Abstract
Previous case–control studies have suggested a possible increased risk of Amyotrophic Lateral Sclerosis (ALS) with physical activity (PA), but this association has never been studied in prospective cohort studies. We therefore assessed the association between PA and risk of death from ALS in the European Prospective Investigation into Cancer and Nutrition. A total of 472,100 individuals were included in the analysis, yielding 219 ALS deaths. At recruitment, information on PA was collected thorough standardised questionnaires. Total PA was expressed by the Cambridge Physical Activity Index (CPAI) and analysed in relation to ALS mortality, using Cox hazard models. Interactions with age, sex, and anthropometric measures were assessed. Total PA was weakly inversely associated with ALS mortality with a borderline statistically significant trend across categories (p = 0.042), with those physically active being 33 % less likely to die from ALS compared to those inactive: HR = 0.67 (95 % CI 0.42–1.06). Anthropometric measures, sex, and age did not modify the association with CPAI. The present study shows a slightly decreased—not increased like in case–control studies—risk of dying from ALS in those with high levels of total PA at enrolment. This association does not appear confounded by age, gender, anthropometry, smoking, and education. Ours was the first prospective cohort study on ALS and physical activity.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Amyotrophic Lateral Sclerosis (ALS) is a progressive motor disease characterised by degeneration of the upper and lower motor neurons, with a median survival of 3 years [1]. Cigarette smoking is the only environmental factor which has been shown to increase the risk for this disease in case–control and cohort studies with solid design [2–5].
The observation that ALS incidence in Italy was increased among football players [6], recently reproduced in USA among American Football players [7], is consistent with the hypothesis, among others, that intense physical activity (PA) could be a risk factor for developing ALS. This hypothesis was firstly prompted by a US case–control study showing an increased risk of ALS among people who reported having participated in organised sports in high school [8]. It is supported by another small pilot case–control study from the USA showing an increased risk of ALS among those reporting more leisure-time PA, and those sweating while working [9]; by a more recent large population-based case–control study showing that leisure-time (but not occupational or vigorous) physical activity was associated with ALS (although there was not a clear dose–response relationship) [10]; and by a large population-based case–control study in Japan showing doubled risk of ALS among those practicing vigorous physical activity compared to physically inactive [11]. Conversely, a previous Dutch case–control study did not observe an association between PA and ALS: there was a younger age of symptom onset among those with a higher cumulative leisure PA [12]; although this was potentially explained by a birth cohort effect [13]. A very recent large case–control study found an inverse association between physical activity and ALS [14]. The main epidemiological observations to date on physical activity and ALS are summarised in Table 1.
Hypotheses other than that of an association between PA and ALS which are indicated by the evidence produced so far include: (1) that participating in sports (and not PA per se) can increase the risk of ALS (for example via repeated head or limb traumas, or ingestion of illicit substances enhancing sportive performance); or (2) that the age when physical activity is undertaken modifies the risk of ALS. On the other hand, being lean and athletic might be a phenotypic expression of genetic susceptibility to ALS; this might be supported by the finding that cardiovascular fitness was found to be associated with ALS in a record linkage study [21]. To our knowledge, the association between PA and risk of ALS has never been investigated in a prospective study.
In a recent report from the EPIC cohort, a lower body mass index (BMI) in men and a lower waist-to-hip ratio (WHR) in women were associated with an increased risk of dying from ALS [22]. Similar results of a decreased risk in both men and women with increased BMI were recently reported in five US cohorts [23]. To what extent this association is modified by PA has not been explored so far.
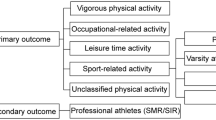
The aims of this study are to: (1) assess the association between total PA and risk of death from ALS in the European Prospective Investigation into Cancer and Nutrition (EPIC); (2) explore the contribution of other cumulative measures of PA (occupational, household, recreational, potentially traumatic, practising sports, and vigorous PA) on the risk of ALS; and (3) investigate to what extent these associations are confounded or modified by anthropometric measures or other factors (sex and age).
