding author
Additional information
Peyton PJ, Thompson D, Junor P. Non-invasive automated measurement of cardiac output during stable cardiac surgery using a fully integrated differential CO2 Fick method.
Rights and permissions
About this article
Cite this article
Peyton, P.J., Thompson, D. & Junor, P. Non-invasive automated measurement of cardiac output during stable cardiac surgery using a fully integrated differential CO2 Fick method. J Clin Monit Comput 22, 285–292 (2008). https://doi.org/10.1007/s10877-008-9131-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-008-9131-2