Abstract
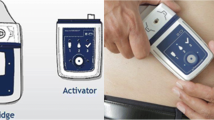
The prevalence of heart failure (HF) continues to rise in developed nations. Symptomatic congestion is the most common reason for patients to seek medical attention, and management often requires intravenous (IV) diuretic administration in the hospital setting. Typically, the number of admissions increases as the disease progresses, not only impacting patient survival and quality of life but also driving up healthcare expenditures. pH-neutral furosemide delivered subcutaneously using a proprietary, single-use infusor system (Furoscix) has a tremendous potential to transition in-hospital decongestive therapy to the outpatient setting or to the patient’s home. This review is aimed at providing an overview of the pharmacodynamic and pharmacokinetic profile of the novel pH-neutral furosemide in addition to the most recent clinical trials demonstrating its benefit when used in the home setting. Given the newest data and approval by the Food and Drug Administration in the US, it has the potential to revolutionize the care of patients with decompensated HF. Undoubtedly, it will lead to improved quality of life as well as significantly reduced healthcare costs related to hospital admissions.

Similar content being viewed by others
Availability of data and materials
All data used to prepare this manuscript are available online.
Abbreviations
- HF:
-
Heart failure
- ADHF:
-
Acute decompensated heart failure
- ED:
-
Emergency department
- CVD:
-
Cardiovascular disease
- ECF:
-
Extracellular fluid
- IV:
-
Intravenous
- SC:
-
Subcutaneous
- NYHA:
-
New York Heart Association
- KCCQ-12:
-
Kansas City Cardiomyopathy Questionnaire
References
Bozkurt B, Coats AJ, Tsutsui H, Abdelhamid M, Adamopoulos S, Albert N et al (2021) Universal definition and classification of heart failure. J Card Fail 27:387–413. https://doi.org/10.1016/j.cardfail.2021.01.022
Benjamin EJ, Blaha MJ, Chiuve SE, Cushman M, Das SR, Deo R et al (2017) Heart Disease and Stroke Statistics Update: a report from the American Heart Association. Circ 135. https://doi.org/10.1161/CIR.0000000000000485
Tsao CW, Aday AW, Almarzooq ZI, Alonso A, Beaton AZ, Bittencourt MS et al (2022) Heart Disease and Stroke Statistics Update: a report from the American Heart Association. Circ 145. https://doi.org/10.1161/CIR.0000000000001052
Zilberberg MD, Nathanson BH, Sulham K, Mohr JF, Goodwin MM, Shorr AF (2023) Descriptive epidemiology and outcomes of patients with short stay hospitalizations for the treatment of congestive heart failure in the US. Clin Outcomes Res 15:139–149. https://doi.org/10.2147/CEOR.S400882
Khan MS, Sreenivasan J, Lateef N, Abougergi MS, Greene SJ, Ahmad T et al (2021) Trends in 30- and 90-day readmission rates for heart failure. Circ Heart Fail 14. https://doi.org/10.1161/CIRCHEARTFAILURE.121.008335
Urbich M, Globe G, Pantiri K, Heisen M, Bennison C, Wirtz HS et al (2020) A systematic review of medical costs associated with heart failure in the USA (2014–2020). Pharmacoeconomics 38:1219–1236. https://doi.org/10.1007/s40273-020-00952-0
Lin AH, Chin JC, Sicignano NM, Evans AM (2017) Repeat Hospitalizations Predict Mortality in Patients With Heart Failure. Mil Med 182:e1932–e1937. https://doi.org/10.7205/MILMED-D-17-00017
Lee DS, Austin PC, Stukel TA, Alter DA, Chong A, Parker JD et al (2009) “Dose-dependent” impact of recurrent cardiac events on mortality in patients with heart failure. Am J Med 122:162.e1-162.e9. https://doi.org/10.1016/j.amjmed.2008.08.026
Setoguchi S, Stevenson LW, Schneeweiss S (2007) Repeated hospitalizations predict mortality in the community population with heart failure. Am Heart J 154:260–266. https://doi.org/10.1016/j.ahj.2007.01.041
Lewis EF, Li Y, Pfeffer MA, Solomon SD, Weinfurt KP, Velazquez EJ et al (2014) Impact of cardiovascular events on change in quality of life and utilities in patients after myocardial infarction. JACC Heart Fail 2:159–165. https://doi.org/10.1016/j.jchf.2013.12.003
