Abstract
Purpose
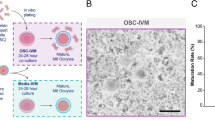
Oocyte competence is critical in success of assisted reproduction. Metabolic signaling between oocyte and cumulus cells within the cumulus-oocyte complex procure oocyte development. This study evaluated the relationship between respirometric activity of cumulus cells and maturity of corresponding oocytes.
Methods
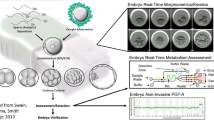
In prospective cohort study, 20 women of age 28–42 undergoing IVF procedure were involved. To evaluate oocyte maturity, the cumulus cells from individual oocytes were assessed flow cytometrically by double labeling of cells with mitochondria specific dyes. The respirometric stress analysis using ATPase inhibitor oligomycin was applied to assess mitochondria metabolic abnormalities.
Results
The cumulus cells from each of 327 oocytes were analyzed. The respirometric index of cumulus cells (O′R) strongly correlates with maternal ovarian reserve, showing to be higher in patients with higher AMH (p < 0.0017). Cumulus cells from immature oocytes had severe mitochondria deficiency, i.e., low O′R, than those from mature oocytes (p < 0.02). No significant difference in respirometric capacity was found between cumulus cells associated with good vs poor-quality embryos.
Conclusions
The oocyte maturity is potentially related to the mitochondria activity of cumulus cells.






Similar content being viewed by others
References
Kovalevsky G, Patrizio P. High rates of embryo wastage with use of assisted reproductive technology: a look at the trends between 1995 and 2001 in the United States. Fertil Steril. 2005;84(2):325–30. https://doi.org/10.1016/j.fertnstert.2005.04.020.
te Velde ER, Pearson PL. The variability of female reproductive ageing. Hum Reprod Update. 2002;8(2):141–54.
Wu LL, Dunning KR, Yang X, Russell DL, Lane M, Norman RJ, et al. High-fat diet causes lipotoxicity responses in cumulus-oocyte complexes and decreased fertilization rates. Endocrinology. 2010;151(11):5438–45. https://doi.org/10.1210/en.2010-0551.
Colton SA, Humpherson PG, Leese HJ, Downs SM. Physiological changes in oocyte-cumulus cell complexes from diabetic mice that potentially influence meiotic regulation. Biol Reprod. 2003;69(3):761–70. https://doi.org/10.1095/biolreprod.102.013649.
Sanchez T, Seidler EA, Gardner DK, Needleman D, Sakkas D. Will noninvasive methods surpass invasive for assessing gametes and embryos? Fertil Steril. 2017;108(5):730–7. https://doi.org/10.1016/j.fertnstert.2017.10.004.
Dumesic DA, Meldrum DR, Katz-Jaffe MG, Krisher RL, Schoolcraft WB. Oocyte environment: follicular fluid and cumulus cells are critical for oocyte health. Fertil Steril. 2015;103(2):303–16. https://doi.org/10.1016/j.fertnstert.2014.11.015.
Silvestre F, Boni R, Fissore RA, Tosti E. Ca2+ signaling during maturation of cumulus-oocyte complex in mammals. Mol Reprod Dev. 2011;78(10–11):744–56. https://doi.org/10.1002/mrd.21332.
Su YQ, Sugiura K, Wigglesworth K, O'Brien MJ, Affourtit JP, Pangas SA, et al. Oocyte regulation of metabolic cooperativity between mouse cumulus cells and oocytes: BMP15 and GDF9 control cholesterol biosynthesis in cumulus cells. Development. 2008;135(1):111–21. https://doi.org/10.1242/dev.009068.
Downs SM, Mastropolo AM. The participation of energy substrates in the control of meiotic maturation in murine oocytes. Dev Biol. 1994;162(1):154–68. https://doi.org/10.1006/dbio.1994.1075.
