Abstract
The network perspective on psychopathology suggests that mental disorders can be regarded as networks of elements that influence each other. In this study, we used network analysis to explore the temporal interactions of anxiety and depression symptoms at the level of day-to-day experiences and find potential explanatory pathways for their comorbidity. We collected intensive longitudinal data from a sample of undergraduate students and fitted a Multilevel Vector Autoregressive model on GAD and MDD DSM-5 symptoms. “Sad mood” and “Concentration difficulties” were responsible for the most connections between anxiety and depression symptoms and were also among the most central symptoms. It is possible that anxio-depressive comorbidity can be explained by the presence of “Sad mood” and “Concentration difficulties” and targeting these two symptoms in therapy can lead to beneficial effects in comorbid cases.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
In cases primarily diagnosed with anxiety, 63% have a current depressive disorder, while 81% develop depression at some point in their lives (Lamers et al., 2011). Even though percentages vary across studies, anxiety and depression are considered among the most frequently co-occurring mental disorders (Cummings et al., 2014). Comorbidity leads to higher levels of impairment in different areas of life as opposed to the situation when there is only one diagnosis (Hirschfeld, 2001). For instance, in comparison with non-comorbid cases, comorbid anxiety and depression cases show a higher number of suicide attempts, more significant academic problems (Lewinsohn et al., 1995), poorer quality of life (Zhou et al., 2017) and global functioning (Fusar-Poli et al., 2014), and greater risk for cardiovascular disease (Kemp et al., 2012).
Efforts to explain the comorbidity between anxiety and depression have traditionally revolved around finding a latent variable outside anxiety and depression per se. For instance, high neuroticism is considered a risk factor for comorbidity of anxiety and depression (Lamers et al., 2011). However, neuroticism is generally correlated with different psychopathological aspects (Brandes & Tackett, 2019) and cannot be considered a specific explanation for anxiety and depression comorbidity. A popular theoretical model on this subject is the Tripartite Model (Clark & Watson, 1991), which suggests that anxiety and depression are comorbid due to the high negative affectivity that characterises the two. However, in the most recent review of literature on the topic, Cummings et al. (2014) argue that the Tripartite Model does not fully account for the heterogeneity of anxiety disorders and manifests variability across studies on what component of the Tripartite Model (i.e., physiological hyper-arousal, low positive affect, high negative affect) can be considered an explanation for anxiety-depression comorbidity.
Recently, the study of comorbidity in psychopathology was approached from a different perspective – network analysis (Cramer et al., 2010). Network analysis is a relatively new paradigm that conceptualises mental disorders as causal systems of interrelated elements rather than categories or latent variables. Instead of being considered indicators of latent disorders, elements of the network (e.g., symptoms, personality traits, attitudes, feelings) form the network of interacting elements, from which a disorder can emerge.
Identification of Central Symptoms
Node centrality summarizes specific patterns of associations of a node with the rest of the network (Bringmann et al., 2019; Costantini et al., 2015). Usually, estimating node centrality is one of the main aims in a network analysis study, as it can help obtain insights on the relative importance of symptoms within a disorder. Multiple studies have tackled this subject regarding anxiety and depression comorbidity, operationalised through the DSM-5 diagnostic criteria for Major Depressive Disorder (MDD) and Generalized Anxiety Disorder (GAD). Symptoms “Sad mood” and “Excessive worry” have been almost ubiquitously identified as the most central (or highly central) in cross-sectional networks (An et al., 2019; Bai et al., 2021; Beard et al., 2016; Bi & Li, 2021; Cramer et al., 2010; Fried et al., 2016; Garabiles et al., 2019; Konac et al., 2021; McElroy et al., 2018; Peel et al., 2021; Ren et al., 2021; Tundo et al., 2021). Symptoms “Anhedonia”, “Worthlessness”, and “Fatiguability” were also identified as highly central, although with greater variability across studies.
Networks estimated on cross-sectional data do not allow making inferences regarding variability within individuals, and they allow estimating only undirected connections, not being able to distinguish the direction of the effects. Conversely, networks estimated on intensive longitudinal data allow modelling between-subject and within-subject dynamics separately (Costantini et al., 2019; Epskamp et al., 2018). Furthermore, at the within-subject level, longitudinal data can be used not only to infer contemporaneous connections, but also to estimate temporal networks, which encode predictions across subsequent time-points, thus providing directed connections (Bringmann et al., 2013). In turn, directed connections allow estimating directed centrality indices (Costantini et al., 2015) (e.g., instrength – how much a node is temporally dependent on other nodes, and outstrength – how much a node predicts variations of other nodes in the future), thus allowing a distinction between nodes that are strongly predicted by other nodes at previous timepoints and nodes that predict other nodes over time.
