Abstract
Individuals with autism spectrum disorders (ASD) are at higher risks of developing chronic oral health conditions. This trial compared the efficacy of two tooth-brushing educational interventions on the oral hygiene status {Simplified Oral Hygiene Index (OHI-S)} among 7–15-year-old students with ASD in Tehran. Four schools were divided to intervention (video modeling) and comparison (social story) school groups. The OHI-S of 137 participants had been evaluated at baseline and 133 were analyzed finally after one month. Baseline characteristics were similar between both groups. OHI-S improvement was significantly higher in intervention group. We concluded that tooth-brushing educational intervention using video modeling based on modern technologies would improve oral hygiene status more than traditional social stories (standard education) in individuals with ASD. Trial registration number: IRCT20200208046413N1, Registration date: 2020–07-05.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Autism spectrum disorder (ASD) is one of the most severe childhood neuropsychiatric conditions. ASD is characterized by impairment in social interactions with repetitive behaviors and a restricted range of interests and functions (Happé, 2011). Individuals with ASD are at a higher risk of developing chronic non-communicable oral health conditions due to factors like poor dietary preferences, behaviors, and specific aversions (Feucht & Ogata, 2010; Jaber, 2011). The increasing prevalence of ASD has raised global interest in oral health concerns in these individuals. In addition, this coincides with one of the global oral health goals to promote the oral health of this population (Beaglehole, 2003; Gandhi & Klein, 2014).
Toothbrushing has an essential role in oral health maintenance and is one of the basic self-care skills. However, evidence suggests that children with ASD have difficulties in their daily toothbrushing practice (Du, Yiu, King, and disorders, 2019). Preventive educational interventions with emphasis on teaching an easy, proper and effective toothbrushing technique may be desirable to improve the oral health, particularly in young individuals with ASD (Piraneh et al., 2022). Accordingly, effective toothbrushing training can improve these children’s self-care and reduce their parents’ burdens and exhaustion (Zhou et al., 2020).
Special educational methods and intervention approaches are required to improve the toothbrushing practice in individuals with ASD. The most common method is visual pedagogy, which benefits from these children’s ability to respond better to pictures and images rather than conceptual words. It appears to be an effective training method for children with autism both at home and in school (Bäckman & Pilebro, 1999). Visual pedagogy has also been used to develop several types of educational techniques and instruments such as pictured books, social stories, video modeling, picture containing apps, etc. Social stories are a common strategy for children with ASD. These stories are short by design and rely on a ratio of descriptive, perspective and/or affirmative sentences in addition to visual cues (Gandhi & Klein, 2014; Styles, 2011). Video uses technology to deliver modeling interventions efficiently and provides the learners with accurate and consistent exemplars of the target behavior being performed (Hong et al., 2016). Furthermore, Peer Mediated Interventions (PMI) has also been identified as a versatile and potentially effective intervention approach to teach a variety of skills to individuals with ASD (Watkins et al., 2015). Parent-mediated interventions are also increasingly used to target skill deficits in children with autism (Shalev et al., 2020).
To conduct an effective intervention, there is a need for a conceptual framework that guides the construction of the intervention and its evaluation. The PRECEDE-PROCEED model can be used as a framework to design and evaluate an oral health promotion effort. In this framework, health behavior is regarded as being influenced by both individual and environmental factors; hence, it has two distinct parts. The first part is an “educational diagnosis” – PRECEDE, an acronym for Predisposing, Reinforcing and Enabling Constructs in Educational Diagnosis and Evaluation. The second part is an “ecological diagnosis” – PROCEED, an acronym for Policy, Regulatory, and Organizational Constructs in Educational and Environmental Development. The PRECEDE component allows researchers to work backward from the ultimate goal of the research (distal outcomes) to create a blueprint to instruct the formation of the intervention or strategy. The PROCEED component may lay out the evaluation, including pilot study and efficacy study methodologies (Crosby & Noar, 2011).
Due to the importance of oral health in autistic individuals, increasing prevalence of ASD in the world, and limited studies investigating oral health education and promotion in individuals with autism, it is necessary to conduct a study to evaluate the effect of oral hygiene educational interventions on the oral hygiene status of children with ASD. Therefore, the present study was conducted to evaluate and compare the effect of two different toothbrushing educational interventions (social story based toothbrushing education versus video-modeling based toothbrushing training) on the oral hygiene status of primary school students with ASD aged 7–15 years old in Tehran, Iran using the Simplified Oral Hygiene Index (OHI-S) (Greene & Vermillion, 1964). The framework of the trial program was designed based on the branches of the PRECEDE–PROCEED planning model (Crosby & Noar, 2011; Saied-Moallemi, 2010).
