Abstract
Objective
To determine whether euploidy rates and blastocyst development differ in a continuous culture medium under different CO2 concentrations.
Design and method
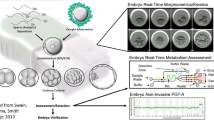
A single-center retrospective study was performed from July 2018 to October 2019 including 44 fresh cycles with at least four fresh mature oocytes (MII) without severe male factor infertility. Sibling MII were injected and cultured in Global®Total®LP under 6.0% (pHe = 7.374 ± 0.014) or 7.0% (pHe = 7.300 ± 0.013) CO2, 5.0% O2, and 89.0% or 88.0% N2. Analyzed variables were normally fertilized oocytes (2PN), cleavage rate, blastulation rate on day 5/2PN, usable blastocyst (blastocysts biopsied/2PN), and euploidy rates. Blastocyst’s trophectoderm biopsy was performed on day 5, 6, or 7 for genetic testing and mitochondrial DNA (mtDNA) quantification by next-generation sequencing.
Results
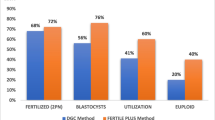
Women’s mean age was 33.0 ± 6.6 years old. From a total of 604 MII, no differences were found in normal fertilization and cleavage rates on day 3 between 6.0 and 7.0% CO2 (72.3% vs 67.1%, p = 0.169 and 96.6% vs 96.3%, p = 0.897, respectively). Blastulation rate on day 5/2PN was comparable between 6.0 and 7.0% CO2 (68.1% vs 64.2%, p = 0.409). Although usable blastocyst rate was not different (54.3% vs 55.3%, p = 0.922), total euploidy rates differed significantly (58.7% vs 42.8%, p = 0.016) between 6.0% and 7.0% CO2, respectively. The mean blastocyst mtDNA content was significantly lower in 6.0% CO2 (30.4 ± 9.1 vs 32.9 ± 10.3, p = 0.037).
Conclusion
Blastocyst development is not affected when embryos are cultured in vitro at 6.0% or 7.0% CO2, while euploidy rates are significantly decreased at a higher CO2 concentration, therefore at a lower pHe.


Similar content being viewed by others
References
Swain JE, Carrell D, Cobo A, Meseguer M, Rubio C, Smith GD. Optimizing the culture environment and embryo manipulation to help maintain embryo developmental potential. Fertil Steril. 2016;105(3):571–87. https://doi.org/10.1016/j.fertnstert.2016.01.035 Erratum in: Fertil Steril. 2016 May;105(5):1377.
Gatimel N, Moreau J, Parinaud J, Léandri RD. Need for choosing the ideal pH value for IVF culture media. J Assist Reprod Genet. 2020;37(5):1019–28. https://doi.org/10.1007/s10815-020-01726-5.
Swain JE. Is there an optimal pH for culture media used in clinical IVF? Human Reprod Update. 2012;18(3):333–9. https://doi.org/10.1093/humupd/dmr053.
Swain JE. Optimizing the culture environment in the IVF laboratory: impact of pH and buffer capacity on gamete and embryo quality. Reprod Biomed Online. 2010;21(1):6–16. https://doi.org/10.1016/j.rbmo.2010.03.012.
Koustas G, Sjoblom C. Epigenetic consequences of pH stress in mouse embryos. Hum Reprod. 2011;26:i78. https://doi.org/10.1093/humrep/26.s1.51.
Hentemann M, Mousavi K, Bertheussen K. Differential pH in embryo culture. Fertil Steril. 2011;95(4):1291–4. https://doi.org/10.1016/j.fertnstert.2010.10.018.
Edwards LJ, Williams DA, Gardner DK. Intracellular pH of the preimplantation mouse embryo: effects of extracellular pH and weak acids. Mol Reprod Dev. 1998;50(4):434–42. https://doi.org/10.1002/(SICI)1098-2795(199808)50:4%3c434::AID-MRD7%3e3.0.CO;2-J.
Regula CS, Pfeiffer JR, Berlin RD. Microtubule assembly and disassembly at alkaline pH. J Cell Biol. 1981;89(1):45–53. https://doi.org/10.1083/jcb.89.1.45.
Squirrell JM, Lane M, Bavister BD. Altering intracellular pH disrupts development and cellular organization in preimplantation hamster embryos. Biol Reprod. 2001;64(6):1845–54. https://doi.org/10.1095/biolreprod64.6.1845.
