Abstract
The combination of depression and anxiety is among the most prevalent comorbidities of disorders leading to substantial functional impairment in children and adolescents. The network perspective offers a new paradigm for understanding and measuring psychological constructs and their comorbidity. The present study aims to apply network analysis to explore the comorbidity between depression and anxiety symptoms. Specifically, the study examines bridge symptoms, comorbidity, and shortest pathway networks and estimates the impact of the symptoms in the network’s connectivity and structure. The findings show that “feeling lonely” and “feeling unloved” are identified as the most central bridge symptoms. The shortest path network suggests that the role of a mixed anxiety-depressive symptomatology, and specific and non-specific symptoms of clinical criteria, such as “worries,” “feels depressed,” “fears school,” and “talks about suicide” could serve as a warning for comorbidity.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
From a standard symptomatological and interdisciplinary perspective, studies in the area of health have confirmed that comorbidity of two or more mental disorders occurs at rates higher than those expected by chance [1,2,3,4]. This comorbidity, or joint occurrence, means that an individual is affected by two or more different disorders at the same time. However, comorbidity can be based on different perspectives. Traditionally, there have been two different frameworks: a clinical interpretation framework (i.e., categorical criteria and clinical judgment) and a psychometric or dimensional framework (i.e., assuming the latent variables as proxies of diagnoses). Within a psychometric framework, comorbidity is generally conceptualized as a (bi)directional relationship between two latent variables (i.e., disorders as a cluster of directly related symptoms) that underlie a set of symptoms. More currently, from a network approach [1, 3, 5, 6] focused on individual symptoms and their associations, comorbidity of the two disorders can be explained by specific cross-connections among items from these disorders (i.e., overlapping symptoms/bridge symptoms) instead of either a correlation between two disorders or as the result of a common underlying (neurobiological) dysfunction or “super disorder” [7]. From the network perspective, comorbidity exists when mental disorders have shared symptoms [3, 5, 6], a phenomenon that has become the rule rather than the exception, particularly during childhood and adolescence [1, 8].
The phenomenon of comorbidity is related to an increase in severity, poorer treatment results, increased health system costs, and higher suicide rates [9, 10], underlining the urgent need to study, understand, and address this issue. Depression and anxiety are among the most prevalent comorbid disorders, especially in child and adolescent populations [11,12,13,14,15]; this is alarming because each disorder is independently associated with substantial functional impairment and future mental health problems. Together, they represent a far greater threat to health (e.g., functional impairment, substance abuse, and poorer response to treatment) [16,17,18,19,20].
Although anxiety and depression in youth are meaningfully linked, different theoretical models have proposed important distinctions [11]. According to the tripartite model, high physiological arousal is specific to anxiety, while low positive affectivity is specific to depression; however, both share a common component, namely high negative affectivity [21, 22]. The tripartite structure consisting of general distress, physiological hyperarousal (specific anxiety), and anhedonia (specific depression) shares a significant nonspecific component with the anxious and depressed syndromes. This component encompasses general affective distress (negative affect).This tripartite view implies that a complete description of the affective domain requires assessing both the common and the unique elements of the syndromes. Dysfunctional high negative affect essentially signals the presence of either of these disorders (anxiety-depression diagnoses) and differentiation of depression and anxiety is provided by the two specific factors: children who report not only very high levels of general distress, but also both anhedonia and psychophysiological hyperarousal, will be diagnosed as mixed anxiety-depression. However, each disorder will be characterized by general components (conceptualized as negative affectivity or general distress) that contribute to comorbidity among disorders, as well as specific or narrow components that distinguish them (i.e., anxious arousal for anxiety, anhedonia or low positive affectivity for depression). In other words, high negative affect leads to vulnerability of both mood and anxiety disorders, whereas low positive affect is related to depression and high positive affect is related to anxiety.
Differential emotions theory postulates that, as an emotion is experienced, it becomes associated with other emotions such that specific emotions tend to occur together or may influence the expression of other emotions. For instance, the emotions of joy, shame, and guilt account for the largest amount of variance in depression scores [23]. From this perspective, disorder comorbidity data between anxiety and depression are likely to reflect shared etiological processes based on a two-factor structure of internalizing disorders: fear disorders (i.e., anxiety disorders or symptoms), and anxious-mood disorders (i.e., depression disorders or symptoms). Thus, the two disorders may have similar emotional features; however, the predominant emotion in anxiety is fear, whereas in depression it is sadness [24,25,26].
The multiple pathways model suggested by Cummings et al. [13] adopts the central proposition of the tripartite model distinguishing between fear and distress while also considering heterogeneity among anxiety disorders [13, 27]. Accordingly, some shared and stratified risk factors contribute to the development of the comorbid disorder from multiple potential pathways: (a) youths with a diathesis for anxiety, with subsequent comorbid depression resulting from anxiety-related impairment (Pathway 1); (b) youths with a shared diathesis for anxiety and depression, who may experience both disorders simultaneously (Pathway 2); (c) youths with a diathesis for depression, with subsequent comorbid anxiety resulting from depression-related impairment (Pathway 3). Under this model, anxiety and depression are viewed from both categorical and dimensional perspectives, because examining symptoms or performing diagnosis can lead to different conclusions about the order of onset of anxiety and depressive disorders [13].
On the basis of these models, multiple conceptual explanations could be provided for comorbidity. Among other reasons, disorders could co-occur because they share the same diathesis (i.e., neuroticism, behavioral inhibition), genetic factors, major life events (e.g., loss of a loved one), social-cognitive risk factors, or because one disorder (or some specific symptoms) can trigger the onset of another disorder.
Traditionally, as with many other psychological constructs, the measurement of the relationship between anxiety and depression has been explored methodologically based on the proposition of the reflective latent variable models, which consider the items reflecting the manifestation of a latent variable or those reflecting an underlying psychological construct or entity [28, 29]. However, in recent years, the network perspective has changed the way psychological constructs are understood and measured. In this perspective, psychological attributes exist as systems whose components are autonomous causal entities that mutually influence each other [3, 29], while highly “central” symptoms (those with stronger inter-symptom connections) spread symptom activation throughout the network [30].
