Abstract
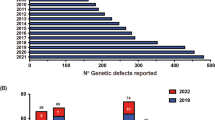
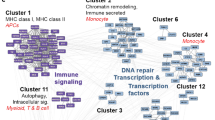
Systemic lupus erythematosus (SLE) is a chronic autoimmune disease that is characterized by its large heterogeneity in terms of clinical presentation and severity. The pathophysiology of SLE involves an aberrant autoimmune response against various tissues, an excess of apoptotic bodies, and an overproduction of type-I interferon. The genetic contribution to the disease is supported by studies of monozygotic twins, familial clustering, and genome-wide association studies (GWAS) that have identified numerous risk loci. In the early 70s, complement deficiencies led to the description of familial forms of SLE caused by a single gene defect. High-throughput sequencing has recently identified an increasing number of monogenic defects associated with lupus, shaping the concept of monogenic lupus and enhancing our insights into immune tolerance mechanisms. Monogenic lupus (moSLE) should be suspected in patients with either early-onset lupus or syndromic lupus, in male, or in familial cases of lupus. This review discusses the genetic basis of monogenic SLE and proposes its classification based on disrupted pathways. These pathways include defects in the clearance of apoptotic cells or immune complexes, interferonopathies, JAK-STATopathies, TLRopathies, and T and B cell dysregulations.



Similar content being viewed by others
Data Availability
No datasets were generated or analysed during the current study.
References
Aringer M et al. 2019 European League Against Rheumatism/American College of Rheumatology classification criteria for systemic lupus erythematosus. Ann Rheum Dis. 2019;78(9):1151–9. https://doi.org/10.1136/annrheumdis-2018-214819.
Tsokos GC, Lo MS, Reis PC, Sullivan KE. New insights into the immunopathogenesis of systemic lupus erythematosus. Nat Rev Rheumatol. 2016;12(12):716–30. https://doi.org/10.1038/nrrheum.2016.186.
Lemke G. How macrophages deal with death. Nat Rev Immunol. 2019;19(9):539–49. https://doi.org/10.1038/s41577-019-0167-y.
Doran AC, Yurdagul A, Tabas I. Efferocytosis in health and disease. Nat Rev Immunol. 2020;20(4):254–67. https://doi.org/10.1038/s41577-019-0240-6.
Mehrotra P, Ravichandran KS. Drugging the efferocytosis process: concepts and opportunities. Nat Rev Drug Discov. 2022;21(8):601-620. https://doi.org/10.1038/s41573-022-00470-y.
Rose T, Dörner T. Drivers of the immunopathogenesis in systemic lupus erythematosus. Best Pract Res Clin Rheumatol. 2017;31(3):321–33. https://doi.org/10.1016/j.berh.2017.09.007.
Kamphuis S, Silverman ED. Prevalence and burden of pediatric-onset systemic lupus erythematosus. Nat Rev Rheumatol. 2010;6(9):538–46. https://doi.org/10.1038/nrrheum.2010.121.
Arnaud L, Fagot J-P, Mathian A, Paita M, Fagot-Campagna A, Amoura Z. Prevalence and incidence of systemic lupus erythematosus in France: a 2010 nation-wide population-based study. Autoimmun Rev. 2014;13(11):1082–9. https://doi.org/10.1016/j.autrev.2014.08.034.
Bader-Meunier B, et al. Initial presentation of childhood-onset systemic lupus erythematosus: a French multicenter study. J Pediatr. 2005;146(5):648–53. https://doi.org/10.1016/j.jpeds.2004.12.045.
Alexander T, Hedrich CM. Systemic lupus erythematosus – are children miniature adults? Clin Immunol. 2022;234:108907. https://doi.org/10.1016/j.clim.2021.108907.
Papadimitraki ED, Isenberg DA. Childhood- and adult-onset lupus: an update of similarities and differences. Expert Rev Clin Immunol. 2009;5(4):391–403. https://doi.org/10.1586/eci.09.29.
Gutierrez-Arcelus M, Rich SS, Raychaudhuri S. Autoimmune diseases — connecting risk alleles with molecular traits of the immune system. Nat Rev Genet. 2016;17(3):160. https://doi.org/10.1038/nrg.2015.33.
Criswell LA. The genetic contribution to systemic lupus erythematosus. Bull NYU Hosp Jt Dis. 2008;66(3):176–83.