Methods
Trial Design
A quasi-randomized (male students aged 7–15 years old with autism spectrum disorder studying in four primary schools in intervention and comparison groups with simple randomization [1:1]) two-arm, non-blind, parallel, controlled trial was conducted in Iran.
Participants
Eligible participants were male students with ASD aged 7–15 years old in the first to sixth grades of governmental special primary schools in Tehran, Iran. The inclusion criteria were parents’ consent for their child to participate in the study, age 7–15 years, ASD level 1 or 2, and access to the Internet and WhatsApp social network. The two exclusion criteria were the presence of other physical or developmental disabilities and inability to cooperate. All the students of these four schools including 161 students in 38 classrooms were invited. The parents of 147 students consented to their children’s participation in the study by signing informed consent forms after obtaining information about the purpose and process of the study (response rate: 91.3%). According to the inclusion criteria, 10 students who were diagnosed as ASD level 3 were excluded.
Study Settings
The study took place at the four public primary special schools that provide special training and care exclusively for male students with ASD in Tehran, Iran, from November 2019 to March 2020. (Besharat Special School, Imam Jafar Sadegh Special School, Payambar-e-Azam Special School, and Peyk-e-Honar Special School).
Randomization
Each school was considered as a randomization unit. As the number of schools was limited, the present study was conducted as a quasi-randomized controlled trial and these four schools were randomized to two equal arms of parallel school groups. Therefore, for simple randomization, each school’s name was written on a piece of paper and concealed in an envelope by a third person. These four schools were randomly allocated to the intervention and comparison groups by drawing envelopes randomly.
Sample Size
The sample size was calculated with the sample size calculation formula for clinical trials using mean and standard deviation (OHI-S mean difference = 0.6) (Charan & Biswas, 2013). Assuming that 20% of the students could be lost to follow-up, 60 students were needed. Considering a design effect of 1.5, at least 90 students were required.
Outcomes
The outcome variable was oral hygiene improvement measured as a decrease in the OHI-S score. The OHI-S consists of two parts, including the Debris Index (DI) and Calculus Index (CI). Debris is the soft foreign matter loosely attached to the teeth. It consists of mucin, bacteria and food, and varies in color from greyish white to green or orange, and calculus is defined as a deposit of inorganic salts composed primarily of calcium carbonate and phosphate mixed with food debris, bacteria and desquamated epithelial cells (Greene & Vermillion, 1964). Six tooth surfaces (3, 8, 14, 19, 24, and 30 in the permanent dentition or A, E, F, K, O, and P in the primary dentition) are scored on a scale of 0 to 3. The debris scores are summed and divided by the number of examined teeth for each subject to calculate DI. The same process is used to calculate CI. The sum of DI and CI equals the OHI-S (Kolawole & Folayan, 2019).
A valid and reliable instrument was designed and developed by an expert panel to measure the parents’ oral health knowledge and attitude as well as the student’s oral health behaviors. This instrument had acceptable content validity index (CVI) (≥ 0.83) and content validity ratio (CVR) (≥ 0.75) values (Polit & Beck, 2004). Subsequently, the face validity of the questionnaire was found to be acceptable according to twelve parents who answered questions about the clarity and comprehensibility of the questionnaire in a pilot study. The internal reliability was assessed by Cronbach’s alpha coefficient, which was 0.96. The intra-class correlation coefficient (ICC) was above 0.70 in test–retest analysis. They both had acceptable limits (Taber, 2018).
The questionnaire consisted of four parts. The first part was about demographic and basic characteristics of the students including age, education level of parents, and the household economic status. The second part used four items to evaluate the oral health behavior of autistic children (including sugary snack consumption, toothbrushing frequency and routines, and frequency of fluoridated toothpaste use). The third part contained eight items on the parents’ oral health knowledge, and the last part included six items on the parents’ attitude towards oral health.
The parents’ education level was assessed by their last academic degree via a multiple-choice question ordinated in six education levels including: 1-illiterate, 2-unfinished high school education, 3-high school diploma, 4-associated degree, 5-bachelor’s degree, and 6-master’s degree or higher. Then, the levels were dichotomized according to statistical distribution into two groups of 1-associate degree or less and 2-higher than associate degree. The household economic status was assessed according to relative poverty in urban areas of Iran, which was estimated at 360 USD at the time of the study. A monthly income of below 360 USD was considered as low-income and above 360 USD was considered as high income.