The associations within the system can be examined through two key analytical approaches. One approach involves computing regularized partial correlations networks using a penalized algorithm that ensures only the most significant relationships remain. The other utilizes centrality indices (strength, betweenness, closeness, and expected influence) to identify the nodes that have the strongest edges, lead to the shortest distance, and act as the best intermediaries between the connected components [31,32,33]. The dynamic perspective of this analytical approach makes it possible to identify the shortest path between specific nodes in the network by visually highlighting the most significant edges within it [34], and to analyze the individual node impact in a network by estimating whether networks could vary in structure and connectivity depending on the levels of symptoms [35].
Comorbidity has been explored using a network perspective in multiple studies [30]. Cramer et al. [2] hypothesize that it arises when there are symptoms (e.g., sleep disturbances and fatigue, concentration problems, and restlessness) bridging two disorders (e.g., depression and generalized anxiety). These are called bridge symptoms and can spread activation from one disorder to the other (e.g., worry as core symptom of generalized anxiety leads to sleep problems and fatigue, which leads to a sad mood as a central symptom of depression). They also propose a method for visualizing comorbidity networks in which criteria for key aspects of interpretation about relationships and the positioning of nodes are taken into account. The more two symptoms co-occur, the thicker the edge will look, and overlapping symptoms are placed in the middle of the graph while non-overlapping ones are placed on the extreme left and right.
Boschloo et al. [6], exploring psychological symptoms criteria for diagnosing clinical disorders, conclude that all diagnoses are connected via specific symptom pairs to at least three other diagnoses. Fried et al. [9] indicate that one implication of the network view on comorbidity is that diagnoses may co-occur as a function of their number of shared symptoms. At the time, this was empirically unresolved because, in general terms, the studies measured and visualized the bridge symptoms using traditional network centrality measures [31, 32]. Jones, Ma, and McNally's 2019 study [3] presents formal quantitative methods for identifying bridge symptoms by developing four network statistics, called bridge centrality measures, considering the community (defined as the theoretically based group of nodes corresponding to a psychiatric disorder based on clinical criteria, not based on any network analytic procedure) [3, 36].
Research on the comorbidity of depression and anxiety symptoms applying network analysis has found that “concentration problems” and “feeling sad” are central symptoms for depression, while a relevant co-occurrence between “loneliness” and other symptoms was found through its association with loss and a lack of instrumental social support even in adulthood [37]. Feelings of restlessness, fatigue, and fear were also found as central symptoms on an internalizing symptom network in a clinical sample of 8–18-years old [38]. Across ages, an increase in connectivity throughout aging development suggests that symptoms may reinforce each other, potentially contributing to the high levels of lifetime continuity for these disorders [39]. Although these are important findings, there is a need for deeper exploration of the comorbidity between depression and anxiety.
The aim of this study is to explore the comorbidity between depression and anxiety symptoms in the context of the knowledge outlined above. The specific aims are (a) to determine the bridge centrality measures for each node and identify bridge symptoms; (b) to explore the associations of the symptoms between the communities by creating a comorbidity network and a shortest pathway network; and (c) to analyze the impact on the strength and structure of the comorbidity network.
Given the high comorbidity that exists between these two disorders, the literature presents us with several expected findings. Regarding the structure and dynamics of the network, we expect from a general view that measures of centrality will indicate: (1) that various symptoms are the most central (hypothesis a); and (2) that numerous bridge symptoms can be identified (hypothesis b). In accordance with these general results, we expect (3) that the comorbidity network will be highly interconnected and the shortest pathway could vary in relation to the nature of the symptoms (hypothesis c); that (4) symptoms related to negative affect may function as bridge symptoms, since this construct has been found to be a component of both depression and anxiety (hypothesis d); and (5) interpersonal symptoms will show higher scores on bridge centrality measures given the capacity of interpersonal behaviors to activate other symptoms in the network (hypothesis e).
Methods
Participants
The sample consisted of 986 Spanish children and adolescents, including 540 girls (55%) and 446 boys (45%). Their ages ranged from 9 to 18 years (M = 13.09; SD = 2.01). Participants were selected from various public and charter schools in several Spanish cities. As shown in Table 1, the distribution of participants according to age and sex variables was homogeneous (x2 = 2.56; gl = 3; p = 0.47).
Procedure
The Ethics Commission of the National University of Distance Education (UNED) approved the study and its compliance with the ethical and data protection standards required by European legislation. Approval was then requested from the schools and informed consent was sought from the parents and the participants themselves. Data collection was subsequently carried out in the classrooms with the class groups already established. All the questionnaires were identified using codes to ensure participants’ anonymity. Participation was voluntary and the instructions and evaluation conditions were similar for all participants.
Measures
Clinical symptoms of depression were measured using the Center for Epidemiological Studies Depression Scale for Children and Adolescents, CES-DC [40,41,42,43]. This scale groups behaviors into depressed affect, somatic problems, interpersonal problems, and positive affect. It consists of 20 items with four Likert-type response options (from 1 = “almost nothing” to 4 = “a lot”).
The Youth Self-Report, YSR [44, 45], was used to study the symptoms of depression-anxiety. The YSR uses self-report of symptoms to evaluate emotional and behavioral problems in children and adolescents. It has 112 items measured on a Likert scale with three answer options (from 0 = “not true” to 3 = “true, very often or fairly often”). The higher the score on the subscales, the higher the degree of psychopathology. The present study only used data from the depression-anxiety subscale, which mixes the manifest behaviors of the two disorders. Two expert clinicians (95% inter-rater reliability) used the Diagnostic and Statistical Manual of Mental Disorders [46] to identify depression and anxiety items by their content (e.g., negative affect, somatic, cognitive, interpersonal) and specificity (i.e., specific versus non-specific). Specific items formed part of the particular or essential criteria for depression or anxiety. Non-specific items, meanwhile, were associated with either anxiety or depression as part of the nomological network of these disorders or were used to operationalize the clinical significant criterion as an additional requirement (e.g., duration, severity, family, social and work/school discomfort/distress or impairment). The items used in this study are shown in Table 2.
