Abstract
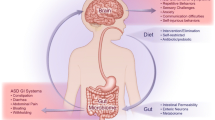
Autism spectrum disorder (ASD) is a complex neurological and developmental disorder, and a growing body of literature suggests the presence of autonomic nervous system (ANS) dysfunction in individuals with ASD. ANS is part of the “gut brain axis”, which consists of an intricate interplay between the gut microbiome, mucosal immune system, enteric nervous system, ANS, and central processes receiving input from the vagus nerve. Measurements of the gut microbiome and the autonomic indices can serve as non-invasive markers of the status of the gut-brain axis in ASD. To our knowledge, no previous studies have explored the relationship between ANS and gut microbiome in individuals with ASD. Furthermore, while previous studies investigated the use of autonomic indices and gut microbiome independently as markers of ASD-related comorbidities, such as anxiety, cardiovascular issues, and gastrointestinal dysfunction, the use of combined autonomic indices and gut microbiome factors to classify ASD and control subjects has not been explored. In this study, we characterized autonomic function of a group of individuals with ASD in comparison to their paired, first-degree relative controls. Second, we explored the ASD gut-brain-axis through the relationship between gut microbiome markers and autonomic indices, as well as the correlation between the gut-brain-axis and clinical presentation of ASD. Lastly, this study explores the predictive capability of gut-brain-axis biomarkers (including autonomic and microbiome indices) in subtyping ASD cases, serving as a starting point to investigate the possibility of assisting in ASD screening and diagnosis that still heavily relies on psychological testing, which may be based on highly subjective standards.



Similar content being viewed by others
Data Availability
All the data and code scripts in this project have been deposited to https://doi.org/10.6084/m9.figshare.11369133.v1.
Abbreviations
- AD(H)D:
-
Attention deficit (hyperactivity) disorder
- ANS:
-
Autonomic nervous system
- ASD:
-
Autism spectrum disorders
- ATEC:
-
Autism treatment evaluation checklist
- AUC:
-
Area under the curve
- BVP:
-
Blood volume pulse
- CI:
-
Confidence interval
- CNS:
-
Central nervous system
- cvNNI:
-
Coefficient of variation
- CVSD:
-
Coefficient of variation of successive differences
- DSM-5:
-
Diagnostic and statistical manual of mental disorders
- EDA:
-
Electrodermal activity
- FDR:
-
False discovery rate
- GI:
-
Gastrointestinal
- HR:
-
Heart rate
- IBI:
-
Interbeat interval
- IQ:
-
Intelligence quotient
- LOOCV:
-
Leave-one-out cross-validation
- MGH:
-
Massachusetts general hospital
- NNI50:
-
Number of pairs of successive NN (R–R) intervals that differ by more than 50 ms
- OASIS:
-
Overall anxiety severity impairment scale
- PCA:
-
Principal component analysis
- PHQ-9:
-
Patient health questionnaire
- pNNI50:
-
Percentage of adjacent NN (R–R) intervals that differ by more than 50 ms
- RMSSD:
-
Root mean square of successive differences
- ROC:
-
Receiver operator characteristics
- rRNA:
-
Ribosomal RNA
- sdNN:
-
Standard deviation of NN (R–R) intervals
References
Allen, J. (2007). Photoplethysmography and its application in clinical physiological measurement. Physiological Measurement, 28, R1–R39. https://doi.org/10.1088/0967-3334/28/3/R01.
Baio, J., Wiggins, L., Christensen, D. L., Maenner, M. J., Daniels, J., Warren, Z., et al. (2018). Prevalence of autism spectrum disorder among children aged 8 years—Autism and developmental disabilities monitoring network, 11 sites, United States, 2014. MMWR Surveillance Summaries, 67, 1–23. https://doi.org/10.15585/mmwr.ss6706a1.
Bari, D. S., Aldosky, H. Y. Y., Tronstad, C., Kalvøy, H., & Martinsen, Ø. G. (2017). Electrodermal responses to discrete stimuli measured by skin conductance, skin potential, and skin susceptance. Skin Research and Technology, 24, 108–116. https://doi.org/10.1111/srt.12397.
Bauman, M. L. (2010). Medical comorbidities in autism: Challenges to diagnosis and treatment. Neurotherapeutics, 7, 320–327. https://doi.org/10.1016/j.nurt.2010.06.001.