Two longitudinal network studies used Ecological Momentary Assessments (EMA) to address the subject of centrality in joint anxiety and depression networks. However, the existing longitudinal networks are only partially comparable with those estimated in cross-sectional studies because the reported networks included aspects outside of the DSM-5 criteria for MDD and GAD. For instance, in the study of Vos et al. (2017), “feeling happy” and “feeling anxious” had the highest outstrength centrality, “feeling happy” being a non-DSM feature. Fisher et al. (2017) have obtained similar results as two non-DSM symptoms have emerged with high levels of outstrength – “feeling positive” and “feeling hopeless”. Interestingly, in both studies, symptoms that were repeatedly found as highly central in cross-sectional networks (i.e., “Sad mood”, “Excessive worry”) were among the least influential in the two EMA studies. In both cases, “Sad mood” had the highest instrength centrality and very low outstrength centrality, meaning that “Sad mood” is frequently a successor of other anxious-depressive symptoms rather than their predictor. Similar results were obtained for the symptom “Excessive worry” in the study of Fisher et al. (2017) (Vos et al. (2017) did not include “Excessive worry” in their network).
In summary, there are numerous cross-sectional network studies on the topic of depression and anxiety comorbidity but a lot less longitudinal studies that would allow the estimation of the direction of edges and directed centrality indices. These studies indicate that “Sad mood” and “Excessive worry” are highly central nodes, but intensive longitudinal designs point out that they are more likely the outcomes of other symptoms of depression and anxiety rather than their source. Future studies that would clarify the role of these nodes are needed. Also, the few existing longitudinal studies have computed their networks on a different set of symptoms than those proposed by DSM-5, and therefore did not account for the majority of anxiety and depression characteristics. We fill a gap in the literature by studying DSM-5 anxiety and depression symptoms dynamic in a time-series network, and compute directed centrality indices which will help identify the most influential nodes in the network, responsible for the comorbidity of the two disorders.
Bridge Centrality
Jones et al. (2021) have introduced a method for identifying bridge symptoms which quantifies the centrality of nodes by considering only their connections with nodes from another community. For example, a network of anxiety and depression consists of two theoretical communities of nodes: one comprised of symptoms of depression and the other of symptoms of anxiety. A node has high bridge centrality if it has the most connections that go outside of the community that it belongs. Assuming that comorbidity between two disorders can be explained by connections between specific symptoms, and that some symptoms are correlated to the other disorder more strongly than others, using bridge centrality metrics will help to identify symptom level explanations regarding the comorbidity of anxiety and depression. This method applied in some cross-sectional network studies, and “Sad mood” has once again emerged as a highly central symptom (Bai et al., 2021; Beard et al., 2016; Garabiles et al., 2019; Konac et al., 2021; Ren et al., 2021). However, there is more heterogeneity across studies in this regard than the results on regular centrality. Some did not obtain high bridge centrality values for “Sad mood” (Kaiser et al., 2021) and different symptoms like “Psychomotor agitation/retardation” (Beard et al., 2016; Bi & Li, 2021; Kaiser et al., 2021), “Worry” (Konac et al., 2021), “Restlessness” (Garabiles et al., 2019; Ren et al., 2021), “Anhedonia” (Bai et al., 2021; Garabiles et al., 2019) were found to have the most connections with the nodes from the opposite community (had high bridge centrality).
The Present Study
Aim 1
Analyse centrality and bridge centrality of anxiety and depression symptoms based on intensive longitudinal data.
To add to the previous efforts to explain anxiety and depression comorbidity through network analysis, the main aim of this study is estimating bridge centrality metrics on a time-series network of depression and anxiety symptoms. Studies that used bridge centrality metrics did not consider that certain symptoms belong both to anxiety and depression. For example, in Garabiles et al. (2019) and in Kaiser et al. (2021), “Concentration difficulties”, “Sleep difficulties”, and “Fatiguability” were considered only as part of the depression community of nodes. Although this is congruent with the questionnaires used in the two studies (i.e., PHQ-9 and GAD-7), these symptoms are characteristics of both MDD and GAD (American Psychiatric Association, 2013). We will address this issue by computing bridge centrality for both possible symptom compositions of communities.
Aim 2
Analyse and describe the role of “Sad mood” in anxiety and depression comorbidity. Given the emergence of “Sad mood” as a highly central symptom in multiple studies, we will accord attention to describing its role in our time-series network and identifying possible pathways through which it is related to other symptoms.
Method
Participants
Data was collected from a sample of 145 undergraduate Romanian psychology students in exchange for course credit. Five participants were removed because they had less than 20 pairs of consecutive measurements, and other 14 participants were removed because they did not show any variance in four or more variables and including these participants resulted in model convergence issues. The final sample thus consisted of 126 participants (mage = 22.11 years, S.D. = 6.09 years, 88.88% female). According to DSM-5 diagnostic criteria, levels of depression above the clinical threshold were manifested at baseline by 41.26% of participants, 30.95% had clinical levels of anxiety, and 22.22% had clinical levels of both. Only 3.96% did not report the presence of any anxious or depressive symptoms at baseline. During the enrolment stage, participants were presented with a consent form informing them about the study's purpose, confidentiality, right of withdrawal, and offered contact information.