Behrman HR, Preston SL, Pellicer A, Parmer TG. Oocyte maturation is regulated by modulation of the action of FSH in cumulus cells. Prog Clin Biol Res. 1988;267:115–35.
Lolicato F, Brouwers JF, de Lest CH, Wubbolts R, Aardema H, Priore P, et al. The cumulus cell layer protects the bovine maturing oocyte against fatty acid-induced lipotoxicity. Biol Reprod. 2015;92(1):16. https://doi.org/10.1095/biolreprod.114.120634.
Sugiura K, Su YQ, Diaz FJ, Pangas SA, Sharma S, Wigglesworth K, et al. Oocyte-derived BMP15 and FGFs cooperate to promote glycolysis in cumulus cells. Development. 2007;134(14):2593–603. https://doi.org/10.1242/dev.006882.
Sanchez-Lazo L, Brisard D, Elis S, Maillard V, Uzbekov R, Labas V, et al. Fatty acid synthesis and oxidation in cumulus cells support oocyte maturation in bovine. Mol Endocrinol. 2014;28(9):1502–21. https://doi.org/10.1210/me.2014-1049.
Miao YL, Liu XY, Qiao TW, Miao DQ, Luo MJ, Tan JH. Cumulus cells accelerate aging of mouse oocytes. Biol Reprod. 2005;73(5):1025–31. https://doi.org/10.1095/biolreprod.105.043703.
Ikeda S, Imai H, Yamada M. Apoptosis in cumulus cells during in vitro maturation of bovine cumulus-enclosed oocytes. Reproduction. 2003;125(3):369–76.
Lee KS, Joo BS, Na YJ, Yoon MS, Choi OH, Kim WW. Cumulus cells apoptosis as an indicator to predict the quality of oocytes and the outcome of IVF-ET. J Assist Reprod Genet. 2001;18(9):490–8.
Dumesic DA, Guedikian AA, Madrigal VK, Phan JD, Hill DL, Alvarez JP, et al. Cumulus cell mitochondrial resistance to stress in vitro predicts oocyte development during assisted reproduction. J Clin Endocrinol Metab. 2016;101(5):2235–45. https://doi.org/10.1210/jc.2016-1464.
Bentov Y, Yavorska T, Esfandiari N, Jurisicova A, Casper RF. The contribution of mitochondrial function to reproductive aging. J Assist Reprod Genet. 2011;28(9):773–83. https://doi.org/10.1007/s10815-011-9588-7.
Wu LL, Russell DL, Norman RJ, Robker RL. Endoplasmic reticulum (ER) stress in cumulus-oocyte complexes impairs pentraxin-3 secretion, mitochondrial membrane potential (DeltaPsi m), and embryo development. Mol Endocrinol. 2012;26(4):562–73. https://doi.org/10.1210/me.2011-1362.
Schatten H, Sun QY, Prather R. The impact of mitochondrial function/dysfunction on IVF and new treatment possibilities for infertility. Reprod Biol Endocrinol : RB&E. 2014;12:111. https://doi.org/10.1186/1477-7827-12-111.
Chappel S. The role of mitochondria from mature oocyte to viable blastocyst. Obstet Gynecol Int. 2013;2013:183024–10. https://doi.org/10.1155/2013/183024.
Galluzzi L, Kepp O, Trojel-Hansen C, Kroemer G. Mitochondrial control of cellular life, stress, and death. Circ Res. 2012;111(9):1198–207. https://doi.org/10.1161/CIRCRESAHA.112.268946.
Goldenthal MJ, Marin-Garcia J. Mitochondrial signaling pathways: a receiver/integrator organelle. Mol Cell Biochem. 2004;262(1–2):1–16.
Gardner DK, Lane M, Stevens J, Schoolcraft WB. Noninvasive assessment of human embryo nutrient consumption as a measure of developmental potential. Fertil Steril. 2001;76(6):1175–80.