The parents’ oral health knowledge was assessed with eight true/false questions. A correct answer to each question received a score of 1 and a wrong answer received a score of 0. Accordingly, the sum score of these eight responses indicated the parents’ overall knowledge score that ranged from 0 to 8. Finally, the overall score was converted to the overall knowledge percentage for easier understanding. The parents’ attitude towards oral health was assessed using six questions on a five-point Likert scale (completely agree = 1, almost agree = 2, no idea = 3, almost disagree = 4, and completely disagree = 5). The answers were coded and aligned from the lowest proper value to the highest and scored from 1 to 5 respectively. Then, the sum score of these six responses indicated the parents’ overall attitude score, which ranged from 6 to 30. In addition, the overall score was converted to the overall attitude percentage.
Pilot Study and Calibration
Prior to the main study, a pilot study was conducted in a private charity educational center for autistic children in Tehran. Eleven children with ASD participated in the pilot study. For intra-examiner calibration, the examiner—a general dentist-examined 10 children and recorded the OHI-S. A second examination was conducted after 30 min. The intra-class correlation coefficient (ICC) was calculated for the debris index (DI), calculus index (CI), and OHI-S (ICC = 1). The inter-examiner agreement was assessed between the examiner and an oral public health specialist. An ICC of 1 was calculated for the OHI-S (ICC for DI and CI = 1).
Baseline
A week before oral examination, a social story that contained pictures of the examiner and examination steps was given to the parents with an information sheet containing necessary instructions regarding storytelling and showing the numbered pictures in the mentioned order at least three times a day during the week. Subsequently, the questionnaire was completed by one of the parents. A psychologist who was evaluating the students in the study as to the level of severity assessed the severity of autism (ASD level 1: mild ASD, level 2: moderate ASD, and level 3: severe ASD) according to the Diagnostic and Statistical Manual of Mental Disorders, 5th Edition (DSM-5) (Association, 2013). On the examination day, the students were visited in a classroom known as the “health room” one by one with their teachers. The students were asked to sit on a bench. The examination was carried out under natural light using an intra-oral examination mirror and the OHI-S was recorded. In addition, the cooperation level of the students during examination was reported using the Frankle scale (Nilchian et al., 2017). Basic characteristics were similar between the two groups. A soft toothbrush and tasteless fluoridated toothpaste were given to each student as a reward at the end of the oral examination.
Interventions
This study was designed based on the modified PRECEDE-PROCEED oral health promotion model (Saied-Moallemi, 2010). The different parts of the model in the present study were as follows: 1-Fluoride therapy is routinely provided for grades 1 to 6 in all schools twice a year by the Iranian Ministry of Health as a national program (considered as an environmental factor), 2-The education level of the parents and the household income were enabling factors, 3-The child’s level of ASD was considered a predisposing factor, 4-The parents’ oral health knowledge and attitude as well as their supervision over their children’s toothbrushing practice were considered as reinforcing factors (Fig. 1).
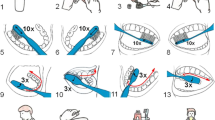
Based on the experts’ opinion and the relevant literature that has shown the visual pedagogy approach to be an effective and practical method to educate individuals with ASD (Pilebro & Bäckman, 2005; Smutkeeree et al., 2020), we decided to use this approach to train these students to use the Fones toothbrushing technique. Tailoring the intervention educational package was based on the modern technology and used video modeling. Research has demonstrated oral hygiene improvement after toothbrushing training via video modeling interventions in children with ASD (Popple et al., 102016). The educational package used for comparison (social story) was designed based on the standard routine of education in schools for students with ASD. Social story interventions have been used to improve toothbrushing skills in children with or without autism; however, they have proven more efficient in improving the oral hygiene status in children with autism (Zhou et al., 2020). In the two intervention schools, the parents in the intervention groups were invited to a face-to-face meeting in order to provide information about sugary foods and the effect on tooth surfaces and the oral cavity. The importance of plaque control was discussed and instructions regarding the intervention video were provided as the first step. The parents were taught how their children should brush their teeth through video modeling (Hong et al., 2016). Subsequently, a video that was already prepared was played for them, a 3-min video that presented the Fones brushing technique in 23 smaller stages. The Fones technique was selected because it is easy to learn and apply, especially for the students with ASD and their caregivers (Dias et al., 2010). In the video, a 10-year-old boy presented the stages slowly and a background voice narrated a simple sentence in each stage to instruct the student. The video file was sent to parents via the WhatsApp social network. The parents were asked to play the video every day and practice the stages with their children as much as possible. A poster containing selected photos taken from the above video was given to parents to place on the bathroom wall where their children brushed their teeth to help them remember the stages. Reminder WhatsApp messages were sent to the parents three times a week. In order to prepare a supportive environment, as a PMI for the students, a training session was held for teachers to teach them the Fones brushing technique. The teachers were asked to play the video for the students in the classroom and help the students practice toothbrushing with their classmates in the school environment twice a week. The posters that were given to the parents containing photos from the video were also displayed in the school restrooms where the students brushed their teeth.
