Abstract
In the United States, Black communities face a complex mental health burden, with growing attention on addressing these disparities through the lens of holistic wellbeing. Given the dearth of research on faith-based interventions focused on mental health through the lens of holistic wellbeing, this study evaluates the impact of a spirituality-based, peer-led one-group pre-test post-test pilot intervention in a sample of Black individuals in the Bronx, New York City. The eight-session creating healthy culture curriculum, focused on improving mental health and spiritual wellbeing, was collaboratively developed through community partnerships. Post-intervention results indicated significantly reduced odds of moderate to severe depression (AOR:0.20), and increased sense of community, social support, role of religion in health, flourishing, and reduced trouble sleeping. In-depth interviews with participants further highlighted the interconnected role between psychosocial and mental health indicators. Findings support importance of holistically developing, implementing, and evaluating spirituality-based mental health interventions in Black communities.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
In the United States (US), Black communities experience a diverse range of physical and mental health disparities (Baciu et al., 2017), including a disproportionality high prevalence of chronic conditions (such as heart disease, diabetes and hypertension) and lower life expectancy than White populations (a disparity which has grown further during the COVID-19 pandemic) (Andrasfay & Goldman, 2021; Quiñones et al., 2019). Moreover, Black individuals are more likely to be victims of violent crimes proportional to their population (San Diego Association of Governments (SANDAG), 2020), and report a higher workplace injury rate compared to all other racial and ethnic sub-groups (Seabury et al., 2017). These physical health disparities intersect with more complex disparities in mental health; while the 2015 estimated lifetime prevalence of depression among Non-Hispanic Black (5.39%) Americans was lower than Non-Hispanic Whites (8.00%) (Weinberger et al., 2018), estimates of lifetime prevalence of post-traumatic stress disorder (PTSD) indicate a significantly higher proportion among Black (8.7%) than White Americans (7.4%) (Roberts et al., 2011).
In a recent report on nationwide disparities in depression treatment, in adjusted analyses, Black individuals were about half as likely was White individuals to receive depression treatment (AOR:0.52) (McGregor et al., 2020). Data from across the US has also shown that victims of fire-arm homicides are majority (65.3%) Black, with police-involved deaths of Black individuals also significantly higher than White individuals (Edwards et al., 2018; Wong et al., 2020). Exposure to growing concerns of systemic discrimination and violence, such as police killings, have been specifically linked with poor mental outcomes among Black communities (Bor et al., 2018). Ultimately, the physical and mental health burden experienced by Black communities are often localized to specific areas in the US that experience structural-level barriers to health. In New York City (NYC) for example, the borough of Bronx has the highest proportion of Black (43.6%) residents, but also the city's highest poverty rate (26.2%), lowest high school educational attainment (72.8%), and highest prevalence of disabled people (11.4%) (United States Census Bureau, 2019). Out of all 62 counties in New York, the Bronx has also been ranked the least healthy (a composite of multiple health indicators) and is also among the least healthy counties in the country (New York State Health Foundation, 2019).
To meet these complex health needs in Black communities, there has been growing advocacy to understand and address health disparities holistically within the concept of general wellness, defined as "the active pursuit of activities, choices and lifestyles that lead to a state of holistic health" (Global Wellness Institute, n.d.). The idea of wellness integrates multiple social and structural forces in the experience with health, the capacity to actively address or cope with health needs, and general perceptions about one's life (Centers for Disease Control and Prevention (CDC), 2018; Stoewen, 2015). Enhancing general wellness has been associated with reduced anxiety, depression, stress, and improved physical health (e.g., reduced A1C among diabetics and improved cholesterol, diet, and exercise outcomes) (Massey et al., 2019; Russell et al., 2020). The concept can further be disaggregated into the domains of physical, intellectual, emotional, social, spiritual, vocational, financial, and environmental wellness (Stoewen, 2017). Perceived social support (feeling that one has people to turn to in times of need), sense of community (feeling connected within one's communities), sense of control (feeling of having control over one's outcomes), and overall "flourishing" (feeling that all aspects of one's life are going well) have also been studied as components of wellbeing (Chu et al., 2010; de Quadros-Wander et al., 2014; Pozzi et al., 2014; VanderWeele, 2017). Moreover, spiritual health and wellbeing (defined as the meaningfulness of one's life, one's personal or communal sense of purpose, and/or one's connection to a transcendental power or the natural environment Fisher et al., 2000; Ghaderi et al., 2018)) are particularly salient dimensions in the experience of health and wellbeing among Black communities in the US (Bolger et al., 2018; Park & Millora, 2010).
Although interventions aimed at addressing the mental health needs of Black communities have included collaborative care and therapeutic communications with providers, screenings in nursing homes and clinics, psychoeducation, and creating informal networks of social support, faith-based health interventions have grown in significance (Bhui et al., 2013; Grier-Reed, 2013; Hays, 2015; Lee-Tauler et al., 2018). The significance of faith-based organizations (FBOs) in Black populations, such as churches, are a reflection of the link between spirituality and health (particularly mental health) in the community, and also serve as trusted community centers and important distributors of social and health resources (Blank et al., 2002; Hays, 2015; Nguyen, 2020). Faith-based health programs have aimed to address both physical and mental health needs; these collaborations can include working with churches in recruitment and delivery of a program (including incorporating spiritual elements) (Yeary et al., 2012). Among Black communities specifically, churches have played a vital role in addressing emerging health challenges (such as HIV/AIDS) and increasing healthcare utilization (Eke et al., 2010). A systematic review showed that faith-based health interventions in Black communities have been effective in improving reducing substance use, smoking, and depression (Hankerson & Weissman, 2012), however interventions were largely aimed at specific lifestyle or substance use knowledge, attitude, or behavioral outcomes without a specific focus of improving mental health (e.g. depression, PTSD symptoms). The review also highlighted that past faith-based interventions have been culturally tailored to emphasize elements of Black culture and spirituality (e.g., using gospel music and devotional booklets as part of interventional activities). Advocacy of FBO-collaborations has also focused on the importance of religious coping practices to address mental health needs in Black communities (Hays, 2015).