Data Analysis Plan
R Program [47] was used to conduct all the analyses. First, an exploratory descriptive analysis of the items was performed. In total, the highest percentage of missing data was 2% for the CES-DC items and 3% for the YSR items. It is standard to consider percentages under 20% to be candidates for imputation [48]. Multiple imputation is recommended as the best method for Likert-type scales [49, 50], even for the CES-DC [51]. Among the multiple imputation techniques used, the random forest approach is considered the most accurate for considering the various patterns of missing data [52,53,54]. Hence, in the present study, missing data were imputed with multiple imputation via the random forest technique using the MICE package [55].
To explore the comorbidity between symptoms of depression and anxiety-depression from the network perspective, bridge symptoms were determined based on four measures of bridge centrality: the bridge strength and expected influence, which estimates a node’s sum connectivity with other disorders and differs by taking or not taking the absolute value of edges before summing them; bridge betweenness, which assesses the number of times a node lies on the shortest path between any two nodes from two distinct disorders; and bridge closeness, which reflects the average distance from a node to all nodes outside of its own disorder. In sum, all are estimated based on the number of edges and edge weights, distance, and intermediation of the nodes in the network [3]. The concordance on bridge symptoms by measures of bridge centrality was visualized using a co-occurrence graph [56].
The comorbidity and shortest pathway networks between disorders were also visualized. The bridge symptoms shown in the first network were determined as top scoring nodes given the bridge centrality measures as it is the suggested method to detect bridge symptoms [3]. The second network can be seen as a roadmap that allows clear identification of possible pathways and mediating items between nodes [34, 57]. Lastly, the impact of each symptom on the global strength and structure of the comorbidity network was studied [35].
Bridge centrality, bridge symptoms, and impact were estimated using the bridge and impact functions in the networktools package [58]. For the comorbidity and the shortest pathway networks the qgraph package [34] was also used, with the functions qgraph applying method EBICglasso and pathways.
Results
Bridge Centrality Measures and Bridge Symptoms
Bridge centrality measures were determined for each symptom. The first ones are shown in Fig. 1. The symptoms that are relevant due to their strong connectedness between disorders (bridge strength > 1.00 and expected bridge influence steps 1 and 2 > 1.00) are “feels lonely” (CES14), “I feel people dislike me” (CES19), “trouble getting active” (CES20), “people have been unfriendly” (CES15), and “bothered more than usual” (CES1).
The symptoms that are the greatest intermediaries (bridge betweenness > 1.00) between nodes from both disorders are “talks about suicide” (YSR91), “feels unloved” (YSR33), “fears school” (YSR30), and, in common with the symptoms with the strongest connectedness, “feels lonely” (CES14) and “I feel people dislike me” (CES19).
The symptoms that show the shortest distance (bridge closeness > 1.00) between the two disorders are “feels lonely” (CES14), “I feel people dislike me” (CES19), "trouble getting active” (CES20), “talks about suicide” (YSR91), and “talks less than usual” (CES13).
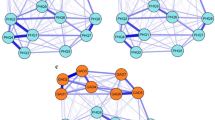
Based on the results of the bridge centrality measures, the bridge symptoms of the comorbidity network between anxiety and depression were estimated; these are shown in Fig. 2. The node type differentiates those that are bridge symptoms in more than two measures of bridge centrality (shared bridge nodes), and the specific symptoms are those that have a single measure of bridge centrality (specific bridge nodes).
Both “feels lonely” (CES14) and “feels unloved” (YSR33) were identified as bridge symptoms in all the bridge centrality measures. The combination of bridge strength and bridge closeness further pointed to “trouble getting active” (CES20) and “I feel people dislike me” (CES19); while the combination of bridge betweenness and bridge closeness added “talks about suicide” (YSR91) and “talks less than usual” (CES13). The specific bridge symptoms “thinks life has been a failure” (CES9) and “feels just as good as others” (CES4) were highlighted in bridge strength. “Everything has been an effort” (CES7) and “fears school” (YSR30) were identified in bridge betweenness, and “people has been unfriendly” (CES15) was identified in bridge closeness.
Comorbidity and Shortest Path Networks
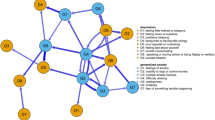
To explore the relationships of the symptoms between anxiety and depression, a comorbidity network and a shortest pathway network were created. Both are presented in Fig. 3. In the comorbidity network, moderate and strong correlations (represented by thicker edges) are observed between some nodes of the network. It can be visually identified that the boundaries between the two communities of symptoms are diffuse and clearly interconnected rather than being specific to one or the other disorder.
In Fig. 3b other interesting connections can be observed. The circle from “YSR31: Fears doing something bad” to “YSR30: Fears school” to “YSR33: Feels unloved” and back to YSR31 connects with a symptom of a depressive nature (“YSR35: Feels worthless”). Where “YSR33: Feels unloved” is a symptom apart from anxiety-depression, it can be considered as a warning of comorbidity. Meanwhile, the circle from “CES14: Feels lonely” to “CES15: People have been unfriendly” to “CES19: I feel people dislike me” and back to CES14 connects with suicidal ideation (“YSR91: Talks about suicide”); these items are related to interpersonal relationships.
Impact of the Symptoms
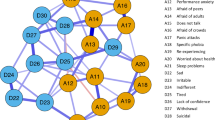
The impact on the strength and structure of the comorbidity network were analyzed. Figure 4 shows that the symptoms with the greatest influence on network connectivity according to the global strength impact coefficient (GSI > 1.00) are “worries” (YSR112), “feels depressed” (CES6), “nervous/tense” (YSR45), “feels sad” (CES18), “sleeps restlessly” (CES11), and “bothered more than usual” (CES1). The symptoms with the greatest potential to cause change in the structure of the network (NSI > 1.00) are “fears school” (YSR30), “feels unloved” (YSR33), “talks about suicide” (YSR91), and “worries” (YSR112).