Vázquez-Diez C, FitzHarris G. Causes and consequences of chromosome segregation error in preimplantation embryos. Reproduction. 2018;155(1):R63–76. https://doi.org/10.1530/REP-17-0569.
Summers MC, Biggers JD. Chemically defined media and the culture of mammalian preimplantation embryos: historical perspective and current issues. Hum Reprod Update. 2003;9(6):557–82. https://doi.org/10.1093/humupd/dmg039.
Quinn P, Cooke S. Equivalency of culture media for human in vitro fertilization formulated to have the same pH under an atmosphere containing 5% or 6% carbon dioxide. Fertil Steril. 2004;81(6):1502–6. https://doi.org/10.1016/j.fertnstert.2004.02.093.
Consensus Group C. ‘There is only one thing that is truly important in an IVF laboratory: everything’ Cairo consensus guidelines on IVF culture conditions. Reprod Biomed Online. 2020;40(1):33–60. https://doi.org/10.1016/j.rbmo.2019.10.003.
Wales RG, Quinn P, Murdoch RN. The fixation of carbon dioxide by the eight-cell mouse embryo. J Reprod Fertil. 1969;20(3):541–3. https://doi.org/10.1530/jrf.0.0200541.
Graves CN, Biggers JD. Carbon dioxide fixation by mouse embryos prior to implantation. Science. 1970;167(3924):1506–8. https://doi.org/10.1126/science.167.3924.1506.
Gianaroli L, Plachot M, van Kooij R, Al-Hasani S, Dawson K, DeVos A, Magli MC, Mandelbaum J, Selva J, van Inzen W. Committee of the Special Interest Group on Embryology, ESHRE guidelines for good practice in IVF laboratories. Human Reprod. 2015;15(10):2241–6. https://doi.org/10.1093/humrep/15.10.2241.
Practice Committee of American Society for Reproductive Medicine; Practice Committee of Society for Assisted Reproductive Technology. Revised guidelines for human embryology and andrology laboratories. Fertil Steril. 2008;90(5 Suppl):S45–59. https://doi.org/10.1016/j.fertnstert.2008.08.099.
Gruber I, Klein M. Embryo culture media for human IVF: which possibilities exist?. J Turk Ger Gynecol Assoc. 2011;12(2):110–117. Published 2011 Jun 1. https://doi.org/10.5152/jtgga.2011.25.
Van Blerkom J. Mitochondrial function in the human oocyte and embryo and their role in developmental competence. Mitochondrion. 2011;11(5):797–813. https://doi.org/10.1016/j.mito.2010.09.012.
Sighinolfi G, Grisendi V, La Marca A. How to personalize ovarian stimulation in clinical practice. J Turk German Gynecol Assoc. 2017;18(3):148–53. https://doi.org/10.4274/jtgga.2017.0058.
Gardner DK, Schoolcraft WB. 1999. In vitro culture of human blastocyst. In: Jansen R, Mortimer D, editors. Towards reproductive certainty: fertility and genetics beyond 1999. Cornforth: Parthenon Publishing; 1999. p. 378–88.
Katayama KP, Stehlik J, Kuwayama M, Kato O, Stehlik E. High survival rate of vitrified human oocytes results in clinical pregnancy. Fertil Steril. 2003;80(1):223–4. https://doi.org/10.1016/s0015-0282(03)00551-x.
Phillips NR, Sprouse ML, Roby RK. Simultaneous quantification of mitochondrial DNA copy number and deletion ratio: a multiplex real-time PCR assay. Sci Rep. 2014;4:3887. https://doi.org/10.1038/srep03887.
Gardner DK, Kelley RL. Impact of the IVF laboratory environment on human preimplantation embryo phenotype. J Dev Orig Health Dis. 2017;8(4):418–35. https://doi.org/10.1017/S2040174417000368.
Swain JE. Optimal human embryo culture. Semin Reprod Med. 2015;33(2):103–17. https://doi.org/10.1055/s-0035-1546423.
Wale PL, Gardner DK. The effects of chemical and physical factors on mammalian embryo culture and their importance for the practice of assisted human reproduction. Hum Reprod Update. 2016;22(1):2–22. https://doi.org/10.1093/humupd/dmv034.
Swearman H, Koustas G, Knight E, Liperis G, Grupen C, Sjoblom C. pH: the silent variable significantly impacting meiotic spindle assembly in mouse oocytes. Reprod Biomed Online. 2018;37(3):279–90. https://doi.org/10.1016/j.rbmo.2018.06.022.
