Abstract
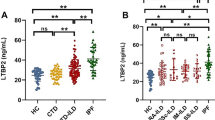
Interstitial lung disease (ILD) is a frequent extra-articular manifestation of rheumatoid arthritis (RA) and increases mortality in patients with RA. Early identification of ILD, especially the usual interstitial pneumonia (UIP) pattern with a poor prognosis, is important for guiding treatment of RA-ILD and preventing damage resulting from a delay in diagnosis. Interleukin-36 (IL-36) cytokines are involved in connective tissue diseases. However, IL-36 expression in RA-ILD is unknown. In this study, the clinical relevance of plasma IL-36 cytokines was evaluated in 39 patients with RA-ILD and three other groups (30 healthy controls [HCs], 35 RA patients without ILD, and 27 patients with idiopathic pulmonary fibrosis [IPF]) in the Chinese population. Plasma IL-36α and IL-36γ concentrations were elevated in patients with RA-ILD compared with those in HCs and patients with RA. RA-ILD patients with UIP pattern had higher plasma IL-36γ concentrations than those with RA-ILD without UIP, but these were lower than those in patients with IPF. Receiver operating curve analysis suggested that IL-36α and IL-36γ were potential biomarkers for identifying ILD in patients with RA. Additionally, the optimal cutoff value of IL-36γ for distinguishing RA-ILD with the UIP pattern from RA-ILD without UIP was 555.40 pg/mL and that for distinguishing RA-ILD from IPF was 655.10 pg/mL. No significant difference in plasma IL-36β or IL-36Ra concentrations was found between patients with RA-ILD and the three other groups. We also found that the lungs originating from different types of patients with PF, including RA-ILD and IPF, and those from mice following bleomycin-induced PF were characterized by increased IL-36γ expression. Our findings suggest that using IL-36 cytokines to identify patients with RA for further ILD workups may provide additional diagnostic value to the current clinically available assays. Moreover, IL-36γ may help to identify the presence of the UIP pattern in patients with RA-ILD and to discriminate RA-ILD from IPF.




Similar content being viewed by others
References
Smolen, J.S. 2020. Rheumatoid arthritis primer - behind the scenes. Nature Reviews. Disease Primers 6 (1): 32. https://doi.org/10.1038/s41572-020-0168-y.
Alunno, A., R. Gerli, R. Giacomelli, and F. Carubbi. 2017. Clinical, epidemiological, and histopathological features of respiratory involvement in rheumatoid arthritis. BioMed Research International 2017: 7915340. https://doi.org/10.1155/2017/7915340.
Figus, F.A., M. Piga, I. Azzolin, R. McConnell, and A. Iagnocco. 2021. Rheumatoid arthritis: Extra-articular manifestations and comorbidities. Autoimmunity Reviews 20 (4): 102776. https://doi.org/10.1016/j.autrev.2021.102776.
Chinese Rheumatology Association. 2018. 2018 Chinese guideline for the diagnosis and treatment of rheumatoid arthritis. Zhonghua Nei Ke Za Zhi 57 (4): 242–251. https://doi.org/10.3760/cma.j.issn.0578-1426.2018.04.004.
Yan, S.Y., Y. Cui, G.F. Zhang, G.F. Dong, Y. Feng, and Y.Y. Song. 2019. The incidence of extra-articular manifestations in southern Chinese patients with inflammatory joint diseases. International Journal of Rheumatic Diseases 22 (9): 1686–1694. https://doi.org/10.1111/1756-185X.13657.
Li, L.L., R. Liu, Y.F. Zhang, J.F. Zhou, Y.F. Li, Y.T. Xu, et al. 2020. A retrospective study on the predictive implications of clinical characteristics and therapeutic management in patients with rheumatoid arthritis-associated interstitial lung disease. Clinical Rheumatology 39 (5): 1457–1470. https://doi.org/10.1007/s10067-019-04846-1.
Liu, L., Ch.X. Fang, B. Sun, R.Y. Bao, and H.F. Zhang. 2022. Predictors of progression in rheumatoid arthritis-associated interstitial lung disease: A single-center retrospective study from China. International Journal of Rheumatic Diseases 25 (7): 795–802. https://doi.org/10.1111/1756-185X.14351.
Bongartz, T., C. Nannini, Y.F. Medina-Velasquez, S.J. Achenbach, C.S. Crowson, J.H. Ryu, et al. 2010. Incidence and mortality of interstitial lung disease in rheumatoid arthritis: A population-based study. Arthritis and Rheumatism 62 (6): 1583–1591. https://doi.org/10.1002/art.27405.
Kim S.U., B.K. Kim, J.Y. Park, D.Y. Kim, S.H. Ahn, Y.B. Park, et al. 2020. Fibrosis-4 index at diagnosis can predict all-cause mortality in patients with rheumatoid arthritis: a retrospective monocentric study. Modern Rheumatology. 30 (1): 70–77. https://doi.org/10.1080/14397595.2018.1558760.