Discussion
In exploring the relationships of symptoms of depression and anxiety, it was found through the bridge centrality measures that some symptoms play the role of a bridge system and could thus explain the interconnection or comorbidity between the symptom communities of the respective disorders. This is consistent with hypotheses a and b and with previous findings [2, 3]. Some of the symptoms involved in the bridge system are non-specific (i.e., “feels lonely,” “people have been unfriendly,” “feels unloved”) and others are specific to anxiety (i.e., “fears school,” “talks less than usual”) or depression (i.e., “bothered more than usual,” “trouble getting active,” “talks about suicide”).
Among those bridge symptoms, all measures of bridge centrality align on “feels lonely” and “feels unloved” as the most significant symptoms in the comorbidity between the disorders. Considering their connotations in relation to the perception and experience of an interpersonal deficit or difficulty (represented by measures such as “people have been unfriendly,” “fears school,” “talks less than usual,” and “I feel people dislike me”), all appear to be associated with psychological maladjustment emerging from several problems whose interactions build a connected network of symptoms. In this sense, the notion of mental health would correspond to a stable state of a weakly connected network of symptoms, while psychological maladjustment would correspond to a stable state of strongly connected symptoms [1, 29, 59]; this coincides with the idea of an essential link and effect with social and academic functioning in both depression and anxiety [13, 15].
Symptoms of depression such as social withdrawal, loss of motivation, sleep disturbance, and reduced energy tend to impact a child’s ability to attend school, particularly absenteeism, unexcused absences/truancy, and school refusal [20]. Likewise, children with anxiety problems may refuse to attend school in order to avoid school-related situations that cause distress or negative affect; or to escape aversive social and/or evaluative situations [60, 61]. Both depressed and anxious children may demonstrate social deficits (e.g., low social skills and social status) and, as a result, do not receive positive social reinforcement; and they have more problems coping with negative life events and high stress. Such symptoms also point to children's negative academic cognitions (i.e., poor beliefs about their important role in academic competence and ability to control academic outcomes) and poor academic performance (14). Consistent with hypothesis e, the interpersonal symptoms show higher scores on the bridge centrality measures based on their capacity to activate other symptoms in the network.
The significance of “feels lonely” emphasizes the importance of considering the perception of loneliness, understood as the discrepancy or dissatisfaction between the personal desire for social relationships and the relationships that actually exist, in addition to a feeling of physical or emotional disconnection from others [62]. This is of particular concern because, from a theoretical perspective, this is not considered to be a symptom or standard criterion for clinical diagnosis in categorical diagnostic taxonomies [46], despite multiple studies revealing the relevance of this symptom, including in the Spanish adolescent population [63, 64]. Also “feels unloved” acquires importance if one considers how essential family and interpersonal relationships of acceptance and love are throughout the development of an individual [65,66,67,68]. Adults with good mental health are typically those who are able to develop adequate socio-emotional competencies in their relationships with peers and authority figures in their childhood and adolescence. They also experience conflict within the framework of an authoritative and democratic parental style, in which there is a reasonable balance between love and control from parental figures [69, 70].
The comorbidity network shows that despite strong interconnectedness, the communities of depression and anxiety symptoms are diffuse. This is to be expected among children, given findings in the previous literature on the theoretical explanations highlighting the coexistence of anxiety and depression, commonly involving a full spectrum of symptoms, even though both are conceived as single and distinct disorders [8, 13, 15, 71]. It is in line with recent empirical findings for The Hierarchical Taxonomy of Psychopathology (HiTOP), a new diagnostic classification in which the symptoms of both anxiety and depression are considered to form part of a “Distress” subfactor inside the “Internalizing” spectra [72, 73]. Also, as expected (hypothesis d), the findings are consistent with the common factor of negative affect between anxiety and depression [21].
The shortest pathway network varies, as expected (hypothesis c). When a group of items, or symptoms, such as “fears doing something bad,” “fears school,” and “feels unloved,” connects with a symptom of a depressive nature such as “feels worthless,” the symptom of “feels unloved” should be given special attention when the comorbidity is studied. The same is also true when related items such as “feels lonely,” “people have been unfriendly,” “I feel people dislike me” connects with suicidal ideation in the form of “talks about suicide.” All these items relate to interpersonal relationships and, consistent with hypothesis e (loneliness/isolation, unkind people), have an important role in maintaining the symptomatology and activating a potential comorbid depression-anxiety network [19, 20, 74].
It is also important to highlight in this circle the role of item “Talks about suicide.” This is an item related to interpersonal (communication about suicide) and cognitive (ideation of suicide) contents. Suicidal ideation and communication have been mainly associated with depression and especially to depression-anxiety comorbidity as a sign of loneliness grows, which can be severe in young people [19]. From an interpersonal perspective, it is important that research shows significant relationships between different interpersonal factors (e.g., poor social support, relationship quality, peer victimization, social rejection, isolation) and suicide behaviors [75,76,77] (hypothesis e).
In a way, these subpaths or circles are related to previous theoretical findings and provide support for them. Some models suggest that anxiety often temporally precedes depression, but the combination of the two marks a particularly heightened vulnerability and negative prognosis [11, 13]. Others support the conclusion that there is a shared common factor, as in the tripartite model, which includes mixed symptoms called “negative affect” [21]. Still others suggest a multiple pathways model [27], which acknowledges that the comorbidity differs based on the type of anxiety disorder; for example, core risk factors (e.g., genetics) interact with interpersonal risk factors (e.g., loneliness) and cognitive vulnerabilities (e.g., hopelessness), leading to depression among children with social phobia [13, 78, 79].
Symptoms of “worries” and “nervous/tense” (associated with anxiety) as well as “feels depressed” and “feels sad” (associated with depression) stand out in terms of their impact on the connectivity of the network. This is congruent with the main diagnostic criteria of both depression (depressed mood) and anxiety (tension/nervousness) [46, 80] and with existing literature on both disorders across development (ages 5–14), which identify feeling “anxious/fearful” and “unhappy/sad” as the most central symptoms [39]. Again, most of these items are related to the negative affect, in line with the tripartite model. Worry (an essential symptom of generalized anxiety disorder [GAD]) is a symptom that, despite being specific to anxiety, is very present in depressive disorders. This is also consistent with the literature that asserts that there is no difference between depression and GAD [81,82,83,84,85].