Moreover, peer-led interventions have specifically been shown to be powerful in improving social connectedness and engagement, as well as improving health outcomes and health-related knowledge, attitudes, beliefs, and behaviors (including among Black communities) (Ramchand et al., 2017; Tang et al., 2015; Williams et al., 2010). Peer support has been identified as a core feature of mental health recovery, and such interventions (which involve having individuals of closely connected to participants or from a similar background be involved in the implementation of the program) have been particularly efficacious in improving mental health outcomes by facilitating better communication of mental health experiences and creating structures of trust and understanding (Druss et al., 2010; Patalay et al., 2017; Repper & Carter, 2011). Faith-based peer-led mental interventions have also been shown to be effective in reducing anxiety and depression (Rogers & Stanford, 2015), however such interventions have yet to be examined to meet the mental health needs of marginalized Black communities (such as Black residents the in Bronx, NYC), particularly interventions incorporating principles of broader wellbeing. Likewise, while digital peer-led interventions (e.g., using peer-led or peer-developed videos and emails) have been explored to address mental health needs (Fortuna et al., 2020), such technologies remain underexplored among older populations and Black communities (both of which have been particularly vulnerable during the COVID-19 pandemic and could benefit from such socially-distant intervention methods) (Gold et al., 2020). Therefore, this study describes the impact of a remote, peer-led intervention focused on improving mental health through a holistic, spirituality-based approach among Black participants attending congregations in the Bronx (NYC). Specifically, the intervention sought to deepen participants’ relationships with God or a higher power (“Higher Power” hereafter) and each other, and practiced the spiritual disciplines of faith, trust, forgiveness, empathy, caring and kindness.
Methods
Study Population
Creating Healthy Culture (CHC) was a one-group pre-test post-test pilot intervention conducted between November 2020 and February 2021. The project utilized principles of community-based participatory research (CBPR) to guide the development, implementation, and evaluation of the study (Israel et al., 2017). New York University Grossman School of Medicine worked in partnership with the Groundswell Group (GG) and the Network for Human Understanding (NHU), community-based organizations that seek to build a stronger sense of community and a deeper level of spiritual awareness and sensitivity. Rev. Addie Banks, who leads GG, had previously pastored at a congregation in the Bronx for over twenty years and has since worked as an advocate and spiritual leader for the religious and spiritual communicates of Bronx, NY. Leveraging its existing network of partners, GG and NHU recruited nine congregations located in Bronx, NY and from diverse denominations including Methodist, Mennonite, Episcopal, and non-denominational. These congregations are primarily attended by diverse sub-groups of Black communities, including those from the Caribbean as well as Central and South America. Each leader at the congregation then identified one to two peer educators who would deliver the intervention, totaling 17 peer educators across all sites. Peer educators were purposively selected by the congregation leaders based on their level of involvement in church activities, previously demonstrated leadership, and interest in becoming a peer educator. Each educator received four sessions of training lasting approximately two hours each, facilitated by GG and NHU. Based on a list of eligible individuals generated by the congregation leader, peer educators recruited individuals within each congregation to participate in the intervention; contacted individuals could decline to participate without fear of consequences, which was stated again during the verbal consent process. Participants were eligible if they: (1) were over 18 years of age, and (2) had attended a service at their congregation at least three times in the past year. Eligible participants were identified by both the congregation leaders and peer educators via a convenience sampling approach based on their level of involvement in church activities and perceived interest in potential participation. The Institutional Review Board of the New York University Grossman School of Medicine approved the study and the trial was registered at ClinicalTrials.gov (NCT04353427).
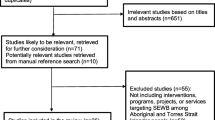
All eligible individuals who were nominated by the congregation leaders (n = 94) agreed to participate in the intervention when contacted by the peer educators and were verbally consented by a research assistant at the partner academic institution. Out of these 94 participants, three participants never attended any sessions, five participants were excluded from analysis due to low attendance (defined as having attended less than 6 of 8 sessions), and an additional two participants were lost to follow-up (unable to be reached for endpoint survey). A total of 84 participants were included in the final analysis; 78 participants attended all eight sessions and the remaining six participants attended seven of eight sessions. Participants were compensated $90 after completion of the baseline survey and an additional $160 upon completing the follow-up survey for those who attended at least 6 of the 8 sessions (a total of $250 for full program participation).
Intervention
GG and NHU developed an eight-session curriculum focused on mental health problem identification, improving overall spiritual well-being, and addressing feelings related to anxiety, stress, and trauma through spirituality-based strategies. The curriculum was developed using a combination of spiritual disciplines that are rooted in the teachings of St. Ignatius of Loyala, and have been used for hundreds of years in a process called "Spiritual Direction and Spiritual Formation," to deepen people's relationship with and experience of the power and the presence of the Higher Power (Osorio, 2005). This includes Contemplative Prayer and Lectio Divina, a process of reading Scripture so that it has a deep emotional impact on the reader. The curriculum also incorporated a cognitive-behavioral approach to changing participant's thought patterns to reduce negative thinking and develop the habit of positive thinking that supports a mental and emotional state of faith, peace and wellbeing (Tan, 2013).
The session topics included: (1) Your journey to healing, health and wellness; (2) The healing power of a life shared with a Higher Power; (3) The healing power of prayer; (4) The body as temple; (5) Transformed and healed by the renewing of your mind; (6) The healing power of relationships; (7) Healing the wounds of the heart; (8) The healing power of forgiveness (See Table 1 for a description of the sessions). The group sessions, which were largely interactive and involved discussions with both educators and other participants, were delivered remotely via a videoconferencing platform approximately once a week for a total duration of eight to ten weeks. Sessions, on average, were about 2 hours in length, were comprised of 9 participants across participating congregations (range 3–16). Each session started with the peer educators sharing the session’s key principles and leading a dialogue with participants, which allowed the participants to share their reflections on the topic.
Data Collection
Surveys with participants were collected at baseline and at follow-up, immediately after completion of the intervention. Surveys were administered via phone by a trained research coordinator and data were entered directly into REDCap—an online research database. Surveys measured sociodemographic characteristics, mental health outcomes (i.e., depression and post-traumatic stress disorder), and psychosocial variables (e.g., social support, sense of community, spirituality). The selection of the primary and secondary outcomes in the survey were informed by consultation with both community and academic partners and aimed to capture different dimensions of holistic wellbeing (particularly spiritual and mental wellbeing). Given the link between diverse mental health outcomes and wellbeing (Massey et al., 2019; Russell et al., 2020), community partners emphasized assessing multiple facets of both mental health and wellbeing, which informed the decision to measure both depression and PTSD in the study.