Methods
Participants
The EPIC study was approved by the ethical committee of the International Agency for Research on Cancer (IARC) and by the ethics committees of each participating centre; all participants signed an informed consent. Ninety-one percent of the 518,408 participants were aged 35–70 years and were recruited from the general population residing in defined geographical areas between 1992 and 2002, in 23 centres across 10 Western European countries (Norway, Sweden, Denmark, United Kingdom, Netherlands, Germany, France, Spain, Italy, and Greece) [24]. Exceptions were the French cohort (based on women members of the health insurance for state school), the Ragusa (Italy) cohort (based on blood donors and their spouses), the Utrecht (Netherlands) and Florence (Italy) cohorts (based on breast cancer screening participants), and part of the Oxford (UK) cohort (based on vegetarians and vegans) [24]. The Norway, France, Naples (Italy), and Utrecht cohorts were restricted to women.
At recruitment, information on lifestyle and dietary habits was collected through standardised questionnaires and anthropometric characteristics were measured. Follow-up for mortality and specific causes of death is carried out actively or through linkage with mortality registries at regional and national levels [24]. To date, follow-up is 98.5 % complete. The Norwegian EPIC sub-cohort (n = 37,185) was excluded from the present analysis because it did not give rise to any ALS cases, given its younger age composition.
Information on mortality and causes of death was collected independently: follow-up time was censored in case of dropout, loss of follow-up or fatal events other than ALS death (whichever occurred first). Each EPIC centre had a different last date of follow-up, based on when a drop in the number of reported causes of death was observed, for minimising false negatives [22]. This resulted in censoring follow-up time at some stage between June 2005 and June 2009, generating 5,815,773 person-years for 472,100 subjects after excluding 9123 (1.9 %) individuals with missing data on exposure or confounding variables.
Case ascertainment
ALS cases were defined as those subjects for whom “motor neuron disease” (G12.2 according to the 10th revision of the International Statistical Classification of Diseases, Injuries and Causes of Death) was reported as an immediate, antecedent or underlying cause of death (for more details, see [2]).
Physical activity assessment
The assessment of PA measures is described in detail elsewhere [24, 25]. In brief, participants replied to a questionnaire at baseline about occupational PA, and recreational PA, including duration and frequency of walking, cycling, gardening (average values in summer and winter), household work, do-it-yourself (DIY) activities, and sports during the previous year.
Total PA was investigated using the Cambridge Physical Activity Index (CPAI), which combines occupational PA (sedentary occupation, standing occupation, manual/heavy manual work) with time participating in sports and spent cycling [26]. The total hours per week spent cycling or participating in sports was categorised in four levels (no, ≤3.5 h/week; >3.5 and ≤7.0 h/week; >7.0 h/week); based on a 4 × 4 matrix, participants were then classified in four final categories: inactive (sedentary job, no leisure time PA); moderately inactive (standing occupation and no leisure time PA or sedentary occupation and ≤3.5 h/week of leisure time PA); moderately active (manual occupation and no leisure time PA, or standing occupation and ≤3.5 h/week of leisure time PA, or sedentary occupation and >3.5 but ≤7 h/week of leisure time PA): and active (sedentary job with >7 h/week of leisure time PA, or standing job and >3.5 h/week of leisure time PA, or manual job and any leisure time PA, or heavy manual job) [26]. The index was developed by comparing the EPIC PA questionnaire with objective measures of cardio-respiratory fitness and energy expenditure assessed by heart-rate monitoring with individual calibration (measures validated against gold standard techniques) [26], and recently revalidated against a brief questionnaire examining energy expenditure and time spent in moderate and vigorous physical activity [27].
Information on housework, DIY, gardening and climbing stairs was combined to estimate the overall amount of household activity. Recreational PA included walking, cycling, gardening, sports, and DIY. Potentially traumatic PA was defined as performing manual or heavy manual work, playing sport, or doing DIY. Duration and frequency were directly estimated, and intensity (i.e. energy expenditure) was estimated by assigning metabolic equivalents (METs), ranging from 3 for walking and household activities to 6 for sports [28]. Household and recreational PA were categorised in quartiles of distribution; playing sports was categorized as 0, <12 (below the median) or 12+ (above the median) MET-h/week; vigorous PA was categorized as 0, ≤2 (below the median), or >2 (above the median) h/week; potentially traumatic PA was classified as ever/never.