Symptoms that have strong impact on the structure of the network are more related to comorbidity [35]; “fears school,” “feels unloved,” and “talks about suicide” are the three nodes that could warn of a greater risk of comorbidity and, therefore, of severity and dysfunction. This increases in importance when considering the associations between depression and poor school attendance, particularly absenteeism and unexcused absences/truancy [20], and the fact that adolescents who associate with deviant peers are more likely to report a greater intensity (increased frequency and duration and decreased controllability) of their suicidal ideation [75]. These three symptoms may suggest the level of severity and the clinical significance of these psychological problems.
In summary, the hypotheses were partially confirmed. Of the three bridge centrality measures, only “feels lonely” and “feels unloved” were considered the most central bridge symptoms. The comorbidity network was diffuse and interconnected, consistent with the theoretical proposition of a shared common factor of negative affect between anxiety and depression [21]. Further, the pathway network shows at least two routes for the relationships between the symptoms. Both the connection between symptoms of fears and the self-perception of worth and unloved, and symptoms of interpersonal relationships connecting with suicidal ideation, are highlighted.
Given the previous findings, there are some practical implications to be made. When evaluating evolution or prognosis, clinicians could consider these findings when both disorders are present in patients and provoke symptomology that should be attended to. They may consider the most central and impactful bridge symptoms in the comorbidity network as reference points for diagnosis and clinical assessment and also as targets in prevention practices, counseling, and group/community interventions [86]. The latter should take into account that some symptoms involving negative affect, interpersonal connotations, and cognitive biases can be worked on through training and psychoeducational activities with groups of children and adolescents.
It should be mentioned that this study has a limitation in that we did not consider the more physiological symptoms (e.g., tachycardia, dizziness, shortness of breath) associated with anxiety and/or depression. However, the evidence for physiological symptoms related to depression and anxiety problems is not as strong in child samples as it is in adult samples [87]. Another limitation is that this study was carried out with cross-sectional data in the general population, and thus we could neither study a dynamic sequence nor explore any differences by age groups or sex in clinically referred children and adolescents. As the participants were taken from the general and non-clinical population, they did not share a clinical diagnosis of anxiety and depression.
Future research could carry out comparative research by sex and age groups to identify any differences in the symptomatic dynamics of comorbidity during development and across gender groups and could also explore differences related to cultural variables [38, 39]. It could also adopt multi-method and multi-informant approaches, which could be equivalent to the applied idiographic and nomothetic approaches in comparative research studies with clinical populations. Finally, further research could apply additional analyses, such as personalized networks or time-series networks, complemented with qualitative analysis, and consider cross-cultural, transdisciplinary or international research perspectives [14, 88,89,90,91,92,93].
Summary
The aim of this study was to explore the comorbidity between depression and anxiety symptoms from the network perspective. The specific aims were (a) to determine the bridge centrality measures for each node and identify bridge symptoms; (b) to explore the associations of the symptoms between the communities by creating a comorbidity network and shortest pathway network; and (c) to analyze the impact on the strength and structure of the comorbidity network. Data were gathered from Spanish children and adolescents aged 9 to 18 years (N = 986). Bridge symptoms were estimated through measures of bridge centrality; comorbidity, shortest pathway networks, and the impact of the symptoms on the networks were explored. Both “feels lonely” and “feels unloved” were identified as the most central bridge symptoms among others of interpersonal connotation and specific diagnostic criteria for each disorder. The shortest path network suggests the role of a mixed anxiety-depressive symptomatology that highlights the connection between symptoms of fears and the self-perception of worth and feeling unloved, and the connection between symptoms of interpersonal relationships and suicidal ideation. Lastly, specific symptoms of both anxiety (e.g., “worries,” “nervous/tense”) and depression (e.g., “feels depressed,” “feels sad”) as well as non-specific symptoms (e.g., “fears school,” “feels unloved,” “talks about suicide”) were shown to strongly impact the connectedness and the structure of the network, which can be considered as a warning of comorbidity.
References
Borsboom D, Cramer AOJ, Schmittmann VD et al (2011) The small world of psychopathology. PLoS One 6:e27407. https://doi.org/10.1371/journal.pone.0027407
Cramer AO, Waldorp LJ, van der Maas HLJ, Borsboom D (2010) Comorbidity: a network perspective. Behav Brain Sci 33:137–150. https://doi.org/10.1017/S0140525X09991567
Jones PJ, Ma R, McNally RJ (2019) Bridge centrality: a network approach to understanding comorbidity. Multivar Behav Res. https://doi.org/10.1080/00273171.2019.1614898
Rohde P (2009) Comorbidities with adolescent depression. In: Nolen-Hoeksema S, Hilt LM (eds) Handbook of depression in adolescents. Taylor & Francis, pp 140–177