Procedure
The possibility to enrol in the study was announced to students at the beginning of several lectures at [masked for peer review]. Participants were verbally explained what the participation in the study implies. To assist the decision process, the same information was also provided in a PDF that contained step-by-step instructions regarding the duration of the study, number of questions, nature of the questions, number of daily measurements, the schedule of daily notifications, information about how to use PIEL survey app as a participant and contact information in case they needed further assistance before or during the study. Potential participants were given a link, in which they found detailed information about the study procedure and provided informed consent. Those that agreed to participate, they were asked to fill in an enrolment questionnaire, which investigated demographics, their level of depression and anxiety, and inclusion criteria. To be eligible, participants had to indicate that they had a smartphone that would allow the installation of the experience sampling application, and that their daily schedule would allow them to access their phone whenever they received a notification. The experience sampling procedure was implemented through the PIEL survey application (Jessup et al., 2012). Participants answered a set of questions concerning anxious and depressive symptoms three times per day at a 4-h interval from one measurement to another, over a period of 21 days during the academic year. The first daily beep was adapted to each participant waking hour to avoid potential data loss caused by the overlap between sleeping hours and beeps. For example, if a participant indicated 8:00 AM as their usual waking hour, PIEL survey app would automatically send them a notification at noon, 4:00 PM, and 8:00 PM. A mean of 57.74 (SD = 4.54) completions was obtained per participant out of a possible 63, with a 9.16% missingness rate in the total sample included in the final analysis.
Measures
Depressive Symptoms
Romanian version of the Patient Health Questionnaire (Kroenke et al., 2001) (PHQ-9) was used to assess depressive symptomatology at baseline. PHQ-9 has nine items measured on 4 points Likert scale from 0 (Not at all) to 3 (Nearly every day). The scores for PHQ-9 range between 0 and 27. Internal consistency for this scale in the recruitment phase in our study was excellent (α = 0.88).
Anxious Symptoms
The Generalised Anxiety Disorder Questionnaire-IV (Newman et al., 2002) was used to assess anxiety symptoms at baseline. GAD-Q-IV consists of 11 dichotomous items corresponding to DSM-IV and DSM-V criteria for GAD, with Yes and No as response options. The scale also has an open-ended question regarding the content of worries and two 9-point Likert scale questions that assess the impairment associated with anxious symptomatology. As the wording of GAD-Q-IV is similar to that of DSM-V criteria, we used the Romanian version of DSM-V to translate the questionnaire’s items. GAD-Q-IV showed a good level of reliability in the recruitment phase (α = 0.8).
Ecological Momentary Assessments
We used the PHQ-9 and GAD-Q-IV questionnaires as the basis for the EMA items and adapted them for the EMA context. Items used for EMA are presented in Table 1, together with their descriptive statistics. Instructions and response options were reformulated so that they refer to momentary states. Participants indicated on a 4-point Likert scale if they experienced a particular symptom in the past 4 h (since the last beep or since waking up), the options being 1 = “Not at all”, 2 = “A short time”, 3 = “For an extended period of time”, and 4 = “Most of the time”. Items 1 and 2 of GAD-Q-IV were combined into one item, referring to the excess of worry. Within and between-subjects reliability for the resulted items to measure anxiety and depression symptoms were high in all cases. Specifically, reliability values for anxiety were αBP = 0.94 and αWP = 0.86, and for depression αBP = 0.93 and αWP = 0.81.
Data Analysis
We estimated the network structure of anxiety and depression symptoms as a multilevel vector auto-regression model (MVAR) with orthogonal random effects (Bringmann et al., 2013; Epskamp et al., 2018), using the mlVAR (Epskamp et al., 2021) package in R (R Core Team, 2022), version 0.5. and applied a False Discovery Rate controlling procedure described in Bringmann et al. (2013). To estimate bridge strength, bridge indegree, and outdegree (Jones et al., 2021) we used version 1.4.0 of R package networktools (Jones, 2021). Regular centrality measures were also investigated, namely instrength and outstrength (Bringmann et al., 2019). A more extensive description of the data analysis is presented in the Supplemental Materials.
To calculate the proportion of participants potentially eligible for a MDD and/or GAD diagnosis presented in the Participants section, we followed DSM-5 diagnostic thresholds for Major Depressive Disorder and Generalised Anxiety Disorder. An answer of 1 = “Yes” for GAD-Q-IV was considered an indicator for the presence of an anxiety symptom, while an answer of at least 2 = “More than half the days” (at least 1 = “Several days” for item 9) was considered an indicator for the presence of a depression symptoms (The F.A.S.T Lab, 2017).
Results
Network Estimation
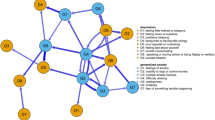
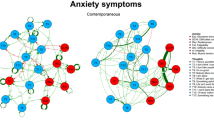
To fit a multilevel VAR model, the data must satisfy three assumptions (Bringmann et al., 2013). The first states that the measurements must be equally spaced in time, and the last measurement in a day cannot predict the subsequent measurement in the morning. We addressed this assumption by setting a fixed time interval of 4 h between measurements. Furthermore, the mlVAR procedure in R deals with the overnight prediction issue by removing the last measurement of each day in the lagged variables. The second assumption is that predicted variables are lagged at the same level. In this case, we only considered the t-1 lag. The third assumption states that data must be stationary, meaning that for each participant, the mean and variance must stay unchanged over time for every variable (Bringmann et al., 2013). We tested this assumption with the Kwiatkowski-Phillips-Schmidt-Shin test on every variable separately for each participant. The test showed that the assumption of stationarity was satisfied for most of the data, 81.14% for level stationarity and 83.83% for trend stationarity. As most of the data was stationary, we did not detrend it. Temporal and contemporaneous networks are illustrated in Fig. 1.
