Summary
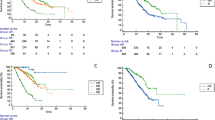
This study aimed to describe the real-world efficacy and safety of the combination therapy of atezolizumab and bevacizumab (Atezo/Bev) for unresectable hepatocellular carcinoma (HCC). This retrospective analysis of a multicenter registry cohort included 268 patients treated with Atezo/Bev. The incidence of adverse events (AE) and its impact on overall survival (OS) and progression-free survival (PFS) were analyzed. Of the 268 patients, 230 (85.8%) experienced AE. The median OS and PFS in the whole cohort were 462 and 239 days, respectively. The OS and PFS were not different in terms of AE, but they were significantly shorter in patients with increased bilirubin level and those with increased aspartate aminotransferase (AST) or alanine aminotransferase (ALT). Regarding increased bilirubin level, the hazard ratios (HRs) were 2.61 (95% confidence interval [CI]: 1.04–6.58, P = 0.042) and 2.85 (95% CI: 1.37–5.93, P = 0.005) for OS and PFS, respectively. Regarding increased AST or ALT, the HRs were 6.68 (95% CI: 3.22–13.84, P < 0.001) and 3.54 (95% CI: 1.83–6.86, P < 0.001) for OS and PFS, respectively. Contrarily, the OS was significantly longer in patients with proteinuria (HR: 0.46 [95% CI: 0.23–0.92], P = 0.027). Multivariate analysis confirmed that proteinuria (HR: 0.53 [95% CI: 0.25–0.98], P = 0.044) and increased AST or ALT (HR: 6.679 [95% CI: 3.223–13.84], P = 0.003) were independent risk factors for a shorter OS. Furthermore, analysis limited to cases who completed at least 4 cycles confirmed that increased AST or ALT and proteinuria were negative and positive factors for OS, respectively. In the real-world setting, increased AST or ALT and bilirubin level during Atezo/Bev treatment were found to have a negative impact on PFS and OS, whereas proteinuria had a positive impact on OS.




Similar content being viewed by others
Data availability
The data presented in this study are available upon request from the corresponding author.
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71:209–249
Huang DQ, Singal AG, Kono Y, Tan DJH, El-Serag HB, Loomba R (2022) Changing global epidemiology of liver cancer from 2010 to 2019: NASH is the fastest growing cause of liver cancer. Cell Metab 34:969-977.e2
Kudo M (2020) Recent advances in systemic therapy for hepatocellular carcinoma in an aging society: 2020 update. Liver Cancer 9:640–662
Finn RS, Qin S, Ikeda M, Galle PR, Ducreux M, Kim TY, Kudo M et al (2020) Atezolizumab plus bevacizumab in unresectable hepatocellular carcinoma. N Engl J Med 382:1894–1905
Kudo M, Finn RS, Qin S, Han KH, Ikeda K, Piscaglia F, Baron A et al (2018) Lenvatinib versus sorafenib in first-line treatment of patients with unresectable hepatocellular carcinoma: A randomised phase 3 non-inferiority trial. Lancet 391:1163–1173
Cheng AL, Guan Z, Chen Z, Tsao CJ, Qin S, Kim JS, Yang TS et al (2012) Efficacy and safety of sorafenib in patients with advanced hepatocellular carcinoma according to baseline status: Subset analyses of the phase III sorafenib Asia-Pacific trial. Eur J Cancer 48:1452–1465
Bruix J, Qin S, Merle P, Granito A, Huang YH, Bodoky G, Pracht M et al (2017) Regorafenib for patients with hepatocellular carcinoma who progressed on sorafenib treatment (RESORCE): A randomised, double-blind, placebo-controlled, phase 3 trial. Lancet 389:56–66
Abou-Alfa GK, Meyer T, Cheng AL, El-Khoueiry AB, Rimassa L, Ryoo BY, Cicin I et al (2018) Cabozantinib in patients with advanced and progressing hepatocellular carcinoma. N Engl J Med 379:54–63