Statistical analysis
Cox proportional hazard models, with age as the main time variable were used to investigate the associations between type and amount of PA and ALS mortality. Hazard ratio (HR) estimates were derived for the entire sample, stratified by age and centre of recruitment. Potential confounders included sex, highest level of education attained (none/primary, technical, secondary, university, undetermined), a composite smoking variable (never smoker, former smoker ≥10 years prior to enrolment; former smoker <10 years prior to enrolment, current smoker 1–4 cigarettes/day; 5–14 cigarettes/day, 15–24 cigarettes/day, ≥25 cigarettes/day, undetermined), BMI in units (kg/m2) and WHR. This composite smoking variable best takes into account the complex pattern of smoking variables on ALS risk found in this cohort [22].
For each Cox regression analysis, a p value for linear trend across categories was calculated by introducing the ordinal variable in the model. The p value for interaction between each PA category and sex, age (<50 years and 50+ years), BMI, and WHR was estimated using the log-likelihood ratio test comparing models with and without the interaction term (allowance made for p < 0.100). To further explore to what extent anthropometric measures could act as confounders separate models were computed: (1) including and excluding them; and (2) stratified by BMI categories [under/normal weight (<25.0 kg/m2), overweight (25.0–29.9 kg/m2), and obese (≥ 30 kg/m2)] and WHR sex-specific quartiles. To explore the extent to which PA modifies the age of ALS onset, the analysis of each PA variable was repeated among those with an age of death from ALS <70 years (N = 120), and among those aged 70+ years (N = 102).
A sensitivity analysis was conducted with models excluding ALS cases arising during the first 3 years of follow-up in order to minimise the potential for reverse causation. Statistical significance was set at 5 % for two-tailed tests.
Results
The characteristics of the cohort participants by the CPAI are described in Table 2.
A total of 219 ALS deaths (76 men and 143 women) arose during follow-up, with the mean follow-up period being 13 years (SD 3 years). Men and younger people were more likely to be physically active; a moderate association between higher levels of PA and higher educational level, lower BMI, and less smoking was observed (Table 2).
Total PA as estimated by the CPAI was inversely associated with ALS mortality, with a statistically significant trend across categories (p = 0.042) in the fully adjusted model (Table 3). Introducing BMI into the model, the statistical significance of the linear trend was maintained (p = 0.032), and risk estimates were slightly strengthened (p value for the interaction with BMI = 0.318); replacing BMI with WHR, the risk estimates were slightly reduced as was the significance level of the linear trend (p = 0.084) (p value for the interaction with WHR = 0.889). Hazard ratio estimates by BMI categories and WHR quartiles are shown in Fig. 1.
HR and relative 95 % CI for categories of Cambridge Index of physical activity by BMI category (a) and quartiles of WHR (b). *p value for trend across categories p = 0.455; †
p value for trend across categories p = 0.101; ‡
p value for trend across categories p = 0.119. §
p value for trend across categories p = 0.340;  p value for trend across categories p = 0.588; ^
p value for trend across categories p = 0.410; ~
p value for trend across categories p = 0.296
p value for trend across categories p = 0.588; ^
p value for trend across categories p = 0.410; ~
p value for trend across categories p = 0.296
The association between CPAI and ALS mortality did not appear to be modified by gender (p interaction = 0.272) or age (p interaction = 0.875). When the main analysis was repeated after excluding those who were unemployed at recruitment (34.7 %) (and thus a priori classified as in a sedentary job occupation), the association between CPAI and ALS remained of similar magnitude although falling short of statistical significance due to the reduction of the sample size (ALS cases = 147).
Occupational, household, recreational, potentially traumatic, sportive, and vigorous PAs were not associated with ALS mortality (Table 3). Although this sample is not powered to allow subgroup analyses, we obtained suggestive results for two interactions. The association with practising sports appeared modified by anthropometry: those normal weight practising sports above the median had a HR 0.77 (95 % CI 0.47–1.26) compared to those who did not practice any sport, those overweight a HR 1.30 (0.77–2.20), and those obese a HR 1.56 (0.63–3.87) (p value for interaction with BMI 0.098); subjects in each quartile of WHR had a HR 0.53 (0.23–1.22), HR 0.82 (0.38–1.76), HR 1.08 (0.56–2.09), and HR 2.15 (1.08–4.31) respectively comparing those practising sport above the median versus those not practicing sports (p value for interaction with WHR 0.045). These findings were not statistically significant, possible due to small numbers; the association with ALS appears to reverse if sports were practised by obese people (Fig. 2). The association with vigorous PA appeared to be modified by age at recruitment (thus age when the exposure was assessed) (p value for interaction = 0.048): despite the reduced sample size (ALS cases = 31), there was a suggestion of a positive association among those reporting vigorous activity early in life (<50 years) HR = 3.20 (95 % CI 0.87–11.74) for ≤2 h/week; and HR = 3.37 (95 % CI 0.88–12.93) for >2 h/week); p value for trend across categories 0.070). This association was not present among those reporting vigorous PA later on [HR = 1.04 (95 % CI 0.67–1.62); HR = 0.74 (95 % CI 0.44–1.26), respectively]. Models run separately for early and late age of ALS onset showed effect estimates comparable to those of the main analysis in both categories (results not shown).