Temporal and contemporaneous networks of anxious and depressive symptoms. Included edges are significant at p < 0.009 for the temporal network and p < 0.022 for the contemporaneous network. The nodes are colour coded to ease the distinction between unique anxiety symptoms, unique depression symptoms, and shared symptoms of both diagnoses. Different geometrical shapes indicate the communities identified empirically through the Walktrap algorithm. Community detection analysis is described in the Supplementary Materials
Centrality
Bridge centrality is illustrated in Fig. 2. We estimated bridge centrality twice with different sets of communities. This was necessary because “Concentration difficulties” and “Fatigability” are considered as features of both anxiety and depression (American Psychiatric Association, 2013). We noticed considerable variation in bridge centrality in the two versions, caused by the node “Concentration difficulties”. Because “Concentration difficulties” had many connections with depressive symptoms, when moving it to the depression community, the number of edges that go inwards and outwards to the anxiety community decreased for multiple nodes, including “Concentration difficulties”. Regular centrality indices are presented in Fig. 3. “Concentration difficulties”, “Worthlessness”, “Anhedonia”, and “Sad mood” were the most influential symptoms as they had the highest outstrength values. “Sad mood” and “Worthlessness” also had high instrength, as well as “Restlessness” and “Fatiguability”. In the contemporaneous network, “Excessive worry” had the highest strength centrality.
Bridge centrality of the temporal and contemporaneous networks. Anxiety = estimated bridge centrality with the inclusion of shared features (“Concentration difficulties” and “Fatiguability”) in the anxiety community. Depression = estimated bridge centrality with the inclusion of shared features in the depression community
Discussion
In the current study, we investigated the time-series network of anxiety and depression symptoms in a sample of undergraduate students. Our main goal was to identify symptoms that could potentially explain why anxiety and depression symptoms often are emerge together, and also to extend the existing literature on cross-sectional networks on this subject with a longitudinal approach.
Aim 1: Centrality of Anxiety and Depression Symptoms
Several symptoms have been found to have important roles in the network of anxiety and depression. “Concentration difficulties” was the most influential node in the overall network with the highest outstrength centrality. “Concentration difficulties” had only one direct edge with an anxiety symptom, namely “Restlessness”, but was related to all depressive symptoms associated with anxious features: “Sad mood”, “Worthlessness”, and “Anhedonia”. In other words, our network indicated that “Concentration difficulties” exacerbates depressive symptoms which in turn lead to anxious symptomatology. Having “Concentration difficulties” as a central symptom is a surprising result as this symptom is usually regarded as a peripheral aspect of depression and anxiety rather than a core feature. However, the appearance of mindfulness-based interventions has highlighted the importance of “Concentration difficulties” for anxiety and depression as the improvement of affectivity is associated with improvement through mindfulness in attention concentration capabilities (Ricarte et al., 2015; Williams, 2008). The results regarding “Concentration difficulties” should also be interpreted in the light of the fact that our participants were enrolled in university courses. Good cognitive performance is arguably more important for students than for someone who is not involved in an educational program, so not being able to concentrate during lectures or while preparing exams could lead to particularly high levels of distress (as reflected by feeling “Sad”, “Worthless”, or “Anhedonic”).
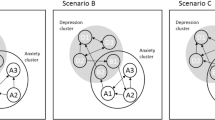
In the first look at anxiety and depression comorbidity through the network perspective, Cramer et al. (2010) have proposed that shared features of these disorders are key elements for comorbidity. The authors theorised that disorder-specific symptoms induce the shared anxious-depressive features, leading to the appearance of symptomatology from the opposite community. This theory was recently tested on time-series data but did not obtain favourable results (Groen et al., 2020). However, in the latter study, worries and irritability were considered as shared symptoms, which are rather anxiety-specific symptoms than shared features. Our results also diverge from Cramer’s theory about shared features. Although “Concentration difficulties” is a shared feature, in our network disorder-specific symptoms also formed between-community associations, while fatiguability (the other shared feature) had very low bridge centrality levels.
“Anhedonia” was another highly central symptom. However, bridge outdegree of “Anhedonia” diminished when the shared features were moved to the depression community. This is explained by the fact that two out of three predictive edges of “Anhedonia” point toward the shared features, and only one towards an anxiety-specific symptom – “Irritability”. Interestingly, “Anhedonia” formed a “vicious loop” relationship type with “Concentration difficulties”. It seems that not being able to concentrate on daily activities also limits the extent to which one can enjoy them or have an interest in them. Furthermore, engaging in such activities will lead to fatigue and will further harden the investment of any other attentional resources. It would be interesting to explore this relationship in future studies as a mechanism that sustains symptoms of anxiety and depression or contributes to their development. Past research has already emphasised the importance of “Anhedonia” by showing that psychotherapy focused on this symptom leads to an overall improvement in depression and anxiety (Craske et al., 2019).