At completion of the intervention, a convenience sample of 27 participants was selected for in-depth interviews (three from each site). Interviews sought to elicit barriers and facilitators to study participation, acceptability, and satisfaction. Interviews were conducted over the phone, audio-recorded, and transcribed verbatim. Interviews lasted approximately 30 min. Although the research coordinator and interviewers did not identify as Black, past research has substantiated that race non-concordance between participants and interviewers do not introduce significant bias during data collection (Batch et al., 2013; Fryer et al., 2016). The interviewer was a research assistant at the partner academic institution and was not a member of these same congregations nor knew any of the participants personally outside of the study context.
Measures
Primary Outcomes
Symptoms of depression were assessed using the 9-item Patient Health Questionnaire (PHQ-9), validated in diverse US populations (Huang et al., 2006), providing a depression score of between 0 and 27 (a score of 10 or higher indicating moderate to severe depression) (Kroenke et al., 2001). PTSD was assessed using the 20-item PTSD checklist for DSM-5 (subdivided into Criteria B, C, D, and E questions), with a provisional PTSD diagnosis being defined as endorsing (rating "moderately" or higher) 1 symptom in Criteria B and C, and 2 in Criteria D and E (U. S. Department of Veterans Affairs, 2021).
Secondary Outcomes
Sense of community was measured using a 12-item version of the Sense of Community Index 2 (SCI-2) comprised of the 6-item membership and 6-item shared emotional connection sub-scales (Chavis et al., 2008). An additional 4-item health-related sense of community sub-scale was also assessed (Dubowitz et al., 2020). Sense of control was measured through the 4-item personal mastery sub-scale (SC-4) of the 12-item Sense of Control scale (Lachman & Weaver, 1998). Social support was measured through the 8-item modified Medical Outcomes Study Social Support Survey (mMOS-SS) (Moser et al., 2012). Flourishing was measured through the 10-item Flourishing Index and 12-item Secure Flourishing Index (VanderWeele, 2017).
The role of spirituality and religion in one's life was assessed by 3 one-item Likert-scale questions asking participants to rate the importance of the following items from not at all (0) to very important (4): religion and/or spirituality in your life, religion and/or spiritualty in the choices you make about health, and religion and/or spiritualty in the way I interact with my loved ones and peers. Spirituality was assessed through the 6-item Daily Spiritual Experience Scale (DSES) (Underwood, 2011). Religious coping was assessed through a 1-item metric derived from the National Latino and Asian American Study (NLAAS) (Ai et al., 2013). Sleep was measured through two items derived from the National Health and Nutrition Examination Survey (NHANES) which asked participants how many hours of sleep they usually get at night and how often they had trouble following asleep in the past month (from never to always) (Whinnery et al., 2014).
Analysis
For the present study, analysis was focused on the 79 participants who identified as Black of the total 84 participants with complete baseline and follow-up data. For quantitative data, descriptive analyses were first conducted to summarize participant demographic information as well as mental health, psychosocial, and sleep related outcome variables at baseline and follow-up. Paired t-tests (continuous variables) and McNemar tests (categorical variables) were conducted to assess differences between baseline and follow-up data. For qualitative data, participant interviews were deductively analyzed using a rapid qualitative analysis, which has been shown to be a valid method of efficiently identifying specific and actionable themes from qualitative data in implementation science research (Gale et al., 2019). This process involved developing a preliminary qualitative codebook that informed the definitions of the quantitative mental health, psychosocial, and sleep related outcome indicators, and using this codebook to identify how each indicator was reflected in participant's daily lives following the intervention from interview data.
Results
Participant Characteristics
Socio-demographic characteristics of the 79 participants analyzed in the study are described in Table 2. The age of participants ranged from 23 to 88, and most were US-born, college educated, and rented or owned their own living accommodation. Most participants (78.5%) had attended their congregation for 7 years or more. Participants also reported a high frequency of attending religious activities.
Quantitative Outcomes
The baseline prevalence of moderate to severe depression and PTSD were high in the sample (Table 3). The odds of depression were significantly lower following the intervention, and the change in PTSD approached significance. Sense of community significantly increased following the intervention; we saw an increase in membership and shared emotional connection, but no significant changes in health-related sense of community were observed. Participant flourishing, secure flourishing, and social support also increased after the intervention, along with daily spiritual experience and perceived importance of religion in one's health choices and interactions. While hours of sleep each day did not significantly change post-intervention, the odds of reporting trouble falling or staying asleep were significantly lower.
Qualitative Outcomes
Analysis of participant interviews corroborated quantitative findings by identifying how participants experienced psycho-social and mental health outcomes in their daily lives, and how these experiences were shaped by the intervention (Table 4). Themes related to changes in sleep behaviors were not identified in the transcripts.
The post-intervention status of the examined mental health-related challenges was observed to be strongly connected with other psycho-social and religious constructs examined. Mental health-related challenges were salient in the lives of participants and included feelings of loneliness, sadness, and anxiety, which were observed to decrease after the intervention. Participants specifically connected the constructs of sense of community and social support as catalysts in the reduction of these mental health challenges (particularly loneliness) through the strengthening of interactions and interpersonal bonds with other participants throughout the course of the intervention. Similarly, while those displaying mental health challenges related to trauma still described the lingering emotional and health impacts of past traumatic events on their current lives, many highlighted the growing significance of religious coping strategies. For example, the role of a Higher Power as a pillar of strength and reliance when coping with the emotional impacts of past trauma was reported:
“He is there. He said I am there with you. He's not going to leave me...wherever I am, I fall on him and he is there to help me...I go through the trauma but in him I rest, you know, so I'm good.”
Many participants also reported a stronger sense of control over one’s life post-intervention. Increased sense of control over one’s physical, spiritual, and mental health was a common theme. Meditating and breathing exercises were noted to have a positive impact on participants’ mental and spiritual health, in part through greater emotional balance and increased self-awareness. Additionally, participants reported better communication with others in their life after the intervention, including more patience and decreased feelings of judgement when participants interacted with the people in their community. Specifically, participants reported having an increased sense of control over their interpersonal relations in that many learned to be forgiving with oneself and others. Releasing such feelings of resentment seemed to not only cast away any feelings of personal guilt but also build tolerance and empathy towards others:
“...this course teaches you that forgiveness comes from the heart and if it comes from the heart...you're not going to dwell on it...A lot of people are going through stuff that they don't even mention...sometimes your neighbor could be going through stuff and maybe that's why they are angry.”