Deapen D, et al. A revised estimate of twin concordance in systemic lupus erythematosus. Arthritis Rheum. 1992;35(3):311–8. https://doi.org/10.1002/art.1780350310.
Ulff-Møller CJ, Svendsen AJ, Viemose LN, Jacobsen S. Concordance of autoimmune disease in a nationwide Danish systemic lupus erythematosus twin cohort. Semin Arthritis Rheum. 2018;47(4):538–44. https://doi.org/10.1016/j.semarthrit.2017.06.007.
Deng Y, Tsao BP. Genetic susceptibility to systemic lupus erythematosus in the genomic era. Nat Rev Rheumatol. 2010;6(12):683–92. https://doi.org/10.1038/nrrheum.2010.176.
Cui Y, Sheng Y, Zhang X. Genetic susceptibility to SLE: recent progress from GWAS. J Autoimmun. 2013;41:25–33. https://doi.org/10.1016/j.jaut.2013.01.008.
Kozyrev SV, et al. Functional variants in the B-cell gene BANK1 are associated with systemic lupus erythematosus. Nat Genet. 2008;40(2):211–6. https://doi.org/10.1038/ng.79.
Jiang SH, et al. Functional rare and low frequency variants in BLK and BANK1 contribute to human lupus. Nat Commun. 2019;10. https://doi.org/10.1038/s41467-019-10242-9.
Alkaissi H, Havarinasab S, Nielsen JB, Söderkvist P, Hultman P. Bank1 and NF-kappaB as key regulators in anti-nucleolar antibody development. PLoS ONE. 2018;13(7):e0199979. https://doi.org/10.1371/journal.pone.0199979.
Belot A, Cimaz R. Monogenic forms of systemic lupus erythematosus: new insights into SLE pathogenesis. Pediatr Rheumatol Online J. 2012;10(1):21. https://doi.org/10.1186/1546-0096-10-21.
Belot A, Cochat P. Monogenic systemic lupus erythematosus. Nephrol Ther. 2012;8(1):1–4. https://doi.org/10.1016/j.nephro.2011.05.003.
Belot A, et al. Contribution of rare and predicted pathogenic gene variants to childhood-onset lupus: a large, genetic panel analysis of British and French cohorts. Lancet Rheumatol. 2020;2(2):e99–109. https://doi.org/10.1016/S2665-9913(19)30142-0.
Agnello V, De Bracco MM, Kunkel HG. Hereditary C2 deficiency with some manifestations of systemic lupus erythematosus. J Immunol Baltim Md 1950. 1972;108(3):837–40.
Moncada B, Day NKB, Good RA, Windhorst DB. Lupus-erythematosus-like syndrome with a familial defect of complement. N Engl J Med. 1972;286(13):689–93. https://doi.org/10.1056/nejm197203302861304.
Santer DM, et al. C1q deficiency leads to the defective suppression of IFN-alpha in response to nucleoprotein containing immune complexes. J Immunol Baltim Md 1950. 2010;185(8):4738–49. https://doi.org/10.4049/jimmunol.1001731.
Batu ED, et al. Whole exome sequencing in early-onset systemic lupus erythematosus. J Rheumatol. 2018;45(12):1671–9. https://doi.org/10.3899/jrheum.171358.
Abel G, Agnello V. Complement deficiency and systemic lupus erythematosus. Elsevier; 2004. pp. 173–201. https://doi.org/10.1016/b9-78-012433-9/01950-0090.
Lintner KE, et al. Early components of the complement classical activation pathway in human systemic autoimmune diseases. Front Immunol. 2016;7:36. https://doi.org/10.3389/fimmu.2016.00036.
Tusseau M, et al. DNASE1L3 deficiency, new phenotypes, and evidence for a transient type I IFN signaling. J Clin Immunol. 2022;42(6):1310–20. https://doi.org/10.1007/s10875-022-01287-5.
Sisirak V, et al. Digestion of chromatin in apoptotic cell microparticles prevents autoimmunity. Cell. 2016;166(1):88–101. https://doi.org/10.1016/j.cell.2016.05.034.
Al-Mayouf SM, et al. Loss-of-function variant in DNASE1L3 causes a familial form of systemic lupus erythematosus. Nat Genet. 2011;43(12):1186–8. https://doi.org/10.1038/ng.975.