“Worthlessness” was also one of the most central nodes in temporal networks and the only symptom connected to “Suicidal ideations”. It is possible that “Worthlessness” acts as a mediator between “Suicidal ideation” and other symptoms, such as “Sad mood” and “Concentration difficulties”. We can speculate that individuals end up feeling bad about themselves (worthless) for being often sad and unable to concentrate even on simple tasks. This, in turn, may lead to development of suicidal ideation. In line with our results, the Interpersonal Theory of Suicide posits that a concept closely related to worthlessness – perceived burdensomeness– is one of the two main elements that is responsible for passive suicidal ideation (Van Orden et al., 2010). It is also worth noting the vicious-circles that involve “Worthlessness”: Not only “Worthlessness” predicts “Sad mood” and “Suicidal ideation”, but it appears that it is also maintained by these symptoms in a continuous vicious feedback-loop.
Aim 2: The Role of “Sad mood” in Anxiety and Depression Comorbidity
Similar to past cross-sectional networks, we found high centrality levels for “Sad mood”. This indicates that the presence of “Sad mood” is associated with higher anxio-depressive symptomatology both at between-subject and within-subject levels. That is, individuals that experience “Sad mood” manifest higher levels of anxio-depressive symptomatology, but also experiencing “Sad mood” at any moment during the day will be followed by the appearance of other depressive or anxious symptoms. Differentiating between-subject effects from within-subject effects is crucial as sometimes the same variables can have a different direction of association for different types of effects (Epskamp et al., 2018).
Similar to Groen et al. (2020) time-series network, “Sad mood” had high bridge centrality and had a direct effect on “Worries”. However, we were not able to differentiate between comorbid, depression-only, and anxiety-only participants as the effect of “Sad mood” on “Worries” in Groen et al. (2020) was present only in the depression group and was reciprocal in the comorbid group. In our case, we can state that the effect is also present in participants from the general population. It is also important to mention that we used a different method than Groen et al. (2020) to estimate the bridge effects, and both methods pointed towards “Sad mood” being a bridge symptom. In the overall network, when not specifying the community structure, “Sad mood” showed lower centrality levels, indicating that this symptom is more important for the comorbidity of the two disorders than for the disorders themselves. This is somehow consistent with the results of Fisher et al. (2017) and Vos et al. (2017), as in their studies, “Sad mood” has manifested low centrality in the overall network. However, both studies included elements of positive affect that were highly correlated and could have potentially reduced the centrality of other symptoms or over-shadowed other significant edges but not as strongly interconnected as the edges between the positive affectivity nodes. For example, in Vos et al. (2017), happiness was the most central node, and predicted other conceptually close nodes as cheerful, enthusiastic, energetic, satisfied, and talkative.
Besides the high centrality in the temporal network, “Sad mood” had the highest bridge centrality in the contemporaneous network on all three computed metrics. All anxiety symptoms were connected directly with “Sad mood”, except “Muscle tension” and “Difficulties controlling worries” that were separated from it only by one node. Overall, “Sad Mood” seems to be associated more with anxiety symptoms than with symptoms from its own community, both in the temporal and contemporaneous network and might be a key element in explaining and possibly inducing anxiety and depression comorbidity.
Strengths
This study is a valuable addition to the vast literature on cross-sectional networks of anxiety and depression symptoms as it’s the first one to address this topic using a time-series network. We had a good representation of DSM-5 MDD and GAD symptomatology in the estimated network and identified several symptoms and mechanisms that might have an important role for these disorders. Additionally, we conducted our analyses by considering the possibility of the shared symptoms to be part of both communities. We also applied bridge centrality metrics on a time-series network which was not attempted before.
Our results could also be of potential interest to practicians. For instance, knowing that depression symptoms are predictive of anxiety symptoms at within-person level, treatment could prioritise the reduction of depressive psychopathology in comorbid cases. It is also possible that reduction of central symptoms “Sad mood”, “Anhedonia” and “Concentration difficulties” could be a key mechanism in treatment of depression and anxiety cases, and comorbid cases as well. Future research should investigate if it’s possible to specifically target “Sad mood” and “Concentration difficulties” in psychotherapy and obtain a general improvement for the client. For example, Emotion-Focused therapy proposes evocation and exploration of negative emotions as treatment strategies for depression Greenberg (2017). It is possible that targeting “Sad mood” with these strategies could lead to an overall improvement in patient’s affectivity. Regarding “Concentration difficulties”, this symptom is successfully targeted through mindfulness-based interventions (Ricarte et al., 2015; Williams, 2008). It is possible that combined Emotion-Focused and mindfulness therapy could be effective for cases where both anxiety and depression symptoms are present.
Limitations
The present study had several limitations. First, our sample consisted mainly of female undergraduate students, limiting the generalizability of the results only to the general youth population. A similar analysis in a clinical or/and more diverse sample could have yielded higher levels of variance in symptoms and led to different results, and also could have had more valuable implications for the disorders per se and not just for individual symptoms. However, many of our findings can be backed up by results from other studies on cross-sectional and time-series data. Another limitation is the relatively low number of beeps per day, which required us to instruct participants to give responses retrospectively for the past 4 h. Future studies should adopt procedures with more than three beeps that ask participants about their state at the moment of the assessment. The third limitation is that we were not able to include “Sleep difficulties” in the analysis, as it cannot vary across momentary measurements. Future research should develop methods that would make it possible to integrate “Sleep difficulties” in this kind of analysis.