Ramakrishna R, Edwards JS, McCulloch A, Palsson BO. Flux-balance analysis of mitochondrial energy metabolism: consequences of systemic stoichiometric constraints. Am J Physiol Regul Integr Comp Physiol. 2001;280(3):R695–704.
Dalton CM, Szabadkai G, Carroll J. Measurement of ATP in single oocytes: impact of maturation and cumulus cells on levels and consumption. J Cell Physiol. 2014;229(3):353–61. https://doi.org/10.1002/jcp.24457.
Collins Y, Chouchani ET, James AM, Menger KE, Cocheme HM, Murphy MP. Mitochondrial redox signalling at a glance. J Cell Sci. 2012;125(Pt 4):801–6. https://doi.org/10.1242/jcs.098475.
Lenaz G. Role of mitochondria in oxidative stress and ageing. Biochim Biophys Acta. 1998;1366(1–2):53–67.
Bing YZ, Hirao Y, Iga K, Che LM, Takenouchi N, Kuwayama M, et al. In vitro maturation and glutathione synthesis of porcine oocytes in the presence or absence of cysteamine under different oxygen tensions: role of cumulus cells. Reprod Fertil Dev. 2002;14(3–4):125–31.
Tatemoto H, Sakurai N, Muto N. Protection of porcine oocytes against apoptotic cell death caused by oxidative stress during in vitro maturation: role of cumulus cells. Biol Reprod. 2000;63(3):805–10.
Kaya A, Gerashchenko MV, Seim I, Labarre J, Toledano MB, Gladyshev VN. Adaptive aneuploidy protects against thiol peroxidase deficiency by increasing respiration via key mitochondrial proteins. Proc Natl Acad Sci U S A. 2015;112(34):10685–90. https://doi.org/10.1073/pnas.1505315112.
Assou S, Haouzi D, Mahmoud K, Aouacheria A, Guillemin Y, Pantesco V, et al. A non-invasive test for assessing embryo potential by gene expression profiles of human cumulus cells: a proof of concept study. Mol Hum Reprod. 2008;14(12):711–9. https://doi.org/10.1093/molehr/gan067.
Setterfield K, Williams AJ, Donald J, Thorburn DR, Kirby DM, Trounce I, et al. Flow cytometry in the study of mitochondrial respiratory chain disorders. Mitochondrion. 2002;1(5):437–45.
Matteucci E, Manzini S, Ghimenti M, Consani C, Giampietro O. Rapid flow cytometric method for measuring mitochondrial membrane potential, respiratory burst activity, and intracellular thiols of human blood leukocytes. Open Chem Biom Methods. 2009;2:65–8.
Rottenberg H, Wu S. Quantitative assay by flow cytometry of the mitochondrial membrane potential in intact cells. Biochim Biophys Acta. 1998;1404(3):393–404.
Gregori G, Denis M, Lefevre D, Beker B. A flow cytometric approach to assess phytoplankton respiration. Methods Cell Sci. 2002;24(1–3):99–106.
Panov A, Orynbayeva Z. Bioenergetic and antiapoptotic properties of mitochondria from cultured human prostate cancer cell lines PC-3, DU145 and LNCaP. PLoS One. 2013;8(8):e72078. https://doi.org/10.1371/journal.pone.0072078.
Nicholls DG, Darley-Usmar VM, Wu M, Jensen PB, Rogers GW, Ferrick DA. Bioenergetic profile experiment using C2C12 myoblast cells. J Vis Exp : JoVE. 2010(46). doi:https://doi.org/10.3791/2511.
Nicholls DG. Mitochondrial membrane potential and aging. Aging Cell. 2004;3(1):35–40.
Barbakadze L, Kristesashvili J, Khonelidze N, Tsagareishvili G. The correlations of anti-mullerian hormone, follicle-stimulating hormone and antral follicle count in different age groups of infertile women. Int J Fertil Steril. 2015;8(4):393–8.