Tsokos GC. Systemic lupus erythematosus. N Engl J Med. 2011;365:2110–21. https://doi.org/10.1056/NEJMra1100359.
Aicardi J, Goutières F. A Progressive familial encephalopathy in infancy with calcifications of the basal ganglia and chronic cerebrospinal fluid lymphocytosis. Ann Neurol. 1984;15(1):49–54. https://doi.org/10.1002/ana.410150109.
Lebon P, Badoual J, Ponsot G, Goutières F, Hémeury-Cukier F, Aicardi J. Intrathecal synthesis of interferon-alpha in infants with progressive familial encephalopathy. J Neurol Sci. 1988;84(2):201–8. https://doi.org/10.1016/0022-510X(88)90125-6.
Crow YJ, Rehwinkel J. Aicardi-Goutières syndrome and related phenotypes: linking nucleic acid metabolism with autoimmunity. Hum Mol Genet. 2009;18(R2):R130–6. https://doi.org/10.1093/hmg/ddp293.
Crow YJ, et al. Mutations in the gene encoding the 3′-5′ DNA exonuclease TREX1 cause Aicardi-Goutières syndrome at the AGS1 locus. Nat Genet. 2006;38(8):Art. no. 8. https://doi.org/10.1038/ng1845.
Crow YJ. Type I interferonopathies: a novel set of inborn errors of immunity. Ann N Y Acad Sci. 2011;1238(1):91–8. https://doi.org/10.1111/j.1749-6632.2011.06220.x.
Crow YJ, Stetson DB. The type I interferonopathies: 10 years on. Nat Rev Immunol. 2022;22(8):471-483. https://doi.org/10.1038/s41577-021-00633-9.
Rice GI, Rodero MP, Crow YJ. Human disease phenotypes associated with mutations in TREX1. J Clin Immunol. 2015;35(3):235–43. https://doi.org/10.1007/s10875-015-0147-3.
Richards A, et al. C-terminal truncations in human 3’-5’ DNA exonuclease TREX1 cause autosomal dominant retinal vasculopathy with cerebral leukodystrophy. Nat Genet. 2007;39(9):1068–70. https://doi.org/10.1038/ng2082.
Liu Y, et al. Activated STING in a vascular and pulmonary syndrome. N Engl J Med. 2014;371(6):507–18. https://doi.org/10.1056/NEJMoa1312625.
König N, et al. Familial chilblain lupus due to a gain-of-function mutation in STING. Ann Rheum Dis. 2017;76(2):468–72. https://doi.org/10.1136/annrheumdis-2016-209841.
Jeremiah N, et al. Inherited STING-activating mutation underlies a familial inflammatory syndrome with lupus-like manifestations. J Clin Invest. 2014;124(12):5516–20. https://doi.org/10.1172/JCI79100.
Lepelley A, et al. Mutations in COPA lead to abnormal trafficking of STING to the Golgi and interferon signaling. J Exp Med. 2020;217(11):e20200600. https://doi.org/10.1084/jem.20200600.
Watkin LB, et al. COPA mutations impair ER-Golgi transport causing hereditary autoimmune-mediated lung disease and arthritis. Nat Genet. 2015;47(6):654–60. https://doi.org/10.1038/ng.3279.
Briggs TA, et al. Spondyloenchondrodysplasia due to mutations in ACP5: a comprehensive survey. J Clin Immunol. 2016;36:220–34. https://doi.org/10.1007/s10875-016-0252-y.
Rodero MP, et al. Type I interferon-mediated autoinflammation due to DNase II deficiency. Nat Commun. 2017;8(1):2176. https://doi.org/10.1038/s41467-017-01932-3.
Thaventhiran JED, et al. Whole-genome sequencing of a sporadic primary immunodeficiency cohort. Nature. 2020;583(7814):Art. no. 7814. https://doi.org/10.1038/s41586-020-2265-1.
Hadjadj J, et al. Early-onset autoimmunity associated with SOCS1 haploinsufficiency. Nat Commun. 2020;11:5341. https://doi.org/10.1038/s41467-020-18925-4.
Gruber C, et al. IL4Rα and IL17A blockade rescue autoinflammation in SOCS1 haploinsufficiency. J Clin Immunol. 2023;44(1):36. https://doi.org/10.1007/s10875-023-01635-z.