Social support and participant’s sense of community also grew in significance in participants’ lives. Many participants reported feeling closer to their community and church members post-intervention. Findings also suggest that participants displayed an increased sense of trust that church members can work to improve overall community health. Even though the intervention was conducted entirely during the COVID-19 pandemic, the use of technology in the program opened more avenues for the participants to reach out to their community members. In many cases, the program helped participants combat isolation induced by the lockdown, which helped to strengthen participant interpersonal relationships. Additionally, due to their enhanced sense of community, the participants were willing and comfortable to share personal stories with each other as a means of further connecting with community members.
“...we have a core of seniors at our Church who show up every Wednesday to help distribute vegetables, fruit and vegetables to the community...I have unlimited options as far as the technology is concerned in terms of reaching out and getting in touch with people...we should consider ourselves physically distanced, but not socially so I don't feel that I've suffered in any way in terms of the human discourse element and the human contact element."
Principles related to the construct of flourishing also emerged in participants’ post-intervention experiences. Many participants reported feeling “at peace” with oneself after the program had ended; one participant, for example, mentioned being at peace after having mended their relationship with a family member, which was an action prompted by their participation in the intervention. Flourishing was also evidenced through the multidimensional impact experienced by participants post-intervention, notably through improved overall mental, spiritual, and physical health. These improvements were linked with greater life satisfaction and overall happiness for the participants in that many participants felt growth in their character and reported having improved social relationships.
"...overall, I am at peace. Much happier moments than before.”
Religion and spirituality were observed as a significant driver of one participant's behaviors and a catalyst of many of the experiences reported. This saliency was in part reflected through the link between religious coping and mental health challenges related to trauma in that participants reported their relationship with a Higher Power to be consoling and a catalyst for alleviating trauma-induced pain. Religious and spiritual influences also were associated with improved mental and spiritual health outcomes for the participants. More specifically, participants noted that meditation and breathing exercises were a gateway to de-stressing and feeling closer to a Higher Power. Relationships with a Higher Power were also linked with routine health behaviors; in particular, their understanding of scripture seemed to affect their sense of control in that some participants mentioned treating their body as a “temple;” specifically, incorporating a religion-based driver in the conscious effort to maintain overall physical health, motivating healthier habits.
“...that week they talked about...the body is a temple, and I decided, you know what? I can just walk instead of taking the bus and I think that helps me physically. Now, whether it affects me mentally, I don't know, but I guess if you're doing well physically, it probably helps you to feel better mentally.”
In terms of feasibility of the intervention itself, most participants reported not facing significant technological challenges. Those that reported using Zoom was challenging added that it was an initial hurdle that they had to overcome but once they were familiar with Zoom, they felt comfortable with how the sessions were delivered. Regardless of whether the sessions were conducted during a pandemic, most participants mentioned that they would prefer to participate in sessions virtually over Zoom instead of sessions conducted in-person.
Discussion
Overall, the implemented pilot spirituality-based, peer-led intervention was observed to have a significant impact in improving mental health and related psycho-social outcomes among a sample of Black residents living in NYC. At baseline, the prevalence of both depression (16.5%) and PTSD (12.7%) were notably higher than past national estimates among Black communities in the general population (5.39%, 8.7%) (Roberts et al., 2011; Weinberger et al., 2018). Findings highlighted the important connection between mental health challenges and psycho-social indicators such as social support and sense of community, while also revealing how religious influences shaped participants' understandings of holistic health and wellbeing as well as coping with past trauma. Indeed, although significant changes in mental health and wellbeing related outcomes were observed, given the structure of the study as a pilot intervention without a control group, strong conclusions cannot be made from post-intervention outcome data. Nonetheless, these preliminary findings suggest spirituality-based, peer-led approaches focused on holistic and religiously integrated understandings of health may have the potential to address mental health disparities among Black communities in the US, and further scaled up research is warranted.
Although the intervention's emphasis of holistic wellbeing through a spirituality-based, peer-led model of health promotion was novel in comparison to past research, findings support other spirituality-based interventions which have similarly observed improvements in depression (Hankerson & Weissman, 2012; Rogers & Stanford, 2015). Likewise, the advocated role of religious-coping in addressing health needs in Black communities and the importance of FBO-collaborations in health research were similarly supported by intervention outcomes (Hays, 2015). Importantly, improvements in overall wellbeing (assessed quantitatively through constructs such as flourishing in the current study and supported qualitatively through concepts related to general, integrated wellness) indicate the importance of evaluating these broader constructs in intervention design to capture potentially salient improvements in quality of life as part of similar spirituality-based, peer-led programs. Likewise, given that these impacts were observed despite the intervention occurring via virtual platforms, findings point to the applicability of virtual modalities of spirituality-based, peer-led intervention to improve health outcomes in Black communities and among older adults (particularly when in-person modes of engagement may face barriers, such as during the COVID-19 pandemic). Interestingly, despite the potential of virtual-platforms of intervention to limit the degree and quality of social engagement (Lowenthal et al., 2020), participants nonetheless noted that sense of community and social support were enhanced during the intervention, suggesting that such barriers can be overcome in virtual settings through similar interventional approaches.
The link between social support, sense of community, and mental health challenges observed in qualitative findings also corroborate past research showing the connection between these outcomes (Townley & Kloos, 2011; Uchino, 2006). Specifically, literature demonstrates that social support plays a significant role in mitigating certain symptoms of depression (such as feelings of loneliness and sadness), coping with mental health related stress and past trauma induced challenges, as well as in the prevention of further negative health consequences as a result of mental health concerns (such as suicidality and physical health deterioration) (Hale et al., 2005; Kleiman & Liu, 2013; Laffaye et al., 2008). Similarly, the link between enhanced sense of belonging and connection to others through an improved sense of community and mental health has been understood through exposure of health promoting behaviors and greater sense of commitment to one’s health through feelings of mutual respect and self-esteem (Berkman & Glass, 2000; House et al., 1988; Palis et al., 2020). Indeed, findings suggest that further community-based research targeting mental health (including spirituality-based and peer-led models) may benefit from targeting these constructs in intervention development as potential moderators or mediators in achieving improvements in mental health.