HR and relative 95 % CI for categories of practising sport by BMI categories (a) and WHR sex-specific quartiles (b). *p value for trend across categories p = 0.345; †
p value for trend across categories p = 0.633; ‡
p value for trend across categories p = 0.354. §
p value for trend across categories p = 0.150;  p value for trend across categories p = 0.577; ^
p value for trend across categories p = 0.878; ~
p value for trend across categories p = 0.033
p value for trend across categories p = 0.577; ^
p value for trend across categories p = 0.878; ~
p value for trend across categories p = 0.033
The sensitivity analysis involving models excluding ALS cases arising during the first 3 years and during the first 5 years of follow-up showed a stronger inverse association between the CPAI and risk of dying from ALS [compared to the inactive, HR for the moderately inactive = 0.79 (95 % CI 0.56–1.12); HR for moderately active = 0.60 (95 % CI 0.39–0.93); and HR for the active = 0.65 (95 % CI 0.40–1.05), p for linear trend = 0.027 after excluding cases arisen during the first 3 years of follow up (N = 197); the same estimates after excluding cases arisen during the first 5 years of follow-up are HR = 0.69 (95 % CI 0.47–1.02); HR = 0.55 (95 % CI 0.34–0.90); and HR = 0.70 (95 % CI 0.42–1.16), p for linear trend = 0.067 (n = 162)]. All other results were substantially unchanged, apart from the widening of the confidence intervals due to the reduction of sample size.
Discussion
The present study shows a borderline significant inverse dose–response relationship between total PA measured at enrolment and subsequent risk of dying from ALS. This association does not appear to be confounded or modified by age, gender, or BMI, smoking, or highest level of education attained; but it became of borderline statistical significance once introducing WHR into model. The CPAI was designed for ranking the participants according to their overall PA based on heart rate monitoring, best reflecting the amount of energy spent in physical activities [26].
This is the first prospective cohort study assessing the type and amount of PA before disease onset, and the subsequent risk of developing and dying from ALS. The finding of an inverse association between PA and risk of ALS is at odds with the majority of findings coming from case–control studies [8, 10, 12, 20].
To date, in fact, all published evidence on the association between ALS and PA comes either from case–control studies [8, 9, 20, 29], or from retrospective cohort studies [6, 7]. The former have the limitation of being prone to recall bias (which might be particularly relevant when assessing PA whose quantification is not easy, and which can be easily related by patients to a disease impairing movements). The retrospective cohort studies investigating the risk of ALS among football players have the advantage of including large numbers, but are limited to a highly selected group, and cannot fully account for potential confounders.
Possible ways in which PA may increase the risk of ALS involve oxidative stress, glutamate excitotoxicity and complex interactions with ALS susceptibility genes [30]. On the other hand, the mechanisms through which PA might protect against ALS are thought to be mediated by exercise-induced changes in motor neuron morphology, muscle-nerve interaction, glial activation, and altering levels of gene expression of anti-apoptotic proteins and neurotrophic factors [31]. The effects of exercise upon astrocytes and angiogenesis are also relevant in ALS as astrocytes play an important structural role in the maintenance of the blood–brain barrier (BBB) [32]. A disruption of the BBB in SOD1 mice was found starting in the early stages of the disease [33]. The extensive disruption of the neurovascular unit may promote the progressive loss of motor neurons, with their integrity dependent upon efficient capillary influx of nutrients and efflux of waste, as well as direct supportive interactions with astrocytes. In the brains of exercised rats, the neurovascular unit is strengthened by increased angiogenesis and astrocyte proliferation [34].