Rodari MM, et al. Insights into the expanding intestinal phenotypic spectrum of SOCS1 haploinsufficiency and therapeutic options. J Clin Immunol. 2023. https://doi.org/10.1007/s10875-023-01495-7.
Parlato M, et al. Loss-of-function mutation in PTPN2 causes aberrant activation of JAK signaling via STAT and very early onset intestinal inflammation. Gastroenterology. 2020;159(5):1968-1971.e4. https://doi.org/10.1053/j.gastro.2020.07.040.
Okada S, et al. Human STAT1 gain-of-function heterozygous mutations: chronic mucocutaneous candidiasis and type I interferonopathy. J Clin Immunol. 2020;40(8):1065–81. https://doi.org/10.1007/s10875-020-00847-x.
Heterozygous STAT1 gain-of-function mutations underlie an unexpectedly broad clinical phenotype | Blood | American Society of Hematology. https://ashpublications-org.proxy.insermbiblio.inist.fr/blood/article/127/25/3154/35201/Heterozygous-STAT1-gain-of-function-mutations. Accessed 17 Nov 2023.
Brown GJ, et al. TLR7 gain-of-function genetic variation causes human lupus. Nature. 2022;605(7909):349–56. https://doi.org/10.1038/s41586-022-04642-z.
Xie C, et al. De novo PACSIN1 gene variant found in childhood lupus and a role for PACSIN1/TRAF4 complex in toll-like receptor 7 activation. Arthritis Rheumatol Hoboken NJ. 2023;75(6):1058–71. https://doi.org/10.1002/art.42416.
Wolf C, et al. UNC93B1 variants underlie TLR7-dependent autoimmunity. Sci Immunol. 2024;eadi9769. https://doi.org/10.1126/sciimmunol.adi9769.
Rieux-Laucat F, et al. Mutations in Fas associated with human lymphoproliferative syndrome and autoimmunity. Science. 1995;268(5215):1347–9. https://doi.org/10.1126/science.7539157.
Wu J, Wilson J, He J, Xiang L, Schur PH, Mountz JD. Fas ligand mutation in a patient with systemic lupus erythematosus and lymphoproliferative disease. J Clin Invest. 1996;98(5):1107–13. https://doi.org/10.1172/JCI118892.
Vaishnaw AK, et al. The spectrum of apoptotic defects and clinical manifestations, including systemic lupus erythematosus, in humans with CD95 (Fas/APO-1) mutations. Arthritis Rheum. 1999;42(9):1833–42. https://doi.org/10.1002/1529-0131(199909)42:9%3c1833::AID-ANR7%3e3.0.CO;2-Q.
Rieux-Laucat F. What’s up in the ALPS. Curr Opin Immunol. 2017;49:79–86. https://doi.org/10.1016/j.coi.2017.10.001.
Kuehn HS, Boast B, Rosenzweig SD. Inborn errors of human IKAROS: LOF and GOF variants associated with primary immunodeficiency. Clin Exp Immunol. 2023;212(2):129–36. https://doi.org/10.1093/cei/uxac109.
Su G, et al. Analysis of five cases of monogenic lupus related to primary immunodeficiency diseases. Inflamm Res Off J Eur Histamine Res Soc Al. 2021;70(10–12):1211–6. https://doi.org/10.1007/s00011-021-01479-6.
Walter JE, et al. Impaired receptor editing and heterozygous RAG2 mutation in a patient with systemic lupus erythematosus and erosive arthritis. J Allergy Clin Immunol. 2015;135(1):272–3. https://doi.org/10.1016/j.jaci.2014.07.063.
Belot A, et al. Protein kinase cδ deficiency causes mendelian systemic lupus erythematosus with B cell-defective apoptosis and hyperproliferation. Arthritis Rheum. 2013;65(8):2161–71. https://doi.org/10.1002/art.38008.
Jefferson L, et al. Phenotypic variability in PRKCD: a review of the literature. J Clin Immunol. 2023. https://doi.org/10.1007/s10875-023-01579-4.
Neehus A-L, et al. Impaired respiratory burst contributes to infections in PKCδ-deficient patients. J Exp Med. 2021;218(9):e20210501. https://doi.org/10.1084/jem.20210501.
Bader-Meunier B, et al. Are RASopathies new monogenic predisposing conditions to the development of systemic lupus erythematosus? Case report and systematic review of the literature. Semin Arthritis Rheum. 2013;43(2):217–9. https://doi.org/10.1016/j.semarthrit.2013.04.009.