Ng KYB, Mingels R, Morgan H, Macklon N, Cheong Y. In vivo oxygen, temperature and pH dynamics in the female reproductive tract and their importance in human conception: a systematic review. Hum Reprod Update. 2018;24(1):15–34. https://doi.org/10.1093/humupd/dmx028.
Swain JE. Controversies in ART: can the IVF laboratory influence preimplantation embryo aneuploidy? Reprod Biomed Online. 2019;39(4):599–607. https://doi.org/10.1016/j.rbmo.2019.06.009.
Dale B, Menezo Y, Cohen J, DiMatteo L, Wilding M. Intracellular pH regulation in the human oocyte. Hum Reprod. 1998;13(4):964–70. https://doi.org/10.1093/humrep/13.4.964.
Barr KJ, Garrill A, Jones DH, Orlowski J, Kidder GM. Contributions of Na+/H+ exchanger isoforms to preimplantation development of the mouse. Mol Reprod Dev. 1998;50(2):146–53. https://doi.org/10.1002/(SICI)1098-2795(199806)50:2%3c146::AID-MRD4%3e3.0.CO;2-K.
Diaz de Pool JDN, Van Den Berg SAA, Pilgram GSK, Ballieux BEPB, Van Der Westerlaken LAJ. Validation of the blood gas analyzer for pH measurements in IVF culture medium: prevent suboptimal culture conditions. PLoS One. 2018;13(11):e0206707. https://doi.org/10.1371/journal.pone.0206707.
Swain JE, Wilding M. Practical pH for the IVF laboratory. J Reprod Stem Cell Biotechnol. 2012;3(2):62–76. https://doi.org/10.1177/205891581200300205.
Bavister BD, Squirrell JM. Mitochondrial distribution and function in oocytes and early embryos. Hum Reprod. 2000;15:189–98. https://doi.org/10.1093/humrep/15.suppl_2.189.
Fragouli E, Spath K, Alfarawati S, et al. Altered levels of mitochondrial DNA are associated with female age, aneuploidy, and provide an independent measure of embryonic implantation potential. PLoS Genet. 2015;11(6):e1005241. https://doi.org/10.1371/journal.pgen.1005241.
Fragouli E, McCaffrey C, Ravichandran K, et al. Clinical implications of mitochondrial DNA quantification on pregnancy outcomes: a blinded prospective non-selection study. Hum Reprod. 2017;32:2340–7. https://doi.org/10.1093/humrep/dex292.
Scott RT, Sun L, Zhan Y, et al. Mitochondrial DNA content is not predictive of reproductive competence in euploid blastocysts. Reprod Biomed Online. 2020;41:183–90.
El-Damen A, Elkhatib I, Bayram A, Arnanz A, Abdala A, Samir S, Lawrenz B, De Munck N, Fatemi HM. Does blastocyst mitochondrial DNA content affect miscarriage rate in patients undergoing single euploid frozen embryo transfer? J Assist Reprod Genet. 2021. https://doi.org/10.1007/s10815-020-02050-8.
Tarahomi M, de Melker AA, van Wely M, Hamer G, Repping S, Mastenbroek S. pH stability of human preimplantation embryo culture media: effects of culture and batches. Reprod Biomed Online. 2018;37(4):409–14. https://doi.org/10.1016/j.rbmo.2018.08.011.
Acknowledgements
We would like to thank Victor Lozoya García for his help and support with statistical evaluation and interpretation.
Author information
Authors and Affiliations
Contributions
AAb, ND, HF: conception and design of the study; AAb, ND, IE, AA, AD, AB, LM, BL, HF: oocyte retrieval; ND, IE, AA, AD, AB, AAb: IVF and ICSI procedure and embryo evaluations; ND, IE, AA, AD, AB, AAb: blastocyst biopsy, tubing and freezing; AAb, NG: construction of the database and data interpretation; AAb: drafting the manuscript; ND, IE, AA, AD, AB, LM, BL, HF: critical review and final approval of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Abdala, A., Elkhatib, I., Bayram, A. et al. Different CO2 settings (6.0% vs 7.0%) do have an impact on extracellular pH of culture medium (pHe) and euploidy rates rather than on blastocyst development: a sibling oocyte study. J Assist Reprod Genet 38, 2915–2923 (2021). https://doi.org/10.1007/s10815-021-02303-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-021-02303-0