The importance of religion in mental health related challenges has also been widely supported in past research (O. Harrison et al., 2001; Shaw et al., 2005). Specifically, religious coping has been understood through the lens of both positive religious coping (e.g., seeking spiritual support and connection, religious purification and forgiveness) and negative religious coping (e.g., punitive religious reappraisals) (Pargament et al., 1998). In analyzing these complex religious influences that have been identified in past research, positive religious coping has largely centered around feelings of spiritual connectedness, beliefs that one's life has meaning, and strengthening one's relationship with a Higher Power as a means of addressing stress (Pargament et al., 1998); such conceptualizations closely mirror qualitative findings of how participants expressed their religiosity within the context of dealing with mental health challenges. However, while the role of religion in coping with trauma was reflected in qualitative findings, no significant changes in indicators of religious coping and the importance of religion in one's life were reflected in the quantitative findings post-intervention; this may reflect that, for participants (who on average had been attending religious congregations for multiple years), religion had already been playing a significant role in their lives.
Nonetheless, significant increases in the role of religion and spirituality in healthy choices and interactions were observed post intervention, which was also reflected qualitatively through participant components on feelings of improved diet and exercise, and how religion may have underpinned these improvements through understanding one's body as "a temple." The concept of the body as a "temple" has be highlighted in past research examining spirituality among Black communities and has similarly underscored the concept as a driver of positive health behaviors through an emphasis of valuing and improving one's body out of divine respect, informed by a holistic understanding of one's health (both physical and mental) (King et al., 2005). The saliency of this concept in the qualitative data directly aligns with interventional emphasis on holistic health and using religion as a driver to enhance one's spiritual, physical, and mental health. Indeed, such results suggest that similar intervention designs can particularly benefit from integrating the promotion of religion or spirituality into various facets of one's daily life (including broader health), and that spirituality-based interventions may benefit from conceptualizing health in a holistic manner to promote overall wellbeing along with specific health outcomes.
Finally, while changes related to sleep were not identified in the interview data and no changes in the amount of sleep were identified in the quantitative data, the proportion of participants reporting trouble falling or staying asleep significantly decreased. While improvements in sleep have been associated with positive mental health outcomes (Freeman et al., 2017), the lack of significant quantitative and qualitative findings suggest that improvements in sleep may play a lesser role in addressing mental health disparities among Black churchgoers, particularly in comparison to other factors such as social support and sense of community. However, since past research in faith-based settings has observed an important link with sleep outcomes and mental health (Oh et al., 2019), further research examining a wider array of sleep indictors (such as sleep quality or disturbances) is warranted.
There are some key limitations to this study that must be acknowledged. First, as a small-scale one-group pre-test post-test pilot study recruited using convenience sampling, we were unable to assess the efficacy of the intervention with a control group. Moreover, the convenience sampling approach targeted high attendance; future interventional research may benefit from recruiting participants with a wider range of congregational attendance, or by collaborating with mental health professionals to conduct a more needs-based recruitment of individuals suffering with depression. Importantly, it is possible that other social or environmental factors in participants' lives external to the intervention played a role in the observed changes in outcome variables. However, these preliminary results set the foundation for more scaled-up interventional research to examine the applicability of the interventional approach through more rigorous, controlled trials. Similarly, the recruited participants had a relatively high socio-economic standing in comparison to other residents in the Bronx (reflected through high educational attainment and lack of financial difficulties), however a positive interventional impact was still observed; future interventions may consider targeting more socio-economically disadvantaged sub-populations. Importantly, while mental health outcomes were only measured quantitatively through self-reported symptoms of depression and PTSD (as opposed to clinical diagnoses of these conditions), future studies may explore more diverse outcomes (such as anxiety or loneliness indicators) or involve the analysis of medical records. Similarly, while changes in physical health related behaviors (such as diet and exercise) were observed in qualitative findings, self-reported or objective measures of such health behaviors were not quantitatively examined, which is an area deserving of further exploration. The lack of statistically significant findings for some outcomes (such as PTSD) may also reflect sample size limitations, which also limited the ability to conduct quantitative interaction analyses with the mental health outcomes and psycho-social indicators; further scaled-up research can support corroboration of study findings and examination of outcome interactions (which were observed qualitatively in the current study). Finally, the disruptive social, economic, and health impact of the COVID-19 pandemic likely played a strong role in participant's experience of the intervention and the outcome variables assessed; further research may benefit from assessing COVID-19 impact related outcomes to adjust for in analyses.
Indeed, despite study limitations, findings highlight the feasibility and acceptability of such formats of remote spirituality-based, peer-led interventions among Black communities. By engaging with FBOs, working with participant peers as lay educators, and emphasizing a holistic approach through health and wellbeing, such programs have the potential to be scaled-up to improve various facets of health and wellbeing in diverse Black communities. Policy makers and community leaders seeking to address health disparities may also benefit from employing such collaborative, community-engaged interventional health promotion initiatives, although further research is needed to explore the adaptability of such collaborative approaches in more scaled-up settings.
References
Ai, A. L., Huang, B., Bjorck, J., & Appel, H. B. (2013). Religious attendance and major depression among Asian Americans from a national database: The mediation of social support. Psychology of Religion and Spirituality, 5, 78–89. https://doi.org/10.1037/a0030625
Andrasfay, T., & Goldman, N. (2021). Reductions in 2020 US life expectancy due to COVID-19 and the disproportionate impact on the Black and Latino populations. Proceedings of the National Academy of Sciences, 118(5), e2014746118. https://doi.org/10.1073/pnas.2014746118
Baciu, A., Negussie, Y., Geller, A., Weinstein, J. N., National Academies of Sciences, E., & Medicine. (2017). The state of health disparities in the United States. In Communities in action: Pathways to health equity. National Academies Press (US).
Batch, B., Ard, J., Vollmer, W., Funk, K., Appel, L., Stevens, V., Samuel-Hodge, C., Loria, C., Hollis, J., & Svetkey, L. (2013). Impact of participant and interventionist race concordance on weight loss outcomes. Obesity (Silver Spring, Md.), 21(4), 712–717. https://doi.org/10.1038/oby.2012.184
Berkman, L. F., & Glass, T. (2000). Social integration, social networks, social support, and health. Social Epidemiology, 1(6), 137–173.
