Abstract
Purpose
To determine the impact of type 2 diabetes mellitus (T2DM) on visual functions, identify different modifiers as risk or protective factors, and find out how these factors affect patients’ visual symptoms and visual functions as a whole.
Methods
We performed an online survey among 1030 participants (400 patients, 630 non-patients). Demographic features and severity of disease were documented, while visual functions were evaluated using National Eye Institute Visual Functioning questionnaire-25 (NEI VFQ-25). Independent t-test, analysis of variance, linear and nonlinear regression models were used to assess all data.
Results
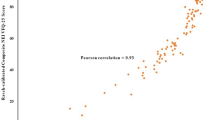
Scores other than color vision among T2DM patients were significantly lower compared with non-T2DM participants. There was significant difference after stratification of age and education, but no significant difference between different genders was observed. Parameters including duration of T2DM, fasting plasma glucose (FPG) and glycosylated hemoglobin A1c (HbA1c) negatively impacted on the scores, with 20 years’ of diabetic duration, 10 mmol/L of FPG, 7.5% of HbA1c being potential cut-off points. Poorer best corrected visual acuity (BCVA) and diagnosis of diabetic retinopathy were risk factors, while they simultaneously produced mediation effect, contributing 5%-78% of effect in the deterioration of visual functions caused by longer diabetic duration and higher blood glucose.
Conclusion
Significant visual impairments and faster deterioration in visual functions were seen in T2DM patients, with older age, lower educational level, longer diabetic duration, poorer blood glucose administration, limited BCVA, and the presence of diabetic retinopathy identified as risk factors. Average BCVA and diabetic retinopathy also yielded mediation effect as diabetic duration lengthened and blood glucose elevated.


Similar content being viewed by others
References
Lancet T (2020) Diabetes Endocrinology Under the lens: diabetic retinopathy. Lancet Diabetes Endocrinol 8(11):869. https://doi.org/10.1016/S2213-8587(20)30347-8 (Epub 2020 Oct 7 PMID: 33038294)
Ogurtsova K, da Rocha Fernandes JD, Huang Y (2017) IDF Diabetes Atlas: Global estimates for the prevalence of diabetes for 2015 and 2040. Diabetes Res Clin Pract 128:40–50. https://doi.org/10.1016/j.diabres.2017.03.024
Heng LZ, Comyn O, Peto T (2013) Diabetic retinopathy: pathogenesis, clinical grading, management and future developments. Diabet Med 30(6):640–650. https://doi.org/10.1111/dme.12089
Romero-Aroca P, Baget-Bernaldiz M, Pareja-Rios A, Lopez-Galvez M, Navarro-Gil R, Verges R (2016) Diabetic macular edema pathophysiology: vasogenic versus inflammatory. J Diabetes Res 2016:2156273. https://doi.org/10.1155/2016/2156273
Khan A, Petropoulos IN, Ponirakis G, Malik RA (2017) Visual complications in diabetes mellitus: beyond retinopathy. Diabet Med. https://doi.org/10.1111/dme.13296
GBD 2019 Blindness and Vision Impairment Collaborators; Vision Loss Expert Group of the Global Burden of Disease Study (2021) Causes of blindness and vision impairment in 2020 and trends over 30 years, and prevalence of avoidable blindness in relation to VISION 2020: the Right to Sight: an analysis for the Global Burden of Disease Study [published correction appears in Lancet Glob Health. 2021 Apr;9(4):e408]. Lancet Glob Health. https://doi.org/10.1016/S2214-109X(20)30489-7
Ting DS, Cheung GC, Wong TY (2016) Diabetic retinopathy: global prevalence, major risk factors, screening practices and public health challenges: a review. Clin Exp Ophthalmol. https://doi.org/10.1111/ceo.12696
Yin L, Zhang D, Ren Q, Su X, Sun Z (2020) Prevalence and risk factors of diabetic retinopathy in diabetic patients: A community based cross-sectional study. Medicine (Baltimore). https://doi.org/10.1097/MD.0000000000019236
Wat N, Wong RL, Wong IY (2016) Associations between diabetic retinopathy and systemic risk factors. Hong Kong Med J. https://doi.org/10.12809/hkmj164869