Quaio CRDC, et al. Autoimmune disease and multiple autoantibodies in 42 patients with RASopathies. Am J Med Genet A. 2012;158A(5):1077–82. https://doi.org/10.1002/ajmg.a.35290.
Oliveira JB, et al. NRAS mutation causes a human autoimmune lymphoproliferative syndrome. Proc Natl Acad Sci. 2007;104(21):8953–8. https://doi.org/10.1073/pnas.0702975104.
Niemela JE, et al. Somatic KRAS mutations associated with a human nonmalignant syndrome of autoimmunity and abnormal leukocyte homeostasis. Blood. 2011;117(10):2883–6. https://doi.org/10.1182/blood-2010-07-295501.
Eni-Aganga I, Lanaghan ZM, Balasubramaniam M, Dash C, Pandhare J. PROLIDASE: a review from discovery to its role in health and disease. Front Mol Biosci. 2021;8:723003. https://doi.org/10.3389/fmolb.2021.723003.
Klar A, et al. Prolidase deficiency: it looks like systemic lupus erythematosus but it is not. Eur J Pediatr. 2010;169(6):727–32. https://doi.org/10.1007/s00431-009-1102-1.
Hodgson R, et al. Prolidase deficiency causes spontaneous T cell activation and lupus-like autoimmunity. J Immunol Author Choice. 2023;210(5):547. https://doi.org/10.4049/jimmunol.2200212.
Rossignol F, et al. Quantitative analysis of the natural history of prolidase deficiency: description of 17 families and systematic review of published cases. Genet Med Off J Am Coll Med Genet. 2021;23(9):1604. https://doi.org/10.1038/s41436-021-01200-2.
He Y, et al. P2RY8 variants in lupus patients uncover a role for the receptor in immunological tolerance. J Exp Med. 2022;219(1):e20211004. https://doi.org/10.1084/jem.20211004.
Tusseau M, Belot A. ‘P2RY8-son’ break of tolerance promotes SLE. J Exp Med. 2022;219(1):e20211972. https://doi.org/10.1084/jem.20211972.
Elhani I, Riller Q, Boursier G, Hentgen V, Rieux-Laucat F, Georgin-Lavialle S. A20 haploinsufficiency: a systematic review of 177 cases. J Invest Dermatol. 2023. https://doi.org/10.1016/j.jid.2023.12.007.
Xu L, et al. Loss-of-function variants in SAT1 cause X-linked childhood-onset systemic lupus erythematosus. Ann Rheum Dis. 2022;81(12):1712–21. https://doi.org/10.1136/ard-2022-222795.
Boussard C, et al. DOCK11 deficiency in patients with X-linked actinopathy and autoimmunity. Blood. 2023. https://doi.org/10.1182/blood.2022018486.
Block J, et al. Systemic inflammation and normocytic anemia in DOCK11 deficiency. N Engl J Med. 2023;389(6):527–39. https://doi.org/10.1056/NEJMoa2210054.
Pescarmona R, et al. Comparison of RT-qPCR and Nanostring in the measurement of blood interferon response for the diagnosis of type I interferonopathies. Cytokine. 2019;113:446–52. https://doi.org/10.1016/j.cyto.2018.10.023.
Wahadat MJ, et al. Serum IFNα2 levels are associated with disease activity and outperform IFN-I gene signature in a longitudinal childhood-onset SLE cohort. Rheumatol Oxf Engl. 2023;62(8):2872–9. https://doi.org/10.1093/rheumatology/keac698.
Nombel A, et al. Assessment of type I interferon response in routine practice in France in 2022. RMD Open. 2023; 9. https://doi.org/10.1136/rmdopen-2023-003211.
Rodríguez-Carrio J, et al. 2022 EULAR points to consider for the measurement, reporting and application of IFN-I pathway activation assays in clinical research and practice. Ann Rheum Dis. 2023;82(6):754–62. https://doi.org/10.1136/ard-2022-223628.
Rice GI, et al. Assessment of interferon-related biomarkers in Aicardi-Goutières syndrome associated with mutations in TREX1, RNASEH2A, RNASEH2B, RNASEH2C, SAMHD1, and ADAR: a case-control study. Lancet Neurol. 2013;12(12):1159–69. https://doi.org/10.1016/S1474-4422(13)70258-8.