Albuquerque de Almeida F, Al MJ, Koymans R, Riistama J, Pauws S, Severens JL (2020) Impact of hospitalisation on health-related quality of life in patients with chronic heart failure. Health Qual Life Outcomes 18:262. https://doi.org/10.1186/s12955-020-01508-8
Whittingham K, Barnes S, Gardiner C (2013) Tools to measure quality of life and carer burden in informal carers of heart failure patients: a narrative review. Palliat Med 27:596–607. https://doi.org/10.1177/0269216313477179
Malik FA, Gysels M, Higginson IJ (2013) Living with breathlessness: a survey of caregivers of breathless patients with lung cancer or heart failure. Palliat Med 27:647–656. https://doi.org/10.1177/0269216313488812
Jha AK, Ojha CP, Krishnan AM, Paul TK (2022) 30-day readmission in patients with heart failure with preserved ejection fraction: insights from the nationwide readmission database. World J Cardiol 14:473–482. https://doi.org/10.4330/wjc.v14.i9.473
Giles L, Freeman C, Field P, Sörstadius E, Kartman B (2020) Humanistic burden and economic impact of heart failure – a systematic review of the literature. F1000Res 8:859. https://doi.org/10.12688/f1000research.19365.2
Harjola V-P, Mullens W, Banaszewski M, Bauersachs J, Brunner-La Rocca H-P, Chioncel O et al (2017) Organ dysfunction, injury and failure in acute heart failure: from pathophysiology to diagnosis and management. A review on behalf of the Acute Heart Failure Committee of the Heart Failure Association (HFA) of the European Society of Cardiology (ESC). Eur J Heart Fail 19:821–36. https://doi.org/10.1002/ejhf.872
Patel H, Shafazand M, Schaufelberger M, Ekman I (2007) Reasons for seeking acute care in chronic heart failure. Eur J Heart Fail 9:702–708. https://doi.org/10.1016/j.ejheart.2006.11.002
Lip G, Zarifis J, Beevers DG (1997) Acute admissions with heart failure to a district general hospital serving a multiracial population. Int J Clin Pract 51:223–227
Jurgens CY, Lee CS, Aycock DM, Masterson Creber R, Denfeld QE, DeVon HA et al (2022) State of the science: the relevance of symptoms in cardiovascular disease and research: a scientific statement from the American Heart Association. Circulation 146. https://doi.org/10.1161/CIR.0000000000001089
Adamson PB (2009) Pathophysiology of the transition from chronic compensated and acute decompensated heart failure: new insights from continuous monitoring devices. Curr Heart Fail Rep 6:287–292. https://doi.org/10.1007/s11897-009-0039-z
Faragli A, Abawi D, Quinn C, Cvetkovic M, Schlabs T, Tahirovic E et al (2021) The role of non-invasive devices for the telemonitoring of heart failure patients. Heart Fail Rev 26:1063–1080. https://doi.org/10.1007/s10741-020-09963-7
Ferrante D, Varini S, Macchia A, Soifer S, Badra R, Nul D et al (2010) Long-term results after a telephone intervention in chronic heart failure. J Am Coll Cardiol 56:372–378. https://doi.org/10.1016/j.jacc.2010.03.049
Koehler F, Winkler S, Schieber M, Sechtem U, Stangl K, Böhm M et al (2011) Impact of remote telemedical management on mortality and hospitalizations in ambulatory patients with chronic heart failure. Circ 123:1873–1880. https://doi.org/10.1161/CIRCULATIONAHA.111.018473
Ong MK, Romano PS, Edgington S, Aronow HU, Auerbach AD, Black JT et al (2016) Effectiveness of remote patient monitoring after discharge of hospitalized patients with heart failure. JAMA Intern Med 176:310. https://doi.org/10.1001/jamainternmed.2015.7712
Angermann CE, Störk S, Gelbrich G, Faller H, Jahns R, Frantz S et al (2012) Mode of action and effects of standardized collaborative disease management on mortality and morbidity in patients with systolic heart failure. Circ Heart Fail 5:25–35. https://doi.org/10.1161/CIRCHEARTFAILURE.111.962969
Morgan JM, Kitt S, Gill J, McComb JM, Ng GA, Raftery J et al (2017) Remote management of heart failure using implantable electronic devices. Eur Heart J 38:2352–2360. https://doi.org/10.1093/eurheartj/ehx227
Chaudhry SI, Mattera JA, Curtis JP, Spertus JA, Herrin J, Lin Z et al (2010) Telemonitoring in patients with heart failure. N Engl J Med 363:2301–2309. https://doi.org/10.1056/NEJMoa1010029