Borsboom D, Cramer AOJ (2013) Network analysis: an integrative approach to the structure of psychopathology. Annu Rev Clin Psychol 9:91–121. https://doi.org/10.1146/annurev-clinpsy-050212-185608
Boschloo L, van Borkulo CD, Rhemtulla M et al (2015) The network structure of symptoms of the diagnostic and statistical manual of mental disorders. PLoS One 10:e0137621. https://doi.org/10.1371/journal.pone.0137621
Barlow DH, Allen LB, Choate ML (2016) Toward a unified treatment for emotional disorders - republished article. Behav Ther 47:838–853. https://doi.org/10.1016/j.beth.2016.11.005
Hammen C, Compas BE (1994) Unmasking unmasked depression in children and adolescents: the problem of comorbidity. Clin Psychol Rev 14:585–603
Fried E, van Borkulo CD, Cramer AOJ et al (2017) Mental disorders as networks of problems: a review of recent insights. Soc Psychiatry Psychiatr Epidemiol 52:1–10. https://doi.org/10.1007/s00127-016-1319-z
Valderas JM, Starfield B, Sibbald B et al (2009) Defining comorbidity: implications for understanding health and health services. Ann Fam Med 7:357–363. https://doi.org/10.1370/afm.983
Brady EU, Kendall PC (1992) Comorbidity of anxiety and depression in children and adolescents. Psychol Bull 111:244–255. https://doi.org/10.1037/0033-2909.111.2.244
Canals J, Voltas N, Hernández-Martínez C et al (2019) Prevalence of DSM-5 anxiety disorders, comorbidity, and persistence of symptoms in Spanish early adolescents. Eur Child Adolesc Psychiatry 28:131–143. https://doi.org/10.1007/s00787-018-1207-z
Cummings CM, Caporino NE, Kendall PC (2014) Comorbidity of anxiety and depression in children and adolescents: 20 years after. Psychol Bull 140:816–845. https://doi.org/10.1037/a0034733
Jeronimus BF (2019) Dynamic system perspectives on Anxiety and Depression. In: Kunnen ES, de Ruiter NMP, Jeronimus BF, van der Gaag MA (eds) Psychosocial Development in Adolescence: Insights from the Dynamic Systems Approach. Routledge Psychology
Seligman LD, Ollendick TH (1998) Comorbidity of anxiety and depression in children and adolescents: an integrative review. Clin Child Fam Psychol 1:125–144
Albert U, Rosso G, Maina G, Bogetto F (2008) Impact of anxiety disorder comorbidity on quality of life in euthymic bipolar disorder patients: differences between bipolar I and II subtypes. J Affect Disord 105:297–303. https://doi.org/10.1016/j.jad.2007.05.020
Kendall PC, Compton SN, Walkup JT et al (2010) Clinical characteristics of anxiety disordered youth. J Anxiety Disord 24:360–365. https://doi.org/10.1016/j.janxdis.2010.01.009
Lopez B, Turner RJ, Saavedra LM (2005) Anxiety and risk for substance dependence among late adolescents/young adults. J Anxiety Disord 19:275–294. https://doi.org/10.1016/j.janxdis.2004.03.001
Pawlak C, Pascual-Sanchez T, Raë P et al (1999) Anxiety disorders, comorbidity, and suicide attempts in adolescence: a preliminary investigation. Eur Psychiatry 14:132–136. https://doi.org/10.1016/s0924-9338(99)80730-5
Finning K, Ukoumunne O, Ford T et al (2019) The association between child and adolescent depression and poor attendance at school: a systematic review and meta-analysis. J Affect Disord 245:928–938. https://doi.org/10.1016/j.jad.2018.11.055
Clark LA, Watson D (1991) Tripartite model of anxiety and depression: psychometric evidence and taxonomic implications. J Abnorm Psychol 100:316
De Bolle M, De Clercq B, Decuyper M, De Fruyt F (2011) Affective determinants of anxiety and depression development in children and adolescents: an individual growth curve analysis. Child Psychiatry Hum Dev 42:694–711. https://doi.org/10.1007/s10578-011-0241-6
Carey TC, Carey MP, Kelley ML (1997) Differential emotions theory: relative contribution of emotion, cognition, and behavior to the prediction of depressive symptomatology in non-referred adolescents. J Clin Psychol 53:25–34. https://doi.org/10.1002/(sici)1097-4679(199701)53:1%3c25::aid-jclp4%3e3.0.co;2-u
Krueger RF (1999) The structure of common mental disorders. Arch Gen Psychiatry 56:921–926. https://doi.org/10.1001/archpsyc.56.10.921
Watson D (2005) Rethinking the mood and anxiety disorders: a quantitative hierarchical model for DSM-V. J Abnorm Psychol 114:522–536. https://doi.org/10.1037/0021-843X.114.4.522
Higa-McMillan CK, Smith RL, Chorpita BF, Hayashi K (2008) Common and unique factors associated with DSM-IV-TR internalizing disorders in children. J Abnorm Child Psychol 36:1279–1288. https://doi.org/10.1007/s10802-008-9250-8
Brown TA, Chorpita BF, Barlow DH (1998) Structural relationships among dimensions of the DSM-IV anxiety and mood disorders and dimensions of negative affect, positive affect, and autonomic arousal. J Abnorm Psychol 107:179
Fried E (2017) What are psychological constructs? on the nature and statistical modelling of emotions, intelligence, personality traits and mental disorders. Health Psychol Rev 11:130–134. https://doi.org/10.1080/17437199.2017.1306718
Schmittmann VD, Cramer AOJ, Waldorp LJ et al (2013) Deconstructing the construct: a network perspective on psychological phenomena. New Ideas Psychol 31:43–53. https://doi.org/10.1016/j.newideapsych.2011.02.007
Robinaugh DJ, Hoekstra RHA, Toner ER, Borsboom D (2020) The network approach to psychopathology: a review of the literature 2008–2018 and an agenda for future research. Psychol Med 50:353–366. https://doi.org/10.1017/S0033291719003404
Costantini G, Epskamp S, Borsboom D et al (2015) State of the aRt personality research: a tutorial on network analysis of personality data in R. J Res 54:13–29. https://doi.org/10.1016/j.jrp.2014.07.003
Epskamp S (2017) Network psychometrics. PhD Thesis, University of Amsterdam
Epskamp S, Fried E (2018) A tutorial on regularized partial correlation networks. Psychol Methods 23:617–634. https://doi.org/10.1037/met0000167
Epskamp S, Cramer AOJ, Waldorp LJ et al (2012) qgraph: network visualizations of relationships in psychometric data. J Stat Softw 48:1–18
Jones PJ (2017) Impact: a new statistic for network analysis. R package vignette https://cran.r-project.org/web/packages/networktools/vignettes/Impact.pdf