The present data suggest that reverse causality is not a likely explanation of the results: after removing ALS deaths during the first 3 years of follow up, the inverse association strengthened (albeit with a reduced sample size). The role of unemployment in contributing to the CPAI is more complex: it might represent an effect of residual confounding of socio-economic status, or an unmeasured reverse causality. However, the fact that an association of similar magnitude between CPAI and ALS mortality (albeit not significant) is obtained after excluding those subjects who were unemployed at recruitment suggests that residual confounding or reverse causality are perhaps not the most likely explanations.
The present study had lower statistical power to detect interactions, and the findings in this sense should be interpreted cautiously and regarded as hypothesis generating. Nevertheless, it is interesting that there was also a suggestion of an increased risk of ALS from vigorous PA in obese subjects (or subjects with an elevated BMI due to substantial increase of muscle mass) among those practising sports, and in young individuals. Should these be confirmed by further investigations, they may reflect some specific characteristics of these two categories, such as, for example, the use of some stimulating agents enhancing sportive performance and/or promoting weight loss [35]. Some of these compounds, such as anabolic steroids and testosterone, increasingly used and abused by athletes for enhancing performance [36], have been shown to stimulate muscle mass increase [37]. These hormones may increase ALS risk though unknown mechanisms, and may also contribute to the higher incidence of ALS in men than women [38]. This hypothesis is consistent with previous observations linking ALS risk to practising sports in general [17, 20], or being professional football players [6, 7], or varsity athletes [8, 9, 20] or professional athletes [17]. Also, a recent report from Europe describes an inverse association between PA and ALS, except for professional sport players [29, 39]. Unfortunately, we are not able to reproduce the findings on professional sport players in this setting, as this information is not available in EPIC. A cohort effect explaining the suggested increased risk among those practising vigorous PA at younger ages has already been suggested by Ascherio [13] in reference to the study by Veldink et al. [12]; this cannot be ruled out, although it seems an unlikely explanation given that it applies to vigorous activity only. The small sample size and the relative oversampling of women by design in the EPIC study do not allow powered estimates of association in both sexes, separately. Despite the p value for interaction with sex being far non-significant (p = 0.272), we cannot rule out that the present results are at least partially driven by the association in women.
Death records appear to be reliable for ascertaining ALS deaths (and hence ALS itself) in this [2] and other large population studies [40]. Nonetheless, a recent study in UK identified an error in the WHO ICD-10 Alphabetic coding Index where progressive supranuclear palsy was mistakenly given as code G12 [23]. However, a validation exercise on death records demonstrated that only 8 % of the women receiving a diagnosis of ALS were misclassified [3]. Furthermore, misclassification introduced by the use of death records instead of specialist diagnoses would likely be non-differential and thus bias the estimate towards the null; therefore the risk estimates reported here might underestimate true associations.
In summary, in this prospective study, practising more PA was associated with a reduced risk of dying from ALS. This association does not appear to be confounded or modified by age, gender, BMI, smoking and the highest level of education attained, and it is unlikely explained by reverse causation.
References
Armon C. Amyotrophic lateral sclerosis. In: Nelson LM, Tanner CM, Van Den Eeden SK, editors. Neuroepidemiology. From principle to practice. Oxford: Oxford University Press; 2004. p. 162–87.
Gallo V, Bueno-De-Mesquita HB, Vermeulen R, Andersen PM, Kyrozis A, Linseisen J, et al. Smoking and risk for amyotrophic lateral sclerosis: analysis of the EPIC cohort. Ann Neurol. 2009;65(4):378–85.
Doyle P, Brown A, Beral V, Reeves G, Green J. Incidence of and risk factors for motor neurone disease in UK women: a prospective study. BMC Neurol. 2012;12:25.
de Jong SW, Huisman MH, Sutedja NA, van der Kooi AJ, de Visser M, Schelhaas HJ, et al. Smoking, alcohol consumption, and the risk of amyotrophic lateral sclerosis: a population-based study. Am J Epidemiol. 2012;176(3):233–9.
Nelson LM, Matkin C, Longstreth WT Jr, McGuire V. Population-based case–control study of amyotrophic lateral sclerosis in western Washington State. II. Diet. Am J Epidemiol. 2000;151(2):164–73.
Chio A, Benzi G, Dossena M, Mutani R, Mora G. Severely increased risk of amyotrophic lateral sclerosis among Italian professional football players. Brain. 2005;128(Pt 3):472–6.