In the two comparison schools, the parents in the comparison group were provided with same oral health education as the intervention group in the form of pamphlets instead of the face-to-face meeting. Since printed materials such as pamphlets are frequently used for health education and are effective in changing knowledge, attitudes and behavior for a wide range of health-related issues (Redman, 1997), the study was purposely designed to keep the comparison group’s educational package in a common and traditional style as much as possible. A social story containing photos and sentences of the 23 smaller stages of the Fones toothbrushing technique was given to the parents. The parents were asked to practice with their children every day and use the stages in their children’s toothbrushing routine as much as possible. Thus, both intervention and comparison groups were taught how to brush their teeth using the Fones toothbrushing technique in 23 smaller stages by two different visual pedagogic tools (video modeling in the intervention group and social story in the comparison group). The same poster given to the intervention group was given to the parents of children in the comparison group to install on their bathroom wall as well. Reminder WhatsApp messages were sent three times a week, similar to the intervention group. However, no PMIs were used in the comparison group.
Follow-Up
A follow-up evaluation was done one month after the intervention using the same questionnaire used for baseline evaluation. The questionnaire was completed by the parents. Oral examination of the students was done by the same examiner in order to record secondary OHI-S (Fig. 2).
Blinding
In this study, the children and their parents were aware of the educational group they were allocated to. It was not possible to design and implement a double-blind trial since oral examination by a stranger examiner in the follow-up session could affect the children’s cooperation. The only blind party was the statistician.
Statistical Methods
The collected data were entered into a dataset in the SPSS software version 24 (IBM Corp, Released 2017, Armonk, NY). First, the data were scanned, and false entries were cleared from the dataset. There were no missing values at baseline. The students who did not complete the follow-up oral evaluation were not included in the analysis due to lack of outcome variables. The STATA/SE version 14 (Stata Corp, Releasead 2016, College Station, TX) was used for longitudinal data analysis. Considering the normal distribution of the data, quantitative numerical variables are presented as mean and standard deviation (SD) and categorical variables are reported as number (n) and percentage (%). Each classroom was considered a cluster. Due to the close relationships of the students’ parents in the schools and a high probability of intervention contamination, it was not possible to group different clusters in a particular school. In order to evaluate and compare the effect of intervention and comparison educational packages on outcome measures and to consider the internal effect of the clusters (class rooms), multilevel mixed effect linear regression model was used for quantitative variables and multilevel mixed effect logistic regression model was applied to categorical variables. P-values less than 0.05 were considered significant in all analyses.
Results
At baseline, 137 male students from four schools entered the study. Four schools were randomized into two equal arms of parallel school groups. The two intervention schools had 79 students in 22 classrooms and the two comparison schools had 58 students in 16 classrooms. At the follow-up, 133 students remained in the trial that were included in the final analysis (Fig. 3).
At baseline, the mean age of the students was 11.57 ± 2.29 years (male: 100%). The mean oral hygiene status of the students according to the OHI-S was 1.91 ± 0.51. The mean oral health knowledge and attitude scores of the parents were 86.19 ± 14.64 and 82.79 ± 13.06, respectively. The demographic and baseline characteristics of the students in the intervention and comparison groups are presented in Table 1 [Table 1]. The frequency of the parents’ correct responses to oral health knowledge questions in intervention and comparison groups before and after the intervention is demonstrated [Table 2]. The parents in both groups showed an increasing trend of oral health knowledge in all items except item 2 (Eating sweet food causes tooth decay) and item 5 (It is beneficial to visit a dentist for regular check-ups) in the intervention group, which showed a slight decline of 1.3% in the post intervention assessment.
The mean scores of the parents’ oral health attitude in intervention and comparison groups before and after the intervention are placed in Table 3 [Table 3]. The scores of all of the six items had an increasing trend in both groups in post intervention assessment.
Comparison of the effect of two educational packages on the outcome measures between the two groups at one-month follow-up is presented in Table 4 [Table 4]. The OHI-S was significantly lower in the intervention group compared to the comparison group, indicating a better oral health status (p-value = 0.006). Other measured values including the students’ oral health behavior and parents’ oral health knowledge and attitude were not significantly different between the two groups. However, in both groups, the percentage of the parents’ oral health knowledge and attitude had an increasing trend compared to baseline. As for the items of the students’ oral health behavior, the number of students who “brushed at least once a day”, “used fluoridated toothpaste most of the time”, and “brushed their teeth under supervision or aided” had an increasing trend in both groups. The number of students that “consumed sweet snacks twice a day or less” did not change compared to baseline.