Letina S, Blanken TF, Deserno MK, Borsboom D (2019) Expanding network analysis tools in psychological networks: minimal spanning trees, participation coefficients, and motif analysis applied to a network of 26 psychological attributes. Complexity 2019:9424605. https://doi.org/10.1155/2019/9424605
Contreras A, Nieto I, Valiente C et al (2019) The study of psychopathology from the network analysis perspective: a systematic review. Psychother Psychosom 88:71–83. https://doi.org/10.1159/000497425
McElroy E, Patalay P (2019) In search of disorders: internalizing symptom networks in a large clinical sample. J Child Psychol Psychiatry 60:897–906
McElroy E, Fearon P, Belsky J et al (2018) Networks of depression and anxiety symptoms across development. J Am Acad Child Adolesc Psychiatry 57:964–973. https://doi.org/10.1016/j.jaac.2018.05.027
Radloff LS (1977) The CES-D scale: a self-report depression scale for research in the general population. Appl Psychol Meas 1:385–401. https://doi.org/10.1177/014662167700100306
Radloff LS (1991) The Use of the Center for Epidemiologic Studies Depression Scale in Adolescents and Young Adults. J Youth Adolesc 20:149–166. https://doi.org/10.1007/BF01537606
Sánchez-Hernández MO, Delgado B, Carrasco MA, Holgado Tello FP (2018) Facetas de la “Escala de depresión del Centro de Estudios Epidemiológicos para niños y adolescentes” (CES-DC) en españoles: validación empírica. Psicol conduct 26:495–512
Weissman MM, Orvaschel H, Padian N (1980) Children´s symptom and social functioning self-report scales: comparison of mothers´ and children´s reports. J Nerv Ment Dis 168:736–740
Achenbach T (1991) Manual for youth self-report 1991 YSR profile. University of Vermont, Burlington
Achenbach T, Rescorla L (2001) The Manual for the AsEBA school-Age Forms & Profiles. University of Vermont, Research Center for Children, Youth, and Families, Burlington
American Psychiatric Association (2013) Diagnostic and statistical manual of mental disorders : DSM-5, 5th ed. American Psychiatric Association, Arlington, VA
R Core Team (2020) R: a language and environment for statistical computing. R Foundation for Statistical Computing, Vienna
Hair J, Black W, Babin B, Anderson R (2014) Multivariate data analysis, 7a ed. Pearson
Brown TA (2015) Confirmatory factor analysis for applied research. The Guilford Press
Enders CK (2010) Applied missing data analysis. The Guilford Press
Bono C, Ried LD, Kimberlin C, Vogel B (2007) Missing data on the center for epidemiologic studies depression scale: a comparison of 4 imputation techniques. Res Soc Adm Pharm 3:1–27. https://doi.org/10.1016/j.sapharm.2006.04.001
Kokla M, Virtanen J, Kolehmainen M et al (2019) Random forest-based imputation outperforms other methods for imputing LC-MS metabolomics data: a comparative study. BMC Bioinformatics 20:492. https://doi.org/10.1186/s12859-019-3110-0
Shah A, Bartlett J, Carpenter J et al (2014) Comparison of random forest and parametric imputation models for imputing missing data using MICE: a CALIBER study. Am J Epidemiol 179:764–774. https://doi.org/10.1093/aje/kwt312
Tang F, Ishwaran H (2017) Random forest missing data algorithms. Stat Anal Data Min 10:363–377. https://doi.org/10.1002/sam.11348
van Buuren S, Groothuis-Oudshoorn K (2011) mice: multivariate imputation by chained equations in R. J Stat Softw 45:1–67
Fried E (2017) The 52 symptoms of major depression: lack of content overlap among seven common depression scales. J Affect Disord 208:191–197. https://doi.org/10.1016/j.jad.2016.10.019
Isvoranu A, van Borkulo CD, Boyette L-L, et al (2016) A network approach to psychosis: pathways between childhood trauma and psychotic symptoms. Schizophrenia Bulletin 43:sbw055. https://doi.org/10.1093/schbul/sbw055
Jones PJ (2020) networktools: tools for Identifying Important Nodes in Networks. https://CRAN.R-project.org/package=networktools
Bringmann LF, Vissers N, Wichers M et al (2013) A network approach to psychopathology: new insights into clinical longitudinal data. PLoS One 8:e60188. https://doi.org/10.1371/journal.pone.0060188
Beidas R, Crawley S, Mychailyszyn M, Comer J (2010) Cognitive-behavioral treatment of anxious youth with comorbid school refusal: clinical presentation and treatment response. Psychol Top 19:255–271
Kearney C, Albano AM (2007) When children refuse school: a cognitive-behavioral therapy approach, 2nd edn. Oxford University Press, New York
Eccles AM, Qualter P, Panayiotou M et al (2020) Trajectories of early adolescent loneliness: implications for physical health and sleep. J Child Fam Stud 29:3398–3407. https://doi.org/10.1007/s10826-020-01804-3
Martínez-Hernáez Á, Muñoz García A (2010) «Un infinito que no acaba». Modelos explicativos sobre la depresión y el malestar emocional entre los adolescentes barceloneses (España). Primera parte Salud Ment 33:145–152
Martínez-Hernáez Á, Muñoz García A (2010) «Un infinito que no acaba». Modelos explicativos sobre la depresión y el malestar emocional entre los adolescentes barceloneses (España). Segunda parte Salud Ment 33:229–236
Carrasco MA, Delgado B, Holgado-Tello FP (2019) Parental acceptance and children’s psychological adjustment: the moderating effects of interpersonal power and prestige across age. PLoS One 14:e0215325. https://doi.org/10.1371/journal.pone.0215325
Rodríguez Ruíz MM, Carrasco MA, Holgado Tello FP (2019) Father involvement and children’s psychological adjustment: maternal and paternal acceptance as mediators. J Fam Stud 25:151–169. https://doi.org/10.1080/13229400.2016.1211549
Henry LM, Steele EH, Watson KH et al (2020) Stress exposure and maternal depression as risk factors for symptoms of anxiety and depression in adolescents. Child Psychiatry Hum Dev 51:572–584. https://doi.org/10.1007/s10578-019-00940-2
Khan M, Renk K (2018) Understanding the pathways between mothers’ childhood maltreatment experiences and patterns of insecure attachment with young children via symptoms of depression. Child Psychiatry Hum Dev 49:928–940. https://doi.org/10.1007/s10578-018-0808-6