Lehman EJ, Hein MJ, Baron SL, Gersic CM. Neurodegenerative causes of death among retired National Football League players. Neurology. 2012;79(19):1970–4.
Longstreth WT, McGuire V, Koepsell TD, Wang Y, van Belle G. Risk of amyotrophic lateral sclerosis and history of physical activity: a population-based case–control study. Arch Neurol. 1998;55(2):201–6.
Strickland D, Smith SA, Dolliff G, Goldman L, Roelofs RI. Physical activity, trauma, and ALS: a case–control study. Acta Neurol Scand. 1996;94(1):45–50.
Huisman MH, Seelen M, de Jong SW, Dorresteijn KR, van Doormaal PT, van der Kooi AJ, et al. Lifetime physical activity and the risk of amyotrophic lateral sclerosis. J Neurol Neurosurg Psychiatry. 2013.
Okamoto K, Kihira T, Kondo T, Kobashi G, Washio M, Sasaki S, et al. Lifestyle factors and risk of amyotrophic lateral sclerosis: a case–control study in Japan. Ann Epidemiol. 2009;19(6):359–64.
Veldink JH, Kalmijn S, Groeneveld GJ, Titulaer MJ, Wokke JH, van den Berg LH. Physical activity and the association with sporadic ALS. Neurology. 2005;64(2):241–5.
Ascherio A. Physical activity and the association with sporadic ALS. Neurology. 2005;65(6):972–3 (author reply 72–3).
Pupillo E, Messina P, Giussani G, Logroscino G, Zoccolella S, Chio A, et al. Physical activity and amyotrophic lateral sclerosis: a European population-based case–control study. Ann Neurol. 2014;75(5):708–16.
Yu Y, Su FC, Callaghan BC, Goutman SA, Batterman SA, Feldman EL. Environmental risk factors and amyotrophic lateral sclerosis (ALS): a case–control study of ALS in Michigan. PLoS ONE. 2014;9(6):e101186.
Gotkine M, Friedlander Y, Hochner H. Triathletes are over-represented in a population of patients with ALS. Amyotroph Lateral Scler Frontotemporal Degener. 2014;15(7–8):534–6.
Vanacore N, Cocco P, Fadda D, Dosemeci M. Job strain, hypoxia and risk of amyotrophic lateral sclerosis: results from a death certificate study. Amyotroph Lateral Scler. 2010;11(5):430–4.
Chio A, Calvo A, Dossena M, Ghiglione P, Mutani R, Mora G. ALS in Italian professional soccer players: the risk is still present and could be soccer-specific. Amyotroph Lateral Scler. 2009;10(4):205–9.
Valenti M, Pontieri FE, Conti F, Altobelli E, Manzoni T, Frati L. Amyotrophic lateral sclerosis and sports: a case–control study. Eur J Neurol. 2005;12(3):223–5.
Scarmeas N, Shih T, Stern Y, Ottman R, Rowland LP. Premorbid weight, body mass, and varsity athletics in ALS. Neurology. 2002;59(5):773–5.
Turner MR, Wotton C, Talbot K, Goldacre MJ. Cardiovascular fitness as a risk factor for amyotrophic lateral sclerosis: indirect evidence from record linkage study. J Neurol Neurosurg Psychiatry. 2012;83(4):395–8.
Gallo V, Wark PA, Jenab M, Pearce N, Brayne C, Vermeulen R, et al. Prediagnostic body fat and risk of death from amyotrophic lateral sclerosis: the EPIC cohort. Neurology. 2013;80(9):829–38.
O’Reilly EJ, Wang H, Weisskopf MG, Fitzgerald KC, Falcone G, McCullough ML, et al. Premorbid body mass index and risk of amyotrophic lateral sclerosis. Amyotroph Lateral Scler Frontotemporal Degener. 2013;14(3):205–11.
Riboli E, Hunt KJ, Slimani N, Ferrari P, Norat T, Fahey M, et al. European Prospective Investigation into Cancer and Nutrition (EPIC): study populations and data collection. Public Health Nutr. 2002;5(6B):1113–24.
Haftenberger M, Schuit AJ, Tormo MJ, Boeing H, Wareham N, Bueno-de-Mesquita HB, et al. Physical activity of subjects aged 50–64 years involved in the European Prospective Investigation into Cancer and Nutrition (EPIC). Public Health Nutr. 2002;5(6B):1163–76.