Conclusions
Our results show that depression symptoms are more predictive of anxiety symptoms, and depression-specific symptoms predict the establishment of anxiety symptoms more often than vice-versa. Notably, “Sad mood” had the highest bridge centrality metrics both in the temporal and contemporaneous network. “Concentration difficulties” was the most central symptom in the entire network (when not considering the theoretical community structure). As these two symptoms had the most connections connecting anxiety and depression it is possible that they are responsible for the ties between anxious and depressive symptomatology.
Data Availability
Data and data analysis R scrypt are available under a CC-By Attribution 4.0 International license at https://osf.io/pt9dk/.
References
American Psychiatric Association. (2013). Diagnostic and Statistical Manual of Mental Disorders: DSM-5. American Psychiatric Publishing Inc.
An, M. H., Park, S. S., You, S. C., Park, R. W., Park, B., Woo, H. K., Kim, H. K., & Son, S. J. (2019). Depressive symptom network associated with comorbid anxiety in late-life depression. Frontiers in Psychiatry, 10. https://doi.org/10.3389/fpsyt.2019.00856
Bai, W., Xi, H. T., Zhu, Q. Q., Ji, M. M., Zhang, H. Y., Yang, B. X., Cai, H., Liu, R., Zhao, Y. J., Chen, L., Ge, Z. M., Wang, Z. W., Han, L., Chen, P., Liu, S., Cheung, T., Tang, Y. L., Jackson, T., An, F. R., & Xiang, Y. T. (2021). Network analysis of anxiety and depressive symptoms among nursing students during the COVID-19 pandemic. Journal of Affective Disorders, 294, 753–760. https://doi.org/10.1016/j.jad.2021.07.072
Beard, C., Millner, A. J., Forgeard, M. J. C., Fried, E. I., Hsu, K. J., Treadway, M. T., Leonard, C. V., Kertz, S. J., & Bjogvinsson, T. (2016). Network analysis of depression and anxiety symptom relationships in a psychiatric sample. Psychological Medicine, 46(16), 3359–3369. https://doi.org/10.1017/S0033291716002300
Bi, D. D., & Li, X. Y. (2021). Psychological flexibility profiles, college adjustment, and subjective well-being among college students in China: A latent profile analysis. Journal of Contextual Behavioral Science, 20, 20–26. https://doi.org/10.1016/j.jcbs.2021.01.008
Brandes, C. M., & Tackett, J. L. (2019). Contextualizing neuroticism in the Hierarchical Taxonomy of Psychopathology. Journal of Research in Personality, 81, 238–245. https://doi.org/10.1016/j.jrp.2019.06.007
Bringmann, L. F., Elmer, T., Epskamp, S., Krause, R. W., Schoch, D., Wichers, M., Wigman, J. T. W., & Snippe, E. (2019). What Do Centrality Measures Measure in Psychological Networks? Journal of Abnormal Psychology, 128(8), 892–903. https://doi.org/10.1037/abn0000446
Bringmann, L. F., Vissers, N., Wichers, M., Geschwind, N., Kuppens, P., Peeters, F., Borsboom, D., & Tuerlinckx, F. (2013). A Network Approach to Psychopathology: New Insights into Clinical Longitudinal Data. PLoS ONE, 8(4), e60188. https://doi.org/10.1371/journal.pone.0060188
Clark, L. A., & Watson, D. (1991). Tripartite Model of Anxiety and Depression - Psychometric Evidence and Taxonomic Implications. Journal of Abnormal Psychology, 100(3), 316–336. https://doi.org/10.1037/0021-843x.100.3.316
Costantini, G., Epskamp, S., Borsboom, D., Perugini, M., Mottus, R., Waldorp, L. J., & Cramer, A. O. J. (2015). State of the aRt personality research: A tutorial on network analysis of personality data in R. Journal of Research in Personality, 54, 13–29. https://doi.org/10.1016/j.jrp.2014.07.003
Costantini, G., Richetin, J., Preti, E., Casini, E., Epskamp, S., & Perugini, M. (2019). Stability and variability of personality networks. A tutorial on recent developments in network psychometrics. Personality and Individual Differences, 136, 68–78. https://doi.org/10.1016/j.paid.2017.06.011
Cramer, A. O. J., Waldorp, L. J., van der Maas, H. L. J., & Borsboom, D. (2010). Comorbidity: A network perspective. Behavioral and Brain Sciences, 33(2–3), 137. https://doi.org/10.1017/S0140525x09991567
Craske, M. G., Meuret, A. E., Ritz, T., Treanor, M., Dour, H., & Rosenfield, D. (2019). Positive affect treatment for depression and anxiety: A randomized clinical trial for a core feature of anhedonia. Journal of Consulting and Clinical Psychology, 87(5), 457–471. https://doi.org/10.1037/ccp0000396