Bhui, K., McCabe, R., Weich, S., Singh, S., Johnson, M., & Szczepura, A. (2013). THERACOM: A systematic review of the evidence base for interventions to improve Therapeutic Communications between black and minority ethnic populations and staff in specialist mental health services. Systematic Reviews, 2(1), 15. https://doi.org/10.1186/2046-4053-2-15
Blank, M. B., Mahmood, M., Fox, J. C., & Guterbock, T. (2002). Alternative mental health services: The role of the Black Church in the south. American Journal of Public Health, 92(10), 1668–1672. https://doi.org/10.2105/AJPH.92.10.1668
Bolger, D., Tinsley, C., & Ecklund, E. H. (2018). Heaven and health: How Black, Latino, and Korean Christians view the relationship between faith and health. Review of Religious Research, 60(3), 389–402. https://doi.org/10.1007/s13644-017-0321-6
Bor, J., Venkataramani, A. S., Williams, D. R., & Tsai, A. C. (2018). Police killings and their spillover effects on the mental health of black Americans: A population-based, quasi-experimental study. The Lancet, 392(10144), 302–310. https://doi.org/10.1016/S0140-6736(18)31130-9
Centers for Disease Control and Prevention (CDC). (2018). Well-Being Concepts. https://www.cdc.gov/hrqol/wellbeing.htm. Accessed 21 Sep 2021.
Chavis, D. M., Lee, K. S., & Acosta, J. D. (2008). The sense of community (SCI) Revised: The reliability and validity of the SCI-2. Paper presented at the 2nd International Community Psychology Conference, Lisboa, Portugal.
Chu, P. S., Saucier, D. A., & Hafner, E. (2010). Meta-analysis of the relationships between social support and well-being in children and adolescents. Journal of Social and Clinical Psychology, 29(6), 624–645. https://doi.org/10.1521/jscp.2010.29.6.624
de Quadros-Wander, S., McGillivray, J., & Broadbent, J. (2014). The influence of perceived control on subjective wellbeing in later life. Social Indicators Research, 115(3), 999–1010.
Druss, B. G., Zhao, L., von Esenwein, S. A., Bona, J. R., Fricks, L., Jenkins-Tucker, S., Sterling, E., DiClemente, R., & Lorig, K. (2010). The health and recovery peer (HARP) program: A peer-led intervention to improve medical self-management for persons with serious mental illness. Schizophrenia Research, 118(1), 264–270. https://doi.org/10.1016/j.schres.2010.01.026
Dubowitz, T., Nelson, C., Weilant, S., Sloan, J., Bogart, A., Miller, C., & Chandra, A. (2020). Factors related to health civic engagement: Results from the 2018 National Survey of Health Attitudes to understand progress towards a Culture of Health. BMC Public Health, 20(1), 635–635. https://doi.org/10.1186/s12889-020-08507-w
Edwards, F., Esposito, M. H., & Lee, H. (2018). Risk of police-involved death by race/ethnicity and place, United States, 2012–2018. American Journal of Public Health, 108(9), 1241–1248. https://doi.org/10.2105/AJPH.2018.304559
Eke, A. N., Wilkes, A. L., & Gaiter, J. (2010). Organized religion and the fight against HIV/AIDS in the Black community: The role of the Black Church. In D. H. McCree, K. T. Jones, & A. O’Leary (Eds.), African Americans and HIV/AIDS: Understanding and Addressing the Epidemic (pp. 53–68). Springer.
Fisher, J. W., Francis, L. J., & Johnson, P. (2000). Assessing spiritual health via four domains of spiritual wellbeing: The SH4DI. Pastoral Psychology, 49(2), 133–145.
Fortuna, K. L., Naslund, J. A., LaCroix, J. M., Bianco, C. L., Brooks, J. M., Zisman-Ilani, Y., Muralidharan, A., & Deegan, P. (2020). Digital peer support mental health interventions for people with a lived experience of a serious mental illness: Systematic review. JMIR Ment Health, 7(4), e16460. https://doi.org/10.2196/16460
Freeman, D., Sheaves, B., Goodwin, G. M., Yu, L.-M., Nickless, A., Harrison, P. J., Emsley, R., Luik, A. I., Foster, R. G., & Wadekar, V. (2017). The effects of improving sleep on mental health (OASIS): A randomised controlled trial with mediation analysis. The Lancet Psychiatry, 4(10), 749–758.
Fryer, C. S., Passmore, S. R., Maietta, R. C., Petruzzelli, J., Casper, E., Brown, N. A., Butler, J., Garza, M. A., Thomas, S. B., & Quinn, S. C. (2016). The symbolic value and limitations of racial concordance in minority research engagement. Qualitative Health Research, 26(6), 830–841. https://doi.org/10.1177/1049732315575708
Gale, R. C., Wu, J., Erhardt, T., Bounthavong, M., Reardon, C. M., Damschroder, L. J., & Midboe, A. M. (2019). Comparison of rapid vs in-depth qualitative analytic methods from a process evaluation of academic detailing in the Veterans Health Administration. Implementation Science, 14(1), 11. https://doi.org/10.1186/s13012-019-0853-y
Ghaderi, A., Tabatabaei, S. M., Nedjat, S., Javadi, M., & Larijani, B. (2018). Explanatory definition of the concept of spiritual health: A qualitative study in Iran. Journal of Medical Ethics and History of Medicine, 11, 3–3.
Global Wellness Institute. (n.d.). What is wellness?. https://globalwellnessinstitute.org/what-is-wellness/. Accessed 21 Sep 2021.
Gold, J. A., Rossen, L. M., Ahmad, F. B., Sutton, P., Li, Z., Salvatore, P. P., Coyle, J. P., DeCuir, J., Baack, B. N., & Durant, T. M. (2020). Race, ethnicity, and age trends in persons who died from COVID-19—United States, May–August 2020. Morbidity and Mortality Weekly Report, 69(42), 1517.
Grier-Reed, T. (2013). The African American student network: An informal networking group as a therapeutic intervention for Black College students on a predominantly white campus. Journal of Black Psychology, 39(2), 169–184. https://doi.org/10.1177/0095798413478696
Hale, C. J., Hannum, J. W., & Espelage, D. L. (2005). Social support and physical health: The importance of belonging. Journal of American College Health, 53(6), 276–284.