Picard C, et al. Anti-C1q autoantibodies as markers of renal involvement in childhood-onset systemic lupus erythematosus. Pediatr Nephrol. 2017;32(9):1537–45. https://doi.org/10.1007/s00467-017-3646-z.
Hartl J, et al. Autoantibody-mediated impairment of DNASE1L3 activity in sporadic systemic lupus erythematosus. J Exp Med. 2021;218(5):e20201138. https://doi.org/10.1084/jem.20201138.
Salzer E, et al. B-cell deficiency and severe autoimmunity caused by deficiency of protein kinase C δ. Blood. 2013;121(16):3112–6. https://doi.org/10.1182/blood-2012-10-460741.
Kuehn HS, et al. Loss-of-function of the protein kinase C δ (PKCδ) causes a B-cell lymphoproliferative syndrome in humans. Blood. 2013;121(16):3117–25. https://doi.org/10.1182/blood-2012-12-469544.
Lei L, et al. Successful use of ofatumumab in two cases of early-onset juvenile SLE with thrombocytopenia caused by a mutation in protein kinase C δ. Pediatr Rheumatol. 2018;16(1):61. https://doi.org/10.1186/s12969-018-0278-1.
Gu H, et al. Sirolimus is effective in autoimmune lymphoproliferative syndrome-type III: a pedigree case report with homozygous variation PRKCD. Int J Immunopathol Pharmacol. 2021;35:20587384211025936. https://doi.org/10.1177/20587384211025934.
Moreews M, et al. mTOR activation underlies enhanced B cell proliferation and autoimmunity in PrkcdG510S/G510S mice. J Immunol. 2023;210:1209–21. https://doi.org/10.4049/jimmunol.2200818.
Akbar L, Alsagheir R, Al-Mayouf SM. Efficacy of a sequential treatment by belimumab in monogenic systemic lupus erythematosus. Eur J Rheumatol. 2020;7(4):184–9. https://doi.org/10.5152/eurjrheum.2020.20087.
Chen F, et al. Belimumab in childhood systemic lupus erythematosus: a review of available data. Front Immunol. 2022;13:940416. https://doi.org/10.3389/fimmu.2022.940416.
Gómez-Arias PJ, Gómez-García F, Hernández-Parada J, Montilla-López AM, Ruano J, Parra-Peralbo E. Efficacy and safety of Janus kinase inhibitors in type I interferon-mediated monogenic autoinflammatory disorders: a scoping review. Dermatol Ther. 2021;11(3):733–50. https://doi.org/10.1007/s13555-021-00517-9.
Berrada KR, et al. Lung transplantation under a Janus kinase inhibitor in three patients with SAVI syndrome. J Clin Immunol. 2023. https://doi.org/10.1007/s10875-023-01595-4.
Anifrolumab normalizes the type I interferon signature in a cohort of patients with type I interferonopathies. ACR meeting abstracts. https://acrabstracts.org/abstract/anifrolumab-normalizes-the-type-i-interferon-signature-in-a-cohort-of-patients-with-type-i-interferonopathies/. Accessed 17 Dec 2023.
Brodszki N, et al. European Society for Immunodeficiencies (ESID) and European reference network on rare primary immunodeficiency, autoinflammatory and autoimmune diseases (ERN RITA) complement guideline: deficiencies, diagnosis, and management. J Clin Immunol. 2020;40(4):576–91. https://doi.org/10.1007/s10875-020-00754-1.
Mackensen A, et al. Anti-CD19 CAR T cell therapy for refractory systemic lupus erythematosus. Nat Med. 2022;28(10):10. https://doi.org/10.1038/s41591-022-02017-5.
Mougiakakos D, et al. CD19-targeted CAR T cells in refractory systemic lupus erythematosus. N Engl J Med. 2021;385(6):567–9. https://doi.org/10.1056/NEJMc2107725.
Li G, et al. Genetic heterogeneity in Chinese children with systemic lupus erythematosus. Clin Exp Rheumatol. 2021;39(1):214–22.
Misztal MC, et al. Genome-wide sequencing identified rare genetic variants for childhood-onset monogenic lupus. J Rheumatol. 2023;50(5):671–5. https://doi.org/10.3899/jrheum.220513.
de Inocencio J, et al. Somatic NOD2 mosaicism in Blau syndrome. J Allergy Clin Immunol. 2015;136(2):484-487.e2. https://doi.org/10.1016/j.jaci.2014.12.1941.