Cummings, C. M., Caporino, N. E., & Kendall, P. C. (2014). Comorbidity of Anxiety and Depression in Children and Adolescents: 20 Years After. Psychological Bulletin, 140(3), 816–845. https://doi.org/10.1037/a0034733
Epskamp, S., Deserno, M. K., Bringmann, L. F., & Veenman, M. (2021). mlVAR: Multi-Level Vector Autoregression. In (Version 0.5) [R package]. https://CRAN.R-project.org/package=mlVAR
Epskamp, S., Waldorp, L. J., Mõttus, R., & Borsboom, D. (2018). The Gaussian Graphical Model in Cross-Sectional and Time-Series Data. Multivariate Behavioral Research, 53(4), 453–480. https://doi.org/10.1080/00273171.2018.1454823
Fisher, A. J., Reeves, J. W., Lawyer, G., Medaglia, J. D., & Rubel, J. A. (2017). Exploring the Idiographic Dynamics of Mood and Anxiety via Network Analysis. Journal of Abnormal Psychology, 126(8), 1044–1056. https://doi.org/10.1037/abn0000311
Fried, E. I., Epskamp, S., Nesse, R. M., Tuerlinckx, F., & Borsboom, D. (2016). What are “good” depression symptoms? Comparing the centrality of DSM and non-DSM symptoms of depression in a network analysis. Journal of Affective Disorders, 189, 314–320. https://doi.org/10.1016/j.jad.2015.09.005
Fusar-Poli, P., Nelson, B., Valmaggia, L., Yung, A. R., & McGuire, P. K. (2014). Comorbid Depressive and Anxiety Disorders in 509 Individuals With an At-Risk Mental State: Impact on Psychopathology and Transition to Psychosis. Schizophrenia Bulletin, 40(1), 120–131. https://doi.org/10.1093/schbul/sbs136
Garabiles, M. R., Lao, C. K., Xiong, Y. X., & Hall, B. J. (2019). Exploring comorbidity between anxiety and depression among migrant Filipino domestic workers: A network approach. Journal of Affective Disorders, 250, 85–93. https://doi.org/10.1016/j.jad.2019.02.062
Greenberg, L. S. (2017). Emotion-focused therapy of depression. Person-Centered and Experiential Psychotherapies, 16(2), 106–117. https://doi.org/10.1080/14779757.2017.1330702
Groen, R. N., Ryan, O., Wigman, J. T. W., Riese, H., Penninx, B. W. J. H., Giltay, E. J., Wichers, M., & Hartman, C. A. (2020). Comorbidity between depression and anxiety: assessing the role of bridge mental states in dynamic psychological networks. Bmc Medicine, 18(1). https://doi.org/10.1186/s12916-020-01738-z
Hirschfeld, R. M. (2001). The Comorbidity of Major Depression and Anxiety Disorders: Recognition and Management in Primary Care. Prim Care Companion J Clin Psychiatry, 3(6), 244–254. https://doi.org/10.4088/pcc.v03n0609
Jessup, G., Bian, S., Chen, Y. R., & Bundy, A. (2012). P.I.E.L. Survey Application Manual.
Jones, P. (2021). networktools: Tools for Identifying Important Nodes in Networks. In (Version 1.4.0) [R package]. https://CRAN.R-project.org/package=networktools
Jones, P. J., Ma, R., & McNally, R. J. (2021). Bridge Centrality: A Network Approach to Understanding Comorbidity. Multivariate Behavioral Research, 56(2), 353–367. https://doi.org/10.1080/00273171.2019.1614898
Kaiser, T., Herzog, P., Voderholzer, U., & Brakemeier, E. L. (2021). Unraveling the comorbidity of depression and anxiety in a large inpatient sample: Network analysis to examine bridge symptoms. Depression and Anxiety, 38(3), 307–317. https://doi.org/10.1002/da.23136
Kemp, A. H., Quintana, D. S., Felmingham, K. L., Matthews, S., & Jelinek, H. F. (2012). Depression, Comorbid Anxiety Disorders, and Heart Rate Variability in Physically Healthy, Unmedicated Patients: Implications for Cardiovascular Risk. Plos One, 7(2). https://doi.org/10.1371/journal.pone.0030777
Konac, D., Young, K. S., Lau, J., & Barker, E. D. (2021). Comorbidity Between Depression and Anxiety in Adolescents: Bridge Symptoms and Relevance of Risk and Protective Factors. Journal of Psychopathology and Behavioral Assessment, 43(3), 583–596. https://doi.org/10.1007/s10862-021-09880-5
Kroenke, K., Spitzer, R. L., & Williams, J. B. W. (2001). The PHQ-9. Journal of General Internal Medicine, 16(9), 606–613. https://doi.org/10.1046/j.1525-1497.2001.016009606.x
Lamers, F., van Oppen, P., Comijs, H. C., Smit, J. H., Spinhoven, P., van Balkom, A. J., Nolen, W. A., Zitman, F. G., Beekman, A. T., & Penninx, B. W. (2011). Comorbidity patterns of anxiety and depressive disorders in a large cohort study: The Netherlands Study of Depression and Anxiety (NESDA). Journal of Clinical Psychiatry, 72(3), 341–348. https://doi.org/10.4088/JCP.10m06176blu
Lewinsohn, P. M., Rohde, P., & Seeley, J. R. (1995). Adolescent psychopathology .3. The Clinical consequences of comorbidity. Journal of the American Academy of Child and Adolescent Psychiatry, 34(4), 510–519. https://doi.org/10.1097/00004583-199504000-00018