Bowlby J (1979) The Bowlby-Ainsworth attachment theory. Behav Brain Sci 2:637–638. https://doi.org/10.1017/S0140525X00064955
Bretherton I (1992) The origins of attachment theory: John Bowlby and Mary Ainsworth. Dev Psychol 28:759–775. https://doi.org/10.1037/0012-1649.28.5.759
Kovacs M (1990) Comorbid anxiety disorders in childhood onset depressions. In: Maser J, Cloninger C (eds) Comorbidity of mood and anxiety disorders. American Psychiatric Press, Washington DC, pp 272–281
Conway CC, Forbes MK, Forbush KT et al (2019) A hierarchical taxonomy of psychopathology can transform mental health research. Perspect Psychol Sci 14:419–436. https://doi.org/10.1177/1745691618810696
Krueger RF, Kotov R, Watson D et al (2018) Progress in achieving quantitative classification of psychopathology. World Psychiatry 17:282–293. https://doi.org/10.1002/wps.20566
McElroy E, Shevlin M, Murphy J, McBride O (2018) Co-occurring internalizing and externalizing psychopathology in childhood and adolescence: a network approach. Eur Child Adolesc Psychiatry 27:1449–1457. https://doi.org/10.1007/s00787-018-1128-x
Abbott CH, Zisk A, Bounoua N et al (2019) Peer deviance, social networks, and suicide ideation intensity in a clinical sample of adolescents. J Child Fam Stud 28:796–804. https://doi.org/10.1007/s10826-018-01320-5
Geoffroy M-C, Boivin M, Arseneault L et al (2016) Associations between peer victimization and suicidal ideation and suicide attempt during adolescence: results from a prospective population-based birth cohort. J Am Acad Child Adolesc Psychiatry 55:99–105. https://doi.org/10.1016/j.jaac.2015.11.010
Prinstein MJ, Boergers J, Spirito A et al (2000) Peer functioning, family dysfunction, and psychological symptoms in a risk factor model for adolescent inpatients’ suicidal ideation severity. J Clin Child Psychol 29:392–405. https://doi.org/10.1207/S15374424JCCP2903_10
Gibb BE, Alloy LB (2006) A prospective test of the hopelessness theory of depression in children. J Clin Child Adolesc Psychol 35:264–274
Starr LR, Davila J (2012) Responding to anxiety with rumination and hopelessness: mechanism of anxiety-depression symptom co-occurrence? Cognit Ther Res 36:321–337
Widiger TA, Gore WL (2014) Diagnostic and statistical manual (DSM). The Oxford handbook of depression and comorbidity. Oxford University Press, Nueva York, pp 11–28
Curtiss J, Klemanski D (2016) Taxonicity and network structure of generalized anxiety disorder and major depressive disorder: an admixture analysis and complex network analysis. J Affect Disord. https://doi.org/10.1016/j.jad.2016.04.007
Kendler KS, Neale MC, Kessler RC et al (1992) Major depression and generalized anxiety disorder. Same genes, (partly) different environments? Arch Gen Psychiatry 49:716–722. https://doi.org/10.1001/archpsyc.1992.01820090044008
Moffitt TE, Caspi A, Harrington H et al (2007) Generalized anxiety disorder and depression: childhood risk factors in a birth cohort followed to age 32. Psychol Med 37:441–452. https://doi.org/10.1017/S0033291706009640
Nolen-Hoeksema S, Wisco BE, Lyubomirsky S (2008) Rethinking rumination. Perspect Psychol Sci 3:400–424. https://doi.org/10.1111/j.1745-6924.2008.00088.x
Nolen-Hoeksema S, Watkins ER (2011) A heuristic for developing transdiagnostic models of psychopathology: explaining multifinality and divergent trajectories. Perspect Psychol Sci 6:589–609. https://doi.org/10.1177/1745691611419672
Mullarkey MC, Marchetti I, Beevers CG (2019) Using network analysis to identify central symptoms of adolescent depression. J Clin Child Adolesc Psychol 48:656–668. https://doi.org/10.1080/15374416.2018.1437735
Chorpita BF (2002) The tripartite model and dimensions of anxiety and depression: an examination of structure in a large school sample. J Abnorm Child Psychol 30:177–190. https://doi.org/10.1023/a:1014709417132
Epskamp S, van Borkulo CD, van der Veen DC et al (2018) Personalized network modeling in psychopathology: the importance of contemporaneous and temporal connections. Clin Psychol Sci 6:416–427. https://doi.org/10.1177/2167702617744325
Howe E, Bosley HG, Fisher AJ (2020) Idiographic network analysis of discrete mood states prior to treatment. Couns Psychother Res. https://doi.org/10.1002/capr.12295
Piccirillo ML, Rodebaugh TL (2019) Foundations of idiographic methods in psychology and applications for psychotherapy. Clin Psychol Rev 71:90–100. https://doi.org/10.1016/j.cpr.2019.01.002
von Klipstein L, Riese H, van der Veen DC et al (2020) Using person-specific networks in psychotherapy: challenges, limitations, and how we could use them anyway. BMC Med 18:345. https://doi.org/10.1186/s12916-020-01818-0
Yanartaş Ö, Kani HT, Kani AS et al (2019) Depression and anxiety have unique contributions to somatic complaints in depression, irritable bowel syndrome and inflammatory bowel diseases. Psychiatry and Clinical Psychopharmacology 29:418–426. https://doi.org/10.1080/24750573.2019.1589177
Fried E, Stockert S, Haslbeck J et al (2019) Using network analysis to examine links between individual depressive symptoms, inflammatory markers, and covariates. Psychol Med 50:2682–2690. https://doi.org/10.1017/S0033291719002770
Acknowledgements
The authors thank all the participants and their parents.
Funding
Open Access funding provided thanks to the CRUE-CSIC agreement with Springer Nature.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in the studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all the individual participants included in the study and their parents.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sánchez Hernández, M.O., Carrasco, M.A. & Holgado-Tello, F.P. Anxiety and Depression Symptoms in Spanish Children and Adolescents: An Exploration of Comorbidity from the Network Perspective. Child Psychiatry Hum Dev 54, 736–749 (2023). https://doi.org/10.1007/s10578-021-01286-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10578-021-01286-4