Wareham NJ, Jakes RW, Rennie KL, Schuit J, Mitchell J, Hennings S, et al. Validity and repeatability of a simple index derived from the short physical activity questionnaire used in the European Prospective Investigation into Cancer and Nutrition (EPIC) study. Public Health Nutr. 2003;6(4):407–13.
Peters T, Brage S, Westgate K, Franks PW, Gradmark A, Tormo Diaz MJ, et al. Validity of a short questionnaire to assess physical activity in 10 European countries. Eur J Epidemiol. 2012;27(1):15–25.
Ainsworth BE, Haskell WL, Whitt MC, Irwin ML, Swartz AM, Strath SJ, et al. Compendium of physical activities: an update of activity codes and MET intensities. Med Sci Sports Exerc. 2000;32(9 Suppl):S498–504.
Pupillo E, Messina P, Giussani G, Logroscino G, Zoccolella S, Chio A, et al. Physical activity and ALS. A European population-based, case–control study. Ann Neurol. 2014.
Harwood CA, McDermott CJ, Shaw PJ. Physical activity as an exogenous risk factor in motor neuron disease (MND): a review of the evidence. Amyotroph Lateral Scler. 2009;10(4):191–204.
McCrate ME, Kaspar BK. Physical activity and neuroprotection in amyotrophic lateral sclerosis. NeuroMol Med. 2008;10(2):108–17.
Abbott NJ, Ronnback L, Hansson E. Astrocyte–endothelial interactions at the blood–brain barrier. Nat Rev Neurosci. 2006;7(1):41–53.
Garbuzova-Davis S, Haller E, Saporta S, Kolomey I, Nicosia SV, Sanberg PR. Ultrastructure of blood–brain barrier and blood–spinal cord barrier in SOD1 mice modeling ALS. Brain Res. 2007;1157:126–37.
Li J, Ding YH, Rafols JA, Lai Q, McAllister JP 2nd, Ding Y. Increased astrocyte proliferation in rats after running exercise. Neurosci Lett. 2005;386(3):160–4.
Haller CA, Benowitz NL. Adverse cardiovascular and central nervous system events associated with dietary supplements containing ephedra alkaloids. N Engl J Med. 2000;343(25):1833–8.
Wood RI, Stanton SJ. Testosterone and sport: current perspectives. Horm Behav. 2012;61(1):147–55.
Storer TW, Magliano L, Woodhouse L, Lee ML, Dzekov C, Dzekov J, et al. Testosterone dose-dependently increases maximal voluntary strength and leg power, but does not affect fatigability or specific tension. J Clin Endocrinol Metab. 2003;88(4):1478–85.
Kiernan MC, Vucic S, Cheah BC, Turner MR, Eisen A, Hardiman O, et al. Amyotrophic lateral sclerosis. Lancet. 2011;377(9769):942–55.
Pupillo EBECA. Sport-related physical activity and amyotrophic lateral sclerosis. In: 3rd international conference of neurology and eidemiology. Nice, France; 2012.
Beghi E, Logroscino G, Micheli A, Millul A, Perini M, Riva R, et al. Validity of hospital discharge diagnoses for the assessment of the prevalence and incidence of amyotrophic lateral sclerosis. Amyotroph Lateral Scler Other Motor Neuron Disord. 2001;2(2):99–104.
Acknowledgments
This research has been made possible thanks to a grant of the European Community (5th Framework Programme) to Prof. Paolo Vineis (Grant QLK4CT199900927); and a grant of the Compagnia di San Paolo to the ISI Foundation. All authors are independent form founders. Mortality data from the Netherlands are obtained from “Statistics Netherlands”. In addition we would like to thank for their financial support: Europe Against cancer Program of the European Commission (SANCO); ISCIII, Red de Centros RCESP, C03/09; Spanish Ministry of Health (ISCIII RETICC RD06/0020); Deutsche Krebshilfe; Deutsches Krebsforschungszentrum; German Federal Ministry of Education and Research; Danish Cancer Society; Health Research Fund (FIS) of the Spanish Ministry of Health; Spanish Regional Governments of Andalucia, Asturias, Basque Country, Murcia and Navarra; Spanish Ministry of Health (ISCIII RETICC RD06/0020)Cancer Research UK; Medical Research Council, United Kingdom; Stroke Association, United Kingdom; British Heart Foundation; Department of Health, United Kingdom; Food Standards Agency, United Kingdom; Wellcome Trust, United Kingdom Greek Ministry of Health; Greek Ministry of Education; Italian Association for Research on Cancer (AIRC); Italian National Research Council; Dutch Ministry of Public Health, Welfare and Sports (VWS); Netherlands Cancer Registry (NKR); LK Research Funds; Dutch Prevention Funds, Dutch ZON (Zorg Onderzoek Nederland); World Cancer Research Fund (WCRF); Statistics Netherlands (The Netherlands); Swedish Cancer; Swedish Scientific Council; Regional Government of Skåne and Västerbotten, Sweden; Norwegian Cancer Society; Research Council of Norway; French League against cancer, Inserm, Mutuelle Generale l’Education National and IGR.