Discussion
The present study was a quasi-randomized controlled trial aimed to evaluate and compare the effect of social story based toothbrushing education versus video-modeling based tooth-brushing training on oral hygiene status of male students aged 7–15 years old with autism spectrum disorder in the governmental special primary schools of Tehran, Iran. The main finding of this study was that the OHI-S decreasing trend was significantly higher in the intervention group versus the comparison group, which could be due to the higher efficacy of video modeling compared to social stories in ASD children. The post-intervention evaluations showed that the eating habits and oral health behavior were not significantly different between the intervention and comparison groups. This study was conducted in two phases, including pre-intervention (baseline) and follow-up (one month post intervention). The present study introduced and compared two child-friendly noninvasive educational packages for teaching toothbrushing skills to children with ASD. Both educational packages improved the oral hygiene status of children with ASD in the intervention and comparison groups and also enhanced the parents’ oral health knowledge and attitude according to the branches of PRECEDE–PROCEED planning model. However, the parents’ oral health knowledge and attitude were similar between the two groups after the intervention. The Fones brushing technique is considered as a basic skill for oral hygiene maintenance in these individuals as it is easy to learn and apply (Dias et al., 2010). Two different visual educational techniques were used in the study groups. One of the techniques was video modeling, which is one of the newest tools of visual pedagogy and employs technological advances (Hong et al., 2016). This technique was used in the intervention group. The other technique was a popular traditional instrument known as the social story, which was used in the comparison group (Styles, 2011). Both of the intervention and comparison groups used a parent-mediated intervention to maximize the children’s learning through increasing their opportunity to practice toothbrushing at home (Brookman-Frazee et al., 2009). The innovation of the study was that a PMI was included in the educational package of the intervention group to provide a supportive environment for the students in the school (Watkins et al., 2015).
In the one-month follow-up, the effect of the educational packages on the outcome measures was compared between the two groups. The percentage of the parents’ oral health knowledge and attitude had a slightly increasing trend compared to the pre-intervention phase in both groups. As for the students’ oral health behavior, the number of students who brushed at least once a day, often used fluoridated toothpaste, and brushed their teeth under supervision or aided also showed an increasing trend in both groups compared to the baseline. However, the number of students that consumed sugary snacks twice a day or less remained unchanged compared to baseline. In this study, the dietary habits and oral health behavior were not significantly different between intervention and comparison groups after the intervention, which could be due to the short time of intervention that was not long enough to cause a behavior change (Asma’a et al., 2013; Ghaffari et al., 2018). In a meta-analysis, the minimum time required to apply interventions with positive effects on oral health behavior in children was three months. (Ghaffari et al., 2018).
In the one-month follow-up, a decreasing trend was observed in the OHI-S in both groups indicating an improvement in the oral health status, which was consistent with previous studies (Dias et al., 2010; Popple et al., 2016; Zhou et al., 2020). The improvement in the overall oral health was probably due to reminder messages sent to both groups, which may have created a higher priority for oral health (Popple et al., 2016). This decreasing trend in the OHI-S was significantly higher in the intervention group versus the comparison group, which might be related to the significantly higher efficacy of teaching the correct brushing method and more effective plaque removal in the video modeling method due to the better interaction of autistic children with technology compared to the traditional method of social story printed on paper. This finding was consistent with the results of a study by Mohammadpour et al. that found video modeling increased self-help skills, including brushing skills, in children with autism at 1-month and 3-month follow-ups (Mohammadpour et al., 2013). Since video modeling uses visual guides, it is an effective strategy for educating people with ASD (Bellini & Akullian, 2007). According to another study, the visual nature of this strategy helps individuals with ASD find the right frame of reference for behavior in this context. Video modeling may help individuals with ASD to overcome problems such as the inability to focus on a stimulus, which affects imitation and random learning (McCoy & Hermansen, 2007). Another theory suggests that video modeling can help compensate for hypersensitivity to stimuli in individuals with ASD by facilitating their attention to stimuli and prominent symptoms (Charlop-Christy et al., 2000). Video modeling may also increase motivation, and it has been shown that it affects some children with ASD inherently (Charlop-Christy & Daneshvar, 2003). It seems that oral health behavior change in children with autism, including the frequency of toothbrushing per day and using fluoridated toothpaste, especially in those who are hypersensitive to taste and those who have certain eating habits, requires a great deal of practice and repetition. However, training aiming at optimizing the child’s toothbrushing skills with the help of parents or caregivers might improve the plaque removal and oral hygiene status and promotes oral health in these children.