Siersma V, Køster-Rasmussen R, Bruun C, Olivarius NF, Brunes A (2019) Visual impairment and mortality in patients with type 2 diabetes. BMJ Open Diabetes Res Care. https://doi.org/10.1136/bmjdrc-2018-000638
Cusick M, SanGiovanni JP, Chew EY, Csaky KG, Hall-Shimel K, Reed GF, Caruso RC, Ferris FL 3rd (2005) Central visual function and the NEI-VFQ-25 near and distance activities subscale scores in people with type 1 and 2 diabetes. Am J Ophthalmol 139(6):1042–1050. https://doi.org/10.1016/j.ajo.2005.01.008
Mangione, C. M., Lee, P. P., Gutierrez, P. R., Spritzer, K., Berry, S., Hays, R. D., & National Eye Institute Visual Function Questionnaire Field Test Investigators (2001) Development of the 25-item National Eye Institute Visual Function Questionnaire. Archives of Ophthalmology (Chicago, Ill: 1960), 119(7), 1050–1058. https://doi.org/10.1001/archopht.119.7.1050
Fenwick EK, Man REK, Gan ATL et al (2019) Beyond vision loss: the independent impact of diabetic retinopathy on vision-related quality of life in a Chinese Singaporean population. Br J Ophthalmol. https://doi.org/10.1136/bjophthalmol-2018-313082
Schuster AK, Pfeiffer N, Schulz A et al (2017). The impact of pseudophakia on vision-related quality of life in the general population - The Gutenberg Health Study. Aging (Albany NY). https://doi.org/10.18632/aging.101208
Hariprasad SM, Mieler WF, Grassi M, Green JL, Jager RD, Miller L (2008) Vision-related quality of life in patients with diabetic macular oedema. Br J Ophthalmol 92(1):89–92. https://doi.org/10.1136/bjo.2007.122416
Trento M, Passera P, Trevisan M, Schellino F, Sitia E, Albani S, Montanaro M, Bandello F, Scoccianti L, Charrier L, Cavallo F, Porta M (2013) Quality of life, impaired vision and social role in people with diabetes: a multicenter observational study. Acta Diabetol 50(6):873–877. https://doi.org/10.1007/s00592-013-0470-1
Araki A, Ito H (2009) Diabetes mellitus and geriatric syndromes. Geriatr Gerontol Int 9(2):105–114. https://doi.org/10.1111/j.1447-0594.2008.00495.x
Man REK, Gan ATL, Fenwick EK et al (2021) The differential impact of age on vision-related quality of life across the visual impairment spectrum. Ophthalmology. https://doi.org/10.1016/j.ophtha.2020.07.046
Song P, Yu J, Chan KY, Theodoratou E, Rudan I (2018) Prevalence, risk factors and burden of diabetic retinopathy in China: a systematic review and meta-analysis. J Glob Health 8(1):010803. https://doi.org/10.7189/jogh.08.010803
Ben Mehidi A, Massin P, Guyot-Argenton C, Erginay A, Guillausseau PJ, Gaudric A (2003) La rétinopathie diabétique du sujet jeune: l’enfant et l’adolescent [Diabetic retinopathy in children and adolescents]. Diabetes Metab 29(3):300–306
Danet-Lamasou M, Pérès K, Matharan F, Berr C, Carrière I, Tzourio C, Delcourt C, Bourdel-Marchasson I (2018) Near Visual Impairment Incidence in Relation to Diabetes in Older People: The Three-Cities Study. J Am Geriatr Soc 66(4):699–705
de Fine Olivarius N, Siersma V, Almind GJ, Nielsen NV (2011) Prevalence and progression of visual impairment in patients newly diagnosed with clinical type 2 diabetes: a 6-year follow up study. BMC Public Health 11:80. https://doi.org/10.1186/1471-2458-11-80
Kajiwara A, Miyagawa H, Saruwatari J, Kita A, Sakata M, Kawata Y, Oniki K, Yoshida A, Jinnouchi H, Nakagawa K (2014) Gender differences in the incidence and progression of diabetic retinopathy among Japanese patients with type 2 diabetes mellitus: a clinic-based retrospective longitudinal study. Diabetes Res Clin Pract 103(3):e7–e10. https://doi.org/10.1016/j.diabres.2013.12.043
Ozawa GY, Bearse MA Jr, Adams AJ (2015) Male-female differences in diabetic retinopathy? Curr Eye Res 40(2):234–246. https://doi.org/10.3109/02713683.2014.958500
Maric-Bilkan C. (2017) Sex differences in micro- and macro-vascular complications of diabetes mellitus. Clinical science (London, England: 1979), 131(9), 833–846. https://doi.org/10.1042/CS20160998
Zoungas S, Woodward M, Li Q et al (2014) Impact of age, age at diagnosis and duration of diabetes on the risk of macrovascular and microvascular complications and death in type 2 diabetes. Diabetologia. https://doi.org/10.1007/s00125-014-3369-