Author contributions
Dr. Gallo had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: H. Bas Bueno-de-Mesquita, Nicholas Wareham, Rudolf Kaaks, Petra P Peeters, Amalia Mattiello, Valeria Pala, Aurelio Barricante, Maria-Dolores Chirlaque, Ruth C. Travis, Anne Tjønneland, Rosario Tumino, Jose’ Ramon Quiros, Antonia Trichopoulou, Giovanna Masala, Carlotta Sacerdote, Heiner Boeing, Francoise Claver-Chapelon, Elio Riboli, Paolo Vineis. Analysis and interpretation of data: Valentina Gallo, Nicola Vanacore, H. Bas Bueno-de-Mesquita, Roel Vermeulen, Carol Brayne, Petra A. Wark, Heather A Ward, Pietro Ferrari, Mazda Jenab, Peter Andersen. Drafting of the manuscript: Valentina Gallo, Nicola Vanacore, Paolo Vineis. Data collection: H. Bas Bueno-de-Mesquita, Roel Vermeulen, Pietro Ferrari, Mazda Jenab, Nicholas Wareham, Verena Grote, Rudolf Kaaks, Elisabete Weiderpass, Petra P Peeters, Amalia Mattiello, Valeria Pala, Aurelio Barricante, Maria-Dolores Chirlaque, Noémie Travier, Ruth C. Travis, Maria-Jose Sanchez, Hélène Pessah-Rasmussen, Jesper Petersson, Anne Tjønneland, Rosario Tumino, Jose’ Ramon Quiros, Antonia Trichopoulou, Andreas Kyrozis, Despoina Oikonomidou, Giovanna Masala, Carlotta Sacerdote, Larraitz Arriola, Heiner Boeing, Francoise Claver-Chapelon, Lefkos Middleton, Elio Riboli, Paolo Vineis. Critical revision of the manuscript for important intellectual content: H. Bas Bueno-de-Mesquita, Roel Vermeulen, Carol Brayne, Petra A. Wark, Heather A Ward, Pietro Ferrari, Mazda Jenab, Peter Andersen, Patrik Wennberg, Nicholas Wareham, Verena Grote, Rudolf Kaaks, Elisabete Weiderpass, Petra P Peeters, Amalia Mattiello, Valeria Pala, Aurelio Barricante, Maria-Dolores Chirlaque, Noémie Travier, Ruth C. Travis, Maria-Jose Sanchez, Hélène Pessah-Rasmussen, Jesper Petersson, Anne Tjønneland, Rosario Tumino, Jose’ Ramon Quiros, Antonia Trichopoulou, Andreas Kyrozis, Despoina Oikonomidou, Giovanna Masala, Carlotta Sacerdote, Larraitz Arriola, Heiner Boeing, Francoise Claver-Chapelon, Lefkos Middleton, Elio Riboli, Paolo Vineis.
Funding
The EPIC study is funded by a number of grants; however, no funding source had any role in the preparation of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
We declare that we have no conflict of interests.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary Fig. 1
Matrix for the adjudication of the Cambridge Index of Physical Activity categories starting from type of job and duration of sport and cycling in hors/week in the EPIC study (JPEG 78 kb)
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Gallo, V., Vanacore, N., Bueno-de-Mesquita, H.B. et al. Physical activity and risk of Amyotrophic Lateral Sclerosis in a prospective cohort study. Eur J Epidemiol 31, 255–266 (2016). https://doi.org/10.1007/s10654-016-0119-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10654-016-0119-9