Abstract
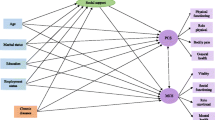
The primary objective of the present study was to assess independent and interactive relations of perceived social support and self-efficacy with four quality of life (QOL) domains namely physical, psychological, social, and environmental in cardiovascular disease (CVD) patients from a South Asian region. Participants were 172 (age 22–60 years) patients recruited from three major government sector hospitals from the fifth biggest city of South Asia. It was found that overall CVD patients had a better QOL in psychological and environmental domains compared to social and psychological. Furthermore, findings from hierarchical regression analyses indicated that perceived social support and self-efficacy were positively associated with the four QOL domains. Besides main effects, a synergistic interaction between social support and self-efficacy emerged indicating that perceived social support was strongly associated with physical and social QOL in CVD patients who had higher self-efficacy levels, while, perceived social support was weakly associated with the physical and social QOL in CVD patients who had lower self-efficacy levels.


Similar content being viewed by others
References
American Association of Cardiovascular and Pulmonary Rehabilitation. (2013). Guidelines for cardiac rehabilitation and secondary prevention programs. Champaign, IL: Human Kinetics.
Arnold, R., Ranchor, A. V., DeJongste, M. J., Koeter, G. H., Ten Hacken, N. H., Aalbers, R., et al. (2005). The relationship between self-efficacy and self-reported physical functioning in chronic obstructive pulmonary disease and chronic heart failure. Behavioral Medicine, 31, 107–115.
Bandura, A. (1997). Self-efficacy: The exercise of control. New York: Freeman.
Bandura, A. (2000). Health promotion from the perspective of social cognitive theory. In P. Norman, C. A. Abraham, & M. Conner (Eds.), Understanding and changing health behavior: From health belief to self-regulation (pp. 299–339). Amsterdam: Harwood Academic.
Bandura, A. (2004). Health promotion by social cognitive means. Health Education and Behavior, 31, 143–164. https://doi.org/10.1177/1090198104263660.
Barbareschi, G., Sanderman, R., Leegte, I. L., Van Veldhuisen, D. J., & Jaarsma, T. (2011). Educational level and the quality of life of heart failure patients: A longitudinal study. Journal of Cardiac Failure, 17(1), 47–53. https://doi.org/10.1016/j.cardfail.2010.08.005.
Bosworth, H. B., Siegler, I. C., Olsen, M. K., Brummet, B. H., Barefoot, J. C., Williams, N. E., et al. (2000). Social support and quality of life in patients with coronary artery disease. Quality of Life Research, 9, 829–839.
Brawley, L. R., Rejeski, W. J., & Lutes, L. (2000). A group-mediated cognitive-behavioral intervention for increasing adherence to physical activity in older adults. Journal of Applied Biobehavioral Research, 5(1), 47–65. https://doi.org/10.1111/j.1751-9861.2000.tb00063.
Brink, E. (2009). Adaptation positions and behaviour among post-myocardial infarction patients. Clinical Nursing Research, 18, 119–135. https://doi.org/10.1177/1054773809332326.
Buckworth, J., & Dishman, R. K. (2002). Exercise psychology. Champaign: Human Kinetics.
Cohen, S., Kaplan, J. R., & &Manuck, S. B. (1994). Social support and coronary heart disease: Underlying psychological and biological mechanisms. In S. A. Shumaker & S. M. Czajkowski (Eds.), Social support and cardiovascular disease (pp. 195–221). New York: Plenum Press.
Cohen, S., & Wills, T. A. (1985). Stress, social support, and the buffering hypothesis. Psychological Bulletin, 98(2), 310–357.
Compare, A., Zarbo, C., Manzoni, G. M., Castelnuovo, G., Baldassari, E., Bonardi, A., … Romagnoni, C. (2013). Social support, depression, and heart disease: A ten year literature review. Frontiers in Psychology, 4, 384. https://doi.org/10.3389/fpsyg.2013.00384.
Dishman, R. K., Saunders, R. P., Motl, R. W., Dowda, M., & Pate, R. R. (2009). Self-efficacy moderates the relation between declines in physical activity and perceived social support in high school girls. Journal of Pediatric Psychology, 34(4), 441–451. https://doi.org/10.1093/jpepsy/jsn100.
Dracup, K., Walden, J. A., Stevenson, L. W., & Bracht, M. L. (1992). Quality of life in patients with advanced heart failure. Journal of Heart and Lung Transplant, 11, 273–279.
Duenas, M., Ramirez, C., Arana, R., & Failde, I. (2011). Gender differences and determinants of health related quality of life in coronary patients: A follow-up study. BioMed Central Journal of Cardiovascular Disorders, 11, 24. https://doi.org/10.1186/1471-2261-11-24.