Koehler F, Koehler K, Deckwart O, Prescher S, Wegscheider K, Winkler S et al (2018) Telemedical Interventional Management in Heart Failure II (TIM-HF2), a randomised, controlled trial investigating the impact of telemedicine on unplanned cardiovascular hospitalisations and mortality in heart failure patients: study design and description. Eur J Heart Fail 20:1485–1493. https://doi.org/10.1002/ejhf.1300
van Veldhuisen DJ, Braunschweig F, Conraads V, Ford I, Cowie MR, Jondeau G et al (2011) Intrathoracic impedance monitoring, audible patient alerts, and outcome in patients with heart failure. Circ 124:1719–1726. https://doi.org/10.1161/CIRCULATIONAHA.111.043042
Abraham WT, Perl L (2017) Implantable hemodynamic monitoring for heart failure patients. J Am Coll Cardiol 70:389–398. https://doi.org/10.1016/j.jacc.2017.05.052
Adamson PB, Abraham WT, Stevenson LW, Desai AS, Lindenfeld J, Bourge RC et al (2016) Pulmonary artery pressure–guided heart failure management reduces 30-day readmissions. Circ Heart Fail 9. https://doi.org/10.1161/CIRCHEARTFAILURE.115.002600
Abraham WT, Stevenson LW, Bourge RC, Lindenfeld JA, Bauman JG, Adamson PB (2016) Sustained efficacy of pulmonary artery pressure to guide adjustment of chronic heart failure therapy: complete follow-up results from the CHAMPION randomised trial. The Lancet 387:453–461. https://doi.org/10.1016/S0140-6736(15)00723-0
Vasko MR (1985) Furosemide absorption altered in decompensated congestive heart failure. Ann Intern Med 102:314. https://doi.org/10.7326/0003-4819-102-3-314
Gottlieb SS, Khatta M, Wentworth D, Roffman D, Fisher ML, Kramer WG (1998) The effects of diuresis on the pharmacokinetics of the loop diuretics furosemide and torsemide in patients with heart failure. Am J Med 104:533–538. https://doi.org/10.1016/S0002-9343(98)00111-9
McDonagh TA, Metra M, Adamo M, Gardner RS, Baumbach A, Böhm M et al (2022) 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur J Heart Fail 24:4–131. https://doi.org/10.1002/ejhf.2333
Mentz RJ, Anstrom KJ, Eisenstein EL, Sapp S, Greene SJ, Morgan S et al (2023) Effect of torsemide vs furosemide after discharge on all-cause mortality in patients hospitalized with heart failure. JAMA 329:214. https://doi.org/10.1001/jama.2022.23924
Ellison DH (2019) Clinical pharmacology in diuretic use. Clin J Am Soc Nephrol 14:1248–1257. https://doi.org/10.2215/CJN.09630818
Carone L, Oxberry SG, Twycross R, Charlesworth S, Mihalyo M, Wilcock A (2016) Furosemide. J Pain Symptom Manage 52:144–150. https://doi.org/10.1016/j.jpainsymman.2016.05.004
Mullens W, Damman K, Harjola V-P, Mebazaa A, Brunner-La Rocca H-P, Martens P et al (2019) The use of diuretics in heart failure with congestion - a position statement from the Heart Failure Association of the European Society of Cardiology. Eur J Heart Fail 21:137–155. https://doi.org/10.1002/ejhf.1369
Albert NM, Barnason S, Deswal A, Hernandez A, Kociol R, Lee E et al (2015) Transitions of care in heart failure. Circ Heart Fail 8:384–409. https://doi.org/10.1161/HHF.0000000000000006
Ryder M, Murphy NF, McCaffrey D, O’Loughlin C, Ledwidge M, McDonald K (2008) Outpatient intravenous diuretic therapy; potential for marked reduction in hospitalisations for acute decompensated heart failure. Eur J Heart Fail 10:267–272. https://doi.org/10.1016/j.ejheart.2008.01.003
Makadia S, Simmons T, Augustine S, Kovell L, Harris C, Chibungu A et al (2015) The diuresis clinic: a new paradigm for the treatment of mild decompensated heart failure. Am J Med 128:527–531. https://doi.org/10.1016/j.amjmed.2014.11.028
Buckley LF, Carter DM, Matta L, Cheng JW, Stevens C, Belenkiy RM et al (2016) Intravenous diuretic therapy for the management of heart failure and volume overload in a multidisciplinary outpatient unit. JACC Heart Fail 4:1–8. https://doi.org/10.1016/j.jchf.2015.06.017
Wierda E, Dickhoff C, Handoko ML, Oosterom L, Kok WE, Rover Y et al (2020) Outpatient treatment of worsening heart failure with intravenous and subcutaneous diuretics: a systematic review of the literature. ESC Heart Fail 7:892–902. https://doi.org/10.1002/ehf2.12677
