Abstract
Introduction
Thiopurines (azathioprine and 6-mercaptopurine) have been used in the management of UC patients for over three decades. Nearly half of patients with UC treated with thiopurines fail to achieve remission or lose remission during treatment. Factors associated with thiopurine failure are poorly understood. The primary aim of our study was to investigate patient-related factors which are associated with thiopurine failure.
Methods
TNF-alpha antagonist-naïve patients with histological diagnosis of UC, receiving thiopurine therapy, with follow-up data from 1 to 3 years were included in the study. Data regarding demographics, laboratory results, and disease characteristics were collected. The primary endpoint was failure of thiopurine therapy, defined as treatment with steroids, therapeutic escalation to TNF-alpha antagonist therapy, or need for surgery.
Results
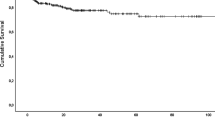
Of the 563 patients identified using ICD-9 codes, 78 TNF-alpha antagonist-naïve patients with a histological diagnosis of UC, receiving thiopurine treatment, were identified. Over the three-year follow-up period, 38 patients failed thiopurine treatment. On adjusted Cox regression, BMI < 25 kg/m2 (HR 3, 95 % CI 1.55–5.83; p value = 0.001) was significantly associated with thiopurine failure. Furthermore, although not statistically significant, there was a strong trend toward thiopurine failure among patients with serum albumin level < 4 g/dL (HR 1.98, 95 % CI 0.97–4; p value = 0.06), non-smoking status (HR 2.2, 95 % CI 0.96–5.06; p value = 0.06), and higher degree of colon inflammation (HR 1.49, 95 % CI 0.96–2.32; p value = 0.08).
Discussion
Our results show that low body mass index is associated with increased risk of failure of thiopurine treatment. Furthermore, there was a strong trend toward thiopurine failure among patients with low serum albumin level (<4gm/dL). These factors should be considered as markers of non-response to thiopurine monotherapy for patients with moderately severe ulcerative colitis.



Similar content being viewed by others
References
Danese S, Fiocchi C. Ulcerative colitis. N Engl J Med. 2011;365:1713–1725. doi:10.1056/NEJMra1102942.
Louis E, Irving P, Beaugerie L. Use of azathioprine in IBD: modern aspects of an old drug. Gut. 2014;. doi:10.1136/gutjnl-2013-306711.
Fraser AG, Orchard TR, Jewell DP. The efficacy of azathioprine for the treatment of inflammatory bowel disease: a 30 year review. Gut. 2002;50:485–489.
Hawthorne AB, Logan RF, Hawkey CJ, et al. Randomised controlled trial of azathioprine withdrawal in ulcerative colitis. BMJ. 1992;305:20–22.
Cañas-Ventura A, Márquez L, Ricart E, et al. Risk of colectomy in patients with ulcerative colitis under thiopurine treatment. J Crohns Colitis. 2014;8:1287–1293. doi:10.1016/j.crohns.2014.03.014.
Gisbert JP, Linares PM, McNicholl AG, Maté J, Gomollón F. Meta-analysis: the efficacy of azathioprine and mercaptopurine in ulcerative colitis. Aliment Pharmacol Ther. 2009;30:126–137. doi:10.1111/j.1365-2036.2009.04023.x.
Atreya I, Neurath MF. Azathioprine in inflammatory bowel disease: improved molecular insights and resulting clinical implications. Expert Rev Gastroenterol Hepatol. 2008;2:23–34. doi:10.1586/17474124.2.1.23.
Ha C, Dassopoulos T. Thiopurine therapy in inflammatory bowel disease. Expert Rev Gastroenterol Hepatol. 2010;4:575–588. doi:10.1586/egh.10.59.
Chatu S, Saxena S, Subramanian V, et al. The impact of timing and duration of thiopurine treatment on first intestinal resection in Crohn’s disease: national UK population-based study 1989–2010. Am J Gastroenterol. 2014;109:409–416. doi:10.1038/ajg.2013.462.
Khan ZH, Mayberry JF, Spiers N, Wicks AC. Retrospective case series analysis of patients with inflammatory bowel disease on azathioprine. A district general hospital experience. Digestion. 2000;62:249–254. doi:10.1159/000007823.
Saibeni S, Virgilio T, D’Incà R, et al. The use of thiopurines for the treatment of inflammatory bowel diseases in clinical practice. Dig Liver Dis. 2008;40:814–820. doi:10.1016/j.dld.2008.03.016.
National Health Accounts Historical 2014. https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/NationalHealthExpendData/NationalHealthAccountsHistorical.html. Accessed December 16, 2014.
Gunnarsson C, Chen J, Rizzo JA, Ladapo JA, Lofland JH. Direct health care insurer and out-of-pocket expenditures of inflammatory bowel disease: evidence from a US national survey. Dig Dis Sci. 2012;57:3080–3091. doi:10.1007/s10620-012-2289-y.