Fleck, M., Louzada, S., Xavier, M., Chachamovich, E., Vieira, G., Santos, L., & Pinzon, V. (2000). Application of the Portuguese version of the abbreviated instrument of quality life WHOQOL-BREF. Revista de Saude Publica, 34, 178–183. https://doi.org/10.1590/S0034-89102000000200012.
Gallant, M. P. (2003). The influence of social support on chronic illness self-management: A review and directions for research. Health, Education & Behavior, 30, 170–195. https://doi.org/10.1177/1090198102251030.
Gaziano, T., Reddy, S., Paccaud, F., Horton, S., & Chaturvedi, V. (2006). Cardiovascular disease. In D. T. Jamison, J. G. Breman, A. R. Measham et al. (Eds.), Disease control priorities in developing countries (2nd ed.). Washington, DC: World Bank.
Goble, A. J., & Worcester, M. U. (1999). Best practice guidelines for cardiac rehabilitation and secondary prevention (1st ed.). Victoria: Department of Human Services.
Graham, I. (2007). European guidelines on cardiovascular disease prevention in clinical practice: Executive summary. Fourth Joint Task Force of the European Society of Cardiology and Other Societies on Cardiovascular Disease Prevention in Clinical Practice. European Heart Journal, 28(19), 2375–2414. https://doi.org/10.1093/eurheartj/ehm316.
Hamilton, K., Warner, L. M., & Schwarzer, R. (2017).The role of self-efficacy and friend support on adolescent vigorous physical activity. Health, Education & Behavior, 44(1), 175–181. https://doi.org/10.1177/1090198116648266.
Hogan, B. E., Linden, W., & Najarian, B. (2002). Social support interventions. Do they work? Clinical Psychology Review, 22, 381–440. https://doi.org/10.1016/S0272-7358(01)00102-7.
Jibeen, T., & Khalid, R. (2010). Development and preliminary validation of Multidimensional Acculturative Stress Scale for Pakistani immigrants in Toronto, Canada. International Journal of Intercultural Relations, 34(3), 233–243. https://doi.org/10.1016/j.ijintrel.2009.09.006.
Joekes, K., Elderen, J., Schreurs, T. V., K (2007). Self-efficacy and self protection are related to quality of life, psychological well-being and self-management in cardiac patients. Journalof Health Psychology, 112(1), 4–16. https://doi.org/10.1177/1359105306069096.
Johansson, P., Agnebrink, M., Dahlstrom, U., & Brostrom, A. (2004). Measurement of health-related quality of life in chronic heart failure, from a nursing perspective—A review of the literature. European Journal of Cardiovascular Nursing, 3(1), 7–20. https://doi.org/10.1016/j.ejcnurse.2003.09.004.
Jose, P. E. (2013). ModGraph-I: A programme to compute cell means for the graphical display of moderational analyses: The internet version, Version 3.0. New Zealand: Victoria University of Wellington. Retrieved from http://pavlov.psyc.vuw.ac.nz/paul-jose/modgraph/.
Khan, M. N., Akhter, M. S., Ayub, M., Alam, S., & Laghari, N. U. (2003). Translation and validation of quality of life scale, the brief version. Journal of the College of Physicians and Surgeons—Pakistan, 13(2), 98–100.
Kulik, J. A., & Mahler, H. I. M. (1993). Emotional support as a moderator of adjustment and compliance after coronary bypass surgery: A longitudinal study. Journal of Behavioral Medicine, 16, 45–63. https://doi.org/10.1007/BF00844754.
Lett, H. S., Blumenthal, J. A., Babyak, M. A., Strauman, T. J., Robins, C., & Sherwood, A. (2005). Social support and coronary heart disease: Epidemiologic evidence and implications for treatment. Psychosomatic Medicine, 67(6), 869–878.
Malik, S., & Afzal, N. (2015). Predictors of quality of life and resilience among outpatients with heart diseases. Journal of Pakistan Psychiatric Society, 12(3), 31–33.
Martiniuk, A. L., Lee, C. M., Lawes, C. M., Ueshima, H., Suh, I., Lam, T. H., et al. (2007). Hypertension: Its prevalence and population attributable fraction for mortality from cardiovascular disease in the Asia-Pacific region. Journal of Hypertension, 25, 73–79. https://doi.org/10.1097/HJH.0b013e328010775f.
Molloy, G. J., Hamer, M., Randall, G., & Chida, Y. (2008). Marital status and cardiac rehabilitation attendance: A meta-analysis. European Journal of Preventive Cardiology, 15(5), 557–561. https://doi.org/10.1097/HJR.0b013e3283063929.