Nakajima, A., E. Inoue, E. Tanaka, G. Singh, E. Sato, D. Hoshi, et al. 2010. Mortality and cause of death in Japanese patients with rheumatoid arthritis based on a large observational cohort, IORRA. Scandinavian Journal of Rheumatology 39 (5): 360–7. https://doi.org/10.3109/03009741003604542.
Fu, Q., L. Wang, L.L. Li, Y.F. Li, R. Liu, and Y. Zheng. 2019. Risk factors for progression and prognosis of rheumatoid arthritis-associated interstitial lung disease: Single center study with a large sample of Chinese population. Clinical Rheumatology 38 (4): 1109–1116. https://doi.org/10.1007/s10067-018-4382-x.
Olson, A.L., J.J. Swigris, D.B. Sprunger, A. Fischer, E.R. Fernandez-Perez, J. Solomon, et al. 2011. Rheumatoid arthritis-interstitial lung disease-associated mortality. American Journal of Respiratory and Critical Care Medicine 183 (3): 372–378. https://doi.org/10.1164/rccm.201004-0622OC.
Wu, E.K., R.D. Ambrosini, R.M. Kottmann, C.T. Ritchlin, E.M. Schwarz, and H. Rahimi. 2019. Reinterpreting evidence of rheumatoid arthritis-associated interstitial lung disease to understand etiology. Current Rheumatology Reviews 15 (4): 277–289. https://doi.org/10.2174/1573397115666190116102451.
Raghu, G., M. Remy-Jardin, J.L. Myers, L. Richeldi, C.J. Ryerson, D.J. Lederer, et al. 2018. Diagnosis of idiopathic pulmonary fibrosis. an official ATS/ERS/JRS/ALAT clinical practice guideline. American Journal of Respiratory and Critical Care Medicine 198: e44–e68. https://doi.org/10.1164/rccm.201807-1255ST.
Juge, P.A., B. Crestani, and P. Dieudé. 2020. Recent advances in rheumatoid arthritis-associated interstitial lung disease. Current Opinion in Pulmonary Medicine 26 (5): 477–486. https://doi.org/10.1097/MCP.0000000000000710.
Atienza-Mateo, B., S. Remuzgo-Martínez, V.M. Mora-Cuesta, D. Iturbe-Fernández, S. Fernández-Rozas, D. Prieto-Peña, et al. 2020. The spectrum of interstitial lung disease associated with autoimmune diseases: data of a 3.6-year prospective study from a referral center of interstitial lung disease and lung transplantation. Journal of Clinical Medicine. 9: 1606. https://doi.org/10.3390/jcm9061606.
Matson, S., J. Lee, and O. Eickelberg. 2021. Two sides of the same coin? A review of the similarities and differences between idiopathic pulmonary fibrosis and rheumatoid arthritis-associated interstitial lung disease. European Respiratory Journal 57 (5): 2002533. https://doi.org/10.1183/13993003.02533-2020.
Yuan, Z.C., W.D. Xu, X.Y. Liu, X.Y. Liu, A.F. Huang, and L.C. Su. 2019. Biology of IL-36 signaling and its role in systemic inflammatory diseases. Frontiers in Immunology 10: 2532. https://doi.org/10.3389/fimmu.2019.02532.
Bassoy, E.Y., J.E. Towne, and C. Gabay. 2018. Regulation and function of interleukin-36 cytokines. Immunological Reviews 281 (1): 169–178. https://doi.org/10.1111/imr.12610.
Dinarello, C.A. 2019. The IL-1 family of cytokines and receptors in rheumatic diseases. Nature Reviews Rheumatology 15 (10): 612–632. https://doi.org/10.1038/s41584-019-0277-8.
Frey, S., A. Derer, M.E. Messbacher, D.L. Baeten, S. Bugatti, C. Montecucco, et al. 2013. The novel cytokine interleukin-36α is expressed in psoriatic and rheumatoid arthritis synovium. Annals of the Rheumatic Diseases 72 (9): 1569–1574. https://doi.org/10.1136/annrheumdis-2012-202264.
Magne, D., G. Palmer, J.L. Barton, F. Mézin, D. Talabot-Ayer, S. Bas, et al. 2006. The new IL-1 family member IL-1F8 stimulates production of inflammatory mediators by synovial fibroblasts and articular chondrocytes. Arthritis Research & Therapy 8 (3): R80. https://doi.org/10.1186/ar1946.
Melton, E., and H.Y. Qiu. 2020. Interleukin-36 cytokine/receptor signaling: A new target for tissue fibrosis. International Journal of Molecular Sciences 21 (18): 6458. https://doi.org/10.3390/ijms21186458.
Elias, M., S. Zhao, H.T. Le, J. Wang, M.F. Neurath, C. Neufert, et al. 2021. IL-36 in chronic inflammation and fibrosis - bridging the gap? The Journal of Clinical Investigation 131 (2): e144336. https://doi.org/10.1172/JCI144336.