D’Haens GR. Top-down therapy for IBD: rationale and requisite evidence. Nat Rev Gastroenterol Hepatol. 2010;7:86–92. doi:10.1038/nrgastro.2009.222.
Park KT, Bass D. Inflammatory bowel disease-attributable costs and cost-effective strategies in the United States: a review. Inflamm Bowel Dis. 2011;17:1603–1609. doi:10.1002/ibd.21488.
Hanson K, Benouna SME. Managing the costs of your IBD care 2013. http://www.ccfa.org/assets/pdfs/managing-costs-of-ibd.pdf. Accessed December 17, 2014.
Sochacka J, Baran W. The investigation of the binding of 6-mercaptopurine to site I on human serum albumin. Protein J. 2012;31:689–702. doi:10.1007/s10930-012-9449-y.
Tesseromatis C, Alevizou A. The role of the protein-binding on the mode of drug action as well the interactions with other drugs. Eur J Drug Metab Pharmacokinet. 2008;33:225–230.
Dotan I, Ron Y, Yanai H, et al. Patient factors that increase infliximab clearance and shorten half-life in inflammatory bowel disease: a population pharmacokinetic study. Inflamm Bowel Dis. 2014;20:2247–2259. doi:10.1097/MIB.0000000000000212.
Fasanmade AA, Adedokun OJ, Ford J, et al. Population pharmacokinetic analysis of infliximab in patients with ulcerative colitis. Eur J Clin Pharmacol. 2009;65:1211–1228. doi:10.1007/s00228-009-0718-4.
Fasanmade AA, Adedokun OJ, Olson A, Strauss R, Davis HM. Serum albumin concentration: a predictive factor of infliximab pharmacokinetics and clinical response in patients with ulcerative colitis. Int J Clin Pharmacol Ther. 2010;48:297–308.
Truelove SC, Witts LJ. Cortisone in ulcerative colitis; preliminary report on a therapeutic trial. Br Med J. 1954;2:375–378.
Kelley-Quon LI, Jen HC, Ziring DA, et al. Predictors of proctocolectomy in children with ulcerative colitis. J Pediatr Gastroenterol Nutr. 2012;55:534–540. doi:10.1097/MPG.0b013e3182619d26.
Stabroth-Akil D, Leifeld L, Pfützer R, Morgenstern J, Kruis W. The effect of body weight on the severity and clinical course of ulcerative colitis. Int J Colorectal Dis. 2014. doi:10.1007/s00384-014-2051-3.
Blain A, Cattan S, Beaugerie L, Carbonnel F, Gendre JP, Cosnes J. Crohn’s disease clinical course and severity in obese patients. Clin Nutr. 2002;21:51–57. doi:10.1054/clnu.2001.0503.
Hass DJ, Brensinger CM, Lewis JD, Lichtenstein GR. The impact of increased body mass index on the clinical course of Crohn’s disease. Clin Gastroenterol Hepatol. 2006;4:482–488. doi:10.1016/j.cgh.2005.12.015.
Sartor RB. Mechanisms of disease: pathogenesis of Crohn’s disease and ulcerative colitis. Nat Clin Pract Gastroenterol Hepatol. 2006;3:390–407. doi:10.1038/ncpgasthep0528.
Kredel LI, Batra A, Stroh T, et al. Adipokines from local fat cells shape the macrophage compartment of the creeping fat in Crohn’s disease. Gut. 2013;62:852–862. doi:10.1136/gutjnl-2011-301424.
Yamamoto K, Kiyohara T, Murayama Y, et al. Production of adiponectin, an anti-inflammatory protein, in mesenteric adipose tissue in Crohn’s disease. Gut. 2005;54:789–796. doi:10.1136/gut.2004.046516.
Iskandar H, Greer JB, Schraut WH, et al. IBD LIVE case series-case 1: smoking, a controversial but effective treatment for ulcerative colitis. Inflamm Bowel Dis. 2014;20:1696–1701. doi:10.1097/MIB.0000000000000188.
Aldhous MC, Drummond HE, Anderson N, et al. Smoking habit and load influence age at diagnosis and disease extent in ulcerative colitis. Am J Gastroenterol. 2007;102:589–597. doi:10.1111/j.1572-0241.2007.01065.x.
Tobin MV, Logan RF, Langman MJ, McConnell RB, Gilmore IT. Cigarette smoking and inflammatory bowel disease. Gastroenterology. 1987;93:316–321.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Thapa, S.D., Hadid, H., Usman, M. et al. Predictors of Thiopurine Treatment Failure in Biologic-Naïve Ulcerative Colitis Patients. Dig Dis Sci 61, 230–237 (2016). https://doi.org/10.1007/s10620-015-3864-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-015-3864-9