Hankerson, S. H., & Weissman, M. M. (2012). Church-based health programs for mental disorders among African Americans: A review. Psychiatric Services, 63(3), 243–249.
Harrison, O. M., Koenig, H. G., Hays, J. C., Eme-Akwari, A. G., & Pargament, K. I. (2001). The epidemiology of religious coping: A review of recent literature. International Review of Psychiatry, 13(2), 86–93. https://doi.org/10.1080/09540260124356
Hays, K. (2015). Black Churches’ capacity to respond to the mental health needs of African Americans. Social Work & Christianity, 42(3).
House, J. S., Landis, K. R., & Umberson, D. (1988). Social relationships and health. Science, 241(4865), 540–545. https://doi.org/10.1126/science.3399889
Huang, F. Y., Chung, H., Kroenke, K., Delucchi, K. L., & Spitzer, R. L. (2006). Using the patient health questionnaire-9 to measure depression among racially and ethnically diverse primary care patients. Journal of General Internal Medicine, 21(6), 547–552.
Israel, B. A., Schulz, A. J., Parker, E. A., Becker, A. B., Allen, A. J., Guzman, J. R., & Lichtenstein, R. (2017). Critical issues in developing and following CBPR principles. Community-Based Participatory Research for Health: Advancing Social and Health Equity, 3, 32–35.
King, S. V., Burgess, E. O., Akinyela, M., Counts-Spriggs, M., & Parker, N. (2005). “Your body is god’s temple”: The spiritualization of health beliefs in multigenerational African American Families. Research on Aging, 27(4), 420–446. https://doi.org/10.1177/0164027505276315
Kleiman, E. M., & Liu, R. T. (2013). Social support as a protective factor in suicide: Findings from two nationally representative samples. Journal of Affective Disorders, 150(2), 540–545.
Kroenke, K., Spitzer, R. L., & Williams, J. B. (2001). The PHQ-9: Validity of a brief depression severity measure. Journal of General Internal Medicine, 16(9), 606–613.
Lachman, M. E., & Weaver, S. L. (1998). The sense of control as a moderator of social class differences in health and well-being. Journal of Personality and Social Psychology, 74(3), 763.
Laffaye, C., Cavella, S., Drescher, K., & Rosen, C. (2008). Relationships among PTSD symptoms, social support, and support source in veterans with chronic PTSD. Journal of Traumatic Stress: Official Publication of the International Society for Traumatic Stress Studies, 21(4), 394–401.
Lee-Tauler, S. Y., Eun, J., Corbett, D., & Collins, P. Y. (2018). A systematic review of interventions to improve initiation of mental health care among racial-ethnic minority groups. Psychiatric Services, 69(6), 628–647. https://doi.org/10.1176/appi.ps.201700382
Lowenthal, P., Borup, J., West, R., & Archambault, L. (2020). Thinking beyond Zoom: Using asynchronous video to maintain connection and engagement during the COVID-19 pandemic. Journal of Technology and Teacher Education, 28(2), 383–391.
Massey, C. N., Feig, E. H., Duque-Serrano, L., Wexler, D., Moskowitz, J. T., & Huffman, J. C. (2019). Well-being interventions for individuals with diabetes: A systematic review. Diabetes Research and Clinical Practice, 147, 118–133. https://doi.org/10.1016/j.diabres.2018.11.014
McGregor, B., Li, C., Baltrus, P., Douglas, M., Hopkins, J., Wrenn, G., Holden, K., Respress, E., & Gaglioti, A. (2020). Racial and ethnic disparities in treatment and treatment type for depression in a national sample of Medicaid recipients. Psychiatric Services, 71(7), 663–669. https://doi.org/10.1176/appi.ps.201900407
Moser, A., Stuck, A. E., Silliman, R. A., Ganz, P. A., & Clough-Gorr, K. M. (2012). The eight-item modified Medical Outcomes Study Social Support Survey: Psychometric evaluation showed excellent performance. Journal of Clinical Epidemiology, 65(10), 1107–1116. https://doi.org/10.1016/j.jclinepi.2012.04.007
New York State Health Foundation. (2019). New York state’s county health rankings in national perspective. https://nyshealthfoundation.org/wp-content/uploads/2019/09/new-york-state-county-health-rankings-national-perspective-sep-2019.pdf. Accessed 21 Sep 2021.
Nguyen, A. W. (2020). Religion and mental health in racial and ethnic minority populations: A review of the literature. Innovation in Aging, 4(5). https://doi.org/10.1093/geroni/igaa035
Oh, H., Ko, J., & Waldman, K. (2019). Church-based sleep screenings to detect mental health problems among Korean-Americans. Journal of Immigrant and Minority Health, 21(6), 1440–1443. https://doi.org/10.1007/s10903-019-00861-1
Osorio, H. R. (2005). Spiritual accompaniment during the spiritual exercises according to ST. Ignatius of Loyola., 108, 19.
Palis, H., Marchand, K., & Oviedo-Joekes, E. (2020). The relationship between sense of community belonging and self-rated mental health among Canadians with mental or substance use disorders. Journal of Mental Health, 29(2), 168–175.
Pargament, K. I., Smith, B. W., Koenig, H. G., & Perez, L. (1998). Patterns of positive and negative religious coping with major life stressors. Journal for the Scientific Study of Religion, 710–724.
Park, J. J., & Millora, M. (2010). Psychological well-being for White, Black, Latino/a, and Asian American Students: Considering spirituality and religion. Journal of Student Affairs Research and Practice, 47(4), 445–461. https://doi.org/10.2202/1949-6605.6143
Patalay, P., Annis, J., Sharpe, H., Newman, R., Main, D., Ragunathan, T., Parkes, M., & Clarke, K. (2017). A pre-post evaluation of OpenMinds: A sustainable, peer-led mental health literacy programme in universities and secondary schools. Prevention Science, 18(8), 995–1005. https://doi.org/10.1007/s11121-017-0840-y
Pozzi, M., Marta, E., Marzana, D., Gozzoli, C., & Ruggieri, R. A. (2014). The effect of the psychological sense of community on the psychological well-being in older volunteers. Europe’s Journal of Psychology, 10(4), 598–612.