Zhu AX, Kang YK, Yen CJ, Finn RS, Galle PR, Llovet JM, Assenat E et al (2019) Ramucirumab after sorafenib in patients with advanced hepatocellular carcinoma and increased α-fetoprotein concentrations (REACH-2): A randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Oncol 20:282–296
Cheng AL, Qin S, Ikeda M, Galle PR, Ducreux M, Kim TY, Lim HY et al (2022) Updated efficacy and safety data from IMbrave150: Atezolizumab plus bevacizumab vs. sorafenib for unresectable hepatocellular carcinoma. J Hepatol 76:862–873
Galle PR, Finn RS, Qin S, Ikeda M, Zhu AX, Kim TY, Kudo M et al (2021) Patient-reported outcomes with atezolizumab plus bevacizumab versus sorafenib in patients with unresectable hepatocellular carcinoma (IMbrave150): An open-label, randomised, phase 3 trial. Lancet Oncol 22:991–1001
Heimbach JK, Kulik LM, Finn RS, Sirlin CB, Abecassis MM, Roberts LR, Zhu AX et al (2018) AASLD guidelines for the treatment of hepatocellular carcinoma. Hepatology 67:358–380
European Association for the Study of the Liver (2018) Electronic address: easloffice.eu, EASL Clinical Practice Guidelines: Management of hepatocellular carcinoma. J Hepatol 69:182–236
Kokudo N, Takemura N, Hasegawa K, Takayama T, Kubo S, Shimada M, Nagano H et al (2019) Clinical practice guidelines for hepatocellular carcinoma: The Japan Society of Hepatology 2017 (4th JSH-HCC guidelines) 2019 update. Hepatol Res 49:1109–1113
Kudo M, Kawamura Y, Hasegawa K, Tateishi R, Kariyama K, Shiina S, Toyoda H et al (2021) Management of hepatocellular carcinoma in Japan: JSH consensus statements and recommendations 2021 update. Liver Cancer 10:181–223
Bruix J, Chan SL, Galle PR, Rimassa L, Sangro B (2021) Systemic treatment of hepatocellular carcinoma: An EASL position paper. J Hepatol 75:960–974
Chuma M, Uojima H, Hattori N, Arase Y, Fukushima T, Hirose S, Kobayashi S et al (2022) Safety and efficacy of atezolizumab plus bevacizumab in patients with unresectable hepatocellular carcinoma in early clinical practice: A multicenter analysis. Hepatol Res 52:269–280
Ochi H, Kurosaki M, Joko K, Mashiba T, Tamaki N, Tsuchiya K, Marusawa H et al (2022) Usefulness of neutrophil-to-lymphocyte ratio in predicting progression and survival outcomes after atezolizumab-bevacizumab treatment for hepatocellular carcinoma. Hepatol Res 53:61–71
Shimose S, Iwamoto H, Tanaka M, Niizeki T, Kajiwara M, Itano S, Moriyama E et al (2022) Association between adverse events and prognosis in patients with hepatocellular carcinoma treated with atezolizumab plus bevacizumab: A multicenter retrospective study. Cancers (Basel) 14:4284
Kanda Y (2013) Investigation of the freely available easy-to-use software ‘EZR’ for medical statistics. Bone Marrow Transplant 48:452–458
Hayakawa Y, Tsuchiya K, Kurosaki M, Yasui Y, Kaneko S, Tanaka Y, Ishido S et al (2022) Early experience of atezolizumab plus bevacizumab therapy in Japanese patients with unresectable hepatocellular carcinoma in real-world practice. Invest New Drugs 40:392–402
Tanaka T, Hiraoka A, Tada T, Hirooka M, Kariyama K, Tani J, Atsukawa M et al (2022) Therapeutic efficacy of atezolizumab plus bevacizumab treatment for unresectable hepatocellular carcinoma in patients with Child-Pugh class A or B liver function in real-world clinical practice. Hepatol Res 52:773–783
Tada T, Kumada T, Hiraoka A, Hirooka M, Kariyama K, Tani J, Atsukawa M et al (2022) Safety and efficacy of atezolizumab plus bevacizumab in elderly patients with hepatocellular carcinoma: A multicenter analysis. Cancer Med 11:3796–3808
Ando Y, Kawaoka T, Kosaka M, Shirane Y, Johira Y, Miura R, Murakami S et al (2021) Early tumor response and safety of atezolizumab plus bevacizumab for patients with unresectable hepatocellular carcinoma in real-world practice. Cancers (Basel) 13:3958
