Abstract
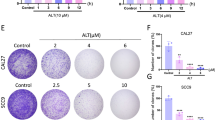
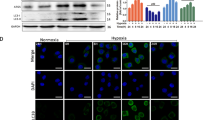
Hypoxia is a key trigger in the transformation of oral leukoplakia into oral cancer. However, it is still too early to determine the role of hypoxia in the development of oral leukoplakia. Prx1, an antioxidant protein, upregulated by hypoxia, regulates cellular autophagy in leukoplakia. This study aimed to understand the mechanisms by which hypoxia induces Prx1 expression during autophagy in oral leukoplakia. We used an experimental model of tongue epithelial hyperplasia induced by 4-nitroquinoline-1-oxide (4NQO) and dysplastic oral keratinocytes. Prx1 knockdown DOK cells, Leuk-1 cells and control cells were harvested, and cell proliferation was assayed using the Cell Counting Kit-8. Several hypoxia and autophagy-related proteins were examined using quantitative real-time polymerase chain reaction, immunohistochemistry, immunofluorescence, and western blotting in cells and mouse tongue tissues. In addition, the ultrastructure of the cells was observed by transmission electron microscopy. Hypoxia induces cell proliferation, autophagic vesicles and the expression of Prx1, BNIP3, LC3II/I and Beclin-1 in DOK and Leuk-1 cells. However, these effects were all attenuated by Prx1 knockdown. Histologically, 4NQO induced epithelial hyperplasia in the tongue mucosa. The expression of proliferation marker PCNA, autophagy-related proteins LC3B and Beclin-1, as well as HIF-1α/BNIP3 was significantly lower in the tongue tissues of Prx1flox/flox:Cre+ mice compared with Prx1flox/flox mice. In Prx1flox/flox:Cre+ mice, an increased expression of HIF-1α/BNIP3, LC3B and Beclin-1 was detected in epithelial hyperplasia tongue tissues compared to normal tissues. The current study suggests that Prx1 may promotes cell proliferation and autophagy in oral leukoplakia cells via the HIF-1α/BNIP3 pathway.





Similar content being viewed by others
References
Bhandari V et al (2019) Molecular landmarks of tumor hypoxia across cancer types. Nat Genet 51(2):308–318
Cai X et al (2023) Development of a Pathomics-Based Model for the Prediction of Malignant Transformation in Oral Leukoplakia. Lab Invest 103(8):100173
Delgado JM et al (2023) The ER membrane protein complex governs lysosomal turnover of a mitochondrial tail-anchored protein, BNIP3, to restrict mitophagy. bioRxiv 17(1):10
Fan T et al (2022) NUPR1 promotes the proliferation and metastasis of oral squamous cell carcinoma cells by activating TFE3-dependent autophagy. Signal Transduct Target Ther 7(1):130
Galluzzi L et al (2017) Molecular definitions of autophagy and related processes. EMBO J 36(13):1811–1836
Gao L et al (2019) CircCDR1as upregulates autophagy under hypoxia to promote tumor cell survival via AKT/ERK(1/2)/mTOR signaling pathways in oral squamous cell carcinomas. Cell Death Dis 10(10):745
Jawad SF et al (2023) The strict regulation of HIF-1α by non-coding RNAs: new insight towards proliferation, metastasis, and therapeutic resistance strategies. Cancer Metastasis Rev 43(1):5–27
Jiang Y et al (2019) LncRNA LINC00460 promotes EMT in head and neck squamous cell carcinoma by facilitating peroxiredoxin-1 into the nucleus. J Exp Clin Cancer Res 38(1):365
Jing X et al (2019) Role of hypoxia in cancer therapy by regulating the tumor microenvironment. Mol Cancer 18(1):157
Joseph JP et al (2018) Hypoxia induced EMT: A review on the mechanism of tumor progression and metastasis in OSCC. Oral Oncol 80:23–32
Kim Y-J et al (2007) Human prx1 Gene Is a Target of Nrf2 and Is Up-regulated by Hypoxia/Reoxygenation: Implication to Tumor Biology. Can Res 67(2):546–554
Klopotowska M et al (2022) PRDX-1 Supports the Survival and Antitumor Activity of Primary and CAR-Modified NK Cells under Oxidative Stress. Cancer Immunol Res 10(2):228–244
Kothari S et al (2003) BNIP3 plays a role in hypoxic cell death in human epithelial cells that is inhibited by growth factors EGF and IGF. Oncogene 22(30):4734–4744
Kujan O, Shearston K, Farah CS (2017) The role of hypoxia in oral cancer and potentially malignant disorders: a review. J Oral Pathol Med 46(4):246–252
Kujan O et al (2023) Automated immunohistochemical quantification of hypoxia biomarkers shows correlation with dysplastic epithelial changes. J Oral Pathol Med 52(6):504–513
Lee LT et al (2018) The correlation between HIF-1 alpha and VEGF in oral squamous cell carcinomas: Expression patterns and quantitative immunohistochemical analysis. J Chin Med Assoc 81(4):370–375