Quiñones, A. R., Botoseneanu, A., Markwardt, S., Nagel, C. L., Newsom, J. T., Dorr, D. A., & Allore, H. G. (2019). Racial/ethnic differences in multimorbidity development and chronic disease accumulation for middle-aged adults. PLoS ONE, 14(6), e0218462. https://doi.org/10.1371/journal.pone.0218462
Ramchand, R., Ahluwalia, S. C., Xenakis, L., Apaydin, E., Raaen, L., & Grimm, G. (2017). A systematic review of peer-supported interventions for health promotion and disease prevention. Preventive Medicine, 101, 156–170. https://doi.org/10.1016/j.ypmed.2017.06.008
Repper, J., & Carter, T. (2011). A review of the literature on peer support in mental health services. Journal of Mental Health, 20(4), 392–411. https://doi.org/10.3109/09638237.2011.583947
Roberts, A. L., Gilman, S. E., Breslau, J., Breslau, N., & Koenen, K. C. (2011). Race/ethnic differences in exposure to traumatic events, development of post-traumatic stress disorder, and treatment-seeking for post-traumatic stress disorder in the United States. Psychological Medicine, 41(1), 71–83. https://doi.org/10.1017/S0033291710000401
Rogers, E. B., & Stanford, M. S. (2015). A church-based peer-led group intervention for mental illness. Mental Health, Religion & Culture, 18(6), 470–481. https://doi.org/10.1080/13674676.2015.1077560
Russell, R. D., Black, L. J., Pham, N. M., & Begley, A. (2020). The effectiveness of emotional wellness programs on mental health outcomes for adults with multiple sclerosis: A systematic review and meta-analysis. Multiple Sclerosis and Related Disorders, 44, 102171. https://doi.org/10.1016/j.msard.2020.102171
San Diego Association of Governments (SANDAG). (2020). San Diego Crime Victims and Suspects in 2019. https://www.sandag.org/uploads/publicationid/publicationid_4683_27645.pdf. Accessed 21 Sep 2021.
Seabury, S. A., Terp, S., & Boden, L. I. (2017). Racial and ethnic differences in the frequency of workplace injuries and prevalence of work-related disability. Health Affairs (project Hope), 36(2), 266–273. https://doi.org/10.1377/hlthaff.2016.1185
Shaw, A., Joseph, S., & Linley, P. A. (2005). Religion, spirituality, and posttraumatic growth: A systematic review. Mental Health, Religion & Culture, 8(1), 1–11. https://doi.org/10.1080/1367467032000157981
Stoewen, D. L. (2015). Health and wellness. The Canadian Veterinary Journal = La Revue Veterinaire Canadienne, 56(9), 983–984.
Stoewen, D. L. (2017). Dimensions of wellness: Change your habits, change your life. The Canadian Veterinary Journal = La Revue Veterinaire Canadienne, 58(8), 861–862.
Tan, S.-Y. (2013). Addressing religion and spirituality from a cognitive-behavioral perspective. In APA handbook of psychology, religion, and spirituality (Vol 2): An applied psychology of religion and spirituality (pp. 169–187). American Psychological Association. https://doi.org/10.1037/14046-008
Tang, T. S., Funnell, M. M., Sinco, B., Spencer, M. S., & Heisler, M. (2015). Peer-led, empowerment-based approach to self-management efforts in diabetes (PLEASED): A randomized controlled trial in an African American community. The Annals of Family Medicine, 13(Suppl 1), S27–S35.
Townley, G., & Kloos, B. (2011). Examining the Psychological Sense of Community for Individuals with Serious Mental Illness Residing in Supported Housing Environments. Community Mental Health Journal, 47(4), 436–446. https://doi.org/10.1007/s10597-010-9338-9
U. S. Department of Veterans Affairs. (2021). PTSD Checklist for DSM-5 (PCL-5). https://www.ptsd.va.gov/professional/assessment/adult-sr/ptsd-checklist.asp. Accessed 21 Sep 2021.
Uchino, B. N. (2006). Social support and health: A review of physiological processes potentially underlying links to disease outcomes. Journal of Behavioral Medicine, 29(4), 377–387.
Underwood, L. G. (2011). The Daily Spiritual Experience Scale: Overview and results. Religions, 2(1). https://doi.org/10.3390/rel2010029
United States Census Bureau. (2019). Quick facts (Bronx County). https://www.census.gov/quickfacts/fact/table/bronxcountynewyork,NY/PST045219. Accessed 21 Sep 2021.
VanderWeele, T. J. (2017). On the promotion of human flourishing. Proceedings of the National Academy of Sciences, 114(31), 8148–8156.
Weinberger, A. H., Gbedemah, M., Martinez, A. M., Nash, D., Galea, S., & Goodwin, R. D. (2018). Trends in depression prevalence in the USA from 2005 to 2015: Widening disparities in vulnerable groups. Psychological Medicine, 48(8), 1308–1315. https://doi.org/10.1017/S0033291717002781
Whinnery, J., Jackson, N., Rattanaumpawan, P., & Grandner, M. A. (2014). Short and long sleep duration associated with race/ethnicity, sociodemographics, and socioeconomic position. Sleep, 37(3), 601–611. https://doi.org/10.5665/sleep.3508
Williams, Q., Ochsner, M., Marshall, E., Kimmel, L., & Martino, C. (2010). The impact of a peer-led participatory health and safety training program for Latino day laborers in construction. Journal of Safety Research, 41(3), 253–261. https://doi.org/10.1016/j.jsr.2010.02.009
Wong, B., Bernstein, S., Jay, J., & Siegel, M. (2020). Differences in racial disparities in firearm homicide across cities: The role of racial residential segregation and gaps in structural disadvantage. Journal of the National Medical Association, 112(5), 518–530. https://doi.org/10.1016/j.jnma.2020.05.014
Yeary, K. H. K., Klos, L. A., & Linnan, L. (2012). The examination of process evaluation use in church-based health interventions: A systematic review. Health Promotion Practice, 13(4), 524–534.
Acknowledgements
This work was supported by the Robert Wood Johnson Foundation (RWJF; Grant 76643). For more detailed information on the curriculum used as part of this intervention, please contact the corresponding author.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ali, S.H., Mohsin, F.M., Banks, A. et al. Peer-Led, Remote Intervention to Improve Mental Health Outcomes Using a Holistic, Spirituality-Based Approach: Results from a Pilot Study. Community Ment Health J 58, 862–874 (2022). https://doi.org/10.1007/s10597-021-00893-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10597-021-00893-8