Xie HL, Wang YB, Jiao GZ, Kong DL, Li Q, Li H, et al. Effects of glucose metabolism during in vitro maturation on cytoplasmic maturation of mouse oocytes. Sci Rep. 2016;6:20764. https://doi.org/10.1038/srep20764.
Reynier P, May-Panloup P, Chretien MF, Morgan CJ, Jean M, Savagner F, et al. Mitochondrial DNA content affects the fertilizability of human oocytes. Mol Hum Reprod. 2001;7(5):425–9.
Zeng HT, Ren Z, Yeung WS, Shu YM, Xu YW, Zhuang GL, et al. Low mitochondrial DNA and ATP contents contribute to the absence of birefringent spindle imaged with PolScope in in vitro matured human oocytes. Hum Reprod. 2007;22(6):1681–6. https://doi.org/10.1093/humrep/dem070.
May-Panloup P, Boucret L, Chao de la Barca JM, Desquiret-Dumas V, Ferre-L’Hotellier V, Moriniere C, et al. Ovarian ageing: the role of mitochondria in oocytes and follicles. Hum Reprod Update. 2016;22(6):725–43. https://doi.org/10.1093/humupd/dmw028.
Hsu AL, Townsend PM, Oehninger S, Castora FJ. Endometriosis may be associated with mitochondrial dysfunction in cumulus cells from subjects undergoing in vitro fertilization-intracytoplasmic sperm injection, as reflected by decreased adenosine triphosphate production. Fertil Steril. 2015;103(2):347–52 e1. https://doi.org/10.1016/j.fertnstert.2014.11.002.
Pacella-Ince L, Zander-Fox DL, Lan M. Mitochondrial SIRT3 and its target glutamate dehydrogenase are altered in follicular cells of women with reduced ovarian reserve or advanced maternal age. Hum Reprod. 2014;29(7):1490–9. https://doi.org/10.1093/humrep/deu071.
Van Blerkom J, Davis P. Mitochondrial signaling and fertilization. Mol Hum Reprod. 2007;13(11):759–70. https://doi.org/10.1093/molehr/gam068.
Panov A, Orynbayeva Z. Determination of mitochondrial metabolic phenotype through investigation of the intrinsic inhibition of succinate dehydrogenase. Anal Biochem. 2017;552:30–7. https://doi.org/10.1016/j.ab.2017.10.010.
Starkov AA. The role of mitochondria in reactive oxygen species metabolism and signaling. Ann N Y Acad Sci. 2008;1147:37–52. https://doi.org/10.1196/annals.1427.015.
Pesta D, Gnaiger E. High-resolution respirometry: OXPHOS protocols for human cells and permeabilized fibers from small biopsies of human muscle. Methods Mol Biol. 2012;810:25–58. https://doi.org/10.1007/978-1-61779-382-0_3.
Yuan YQ, Van Soom A, Leroy JL, Dewulf J, Van Zeveren A, de Kruif A, et al. Apoptosis in cumulus cells, but not in oocytes, may influence bovine embryonic developmental competence. Theriogenology. 2005;63(8):2147–63. https://doi.org/10.1016/j.theriogenology.2004.09.054.
Acknowledgments
The authors are thankful to Saniya Ossikbayeva for her excellent technical assistance. The support of EMD Serono, Inc. to the Main Line Fertility Center is appreciated. The sponsor has no involvement in experimental design, experimental performance, data analysis, and manuscript generation.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
Michael Glassner is a founding partner and the medical director at the Main Line Fertility Center. Other authors have no conflicts of interest to declare.
Rights and permissions
About this article
Cite this article
Anderson, S.H., Glassner, M.J., Melnikov, A. et al. Respirometric reserve capacity of cumulus cell mitochondria correlates with oocyte maturity. J Assist Reprod Genet 35, 1821–1830 (2018). https://doi.org/10.1007/s10815-018-1271-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-018-1271-9