Taylor SI, Yazdi ZS, Beitelshees AL (2021) Pharmacological treatment of hyperglycemia in type 2 diabetes. J Clin Invest. https://doi.org/10.1172/JCI142243
Gebreyohannes EA, Netere AK, Belachew SA (2019) Glycemic control among diabetic patients in Ethiopia: A systematic review and meta-analysis. PLoS ONE. https://doi.org/10.1371/journal.pone.0221790
Foo V, Quah J, Cheung G, Tan NC, Ma Zar KL, Chan CM, Lamoureux E, Tien Yin W, Tan G, Sabanayagam C (2017) HbA1c, systolic blood pressure variability and diabetic retinopathy in Asian type 2 diabetics. J Diabetes 9(2):200–207. https://doi.org/10.1111/1753-0407.12403
Kahloun R, Jelliti B, Zaouali S, Attia S, Ben Yahia S, Resnikoff S, Khairallah M (2014) Prevalence and causes of visual impairment in diabetic patients in Tunisia, North Africa. Eye (Lond) 28(8):986–991. https://doi.org/10.1038/eye.2014.131
Liu Y, Duan C, Fang D, Liu Y, Xu H, Zheng Y, Xuan Y, Wang L, Ye L, Su R, An M (2019) Protective factors for diabetic retinopathy in Type 2 diabetes mellitus patients: Long duration of no less than 10 years. J Diabetes Complications 33(10):107383. https://doi.org/10.1016/j.jdiacomp.2019.05.014
Škrha J, Šoupal J, Škrha J Jr, Prázný M (2016) Glucose variability, HbA1c and microvascular complications. Rev Endocr Metab Disord 17(1):103–110. https://doi.org/10.1007/s11154-016-9347-2
Hsieh YT, Hsieh MC (2020) Fasting plasma glucose variability is an independent risk factor for diabetic retinopathy and diabetic macular oedema in type 2 diabetes: An 8-year prospective cohort study. Clin Experiment Ophthalmol 48(4):470–476. https://doi.org/10.1111/ceo.13728
Lim HB, Shin YI, Lee MW, Lee JU, Lee WH, Kim JY (2020) Association of myopia with peripapillary retinal nerve fiber layer thickness in diabetic patients without diabetic retinopathy. Invest Ophthalmol Vis Sci 61(10):30. https://doi.org/10.1167/iovs.61.10.30
Feitosa-Santana C, Paramei GV, Nishi M, Gualtieri M, Costa MF, Ventura DF (2010) Color vision impairment in type 2 diabetes assessed by the D-15d test and the Cambridge Colour Test. Ophthalmic & Physiological Optics: the Journal of the British College of Ophthalmic Opticians (Optometrists) 30(5):717–723. https://doi.org/10.1111/j.1475-1313.2010.00776.x
Wolff BE, Bearse MA Jr, Schneck ME, Dhamdhere K, Harrison WW, Barez S, Adams AJ (2015) Color vision and neuroretinal function in diabetes. Documenta Ophthalmologica Advances in Ophthalmology 130(2):131–139. https://doi.org/10.1007/s10633-014-9476-4
Hautala N, Aikkila R, Korpelainen J, Keskitalo A, Kurikka A, Falck A, Bloigu R, Alanko H (2014) Marked reductions in visual impairment due to diabetic retinopathy achieved by efficient screening and timely treatment. Acta Ophthalmol 92(6):582–587. https://doi.org/10.1111/aos.12278
Hu Y, Niu Y, Wang D, Wang Y, Holden BA, He M (2015) The association of longitudinal trend of fasting plasma glucose with retinal microvasculature in people without established diabetes. Invest Ophthalmol Vis Sci 56(2):842–848. https://doi.org/10.1167/iovs.14-15943
Funding
This study was supported by Beijing Key Laboratory Opening Funding (Grant number: BKLOF-BYSY202101).
Author information
Authors and Affiliations
Contributions
Study design and concept: SC, JY, XL; Data collection and analysis: YG, YW; Interpretation of data and critical revision of the manuscript: SC, YG, HX, RD, XR, HY, QH, JY; All authors have read and approved the final draft of the manuscript submitted.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declared that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee (Peking University Third Hospital Medical Science Research Ethics Committee, S2020023) and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chai, S., Ge, Y., Wan, Y. et al. Visual functional defects in patients with type 2 diabetes mellitus: a questionnaire based cross-sectional study. Int Ophthalmol 42, 2205–2218 (2022). https://doi.org/10.1007/s10792-022-02220-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-022-02220-w