Dahiya G, Bensimhon D, Goodwin MM, Mohr JF, Alexy T (2022) From oral to subcutaneous furosemide: the road to novel opportunities to manage congestion. Struct Heart 6:100076. https://doi.org/10.1016/j.shj.2022.100076
Quach C, McArthur M, McGeer A, Li L, Simor A, Dionne M et al (2012) Risk of infection following a visit to the emergency department: a cohort study. Can Med Assoc J 184:E232–E239. https://doi.org/10.1503/cmaj.110372
Lindsey BB, Villabona-Arenas ChJ, Campbell F, Keeley AJ, Parker MD, Shah DR et al (2022) Characterising within-hospital SARS-CoV-2 transmission events using epidemiological and viral genomic data across two pandemic waves. Nat Commun 13:671. https://doi.org/10.1038/s41467-022-28291-y
Verma AK, da Silva JH, Kuhl DR (2004) Diuretic effects of subcutaneous furosemide in human volunteers: a randomized pilot study. Ann Pharmacother 38:544–549. https://doi.org/10.1345/aph.1D332
Zacharias H, Raw J, Nunn A, Parsons S, Johnson M (2011) Is there a role for subcutaneous furosemide in the community and hospice management of end-stage heart failure? Palliat Med 25:658–663. https://doi.org/10.1177/0269216311399490
Galindo-Ocaña J, Romero-Mena J, Castillo-Ferrando JR, Aguilera-González C, Bernabeu-Wittel M, Ollero-Baturone M (2013) Subcutaneous furosemide as palliative treatment in patients with advanced and terminal-phase heart failure. BMJ Support Palliat Care 3:7–9. https://doi.org/10.1136/bmjspcare-2012-000296
Picazo Sánchez M, Castillo Lorenzo MN, Cuxart Pérez M, Sans LR (2018) Uso paliativo de la furosemida en infusión continua subcutánea en un paciente trasplantado renal con fallo cardíaco. Nefrologia 38:438–439. https://doi.org/10.1016/j.nefro.2017.09.001
Zatarain-Nicolás E, López-Díaz J, de la Fuente-Galán L, García-Pardo H, Recio-Platero A, San Román-Calvar JA (2013) Subcutaneous infusion of furosemide administered by elastomeric pumps for decompensated heart failure treatment: initial experience. Revista Española de Cardiología (English Edition) 66:1002–1004. https://doi.org/10.1016/j.rec.2013.06.008
Sica DA, Muntendam P, Myers RL, ter Maaten JM, Sale ME, de Boer RA et al (2018) Subcutaneous furosemide in heart failure. JACC Basic Transl Sci 3:25–34. https://doi.org/10.1016/j.jacbts.2017.10.001
Felker GM, Redfield MM, Mentz RJ, Dunlap ME, Lewis GD, Smith AL et al (2019) Subcutaneous furosemide in the treatment of patients with decompensated heart failure: data from the sub-Q pilot studies. J Card Fail 25:S75. https://doi.org/10.1016/j.cardfail.2019.07.213
Gilotra NA, Princewill O, Marino B, Okwuosa IS, Chasler J, Almansa J et al (2018) Efficacy of intravenous furosemide versus a novel, pH-neutral furosemide formulation administered subcutaneously in outpatients with worsening heart failure. JACC Heart Fail 6:65–70. https://doi.org/10.1016/j.jchf.2017.10.001
Furoscix Real-World Evaluation for Decreasing Hospital Admissions in Heart Failure (FREEDOM-HF) https://beta.clinicaltrials.gov/study/NCT03458325?tab=results. Published November 7, 2022. Accessed 29 Jan 2023
Avoiding Treatment in Hospital with FUROSCIX to Manage Congestion in Heart Failure (AT HOME-HF) – a pilot study. https://scpharmaceuticalsinc.gcs-web.com/news-releases/news-release-details/scpharmaceuticals-announces-data-presentations-heart-failure. Published September 30, 2022. Accessed 29 Jan 2023
Author information
Authors and Affiliations
Contributions
WJK, JA, MSM, and RH participated in writing various sections of the manuscript. DB, KT, and TA wrote portions of the paper, edited and integrated the sections, and reviewed the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
Not applicable to the manuscript.
Competing interests
DB and TA serve on the speakers’ bureau and as consultants for scPharmaceuticals. TA is also on the speakers’ bureau for Abbott, Inc. All other authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Khan, W.J., Arriola-Montenegro, J., Mutschler, M.S. et al. A novel opportunity to improve heart failure care: focusing on subcutaneous furosemide. Heart Fail Rev 28, 1315–1323 (2023). https://doi.org/10.1007/s10741-023-10331-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10741-023-10331-4