Zhang, Q., L. Guo, X. Song, C. Lv, P. Tang, Y. Li, et al. 2022. Serum IL-36 cytokines levels in idiopathic pulmonary fibrosis and connective tissue disease-associated interstitial lung diseases. Clinica Chimica Acta 530: 8–12. https://doi.org/10.1016/j.cca.2022.02.015.
Aletaha, D., T. Neogi, A.J. Silman, J. Funovits, D.T. Felson, C.O. Bingham, et al. 2010. 2010 Rheumatoid arthritis classification criteria: An American College of Rheumatology/European League Against Rheumatism collaborative initiative. Arthritis and Rheumatism 62 (9): 2569–2581. https://doi.org/10.1002/art.27584.
Boutet, M.A., G. Bart, M. Penhoat, J. Amiaud, B. Brulin, C. Charrier, et al. 2016. Distinct expression of interleukin (IL)-36α, β and γ, their antagonist IL-36Ra and IL-38 in psoriasis, rheumatoid arthritis and Crohn’s disease. Clinical and Experimental Immunology 184 (2): 159–173. https://doi.org/10.1111/cei.12761.
Wang, X.R., J.P. Xiao, and D.G. Wang. 2021. Elevated levels of serum IL-36α in patients with systemic lupus erythematosus. Biomed Rep. 15 (3): 76. https://doi.org/10.3892/br.2021.1452.
Peñaloza, H.F., R. Geest, and V-D., Ybe J. A., Standiford T. J., Lee J. S. 2021. Interleukin-36 cytokines in infectious and non-infectious lung diseases. Frontiers in Immunology 12: 754702. https://doi.org/10.3389/fimmu.2021.754702.
Antoniou, K.M., G.A. Margaritopoulos, S. Tomassetti, F. Bonella, U. Costabel, and V. Poletti. 2014. Interstitial lung disease. European Respiratory Reviews 23 (131): 40–54. https://doi.org/10.1183/09059180.00009113.
Spagnolo, P., O. Distler, C.J. Ryerson, A. Tzouvelekis, J.S. Lee, F. Bonella, et al. 2021. Mechanisms of progressive fibrosis in connective tissue disease (CTD)-associated interstitial lung diseases (ILDs). Annals of the Rheumatic Diseases 80 (2): 143–150. https://doi.org/10.1136/annrheumdis-2020-217230.
England, B.R., and D. Hershberger. 2020. Management issues in rheumatoid arthritis-associated interstitial lung disease. Current Opinion in Rheumatology 32 (3): 255–263. https://doi.org/10.1097/BOR.0000000000000703.
Nurmi, H.M., M.K. Purokivi, M.S. Karkkainen, H.P. Kettunen, T.A. Selander, and R.L. Kaarteenaho. 2016. Variable course of disease of rheumatoid arthritis-associated usual interstitial pneumonia compared to other subtypes. BMC Pulmonary Medicine 16 (1): 107. https://doi.org/10.1186/s12890-016-0269-2.
Singh, N., J. Varghese, B.R. England, J.J. Solomon, K. Michaud, T.R. Mikuls, et al. 2019. Impact of the pattern of interstitial lung disease on mortality in rheumatoid arthritis: A systematic literature review and meta-analysis. Seminars in Arthritis and Rheumatism 49 (3): 358–365. https://doi.org/10.1016/j.semarthrit.2019.04.005.
Funding
The work was supported by funds from the National Natural Science Foundation of China (Grant Nos. 82070062 and 81870057), the Natural Science Foundation of Hubei Province (Grant No. 2020CFA018), the Climbing Project for Medical Talent of Zhongnan Hospital, Wuhan University (Grant No. PDJH202205), and the Science, Technology and Innovation Seed Fund of Zhongnan Hospital of Wuhan University (Grant No: znpy2019052).
Author information
Authors and Affiliations
Contributions
Yuan Liu, Xiaoqi Chen, and Zhenshun Cheng contributed to the study conception and design. Data and sample collection was performed by Weishuai Zheng, Xingxing Hu, Menglin Zou, Nie Hu, Weiwei Song, Rui Wang, Ying Liu, and Qinhui Hou. The preparation of material, experiment operation, and data analysis were performed by Weishuai Zheng, Xingxing Hu, and Menglin Zou. The first draft of the manuscript was written by Weishuai Zheng, and all authors commented on previous versions of the manuscript. Weishuai Zheng, Xingxing Hu, and Menglin Zou contributed equally to this work and share first authorship. Yuan Liu, Xiaoqi Chen, and Zhenshun Cheng contributed equally to this work. The authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics Approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval for the study was granted by the Medical Ethics Committee of Zhongnan Hospital of Wuhan University.
Consent to Participate
Informed consent was obtained from all individual participants included in the study.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zheng, W., Hu, X., Zou, M. et al. Plasma IL-36α and IL-36γ as Potential Biomarkers in Interstitial Lung Disease Associated with Rheumatoid Arthritis: a Pilot Study in the Chinese Population. Inflammation 46, 285–296 (2023). https://doi.org/10.1007/s10753-022-01733-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-022-01733-x