Limitations
Unfortunately, because of the onset of covid-19 pandemic and closure of all schools across the country, further follow-ups were postponed and then cancelled due to the biological risks. It was difficult to compare the results with previous studies because of the limited number of oral health related clinical trials in the ASD population. Moreover, previous studies were conducted in different age groups and different countries with various cross-cultural values and living standards, dietary habits, genetic backgrounds, etc.
Strengths
The present study was conducted in Tehran, a multicultural city with a population of about 10 million including individuals and families with different socio-demographic statuses (SES), health beliefs, and racial and ethnic backgrounds (Montazeri et al., 2008). To the best of our knowledge, this is the first study of oral health-related interventions in such a large sample size of children with ASD in the Middle East. Parents of the students with ASD were apprehensive about any kind of clinical examinations on their children. In addition, the overload of responsibilities experienced by parents who have children with ASD contributed to a reluctance to teach a new skill to their child. Parents were more likely to participate in the study when an awareness was created about the potential oral health benefits that the Fones tooth-brushing technique could provide. However, despite these difficulties, we were able to collect an acceptable database for the study. Another strength was the study setting, which included schools that enrolled children with ASD. Schools are the best place for examinations since children are used to this environment. A change of location for dental examination would probably provoke negative behaviors in this group of children (Rekha et al., 2012). In addition, the reminder messages sent via WhatsApp for both groups may have had a supportive role in promoting the consistency of the training (Popple et al., 2016).
Conclusion
A quasi-randomized controlled trial was conducted to evaluate and compare the efficacy of social story based toothbrushing education versus video-modeling based tooth-brushing training in promoting the oral hygiene status of male autistic students aged 7–15 years old in Tehran, Iran. The results indicated a higher improvement in oral hygiene status of the video-modeling group compared to the social story group, which could be due to the higher efficacy of video modeling versus social stories in children with ASD. However, the eating habits and oral health behaviors were similar in both groups after the intervention. The findings of the present study suggest that educational interventions using video modeling based on modern technologies could improve the oral hygiene status of individuals with ASD and might reduce the parents’ financial, social, and emotional burdens of health care. For health specialists, this study demonstrates the limitations and commences a pathway to find the best oral health educational interventions. In the future, there is a need for more clinical trials in the field of oral health with focus on the acquisition of toothbrushing skills in individuals with ASD in different populations.
References
Asma’a, M. S., Badr, S. B., Rashed, M. A. J. I. J., & o. D. (2013). Effectiveness of audiovisual modeling on the behavioral change toward oral and dental care in children with autism. Indian Journal of Dentistry, 4(4), 184–190. https://doi.org/10.1016/j.ijd.2013.02.002
Association, A. P. (2013). Diagnostic and statistical manual of mental disorders (DSM-5®): American Psychiatric Pub. Arlington VA.
Bäckman, B., Pilebro, C. J. A., & j. o. d. f. c. (1999). Visual pedagogy in dentistry for children with autism. ASDC Journal of Dentistry for Children, 66(5), 325–331.
Beaglehole, R. (2003). The world health report 2003: shaping the future: World Health Organization. World Health Organization.
Bellini, S., & Akullian, J. J. (2007). A meta-analysis of video modeling and video self-modeling interventions for children and adolescents with autism spectrum disorders. Exceptional Children, 73(3), 264–287. https://doi.org/10.1177/001440290707300301
Brookman-Frazee, L., Vismara, L., Drahota, A., Stahmer, A., & Openden, D. (2009). Parent training interventions for children with autism spectrum disorders (pp. 237–257). In Applied behavior analysis for children with autism spectrum disorders (1st ed.,) Springer.