Benevides, T. W., & Lane, S. J. (2013). A review of cardiac autonomic measures: Considerations for examination of physiological response in children with autism spectrum disorder. Journal of Autism and Developmental Disorders, 45, 560–575. https://doi.org/10.1007/s10803-013-1971-z.
Buffington, S. A., Di Prisco, G. V., Auchtung, T. A., Ajami, N. J., Petrosino, J. F., & Costa-Mattioli, M. (2016). Microbial reconstitution reverses maternal diet-induced social and synaptic deficits in offspring. Cell, 165, 1762–1775. https://doi.org/10.1016/j.cell.2016.06.001.
Cheshire, W. P. (2012). Highlights in clinical autonomic neuroscience: New insights into autonomic dysfunction in autism. Autonomic Neuroscience, 171, 4–7. https://doi.org/10.1016/j.autneu.2012.08.003.
Fleming, S., Thompson, M., Stevens, R., Heneghan, C., Plüddemann, A., Maconochie, I., et al. (2011). Normal ranges of heart rate and respiratory rate in children from birth to 18 years of age: A systematic review of observational studies. The Lancet, 377, 1011–1018. https://doi.org/10.1016/S0140-6736(10)62226-X.
Frank, D. N., Amand, A. L. S., Feldman, R. A., Boedeker, E. C., Harpaz, N., & Pace, N. R. (2007). Molecular-phylogenetic characterization of microbial community imbalances in human inflammatory bowel diseases. Proceedings of the National academy of Sciences of the United States of America, 104, 13780–13785. https://doi.org/10.1073/pnas.0706625104.
Friedman, B. H. (2007). An autonomic flexibility–neurovisceral integration model of anxiety and cardiac vagal tone. Biological Psychology, 74, 185–199.
Hsiao, E. Y., McBride, S. W., Hsien, S., Sharon, G., Hyde, E. R., McCue, T., et al. (2013). Microbiota modulate behavioral and physiological abnormalities associated with neurodevelopmental disorders. Cell, 155, 1451–1463. https://doi.org/10.1016/j.cell.2013.11.024.
Hyland, N. P., & Cryan, J. F. (2016). Microbe-host interactions—Influence of the gut microbiota on the enteric nervous system. Developmental Biology, 417, 182–187. https://doi.org/10.1016/j.ydbio.2016.06.027.
Johnson, K. V. A., & Burnet, P. W. J. (2016). Microbiome: Should we diversify from diversity? Gut Microbes, 7, 455–458. https://doi.org/10.1080/19490976.2016.1241933.
Klusek, J., Roberts, J. E., & Losh, M. (2015). Cardiac autonomic regulation in autism and fragile X syndrome: A review. Psychological Bulletin, 141, 141–175.
Kong, X., Liu, J., Cetinbas, M., Sadreyev, R., Koh, M., Huang, H., et al. (2019). New and preliminary evidence on altered oral and gut microbiota in individuals with autism spectrum disorder (ASD): Implications for ASD diagnosis and subtyping based on microbial biomarkers. Nutrients, 11, 2128–2226. https://doi.org/10.3390/nu11092128.
Kraneveld, A. D., Szklany, K., de Theije, C. G. M., & Garssen, J. D. (2016). Gut-to-brain axis in autism spectrum disorders: Central role for the microbiome. International Review of Neurobiology, 131, 263–287.
Kulkarni, S., Ganz, J., Bayrer, J., Becker, L., Bogunovic, M., & Rao, M. (2018). Advances in enteric neurobiology: The “brain” in the gut in health and disease. Journal of Neuroscience, 38, 9346–9354. https://doi.org/10.1523/JNEUROSCI.1663-18.2018.
Kushki, A., Brian, J., Dupuis, A., & Anagnostou, E. (2014). Functional autonomic nervous system profile in children with autism spectrum disorder. Molecular Autism, 5, 39–39.
Liu, J., Zhang, M., & Kong, X. (2016). Gut microbiome and autism: Recent advances and future perspectives. American Journal of Medicine and Science. https://doi.org/10.7156/najms.2016.0903104.
Lombard, J. H., & Cowley, A. W. (2012). Chapter 38—Neural control of blood vessels. In D. Robertson, I. Biaggioni, G. Burnstock, P. A. Low, & J. F. R. Paton (Eds.), Primer on the autonomic nervous system (3rd ed., pp. 187–191). San Diego: Academic Press.
Mangina, C. A., & Beuzeron-Mangina, J. H. (1996). Direct electrical stimulation of specific human brain structures and bilateral electrodermal activity. International Journal of Psychophysiology, 22, 1–8.