McElroy, E., Fearon, P., Belsky, J., Fonagy, P., & Patalay, P. (2018). Networks of Depression and Anxiety Symptoms Across Development. Journal of the American Academy of Child and Adolescent Psychiatry, 57(12), 964–973. https://doi.org/10.1016/j.jaac.2018.05.027
Newman, M. G., Zuellig, A. R., Kachin, K. E., Constantino, M. J., Przeworski, A., Erickson, T., & Cashman-McGrath, L. (2002). Preliminary Reliability and Validity of the Generalized Anxiety Disorder Questionnaire-IV: A Revised Self-Report Diagnostic Measure of Generalized Anxiety Disorder. Behavior Therapy, 33(2), 215–233. https://doi.org/10.1016/S0005-7894(02)80026-0
Peel, A. J., Armour, C., Buckman, J. E. J., Coleman, J. R. I., Curzons, S. C. B., Davies, M. R., Hubel, C., Jones, I., Kalsi, G., McAtarsney-Kovacs, M., McIntosh, A. M., Monssen, D., Mundy, J., Rayner, C., Rogers, H. C., Skelton, M., Ter Kuile, A., Thompson, K. N., Breen, G., & Eley, T. C. (2021). Comparison of depression and anxiety symptom networks in reporters and non-reporters of lifetime trauma in two samples of differing severity. J Affect Disord Rep, 6, 100201. https://doi.org/10.1016/j.jadr.2021.100201
R Core Team. (2022). R: A Language and Environment for Statistical Computing. In R Foundation for Statistical Computing. https://www.R-project.org/
Ren, L., Wang, Y. F., Wu, L., Wei, Z. H., Cui, L. B., Wei, X. Y., Hu, X. Y., Peng, J. X., Jin, Y. C., Li, F. Z., Yang, Q., & Liu, X. F. (2021). Network structure of depression and anxiety symptoms in Chinese female nursing students. Bmc Psychiatry, 21(1). https://doi.org/10.1186/s12888-021-03276-1
Ricarte, J. J., Ros, L., Latorre, J. M., & Beltran, M. T. (2015). Mindfulness-based intervention in a rural primary school: Effects on attention, concentration and mood. International Journal of Cognitive Therapy, 8(3), 258–270. https://doi.org/10.1521/ijct_2015_8_03
The F.A.S.T Lab. (2017). Printable Versions of imAPP Measures. Stanford Medicine. https://med.stanford.edu/fastlab/research/imapp/msrs/_jcr_content/main/accordion/accordion_content3/download_256324296/file.res/PHQ9%20id%20date%2008.03.pdf
Tundo, A., Musetti, L., Del Grande, C., de Filippis, R., Proietti, L., Marazziti, D., Gibertoni, D., & Dell’Osso, L. (2021). The relationship between depression with anxious distress DSM-5 specifier and mixed depression: A network analysis. Cns Spectrums, 26(3), 251–257. https://doi.org/10.1017/S1092852920000085
Van Orden, K. A., Witte, T. K., Cukrowicz, K. C., Braithwaite, S. R., Selby, E. A., & Joiner, T. E., Jr. (2010). The interpersonal theory of suicide. Psychological Review, 117(2), 575–600. https://doi.org/10.1037/a0018697
Vos, S. D., Wardenaar, K. J., Bos, E. H., Wit, E. C., Bouwmans, M. E. J., & Jonge, P. D. (2017). An investigation of emotion dynamics in major depressive disorder patients and healthy persons using sparse longitudinal networks. Plos One, 12(6). https://doi.org/10.1371/journal.pone.0178586
Williams, J. M. G. (2008). Mindfulness, Depression and Modes of Mind. Cognitive Therapy and Research, 32(6), 721–733. https://doi.org/10.1007/s10608-008-9204-z
Zhou, Y. J., Cao, Z. Q., Yang, M., Xi, X. Y., Guo, Y. Y., Fang, M. S., Cheng, L. J., & Du, Y. K. (2017). Comorbid generalized anxiety disorder and its association with quality of life in patients with major depressive disorder. Scientific Reports, 7.https://doi.org/10.1038/srep40511
Acknowledgements
We would like to express our gratitude to Rossella di Pierro from University of Milano-Bicocca for providing valuable suggestions for the writing of the manuscript. Our work received funding from the European Union’s Horizon 2020 research and innovation programme under the grant agreement No. 952464 (SM, FAS, GC) and from Exploratory Research Projects - 2020 Call under the registration code PN-III-P4-ID-PCE-2020-1964 (SM and FAS).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
We have no known conflict of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Marian, S., Costantini, G., Macsinga, I. et al. The Dynamic Interplay of Anxious and Depressive Symptoms in a Sample of Undergraduate Students. J Psychopathol Behav Assess 45, 150–159 (2023). https://doi.org/10.1007/s10862-022-10014-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10862-022-10014-8