Charan, J., Biswas, T. J. I., & j. o. p. m. (2013). How to calculate sample size for different study designs in medical research? Indian Journal of Psychological Medicin., 35(2), 121. https://doi.org/10.4103/0253-7176.116232
Charlop-Christy, M. H., & Daneshvar, S. J. (2003). Using video modeling to teach perspective taking to children with autism. Journal of Positive Behavior Interventions, 5(1), 12–21. https://doi.org/10.1177/10983007030050010101
Charlop-Christy, M. H., Le, L., Freeman, K. A. J. J., & o. a., & disorders, d. (2000). A comparison of video modeling with in vivo modeling for teaching children with autism. Journal of Autism Developmental Disorders, 30(6), 537–552. https://doi.org/10.1023/A:1005635326276
Crosby, R., & Noar, S. M. J. (2011). What is a planning model? An introduction to PRECEDE-PROCEED. Journal of Public Health Dentistry, 71, 7–15. https://doi.org/10.1111/j.1752-7325.2011.00235.x
Dias, G. G., Prado, E. F., Vadasz, E., & Siqueira, J. T. T. (2010). Evaluation of the efficacy of a dental plaque control program in autistic patients. Journal of Autism and Developmental Disorders, 40(6), 704–708. https://doi.org/10.1007/s10803-009-0918-x
Du, R. Y., Yiu, C. K., King, N. M. J. J., & o. a., & disorders, d. (2019). Oral health behaviours of preschool children with autism spectrum disorders and their barriers to dental care. Journal of Autism and Developmental Disorders, 49(2), 453–459. https://doi.org/10.1007/s10803-018-3708-5
Feucht, S., & Ogata, N. B. (2010). Nutrition concerns of children with autism spectrum disorders. Nutrition, 25(4), 2–15.
Gandhi, R. P., & Klein, U. (2014). Autism spectrum disorders: An update on oral health management. Journal of Evidence Based Dental Practice, 14, 115–126. https://doi.org/10.1016/j.jebdp.2014.03.002
Ghaffari, M., Rakhshanderou, S., Ramezankhani, A., Noroozi, M., & Armoon, B. J. (2018). Oral health education and promotion programmes: Meta-analysis of 17-year intervention. International Journal of Dental Hygiene, 16(1), 59–67. https://doi.org/10.1111/idh.12304
Greene, J. G., Vermillion, J. R. J. T. J., & o. t. A. D. A. (1964). The simplified oral hygiene index. Journal of the American Dental Association, 68(1), 7–13. https://doi.org/10.14219/jada.archive.1964.0034
Happé, F. (2011). Criteria, categories, and continua: Autism and related disorders in DSM-5. Journal of the American Academy of Child & Adolescent Psychiatry, 50(6), 540–542.
Hong, E. R., Ganz, J. B., Mason, R., Morin, K., Davis, J. L., Ninci, J., & Gilliland, W. D. J. (2016). The effects of video modeling in teaching functional living skills to persons with ASD: A meta-analysis of single-case studies. Research in Developmental Disabilities, 57(14), 158–169. https://doi.org/10.1016/j.ridd.2016.07.001
Jaber, M. A. (2011). Dental caries experience, oral health status and treatment needs of dental patients with autism. Journal of Applied Oral Science, 19(3), 212–217. https://doi.org/10.1590/S1678-77572011000300006
Kolawole, K. A., & Folayan, M. O. J. (2019). Association between malocclusion, caries and oral hygiene in children 6 to 12 years old resident in suburban Nigeria. BMC Oral Health, 19(1), 1–9. https://doi.org/10.1186/s12903-019-0959-2
McCoy, K., & Hermansen, E. J. (2007). Video modeling for individuals with autism: A review of model types and effects. Education Treatment of Children, 30(4), 183–213.
Mohammadpour, V., Babapour Kheyroddin, J., & Bakhshipour Roudsari, A. J. (2013). Effects of video modeling on self-help skills in children with autism spectrum disorders. Razi Journal of Medical Sciences, 20(106), 48–56.
Montazeri, A., Goshtasebi, A., & Vahdaninia, M. J. (2008). Educational inequalities in self-reported health in a general iranian population. BMC Research Notes, 1(1), 1–6. https://doi.org/10.1186/1756-0500-1-50
Nilchian, F., Shakibaei, F., & Jarah, Z. T. (2017). Evaluation of visual pedagogy in dental check-ups and preventive practices among 6–12-year-old children with autism. Journal of Autism and Developmental Disorders, 47(3), 858–864. https://doi.org/10.1007/s10803-016-2998-8
Pilebro, C., Bäckman, B. J. I. J., & o. P. D. (2005). Teaching oral hygiene to children with autism. International Journal of Paediatric Dentistry, 15(1), 1–9. https://doi.org/10.1111/j.1365-263X.2005.00589.x
Piraneh, H., Gholami, M., Sargeran, K., & Shamshiri, A. R. (2022). Oral health and dental caries experience among students aged 7–15 years old with autism spectrum disorders in Tehran. Iran. BMC Pediatrics, 22(1), 116. https://doi.org/10.1186/s12887-022-03178-5
Polit, D. F., & Beck, C. T. (2004). Nursing research: Principles and methods. Lippincott Williams & Wilkins.
