Abstract
Purpose
To evaluate the performance of full-thickness (FT) versus partial-thickness (PT) sutures in a full-thickness corneal wound in an animal model.
Methods
This is a prospective, experimental, comparative, longitudinal study. A 6-mm linear, full-thickness corneal incision was performed on the right eye of eight domestic pigs. Eyes were randomly assigned for repair with interrupted PT (80–90% depth) sutures or FT 10-0 nylon sutures. Anterior segment OCT, corneal pachymetry and clinical photographs were obtained 1, 4 and 8 weeks postoperatively. Corneal thickness, depth of suture placement, perilesional edema, coaptation of wound edges and complications were noted. Histopathologic examination was performed at 8 weeks.
Results
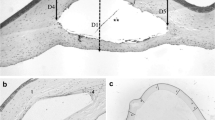
100% of the eyes with FT sutures developed a linear, less opaque scar. 100% of the eyes with PT developed a dense, opaque stromal scar (p = 0.02). Vascularization of the cornea was present in 75% of PT group and 25% in the FT group (p = 0.50). As the corneas healed, there was a marked trend toward thicker corneas in the PT group versus FT group with a median difference of − 63 µm at week 1 [median 788 µm vs. 725 µm, (p = 0.11)], − 38 µm at week 4, (724 µm vs. 686 µm, (p = 0.63)) and − 47 µm median difference at week 8 with (670 µm vs. 623 µm, (p = 0.06)). Histopathology showed disorganization of the collagen fibers and the formation of a retrocorneal fibrous membrane in the PT group.
Conclusions
The FT group presented less corneal edema at week 8 with a more linear and less opaque scar. Histopathology showed a better-organized scar and endothelialization without the formation of a fibrous membrane.






Similar content being viewed by others
References
Oum BS, Lee JS, Han YS (2004) Clinical features of ocular trauma in emergency department. Korean J Ophthalmol 18(1):70–78
Xie L, Zhai H, Dong X, Shi W (2008) Primary diseases of corneal perforation in Shandong Province, China: a 10-year retrospective study. Am J Ophthalmol 145(4):662–666
Kuhn F (2013) Ocular traumatology: from military medicine to individual brilliance. Graefes Arch Clin Exp Ophthalmol 251(3):627–628
Lovald ST, Rau A, Nissman S et al (2017) Finite element analysis and experimental evaluation of penetrating injury through the cornea. J Mech Behav Biomed Mater 66:104–110
Vora GK, Haddadin R, Chodosh J (2013) Management of corneal lacerations and perforations. Int Ophthalmol Clin 53(4):1–10
Hamill MB, Thompson WS (1990) The evaluation and management of corneal lacerations. Retina 10(Suppl 1):S1–S7
Wang T, Zhu L, Peng Y et al (2017) Photochemical cross-linking for penetrating corneal wound closure in enucleated porcine eyes. Curr Eye Res 42(11):1413–1419
Myer CM 4th, Johnson CM, Postma GN, Weinberger PM (2015) Comparison of tensile strength of fibrin glue and suture in microflap closure. Laryngoscope 125(1):167–170
Hamill MB (2002) Corneal and scleral trauma. Ophthalmol Clin North Am 15(2):185–194
Kuhn F (2007) Ocular traumatology. Springer, Berlin
Fini ME, Stramer BM (2005) How the cornea heals: cornea-specific repair mechanisms affecting surgical outcomes. Cornea 24(8 Suppl):S2–S11
Ljubimov AV, Saghizadeh M (2015) Progress in corneal wound healing. Prog Retin Eye Res. https://doi.org/10.1016/j.preteyeres.2015.07.002
Kling S, Hafezi F (2017) Corneal biomechanics—a review. Ophthalmic Physiol Opt 37(3):240–252
Sanchez I, Martin R, Ussa F, Fernandez-Bueno I (2011) The parameters of the porcine eyeball. Graefes Arch Clin Exp Ophthalmol 249(4):475–482
Faber C, Scherfig E, Prause JU, Sørensen KE (2008) Corneal thickness in pigs measured by ultrasound pachymetry in vivo. Scand J Lab Anim Sci 35(1):39–43
Siatiri H, Moghimi S, Malihi M et al (2008) Use of sealant (HFG) in corneal perforations. Cornea 27(9):988–991
Setlik DE, Seldomridge DL, Adelman RA et al (2005) The effectiveness of isobutyl cyanoacrylate tissue adhesive for the treatment of corneal perforations. Am J Ophthalmol 140(5):920–921
Miki D, Dastgheib K, Kim T et al (2002) A photopolymerized sealant for corneal lacerations. Cornea 21(4):393–399
Zheng K, Huang H, Peng K et al (2016) Change of optical intensity during healing process of corneal wound on anterior segment optical coherence tomography. Sci Rep 6(32352):1–6
Massey JY, Hanna C (1974) Penetrating keratoplasty with use of through-and-through nylon sutures. Arch Ophthalmol 91(5):381–385
Berens C, King JH (1961) An atlas of ophthalmic surgery. JB Lippincott Co., Philadelphia, pp 258–259
Macsai MS (2000) The management of corneal trauma advances in the past twenty-five years. Cornea 19(5):617–624
Bobrova NF, Shevchyk VI, Kulbida MP (2011) A -term results of full-thickness suture method of primary surgical treatment of penetrating corneal wound. Oftalmol zh. 3:8–12
Varley GA, Meisler DM (1991) Complications of penetrating keratoplasty: graft infections. Refract Corneal Surg 7(1):62–66
Rocher M, Robert PY, Desmoulière A (2020) The myofibroblasts, biological activities and roles in eye repair and fibrosis. A focus on healing mechanisms in avascular cornea. Eye 34(2):232–240
Matsuda A, Tagawa Y, Matsuda H et al (1997) Expression of macrophage migration inhibition factor in corneal wound healing in rats. Invest Ophthalmol Vis Sci 38(8):1555–1562
Funding
This project was financed by a pilot-study fund from the Asociación para Evitar la Ceguera en México, Hospital “Dr. Luis Sánchez Bulnes”, Ciudad de México, México, and was approved by the Ethics Committee of this institution.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dalma-Weiszhausz, J., Galván-Chávez, M., Guinto-Arcos, E.B. et al. Full- versus partial-thickness sutures: experimental models of corneal injury repair. Int Ophthalmol 41, 325–334 (2021). https://doi.org/10.1007/s10792-020-01585-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-020-01585-0