Molloy, G. J., Perkins-Porras, L., Strike, P. C., & Steptoe, A. (2008). Social networks and partner stress as predictors of adherence to medication, rehabilitation attendance, and quality of life following acute coronary syndrome. Health Psychology, 27(1), 52–58. https://doi.org/10.1037/0278-6133.27.1.52.
Murberg, T. A., & Bru, E. (2001). Social relationships and mortality in patients with congestive heart failure. Journal of Psychosomatic Research, 51(3), 521–527. https://doi.org/10.1016/S0022-3999(01)00226-4.
Orth-Gomer, K. (2000). Stress and social support in relation to cardiovascular health. In P. M. McGabe, N. Schneiderman, T. Field, & A. R. Wellens (Eds.), Stress, coping andcardiovascular disease (pp. 229–240). Mahwah: Lawrence Erlbaum Associates.
Pakistan Bureau of Statistics. (1998). Census report of Pakistan. Tech. Rep. No. 160. Islamabad: Population Census Organization Statistics Division, Government of Pakistan.
Pillai, H. S., & Ganapathi, S. (2013). Heart failure in South Asia. Current Cardiovascular Review, 9(2), 102–111. https://doi.org/10.2174/1573403X11309020003.
Rajati, F., Sadeghi, M., Feizi, A., Sharifirad, G., Hasandokht, T., & Mostafavi, F. (2014). Self-efficacy strategies to improve exercise in patients with heart failure: A systematic review. ARYA Atherosclerosis, 10(6), 319–333.
Reblin, M., & Uchino, B. N. (2008). Social and emotional support and its implication for health. Current Opinion in Psychiatry, 21(2), 201–205. https://doi.org/10.1097/YCO.0b013e3282f3ad89.
Rook, K. S. (1984). Promoting social bonding: Strategies for helping the lonely and socially isolated. American Psychologist, 39, 1389–1407. https://doi.org/10.1037/0003-066X.39.12.1389.
Sarkar, U., Ali, S., & &Whooley, M. A. (2007). Self-efficacy and health status in patients with coronary heart disease: Findings from the heart and soul study. Psychosomatic Medicine, 69, 306–312. https://doi.org/10.1097/PSY.0b013e3180514d57.
Schwarzer, R., & Jerusalem, M. (1995). Generalized self-efficacy scale. In J. Weinman, S. Wright, & M. Johnston (Eds.), Measures in health psychology: A user’s portfolio. Causal and control beliefs (pp. 35–37). Windsor: NFER-NELSON.
Tabassum, U., Rehman, G., Schwarzer, R., & Jerusalem, M. (2003). Urdu adaptation of the General Self-Efficacy Scale. Retrieved from http://userpage.fuberlin.de/~health/urdu.htm.
The World Health Organization. (2002). Reducing risks, promoting healthy life. Geneva: World Health Report. https://doi.org/10.1001/jama.288.16.1974.
Veenstra, M., Pettersen, K. I., Rollag, A., & Stavem, K. (2004). Association of changes in health-related quality of life in coronary heart disease with coronary procedures and sociodemographic characteristics. Health and Quality of Life Outcomes, 2, 56. https://doi.org/10.1186/1477-7525-2-56.
Warner, L. M., Ziegelmann, J. P., Schüz, B., Wurm, S., & Schwarzer, R. (2011). Synergistic effect of social support and self-efficacy on physical exercise in older adults. Journal of Aging and Physical Activity, 19(3), 249–261. https://doi.org/10.1123/japa.19.3.249.
Williams, R. B., Barefoot, J. C., Califf, R. M., Haney, T. L., Saunders, W. B., Pryor, D. B., … Mark, D. B. (1992). Prognostic importance of social and economic resources among medically treated patients with angiographically documented coronary artery disease. The Journal of American Medical association, 267(4), 520–524. https://doi.org/10.1001/jama.1992.03480040068032.
Woodgate, J., Brawley, L. R., & Shields, C. A. (2007). Social support in cardiac rehabilitation exercise maintenance: Associations with self-efficacy and health-related quality of life. Journal of Applied Social Psychology, 37(5), 1041–1059. https://doi.org/10.1111/j.1559-1816.2007.00198.x.
Zimet, G. D., Dahlem, N. W., Zimet, S. G., & Farley, G. K. (1988). The multidimensional scale of perceived social support. Journal of Personality Assessment, 52(1), 30–41. https://doi.org/10.1207/s15327752jpa5201_2.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fatima, S., Jibeen, T. Interplay of Self-efficacy and Social Support in Predicting Quality of Life in Cardiovascular Patients in Pakistan. Community Ment Health J 55, 855–864 (2019). https://doi.org/10.1007/s10597-018-0361-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10597-018-0361-6