Mayer, E. A., Tillisch, K., & Gupta, A. M. (2015). Gut/brain axis and the microbiota. The Journal of Clinical Investigation, 125, 926–938.
McCorry, L. K. (2007). Physiology of the autonomic nervous system. American Journal of Pharmaceutical Education, 71, 78–78.
Messina, A., Monda, V., Sessa, F., Valenzano, A., Salerno, M., Bitetti, I., et al. (2018). Sympathetic, metabolic adaptations, and oxidative stress in autism spectrum disorders: How far from physiology? Frontiers in Physiology, 9, 146–156. https://doi.org/10.3389/fphys.2018.00261.
Mouridsen, S. E., Brønnum-Hansen, H., Rich, B., & Isager, T. (2008). Mortality and causes of death in autism spectrum disorders. Autism, 12, 403–414. https://doi.org/10.1177/1362361308091653.
Muskens, J. B., Velders, F. P., & Staal, W. G. (2017). Medical comorbidities in children and adolescents with autism spectrum disorders and attention deficit hyperactivity disorders: A systematic review. European Child & Adolescent Psychiatry, 26, 1093–1103. https://doi.org/10.1007/s00787-017-1020-0.
Panju, S., Brian, J., Dupuis, A., Anagnostou, E., & Kushki, A. (2015). Atypical sympathetic arousal in children with autism spectrum disorder and its association with anxiety symptomatology. Molecular Autism. https://doi.org/10.1186/s13229-015-0057-5.
Picard, R. W., Devinsky, O., Dworetzky, B., French, J. A., Friedman, D., Lai, M., et al. (2015). The importance of measuring autonomic data in new epilepsy treatments. Epilepsy & Behavior, 46, 54–55. https://doi.org/10.1016/j.yebeh.2015.02.053.
Porges, S. W. (1995). Cardiac vagal tone: A physiological index of stress. Neuroscience and Biobehavioral Reviews, 19, 225–233.
Prince, E. B., Kim, E. S., Wall, C. A., Gisin, E., Goodwin, M. S., Simmons, E. S., et al. (2016). The relationship between autism symptoms and arousal level in toddlers with autism spectrum disorder, as measured by electrodermal activity. Autism, 21, 504–508. https://doi.org/10.1177/1362361316648816.
Rajendra Acharya, U., Paul Joseph, K., Kannathal, N., Lim, C. M., & Suri, J. S. (2006). Heart rate variability: A review. Medical & Biological Engineering & Computing, 44, 1031–1051. https://doi.org/10.1007/s11517-006-0119-0.
Roberts, J. E., Tonnsen, B., Robinson, A., & Shinkareva, S. V. (2012). Heart activity and autistic behavior in infants and toddlers with fragile X syndrome. American Journal on Intellectual and Developmental Disabilities, 117, 90–102. https://doi.org/10.1352/1944-7558-117.2.90.
Rosenfeld, C. S. (2015). Microbiome disturbances and autism spectrum disorders. Drug Metabolism and Disposition, 43, 1557–1571. https://doi.org/10.1124/dmd.115.063826.
Sahar, T., Shalev, A. Y., & Porges, S. W. (2001). Vagal modulation of responses to mental challenge in posttraumatic stress disorder. Biological Psychiatry, 49, 637–643. https://doi.org/10.1016/S0006-3223(00)01045-3.
Sano, A., Picard, R. W., & Stickgold, R. (2014). Quantitative analysis of wrist electrodermal activity during sleep. International Journal of Psychophysiology, 94, 382–389. https://doi.org/10.1016/j.ijpsycho.2014.09.011.
Schmitz, J., Krämer, M., Tuschen-Caffier, B., Heinrichs, N., & Blechert, J. (2011). Restricted autonomic flexibility in children with social phobia. Journal of Child Psychology and Psychiatry, 52, 1203–1211. https://doi.org/10.1111/j.1469-7610.2011.02417.x.
Sgritta, M., Dooling, S. W., Buffington, S. A., Momin, E. N., Francis, M. B., Britton, R. A., et al. (2018). Mechanisms underlying microbial-mediated changes in social behavior in mouse models of autism spectrum disorder. Neuron. https://doi.org/10.1016/j.neuron.2018.11.018.
Shelley, K. H. (2007). Photoplethysmography: Beyond the calculation of arterial oxygen saturation and heart rate. Anesthesia & Analgesia, 105, S31–S36. https://doi.org/10.1213/01.ane.0000269512.82836.c9.