Popple, B., Wall, C., Flink, L., Powell, K., Discepolo, K., Keck, D., & Shic, F. (2016). Brief report: Remotely delivered video modeling for improving oral hygiene in children with ASD: A pilot study. Journal of Autism and Developmental Disorders, 46(8), 2791–2796. https://doi.org/10.1007/s10803-016-2795-4
Redman, S. P., & CL. (1997). A review of the effectiveness of print material in changing health-related knowledge, attitudes and behaviour. Health Promotion Journal of Australia: Official Journal of Australian Association of Health Promotion Professionals, 7(2), 91–99.
Rekha, C. V., Arangannal, P., Shahed, H. J. E. A., & o. P. D. (2012). Oral health status of children with autistic disorder in Chennai. European Archives of Paediatric Dentistry, 13(3), 126–131.
Saied-Moallemi, Z. (2010). Oral health among iranian preadolescents: A school-based health education intervention. Retrieved from https://helda.helsinki.fi/bitstream/handle/10138/20269/oralheal.pdf?sequence=1
Shalev, R. A., Lavine, C., & Di Martino, A. J. (2020). A systematic review of the role of parent characteristics in parent-mediated interventions for children with autism spectrum disorder. Journal of Developmental Physical Disabilities, 32(1), 1–21. https://doi.org/10.1007/s10882-018-9641-x
Smutkeeree, A., Khrautieo, T., Thamseupsilp, S., Srimaneekarn, N., Rirattanapong, P., Wanpen, W. J. J., & o. I. S. o. P., & Dentistry, C. (2020). The effectiveness of visual pedagogy for toothbrushing in children with autism spectrum disorder. Journal of International Society of Preventive and Community Dentistry, 10(4), 415. https://doi.org/10.4103/jispcd.JISPCD_248_20
Styles, A. J. E. P., & i. P. (2011). Social StoriesTM: Does the research evidence support the popularity? Educational Psychology in Practice, 27(4), 415–436. https://doi.org/10.1080/02667363.2011.624312
Taber, K. S. J. R., & i. S. E. (2018). The use of Cronbach’s alpha when developing and reporting research instruments in science education. Research in Science Education, 48(6), 1273–1296. https://doi.org/10.1007/s11165-016-9602-2
Watkins, L., O’Reilly, M., Kuhn, M., Gevarter, C., Lancioni, G. E., Sigafoos, J., & Lang, R. J. (2015). A review of peer-mediated social interaction interventions for students with autism in inclusive settings. Journal of Autism Developmental Disorders, 45(4), 1070–1083. https://doi.org/10.1007/s10803-014
Zhou, N., Wong, H. M., & McGrath, C. J. (2020). Efficacy of social story intervention in training toothbrushing skills among special-care children with and without autism. Autism Research, 13(4), 666–674. https://doi.org/10.1002/aur.2256
Acknowledgments
This study was part of a Ph.D. thesis funded by Research Center for Caries Prevention, Dentistry Research Institute, Department of Community Oral Health, School of Dentistry, Tehran University of Medical Sciences, Tehran, Iran (Grant No. 98-03-238-46126).
Funding
This study was funded by Research Center for Caries Prevention, Dentistry Research Institute, Department of Community Oral Health, School of Dentistry, Tehran University of Medical Sciences, Tehran, Iran (Grant No. 98–03-238–46126). The funder did not influence the research by any means and the research was carried out independently.
Author information
Authors and Affiliations
Contributions
All authors contributed to the design and conceptualization of the study; HP contributed to data collection and intervention conduction; HP, MG and ARS contributed to data analysis; HP, KS, and MG contributed in writing and revising the manuscript. All authors read and approved the final version of the manuscript; and agreed to be responsible for all aspects of the study including the accuracy of the work done.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare that are relevant to the content of this article.
Ethical Approval
This study was approved by the Research Ethic Committee of the School of Dentistry, Tehran University of Medical Sciences (IR.TUMS.DENTISTRY.REC.1398.153). In addition, this trial was registered in the Iranian Registry of Clinical Trials (Registration number: IRCT20200208046413N1).
Consent to Participate
Written informed consent was obtained from parents before the study.
Consent to Publish
The parents and participants were assured that their identity would remain anonymous.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Piraneh, H., Gholami, M., Sargeran, K. et al. Social Story Based Toothbrushing Education Versus Video-Modeling Based Toothbrushing Training on Oral Hygiene Status Among Male Students Aged 7–15 Years Old with Autism Spectrum Disorders in Tehran, Iran: A Quasi-Randomized Controlled Trial. J Autism Dev Disord 53, 3813–3824 (2023). https://doi.org/10.1007/s10803-022-05679-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10803-022-05679-9