Jiménez-Treviño S, González-Roca E, Ruiz-Ortiz E, Yagüe J, Ramos E, Aróstegui JI. First report of vertical transmission of a somatic NLRP3 mutation in cryopyrin-associated periodic syndromes. Ann Rheum Dis. 2013;72(6):1109–10. https://doi.org/10.1136/annrheumdis-2012-202913.
Labrousse M, et al. Mosaicism in autoinflammatory diseases: cryopyrin-associated periodic syndromes (CAPS) and beyond. A systematic review. Crit Rev Clin Lab Sci. 2018;55:432–42. https://doi.org/10.1080/10408363.2018.1488805.
Holzelova E, et al. Autoimmune lymphoproliferative syndrome with somatic Fas mutations. N Engl J Med. 2004;351(14):1409–18. https://doi.org/10.1056/NEJMoa040036.
Beck DB, et al. Somatic mutations in UBA1 and severe adult-onset autoinflammatory disease. N Engl J Med. 2020;383(27):2628–38. https://doi.org/10.1056/NEJMoa2026834.
Almlöf JC, et al. Whole-genome sequencing identifies complex contributions to genetic risk by variants in genes causing monogenic systemic lupus erythematosus. Hum Genet. 2019;138(2):141–50. https://doi.org/10.1007/s00439-018-01966-7.
Charras A, et al. Panel sequencing links rare, likely damaging gene variants with distinct clinical phenotypes and outcomes in juvenile-onset SLE. Rheumatology. 2023;62(SI2):SI210–25. https://doi.org/10.1093/rheumatology/keac275.
Boulisfane-El Khalifi S, et al. COPA syndrome as a cause of lupus nephritis. Kidney Int Rep. 2019;4:1187–1189. https://doi.org/10.1016/j.ekir.2019.04.014.
Crow YJ, AGS group. Clinical non-penetrance associated with biallelic mutations in the RNase H2 complex. J Clin Immunol. 2023;43(4):706–8. https://doi.org/10.1007/s10875-023-01438-2.
Javierre BM, et al. Changes in the pattern of DNA methylation associate with twin discordance in systemic lupus erythematosus. Genome Res. 2010;20(2):170–9. https://doi.org/10.1101/gr.100289.109.
Garau J, et al. Altered DNA methylation and gene expression predict disease severity in patients with Aicardi-Goutières syndrome. Clin Immunol Orlando Fla. 2023;249:109299. https://doi.org/10.1016/j.clim.2023.109299.
Acknowledgements
We thank the patients and families. We also thank Véréna Landel for her help proofreading the manuscripts.
Funding
This research was funded by ANR (ANR-21-CE17-0064 [SOCSIMMUNITY]]), ANR-21-RHUS-08 [COVIFERON]) from the ANR–Recherche Hospitalo Universitaire Program; by the Horizon Europe (01057100 [UNDINE]) from the HORIZON-HLTH-2021-DISEASE-04; le Centre de référence des rhumatismes inflammatoires, des interféronopathies et des maladies autoimmunes (RAISE).
Author information
Authors and Affiliations
Contributions
M.T: Wrote the initial draft and contribute to the conceptualisation of the manuscript. S.K-P: made all the figures and did critical review of the manuscript, J.C, S.V, L.K, S.B, AL. M: did critical review of manuscript, F.R-L, B.B-M: made critically revised the manuscript and contribute to the conceptualisation of the manuscript, A.B: conceptualized the work, critically revised the manuscript and approved the version to be published.
Corresponding author
Ethics declarations
Credits
All the figures were created with BioRender.com.
Competing Interests
AB reports consulting fees from Kabi, Roche Chugai, GlaxoSmithKline, AbbVie, Novartis, and Boehringer Ingelheim; research grants from Boehringer Ingelheim, ANR, and Horizon Europe outside the scope of this comment; and is an unpaid co-chair of the French National Network on Rare Autoimmune and Autoinflammatory Diseases. All other authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tusseau, M., Khaldi-Plassart, S., Cognard, J. et al. Mendelian Causes of Autoimmunity: the Lupus Phenotype. J Clin Immunol 44, 99 (2024). https://doi.org/10.1007/s10875-024-01696-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10875-024-01696-8