Silvetti, M. S., Drago, F., & Ragonese, P. (2001). Heart rate variability in healthy children and adolescents is partially related to age and gender. International Journal of Cardiology, 81, 169–174. https://doi.org/10.1016/s0167-5273(01)00537-x.
Simonoff, E., Pickles, A., Charman, T., Chandler, S., Loucas, T., & Baird, G. (2008). Psychiatric disorders in children with autism spectrum disorders: Prevalence, comorbidity, and associated factors in a population-derived sample. Journal of the American Academy of Child and Adolescent Psychiatry, 47, 921–929. https://doi.org/10.1097/CHI.0b013e318179964f.
Stigler, K. A., Sweeten, T. L., Posey, D. J., & McDougle, C. J. (2009). Autism and immune factors: A comprehensive review. Research in Autism Spectrum Disorders, 3, 840–860. https://doi.org/10.1016/j.rasd.2009.01.007.
Strati, F., Cavalieri, D., Albanese, D., De Felice, C., Donati, C., Hayek, J., et al. (2017). New evidences on the altered gut microbiota in autism spectrum disorders. Microbiome, 5(1), 24. https://doi.org/10.1186/s40168-017-0242-1.
Thapa, R., Alvares, G. A., Zaidi, T. A., Thomas, E. E., Hickie, I. B., Park, S. H., et al. (2019). Reduced heart rate variability in adults with autism spectrum disorder. Autism Research, 12, 922–930. https://doi.org/10.1002/aur.2104.
Turnbaugh, P. J., Hamady, M., Yatsunenko, T., Cantarel, B. L., Duncan, A., Ley, R. E., et al. (2008). A core gut microbiome in obese and lean twins. Nature, 457, 480–484. https://doi.org/10.1038/nature07540.
Umetani, K., Singer, D. H., McCraty, R., & Atkinson, M. (1998). Twenty-four hour time domain heart rate variability and heart rate: Relations to age and gender over nine decades. Journal of the American College of Cardiology, 31, 593–601. https://doi.org/10.1016/S0735-1097(97)00554-8.
van De Sande, M. M. H., van Buul, V. J., & Brouns, F. J. P. H. (2014). Autism and nutrition: The role of the gut-brain axis. Nutrition Research Reviews, 27, 199–214. https://doi.org/10.1017/S0954422414000110.
Venables, P. H., & Mitchell, D. A. (1996). The effects of age, sex and time of testing on skin conductance activity. Biological Psychology, 43, 87–101.
Vuong, H. E., & Hsiao, E. Y. (2017). Emerging roles for the gut microbiome in autism spectrum disorder. Biological Psychiatry, 81, 411–423. https://doi.org/10.1016/j.biopsych.2016.08.024.
Yeragani, V. K., Pohl, R., Berger, R., Balon, R., Ramesh, C., Glitz, D., et al. (1993). Decreased heart rate variability in panic disorder patients: A study of power-spectral analysis of heart rate. Psychiatry Research, 46, 89–103.
Acknowledgments
Dr. Hang Lee, Harvard Catalyst biostatistics core. Dr. Yiqing Song, University of Indiana. Dr. Cunjian Dong, Massachusetts General Hospital.
Funding
This study was funded by Massachusetts General Hospital Grant Number 230361 at the Athinoula A. Martinos Center for Biomedical Imaging, Boston, MA.
Author information
Authors and Affiliations
Contributions
XK devised the project and the main conceptual ideas. XK, MK and JL worked out almost all of the technical details, and XK, JL and MK performed data collections and measurements with help from KL and CH. JL, KL, RT and CH performed bioinformatics analyses and statistical analyses, with assistance from MZ and QC and input from HL; XK and JL wrote the manuscript, with assistance from KL, RT, and MF, and input from JK; JL, KL, and RT drafted the figures with input from XK and JK; XK, JK, JL, KL, RT, and MF participated in manuscript editing.
Corresponding author
Ethics declarations
Conflict of interest
Authors report no conflict of interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kong, X., Liu, J., Liu, K. et al. Altered Autonomic Functions and Gut Microbiome in Individuals with Autism Spectrum Disorder (ASD): Implications for Assisting ASD Screening and Diagnosis. J Autism Dev Disord 51, 144–157 (2021). https://doi.org/10.1007/s10803-020-04524-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10803-020-04524-1