Chan SL, Yip TC, Wong VW, Tse YK, Yuen BW, Luk HW, Lui RN et al (2020) Pattern and impact of hepatic adverse events encountered during immune checkpoint inhibitors - A territory-wide cohort study. Cancer Med 9:7052–7061
Yokohama K, Asai A, Matsui M, Okamoto N, Yasuoka H, Nishikawa T, Ohama H et al (2020) Liver dysfunction is associated with poor prognosis in patients after immune checkpoint inhibitor therapy. Sci Rep 10:14470
Yamamoto T, Ito T, Hase T, Ishigami M, Mizuno K, Yamamoto K, Imai N et al (2022) Immune-related liver injury is a poor prognostic factor in patients with nonsmall cell lung cancer treated with immune checkpoint Inhibitors. Cancer Investig 40:189–198
Hurwitz H, Fehrenbacher L, Novotny W, Cartwright T, Hainsworth J, Heim W, Berlin J et al (2004) Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Engl J Med 350:2335–2342
Karachaliou N, Saloustros E, Vamvakas L, Mavroudis D, Georgoulias V (2010) Proteinuria and favourable clinical response in a patient receiving paclitaxel + bevacizumab for metastatic breast cancer. Ann Oncol 21:1729–1730
Khoja L, Kumaran G, Zee YK, Murukesh N, Swindell R, Saunders MP, Clamp AR et al (2014) Evaluation of hypertension and proteinuria as markers of efficacy in antiangiogenic therapy for metastatic colorectal cancer. J Clin Gastroenterol 48:430–434
Carvalho B, Lopes RG, Linhares P, Costa A, Caeiro C, Fernandes AC, Tavares N et al (2020) Hypertension and proteinuria as clinical biomarkers of response to bevacizumab in glioblastoma patients. J Neurooncol 147:109–116
Iwasa S, Nakajima TE, Nagashima K, Honma Y, Kato K, Hamaguchi T, Yamada Y, Shimada Y (2013) Lack of association of proteinuria and clinical outcome in patients treated with bevacizumab for metastatic colorectal cancer. Anticancer Res 33:309–316
Uysal M, Bozcuk H, Sezgin Göksu S, Murat Tatli A, Arslan D, Gündüz S, Senol Coskun H et al (2014) Basal proteinuria as a prognostic factor in patients with metastatic colorectal cancer treated with bevacizumab. Biomed Pharmacother 68:409–412
Ando Y, Kawaoka T, Kosaka M, Shirane Y,Johira Y, Miura R et al (2022) Risk factors for early onset of proteinuria in patients receiving atezolizumab plus bevacizumab for unresectable hepatocellular carcinoma. Liver Cancer. https://doi.org/10.1159/000528145
Funding
This work was supported by a Grant-in-Aid from the Japan Agency for Medical Research and Development (JP20fk0210067h0001 and JP23fk0210123h0001).
Author information
Authors and Affiliations
Contributions
Shintaro Takaki and Masayuki Kurosaki provided analysis and writing the main manuscript, Hironori Ochi,Toshifumi Tada and Kaoru Tsuchiya reviewed and corrected the main manuscript. Shintaro Takaki, Masayuki Kurosaki, Nami Mori, Keiji Tsuji, Hironori Ochi, Hiroyuki Marusawa, Shinichiro Nakamura, Toshifumi Tada, Narita Ryoichi, Yasushi Uchida, Takehiro Akahane, Masahiko Kondo, Atsunori Kusakabe, Koichiro Furuta, Haruhiko Kobashi, Hirotaka Arai, Riko Nonogi, Takashi Tamada, Chitomi Hasebe, Chikara Ogawa, Takashi Sato, Nobuharu Tamaki, Yutaka Yasui, Kaoru Tsuchiya, Namiki Izumi treated the patients, collected the data and reviewed the final manuscript.
Corresponding author
Ethics declarations
Competing interests
Masayuki Kurosaki, Namiki Izumi and Kaoru Tsuchiya received lecture fees from Chugai. The other authors have no conficts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Takaki, S., Kurosaki, M., Mori, N. et al. Effects on survival of the adverse event of atezolizumab plus bevacizumab for hepatocellular carcinoma: a multicenter study by the Japan Red Cross Liver Study Group. Invest New Drugs 41, 340–349 (2023). https://doi.org/10.1007/s10637-023-01349-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10637-023-01349-4