Li M et al (2022) Transition of autophagy and apoptosis in fibroblasts depends on dominant expression of HIF-1α or p53. J Zhejiang Univ Sci B 23(3):204–217
Liao W et al (2023) CircZNF215 promotes tumor growth and metastasis through inactivation of the PTEN/AKT pathway in intrahepatic cholangiocarcinoma. J Exp Clin Cancer Res 42(1):125
Liu Y et al (2023) Hypoxia-induced GPCPD1 depalmitoylation triggers mitophagy via regulating PRKN-mediated ubiquitination of VDAC1. Autophagy 19(9):2443–2463
Lu Y et al (2021) Peroxiredoxin1 Knockdown Inhibits Oral Carcinogenesis via Inducing Cell Senescence Dependent on Mitophagy. Onco Targets Ther 14:239–251
Mellor HR, Harris AL (2007) The role of the hypoxia-inducible BH3-only proteins BNIP3 and BNIP3L in cancer. Cancer Metastasis Rev 26(3–4):553–566
Moretton A et al (2023) A metabolic map of the DNA damage response identifies PRDX1 in the control of nuclear ROS scavenging and aspartate availability. Mol Syst Biol 19(7):e11267
Normando AGC et al (2023) A meta-analysis reveals the protein profile associated with malignant transformation of oral leukoplakia. Front Oral Health 4:1088022
Riddell JR et al (2012) Peroxiredoxin 1 stimulates endothelial cell expression of VEGF via TLR4 dependent activation of HIF-1α. PLoS ONE 7(11):e50394
Semenza GL (2010) HIF-1: upstream and downstream of cancer metabolism. Curr Opin Genet Dev 20(1):51–56
Shang Q et al (2023) SNAI2 promotes the malignant transformation of oral leukoplakia by modulating p-EMT. Oral Dis n/a(n/a)
Shen Y et al (2021) Establishment and Validation of a Comprehensive Prognostic Model for Patients With HNSCC Metastasis. Front Genet 12:685104
Shi Y et al (2022) Manganese suppresses the development of oral leukoplakia by activating the immune response. Oral Dis 30(2):462–476
Sumera S et al (2023) Overexpression of Hypoxia-Inducible Factor-1α and Its Relation with Aggressiveness and Grade of Oral Squamous Cell Carcinoma. Diagn (Basel) 13:3
Swartz JE et al (2021) HIF-1a expression and differential effects on survival in patients with oral cavity, larynx, and oropharynx squamous cell carcinomas. Head Neck 43(3):745–756
Togo M et al (2020) Diagnostic value of (18)F-FDG-PET to predict the tumour immune status defined by tumoural PD-L1 and CD8(+)tumour-infiltrating lymphocytes in oral squamous cell carcinoma. Br J Cancer 122(11):1686–1694
Wang C et al (2017) Nicotine suppresses apoptosis by regulating α7nAChR/Prx1 axis in oral precancerous lesions. Oncotarget 8(43):75065–75075
Wang Y et al (2018) Peroxiredoxin 1 (PRDX1) Suppresses Progressions and Metastasis of Osteosarcoma and Fibrosarcoma of Bone. Med Sci Monit 24:4113–4120
Wang W et al (2022) Peroxiredoxin 1 inhibits autophagy through interacting with Rab7 in human dysplastic oral keratinocyte cells. Arch Oral Biol 141:105491
Wang M et al (2023) L3MBTL3 is induced by HIF-1α and fine tunes the HIF-1α degradation under hypoxia in vitro. Heliyon 9(2):e13222
Wu L et al (2023) Hypoxia derived exosomes promote the proliferation and metastasis of colorectal cancer through the regulation of HIF-1α/miR-4299/ZBTB4. Life Sci 329:121872
Yu P et al (2021) Claudin-5 Affects Endothelial Autophagy in Response to Early Hypoxia. Front Physiol 12:737474
Zhang M et al (2014) Induction of peroxiredoxin 1 by hypoxia regulates heme oxygenase-1 via NF-κB in oral cancer. PLoS ONE 9(8):e105994
Zhang Y et al (2023) UHRF2 promotes the malignancy of hepatocellular carcinoma by PARP1 mediated autophagy. Cell Signal 109:110782
Zhang Y et al (2024) Autophagy-related lncRNAs in tumor progression and drug resistance: A double-edged sword. Genes Dis 11(1):367–381
Acknowledgements
This research was funded by National Natural Science Foundation of China (82071114).
Author information
Authors and Affiliations
Contributions
Conceptualization, Data curation and Formal analysis, Tang Xiaofei, Zhang Min and Li Jing; Funding acquisition, Zhang Min; Methodology, Li Jing, Li Wenjing, Li Lingyu and Wang Wenchao; Project administration, Zhang Min and Tang Xiaofei; Supervision, Zhang Min; Writing – review & editing, Zhang Min and Tang Xiaofei.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Conflict of interest
The authors declare that there is no conflict of interest regarding the publication of this paper.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, J., Li, W., Li, L. et al. Induction of Peroxiredoxin 1 by Hypoxia Promotes Cellular Autophagy and Cell Proliferation in Oral Leukoplakia via HIF-1α/BNIP3 Pathway. J Mol Histol (2024). https://doi.org/10.1007/s10735-024-10197-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10735-024-10197-2